Key Points
-
The ciliary and centrosome hypothesis on the pathogenesis of cystic diseases of the kidney (CDK) states that the protein products (cystoproteins) of genes that are mutated in CDK in humans, mice or zebrafish are expressed in primary cilia, basal bodies or centrosomes of renal epithelial cells.
-
We discuss the genetics and function of the genes that are mutated in CDK that have recently been identified and their resulting clinical phenotypes.
-
Cystoproteins are involved in complex protein–protein interactions.
-
Cystoproteins are located in the primary cilia, basal bodies or centrosomes of renal epithelial cells.
-
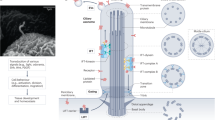
The primary cilium is a sensory organelle that is highly conserved throughout evolution.
-
Many cystoproteins interact with other cystoproteins directly or as members of a protein complex.
-
Cystoproteins are highly conserved in evolution, with orthologues that are expressed in osmosensor ciliated neurons of Caenorhabditis elegans, and in intraflagellar transport (IFT) proteins of Chlamydomonas reinhardtii.
-
Cystoproteins are expressed in several organ systems; mutants therefore give rise to CDK that have pleiotropic phenotypes, such as retinitis pigmentosa, anosmia, ataxia, liver fibrosis, situs inversus, cardiac defects, infertility and obesity.
-
CDK phenotypes are subject to the effects of modifier genes and oligogenic inheritance.
-
The cilia hypothesis of CDK has revolutionized studies into the pathogenesis of many genetic diseases.
-
New therapeutic approaches towards treating CDK are being developed.
Abstract
Cystic kidney diseases are among the most frequent lethal genetic diseases. Positional cloning of novel cystic kidney disease genes revealed that their products (cystoproteins) are expressed in sensory organelles called primary cilia, in basal bodies or in centrosomes. Primary cilia link mechanosensory, visual, osmotic, gustatory and other stimuli to mechanisms of cell-cycle control and epithelial cell polarity. The ciliary expression of cystoproteins explains why many other organs might be also affected in patients with cystic kidney disease. Protein–protein interactions among cystoproteins, and their strong evolutionary conservation, provide a basis for a multidisciplinary approach to unravelling the novel signalling mechanisms that are involved in this disease group.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Olbrich, H. et al. Mutations in a novel gene, NPHP3, cause adolescent nephronophthisis, tapeto-retinal degeneration and hepatic fibrosis. Nature Genet. 34, 455–459 (2003).
The International Polycystic Kidney Disease Consortium. Polycystic kidney disease: the complete structure of the PKD1 gene and its protein. Cell 81, 289–298 (1995). The initial positional cloning of the PKD1 gene, which is mutated in the most frequent autosomal dominant lethal disease in humans.
Hughes, J. et al. The polycystic kidney disease 1 (PKD1) gene encodes a novel protein with multiple cell recognition domains. Nature Genet. 10, 151–160 (1995).
Mochizuki, T. et al. PKD2, a gene for polycystic kidney disease that encodes an integral membrane protein. Science 272, 1339–1342 (1996). The positional cloning of the novel PKD2 gene, which encodes a putative transport channel.
Burn, T. C. et al. Analysis of the genomic sequence for the autosomal dominant polycystic kidney disease (PKD1) gene predicts the presence of a leucine-rich repeat. The American PKD1 Consortium (APKD1 Consortium). Hum. Mol. Genet. 4, 575–582 (1995).
Bhunia, A. K. et al. PKD1 induces p21waf1 and regulation of the cell cycle via direct activation of the JAK–STAT signaling pathway in a process requiring PKD2. Cell 109, 157–168 (2002).
Wilson, P. D. Polycystic kidney disease: new understanding in the pathogenesis. Int. J. Biochem. Cell. Biol. 36, 1868–1873 (2004).
Moyer, J. H. et al. Candidate gene associated with a mutation causing recessive polycystic kidney disease in mice. Science 264, 1329–1333 (1994).
Pazour, G. J. et al. Chlamydomonas IFT88 and its mouse homologue, polycystic kidney disease gene Tg737, are required for assembly of cilia and flagella. J. Cell Biol. 151, 709–718 (2000).
Yoder, B. K., Hou, X. & Guay-Woodford, L. M. The polycystic kidney disease proteins, polycystin-1, polycystin-2, polaris, and cystin, are co-localized in renal cilia. J. Am. Soc. Nephrol. 13, 2508–2516 (2002).
