Key Points
-
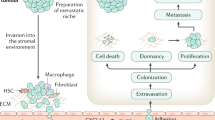
Metastatic tumours represent the greatest threat to the survival of patients with cancer
-
The development of therapies that impede the growth and/or function of tumour cells, while sparing normal host cells, is critical to improving the care of patients with cancer
-
In the case of bone metastases, cells within the bone marrow niche mediate many of the orthopaedic consequences of tumour progression as well as resistance to the antitumour effects of existing therapies
-
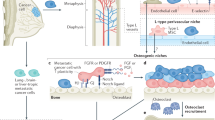
Osteocytes have a key role in the activation and progression of osteolytic metastases
Abstract
In the context of breast cancer, the importance of the skeleton in the regulation of primary tumour development and as a site for subsequent metastasis is well characterized. Our understanding of the contributions made by the host bone and bone marrow cells increasingly demonstrates the extent of the interaction between tumour cells and normal host cells. As a result, the need to develop and utilize therapies that can impede the growth and/or function of tumour cells while sparing normal host bone and bone marrow cells is immense and expanding. The need for these new treatments is, however, superimposed on the orthopaedic management of patients' quality of life, where pain control and continued locomotion are paramount. Indeed, the majority of the anticancer therapies used to date often result in direct or indirect damage to bone. Thus, although the bone microenvironment regulates tumour cell growth in bone, cells within the bone marrow niche also mediate many of the orthopaedic consequences of tumour progression as well as resistance to the antitumour effects of existing therapies. In this Review, we highlight the effects of existing cancer treatments on bone and the bone marrow microenvironment as well as the mechanisms mediating these effects and the current utility of modern orthopaedic interventions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Suva, L. J., Washam, C., Nicholas, R. W. & Griffin, R. J. Bone metastasis: mechanisms and therapeutic opportunities. Nat. Rev. Endocrinol. 7, 208–218 (2011).
Roodman, G. D. Mechanisms of bone metastasis. N. Engl. J. Med. 350, 1655–1664 (2004).
Suva, L. J., Gaddy, D., Perrien, D. S., Thomas, R. L. & Findlay, D. M. Regulation of bone mass by mechanical loading: microarchitecture and genetics. Curr. Osteoporos. Rep. 3, 46–51 (2005).
Shi, H. et al. TLR4 links innate immunity and fatty acid-induced insulin resistance. J. Clin. Invest. 116, 3015–3025 (2006).
Yin, T. & Li, L. The stem cell niches in bone. J. Clin. Invest. 116, 1195–1201 (2006).
Ying, H. et al. Aberrant accumulation of PTTG1 induced by a mutated thyroid hormone β receptor inhibits mitotic progression. J. Clin. Invest. 116, 2972–2984 (2006).
Guise, T. A. et al. Evidence for a causal role of parathyroid hormone-related protein in the pathogenesis of human breast cancer-mediated osteolysis. J. Clin. Invest. 98, 1544–1549 (1996).
Mundy, G. R. & Edwards, J. R. PTH-related peptide (PTHrP) in hypercalcemia. J. Am. Soc. Nephrol. 19, 672–675 (2008).
Kir, S. et al. Tumour-derived PTH-related protein triggers adipose tissue browning and cancer cachexia. Nature 513, 100–104 (2014).
Bonewald, L. F. Osteocyte messages from a bony tomb. Cell Metab. 5, 410–411 (2007).
Dallas, S. L., Prideaux, M. & Bonewald, L. F. The osteocyte: an endocrine cell and more. Endocr. Rev. 34, 658–690 (2013).
Xiong, J. et al. Matrix-embedded cells control osteoclast formation. Nat. Med. 17, 1235–1241 (2011).
Nakashima, T. et al. Evidence for osteocyte regulation of bone homeostasis through RANKL expression. Nat. Med. 17, 1231–1234 (2011).
Mori, G., D'Amelio, P., Faccio, R. & Brunetti, G. Bone–immune cell crosstalk: bone diseases. J. Immunol. Res. 2015, 108451 (2015).
Roato, I. Interaction among cells of bone, immune system