Igarashi, P. & Somlo, S. Genetics and pathogenesis of polycystic kidney disease. J. Am. Soc. Nephrol. 13, 2384–2398 (2002).
Otto, E. A. et al. Mutations in INVS encoding inversin cause nephronophthisis type 2, linking renal cystic disease to the function of primary cilia and left–right axis determination. Nature Genet. 34, 413–420 (2003). Mutations in INVS were identified as the cause of infantile NPHP2, thereby linking renal cystic disease to the function of primary cilia.
Watnick, T. & Germino, G. From cilia to cyst. Nature Genet. 34, 355–356 (2003). The authors propose the hypothesis that the genes that are mutated in renal cystic disease encode proteins (cystoproteins) that are expressed in primary cilia, basal bodies, centrosomes and focal adhesions or adherens junctions of renal epithelial cells.
Badano, J. L. & Katsanis, N. Beyond Mendel: an evolving view of human genetic disease transmission. Nature Rev. Genet. 3, 779–789 (2002).
Burghes, A. H., Vaessin, H. E. & de La Chapelle, A. Genetics. The land between Mendelian and multifactorial inheritance. Science 293, 2213–2214 (2001).
Katsanis, N. et al. Triallelic inheritance in Bardet–Biedl syndrome, a Mendelian recessive disorder. Science 293, 2256–2259 (2001). This article describes the concept that, in some seemingly recessive diseases, further mutations — in addition to the two mutations that are necessary for a recessive phenotype — might be necessary for the full expression of the phenotype, as if they were oligogenic. This finding generated the new hypothesis that Mendelian disorders and polygenic diseases might be part of a continuous spectrum.
Hildebrandt, F. et al. A novel gene encoding an SH3 domain protein is mutated in nephronophthisis type 1. Nature Genet. 17, 149–153 (1997).
Otto, E. et al. A gene mutated in nephronophthisis and retinitis pigmentosa encodes a novel protein, nephroretinin, conserved in evolution. Am. J. Hum. Genet. 71, 1161–1167 (2002).
Otto, E. et al. Nephrocystin-5, a ciliary IQ domain protein, is mutated in Senior–Loken syndrome and interacts with RPGR and calmodulin. Nature Genet. 37, 282–288 (2005).
Badano, J. L., Teslovich, T. M. & Katsanis, N. The centrosome in human genetic disease. Nature Rev. Genet. 6, 194–205 (2005).
Qian, F., Watnick, T. J., Onuchic, L. F. & Germino, G. G. The molecular basis of focal cyst formation in human autosomal dominant polycystic kidney disease type I. Cell 87, 979–987 (1996). The authors demonstrate clonality of kidney cysts in PKD, thereby lending support to the two-hit hypothesis of PKD.
Koptides, M. et al. Loss of heterozygosity in polycystic kidney disease with a missense mutation in the repeated region of PKD1. Hum. Genet. 103, 709–717 (1998).
Watnick, T. et al. Mutations of PKD1 in ADPKD2 cysts suggest a pathogenic effect of trans-heterozygous mutations. Nature Genet. 25, 143–144 (2000).
Wu, G. et al. Somatic inactivation of Pkd2 results in polycystic kidney disease. Cell 93, 177–188 (1998).
Lu, W. et al. Perinatal lethality with kidney and pancreas defects in mice with a targetted Pkd1 mutation. Nature Genet. 17, 179–181 (1997).
Lu, W. et al. Comparison of Pkd1-targeted mutants reveals that loss of polycystin-1 causes cystogenesis and bone defects. Hum. Mol. Genet. 10, 2385–2396 (2001).
Kim, E. et al. The polycystic kidney disease 1 gene product modulates Wnt signaling. J. Biol. Chem. 274, 4947–4953 (1999).
Pritchard, L. et al. A human PKD1 transgene generates functional polycystin-1 in mice and is associated with a cystic phenotype. Hum. Mol. Genet. 9, 2617–2627 (2000).
Boulter, C. et al. Cardiovascular, skeletal, and renal defects in mice with a targeted disruption of the Pkd1 gene. Proc. Natl Acad. Sci. USA 98, 12174–12179 (2001).
Ong, A. C. & Harris, P. C. Molecular pathogenesis of ADPKD: the polycystin complex gets complex. Kidney Int. 67, 1234–1247 (2005).
Bergmann, C. et al. Clinical consequences of PKHD1 mutations in 164 patients with autosomal-recessive polycystic kidney disease (ARPKD). Kidney Int. 67, 829–848 (2005).
Bergmann, C. et al. PKHD1 mutations in autosomal recessive polycystic kidney disease (ARPKD). Hum. Mutat. 23, 453–463 (2004).
Bergmann, C. et al. Spectrum of mutations in the gene for autosomal recessive polycystic kidney disease (ARPKD/PKHD1). J. Am. Soc. Nephrol. 14, 76–89 (2003).
Ward, C. J. et al. The gene mutated in autosomal recessive polycystic kidney disease encodes a large, receptor-like protein. Nature Genet. 30, 259–269 (2002). The initial positional cloning of a novel gene ( PKHD1 ), which is mutated in autosomal recessive polycystic kidney disease.
Onuchic, L. F. et al. PKHD1, the polycystic kidney and hepatic disease 1 gene, encodes a novel large protein containing multiple immunoglobulin-like plexin-transcription-factor domains and parallel β-helix 1 repeats. Am. J. Hum. Genet. 70, 1305–1317 (2002).
Menezes, L. F. et al. Polyductin, the PKHD1 gene product, comprises isoforms expressed in plasma membrane, primary cilium, and cytoplasm. Kidney Int. 66, 1345–1355 (2004).
Smith, C. & Graham, J. Congenital medullary cysts of the kidneys with severe refractory anemia. Am. J. Dis. Child. 69, 369–377 (1945).
Fanconi, G., Hanhart, E. & Albertini, A. Die familiäre juvenile Nephronophthise. Hel. Pediatr. Acta 6, 1–49 (1951) (in German).
Hildebrandt, F. in Pediatric Nephrology (ed. Harmon, W. E.) (Williams & Wilkins, Baltimore, 1999).
Sutters, M. et al. Polycystin-1 transforms the cAMP growth-responsive phenotype of M-1 cells. Kidney Int. 60, 484–494 (2001).
Yamaguchi, T. et al. Calcium restriction allows cAMP activation of the B-Raf/ERK pathway, switching cells to a cAMP-dependent growth-stimulated phenotype. J. Biol. Chem. 279, 40419–40430 (2004).
Veis, D. J., Sorenson, C. M., Shutter, J. R. & Korsmeyer, S. J. Bcl-2-deficient mice demonstrate fulminant lymphoid apoptosis, polycystic kidneys, and hypopigmented hair. Cell 75, 229–240 (1993).
Saunier, S. et al. A novel gene that encodes a protein with a putative src homology 3 domain is a candidate gene for familial juvenile nephronophthisis. Hum. Mol. Genet. 6, 2317–2323 (1997).
Mollet, G. et al. The gene mutated in juvenile nephronophthisis type 4 encodes a novel protein that interacts with nephrocystin. Nature Genet. 32, 300–305 (2002).
Otto, E. et al. Nephrocystin: gene expression and sequence conservation between human, mouse, and Caenorhabditis elegans. J. Am. Soc. Nephrol. 11, 270–282 (2000).
Benzing, T. et al. Nephrocystin interacts with Pyk2, p130Cas, and tensin and triggers phosphorylation of Pyk2. Proc. Natl Acad. Sci. USA 98, 9784–9789 (2001).
Donaldson, J. C. et al. Crk-associated substrate p130Cas interacts with nephrocystin and both proteins localize to cell–cell contacts of polarized epithelial cells. Exp. Cell Res. 256, 168–178 (2000).
Donaldson, J. C., Dise, R. S., Ritchie, M. D. & Hanks, S. K. Nephrocystin-conserved domains involved in targeting to epithelial cell–cell junctions, interaction with filamins, and establishing cell polarity. J. Biol. Chem. 277, 29028–29035 (2002).
Mollet, G. et al. Characterization of the nephrocystin/nephrocystin-4 complex and subcellular localization of nephrocystin-4 to primary cilia and centrosomes. Hum. Mol. Genet. 14, 645–656 (2005).
Hildebrandt, F. & Otto, E. Molecular genetics of nephronophthisis and medullary cystic kidney disease. J. Am. Soc. Nephrol. 11, 1753–1761 (2000).
Gagnadoux, M. F., Bacri, J. L., Broyer, M. & Habib, R. Infantile chronic tubulo-interstitial nephritis with cortical microcysts: variant of nephronophthisis or new disease entity? Pediatr. Nephrol. 3, 50–55 (1989).
Haider, N. B., Carmi, R., Shalev, H., Sheffield, V. C. & Landau, D. A Bedouin kindred with infantile nephronophthisis demonstrates linkage to chromosome 9 by homozygosity mapping. Am. J. Hum. Genet. 63, 1404–1410 (1998).
Mochizuki, T. et al. Cloning of inv, a gene that controls left/right asymmetry and kidney development. Nature 395, 177–181 (1998).
Morgan, D. et al. Inversin, a novel gene in the vertebrate left–right axis pathway, is partially deleted in the inv mouse. Nature Genet. 20, 149–156 (1998).
Nauli, S. M. et al. Polycystins 1 and 2 mediate mechanosensation in the primary cilium of kidney cells. Nature Genet. 33, 129–137 (2003).
Omran, H. et al. Identification of a new gene locus for adolescent nephronophthisis, on chromosome 3q22 in a large Venezuelan pedigree. Am. J. Hum. Genet. 66, 118–127 (2000).
Schuermann, M. J. et al. Mapping of gene loci for nephronophthisis type 4 and Senior–Loken syndrome, to chromosome 1p36. Am. J. Hum. Genet. 70, 1240–1246 (2002).
Saraiva, J. M. & Baraitser, M. Joubert syndrome: a review. Am. J. Med. Genet. 43, 726–731 (1992).
Valente, E. M. et al. Distinguishing the four genetic causes of Jouberts syndrome-related disorders. Ann. Neurol. 57, 513–519 (2005).
Gleeson, J. G. et al. Molar tooth sign of the midbrain–hindbrain junction: occurrence in multiple distinct syndromes. Am. J. Med. Genet. 125A, 125–134; discussion 117 (2004).
Parisi, M. A. et al. The NPHP1 gene deletion associated with juvenile nephronophthisis is present in a subset of individuals with Joubert syndrome. Am. J. Hum. Genet. 75, 82–91 (2004).
Saar, K. et al. Homozygosity mapping in families with Joubert syndrome identifies a locus on chromosome 9q34.3 and evidence for genetic heterogeneity. Am. J. Hum. Genet. 65, 1666–1671 (1999).
Keeler, L. C. et al. Linkage analysis in families with Joubert syndrome plus oculo-renal involvement identifies the CORS2 locus on chromosome 11p12–q13.3. Am. J. Hum. Genet. 73, 656–662 (2003).
Lagier-Tourenne, C. et al. Homozygosity mapping of a third Joubert syndrome locus to 6q23. J. Med. Genet. 41, 273–277 (2004).
Natacci, F. et al. Patient with large 17p11.2 deletion presenting with Smith–Magenis syndrome and Joubert syndrome phenotype. Am. J. Med. Genet. 95, 467–472 (2000).
Ferland, R. J. et al. Abnormal cerebellar development and axonal decussation due to mutations in AHI1 in Joubert syndrome. Nature Genet. 36, 1008–1013 (2004).
Mykytyn, K. & Sheffield, V. C. Establishing a connection between cilia and Bardet–Biedl syndrome. Trends Mol. Med. 10, 106–109 (2004).
Kim, J. C. et al. The Bardet–Biedl protein BBS4 targets cargo to the pericentriolar region and is required for microtubule anchoring and cell cycle progression. Nature Genet. 36, 462–470 (2004). The authors demonstrate a central role of BBS4 in the regulation of cell-cycle progression at centrosomes.
Fan, Y. et al. Mutations in a member of the Ras superfamily of small GTP-binding proteins causes Bardet–Biedl syndrome. Nature Genet. 36, 989–993 (2004).
Chiang, A. P. et al. Comparative genomic analysis identifies an ADP-ribosylation factor-like gene as the cause of Bardet–Biedl syndrome (BBS3). Am. J. Hum. Genet. 75, 475–484 (2004).
Li, J. B. et al. Comparative genomics identifies a flagellar and basal body proteome that includes the BBS5 human disease gene. Cell 117, 541–552 (2004). In this study a bioinformatics approach identifes proteins that are expressed specifically in primary cilia, and uses the data together with positional cloning to identify a novel gene that is mutated in BBS5.
Marshall, J. D. et al. New Alstrom syndrome phenotypes based on the evaluation of 182 cases. Arch. Intern. Med. 165, 675–683 (2005).
Collin, G. B. et al. Mutations in ALMS1 cause obesity, type 2 diabetes and neurosensory degeneration in Alstrom syndrome. Nature Genet. 31, 74–78 (2002).
Hearn, T. et al. Mutation of ALMS1, a large gene with a tandem repeat encoding 47 amino acids, causes Alstrom syndrome. Nature Genet. 31, 79–83 (2002).
Andersen, J. S. et al. Proteomic characterization of the human centrosome by protein correlation profiling. Nature 426, 570–574 (2003).
Hearn, T. et al. Subcellular localization of ALMS1 supports involvement of centrosome and basal body dysfunction in the pathogenesis of obesity, insulin resistance, and type 2 diabetes. Diabetes 54, 1581–1587 (2005).
Ferrante, M. I. et al. Identification of the gene for oral–facial–digital type I syndrome. Am. J. Hum. Genet. 68, 569–576 (2001).
Romio, L. et al. OFD1 is a centrosomal/basal body protein expressed during mesenchymal-epithelial transition in human nephrogenesis. J. Am. Soc. Nephrol. 15, 2556–2568 (2004).
Wolf, M. T. et al. Expression and phenotype analysis of the nephrocystin-1 and nephrocystin-4 homologs in Caenorhabditis elegans. J. Am. Soc. Nephrol. 16, 676–687 (2005).
Ansley, S. J. et al. Basal body dysfunction is a likely cause of pleiotropic Bardet–Biedl syndrome. Nature 425, 628–633 (2003). This paper describes a central role of basal body and centrosome localization for proteins that are defective in Bardet–Biedl syndrome.
Barr, M. M. et al. The Caenorhabditis elegans autosomal dominant polycystic kidney disease gene homologs lov-1 and pkd-2 act in the same pathway. Curr. Biol. 11, 1341–1346 (2001). The C. elegans orthologues of human PKD1 and PKD2 are localized at ciliated neurons and, if defective, give rise to a similar male mating phenotype.
Efimenko, E. et al. Analysis of xbx genes in C. elegans. Development 132, 1923–1934 (2005).
Blacque, O. E. et al. Loss of C. elegans BBS-7 and BBS-8 protein function results in cilia defects and compromised intraflagellar transport. Genes Dev. 18, 1630–1642 (2004).
Praetorius, H. A. & Spring, K. R. Bending the MDCK cell primary cilium increases intracellular calcium. J. Membr. Biol. 184, 71–79 (2001).
Praetorius, H. A., Praetorius, J., Nielsen, S., Frokiaer, J. & Spring, K. R. β1-Integrins in the primary cilium of MDCK cells potentiate fibronectin-induced Ca2+ signaling. Am. J. Physiol. Renal Physiol. 287, F969–F978 (2004).
Praetorius, H. A. & Spring, K. R. The renal cell primary cilium functions as a flow sensor. Curr. Opin. Nephrol. Hypertens. 12, 517–520 (2003).
Lin, F. et al. Kidney-specific inactivation of the KIF3A subunit of kinesin-II inhibits renal ciliogenesis and produces polycystic kidney disease. Proc. Natl Acad. Sci. USA 100, 5286–5291 (2003). The first account of the implication of a bona fide motor protein in renal cystic disease in the mouse.
Kramer-Zucker, A. G. et al. Cilia-driven fluid flow in the zebrafish pronephros, brain and Kupffer's vesicle is required for normal organogenesis. Development 132, 1907–1921 (2005). The authors demonstrate that certain renal epithelial cilia in the zebrafish larval kidney, the spinal cord and Kupffer's vesicle are motile, indicating that fluid flow is a common feature of each of these organs.
Brown, N. E. & Murcia, N. S. Delayed cystogenesis and increased ciliogenesis associated with the re-expression of polaris in Tg737 mutant mice. Kidney Int. 63, 1220–1229 (2003).
Hildebrandt, F. Identification of a gene for nephronophthisis. Nephrol. Dial. Transplant. 13, 1334–1336 (1998).
Boletta, A. et al. Polycystin-1, the gene product of PKD1, induces resistance to apoptosis and spontaneous tubulogenesis in MDCK cells. Mol. Cell 6, 1267–1273 (2000).
Simons, M. et al. Inversin, the gene product mutated in nephronophthisis type II, functions as a molecular switch between Wnt signaling pathways. Nature Genet 37, 537–43 (2005). The authors provide evidence for the renal cystic phenotype of nephronophthisis type 2. They show that inversin mutations cause switching from the non-canonical to the canonical Wnt pathway.
Germino, G. G. Linking cilia to Wnts. Nature Genet. 37, 455–457 (2005).
Nurnberger, J., Bacallao, R. L. & Phillips, C. L. Inversin forms a complex with catenins and N-cadherin in polarized epithelial cells. Mol. Biol. Cell 13, 3096–3106 (2002).
Arnould, T. et al. The polycystic kidney disease 1 gene product mediates protein kinase C α-dependent and c-Jun N-terminal kinase-dependent activation of the transcription factor AP-1. J. Biol. Chem. 273, 6013–6018 (1998).
Tsiokas, L., Kim, E., Arnould, T., Sukhatme, V. P. & Walz, G. Homo- and heterodimeric interactions between the gene products of PKD1 and PKD2. Proc. Natl Acad. Sci. USA 94, 6965–6970 (1997).
Parnell, S. C. et al. Polycystin-1 activation of c-Jun N-terminal kinase and AP-1 is mediated by heterotrimeric G proteins. J. Biol. Chem. 277, 19566–19572 (2002).
Dressler, G. Tubulogenesis in the developing mammalian kidney. Trends Cell Biol. 12, 390–395 (2002).
Morgan, D. et al. Expression analyses and interaction with the anaphase promoting complex protein Apc2 suggest a role for inversin in primary cilia and involvement in the cell cycle. Hum. Mol. Genet. 11, 3345–3350 (2002).
Nishimura, D. Y. et al. Bbs2-null mice have neurosensory deficits, a defect in social dominance, and retinopathy associated with mislocalization of rhodopsin. Proc. Natl Acad. Sci. USA 101, 16588–16593 (2004).
Mykytyn, K. et al. Bardet–Biedl syndrome type 4 (BBS4)-null mice implicate Bbs4 in flagella formation but not global cilia assembly. Proc. Natl Acad. Sci. USA 101, 8664–8669 (2004).
Pazour, G. J. & Rosenbaum, J. L. Intraflagellar transport and cilia-dependent diseases. Trends Cell Biol. 12, 551–555 (2002).
Kulaga, H. M. et al. Loss of BBS proteins causes anosmia in humans and defects in olfactory cilia structure and function in the mouse. Nature Genet. 36, 994–998 (2004).
Iannaccone, A. et al. Clinical evidence of decreased olfaction in Bardet–Biedl syndrome caused by a deletion in the BBS4 gene. Am. J. Med. Genet. A 132, 343–346 (2005).
Boichis, H., Passwell, J., David, R. & Miller, H. Congenital hepatic fibrosis and nephronophthisis. A family study. Q. J. Med. 42, 221–233 (1973).
Hirokawa, N. & Takemura, R. Biochemical and molecular characterization of diseases linked to motor proteins. Trends Biochem. Sci. 28, 558–565 (2003).
Tanaka, T. et al. Lis1 and doublecortin function with dynein to mediate coupling of the nucleus to the centrosome in neuronal migration. J. Cell Biol. 165, 709–721 (2004).
Fath, M. A. et al. Mkks-null mice have a phenotype resembling Bardet–Biedl syndrome. Hum. Mol. Genet. 14, 1109–1118 (2005).
McGrath, J., Somlo, S., Makova, S., Tian, X. & Brueckner, M. Two populations of node monocilia initiate left–right asymmetry in the mouse. Cell 114, 61–73 (2003).
Mrug, M. et al. Kinesin family member 12 is a candidate polycystic kidney disease modifier in the cpk mouse. J. Am. Soc. Nephrol. 16, 905–916 (2005).
Pazour, G. J. & Witman, G. B. The vertebrate primary cilium is a sensory organelle. Curr. Opin. Cell Biol. 15, 105–110 (2003).
Stolc, V., Samanta, M. P., Tongprasit, W. & Marshall, W. F. Genome-wide transcriptional analysis of flagellar regeneration in Chlamydomonas reinhardtii identifies orthologs of ciliary disease genes. Proc. Natl Acad. Sci. USA 102, 3703–3707 (2005).
Ostrowski, L. E. et al. A proteomic analysis of human cilia: identification of novel components. Mol. Cell. Proteomics 1, 451–465 (2002).
Li, S. et al. A map of the interactome network of the metazoan C. elegans. Science 303, 540–543 (2004).
Avner, E. D., Woychik, R. P., Dell, K. M. & Sweeney, W. E. Cellular pathophysiology of cystic kidney disease: insight into future therapies. Int. J. Dev. Biol. 43, 457–461 (1999).
Woo, D. D., Miao, S. Y., Pelayo, J. C. & Woolf, A. S. Taxol inhibits progression of congenital polycystic kidney disease. Nature 368, 750–753 (1994).
Gattone, V. H. 2nd, Wang, X., Harris, P. C. & Torres, V. E. Inhibition of renal cystic disease development and progression by a vasopressin V2 receptor antagonist. Nature Med. 9, 1323–1326 (2003). This paper describes the effective treatment of the renal cystic mouse phenoptype pcy (an orthologue of human NPHP3) with a vasopressin V2 receptor antagonist, implicating the level of intracellular cyclic AMP in the pathogenesis of renal cystic disease.
Torres, V. E. et al. Effective treatment of an orthologous model of autosomal dominant polycystic kidney disease. Nature Med. 10, 363–364 (2004).
Hu, J. & Barr, M. M. ATP-2 interacts with the PLAT domain of LOV-1 and is involved in Caenorhabditis elegans polycystin signaling. Mol. Biol. Cell 16, 458–469 (2005).
Kottgen, M. et al. Trafficking of TRPP2 by PACS proteins represents a novel mechanism of ion channel regulation. EMBO J. 24, 705–716 (2005).
Kim, H., Jeong, W., Ahn, K., Ahn, C. & Kang, S. Siah-1 interacts with the intracellular region of polycystin-1 and affects its stability via the ubiquitin–proteasome pathway. J. Am. Soc. Nephrol. 15, 2042–2049 (2004).
Gallagher, A. R., Cedzich, A., Gretz, N., Somlo, S. & Witzgall, R. The polycystic kidney disease protein PKD2 interacts with Hax-1, a protein associated with the actin cytoskeleton. Proc. Natl Acad. Sci. USA 97, 4017–4022 (2000).
Hidaka, S., Konecke, V., Osten, L. & Witzgall, R. PIGEA-14, a novel coiled-coil protein affecting the intracellular distribution of polycystin-2. J. Biol. Chem. 279, 35009–35016 (2004).
Hart, T. C. et al. Mutations of the UMOD gene are responsible for medullary cystic kidney disease 2 and familial juvenile hyperuricaemic nephropathy. J. Med. Genet. 39, 882–892 (2002).
Parisi, M. A. et al. The NPHP1 gene deletion associated with juvenile nephronophthisis is present in a subset of individuals with Joubert syndrome. Am. J. Hum. Genet. 75, 82–91 (2004).
Dixon-Salazar, T. et al. Mutations in the AHI1 gene, encoding jouberin, cause Joubert syndrome with cortical polymicrogyria. Am. J. Hum. Genet. 75, 979–987 (2004).
Mykytyn, K. et al. Identification of the gene (BBS1) most commonly involved in Bardet–Biedl syndrome, a complex human obesity syndrome. Nature Genet. 31, 435–438 (2002).
Mykytyn, K. et al. Identification of the gene that, when mutated, causes the human obesity syndrome BBS4. Nature Genet. 28, 188–191 (2001).
Katsanis, N. et al. Mutations in MKKS cause obesity, retinal dystrophy and renal malformations associated with Bardet–Biedl syndrome. Nature Genet. 26, 67–70 (2000).
Badano, J. L. et al. Identification of a novel Bardet–Biedl syndrome protein, BBS7, that shares structural features with BBS1 and BBS2. Am. J. Hum. Genet. 72, 650–658 (2003).
Romio, L. et al. OFD1, the gene mutated in oral-facial-digital syndrome type 1, is expressed in the metanephros and in human embryonic renal mesenchymal cells. J. Am. Soc. Nephrol. 14, 680–689 (2003).
Wu, G. et al. Trans-heterozygous Pkd1 and Pkd2 mutations modify expression of polycystic kidney disease. Hum. Mol. Genet. 11, 1845–1854 (2002).
Sun, Z. et al. A genetic screen in zebrafish identifies cilia genes as a principal cause of cystic kidney. Development 131, 4085–4093 (2004).
Bleyer, A. J. & Hart, T. C. Medullary cystic kidney disease type 2. Am. J. Kidney Dis. 43, 1142; author reply 1142–1143 (2004).
Bachmann, S. et al. Renal effects of Tamm–Horsfall protein (uromodulin) deficiency in mice. Am. J. Physiol. Renal Physiol. 288, F559–F567 (2005).
Nishimura, D. Y. et al. Positional cloning of a novel gene on chromosome 16q causing Bardet–Biedl syndrome (BBS2). Hum. Mol. Genet. 10, 865–874 (2001).
Atala, A., Freeman, M. R., Mandell, J. & Beier, D. R. Juvenile cystic kidneys (jck): a new mouse mutation which causes polycystic kidneys. Kidney Int. 43, 1081–1085 (1993).
Cogswell, C. et al. Positional cloning of jcpk/bpk locus of the mouse. Mamm. Genome 14, 242–249 (2003).
Upadhya, P., Birkenmeier, E. H., Birkenmeier, C. S. & Barker, J. E. Mutations in a NIMA-related kinase gene, Nek1, cause pleiotropic effects including a progressive polycystic kidney disease in mice. Proc. Natl Acad. Sci. USA 97, 217–221 (2000).
Upadhya, P., Churchill, G., Birkenmeier, E. H., Barker, J. E. & Frankel, W. N. Genetic modifiers of polycystic kidney disease in intersubspecific KAT2J mutants. Genomics 58, 129–137 (1999).
Huangfu, D. et al. Hedgehog signalling in the mouse requires intraflagellar transport proteins. Nature 426, 83–87 (2003).
Lo, S. H., Yu, Q. C., Degenstein, L., Chen, L. B. & Fuchs, E. Progressive kidney degeneration in mice lacking tensin. J. Cell Biol. 136, 1349–1361 (1997).
Carpenter, C. et al. Renal abnormalities in mutant mice. Nature 380, 292 (1996).
Hiesberger, T. et al. Mutation of hepatocyte nuclear factor-1β inhibits Pkhd1 gene expression and produces renal cysts in mice. J. Clin. Invest. 113, 814–825 (2004). This paper demonstrates that many genes implicated in renal cystic disease are under the control of the transcription factor HNF1B.
Pazour, G. J. et al. The intraflagellar transport protein, IFT88, is essential for vertebrate photoreceptor assembly and maintenance. J. Cell Biol. 157, 103–114 (2002).
Acknowledgements
F.H. is supported by the US National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Related links
Glossary
- MODIFIER GENE
-
A gene that has quantitative effects on the phenotype that is controlled by another genetic locus.
- ADHERENS JUNCTION
-
A cell–cell contact site of epithelial cells that contains the protein cadherin and is positioned just underneath the 'tight junction'.
- FOCAL ADHESION
-
A cell–basement membrane cell-contact site of epithelial cells that contains the proteins α-integrin and β-integrin and has a role in signalling processes from the basement membrane to the cell nucleus.
- STAND DOMAIN
-
A widespread class of P-loop NTPases. The signal transduction ATPases with numerous domains (STAND) have been found in proteins that are implicated in apoptosis, plant disease-resistance, pathogen response in animals and plants and transcriptional regulation in bacteria.
- CILIARY TRANSITION ZONE
-
The region between the basal body and the axoneme of a cilium that is structurally not well-characterized.
- AXONEME
-
The bundle of microtubules and other proteins that forms the core of each cilium or flagellum.
- LISSENCEPHALY
-
'Smoothened brain'. A developmental defect of the brain in which the number of infoldings of the brain surface is reduced.
Rights and permissions
About this article
Cite this article
Hildebrandt, F., Otto, E. Cilia and centrosomes: a unifying pathogenic concept for cystic kidney disease?. Nat Rev Genet 6, 928–940 (2005). https://doi.org/10.1038/nrg1727
Issue Date:
DOI: https://doi.org/10.1038/nrg1727
This article is cited by
-
Nephronophthisis: a pathological and genetic perspective
Pediatric Nephrology (2023)
-
Association of Nephronophthisis 4 genetic variation with cardiorenal syndrome and cardiovascular events in Japanese general population: the Yamagata (Takahata) study
Heart and Vessels (2022)
-
Expression patterns of ciliopathy genes ARL3 and CEP120 reveal roles in multisystem development
BMC Developmental Biology (2020)
-
Use of patient derived urine renal epithelial cells to confirm pathogenicity of PKHD1 alleles
BMC Nephrology (2020)
-
Ribosome profiling reveals a functional role for autophagy in mRNA translational control
Communications Biology (2020)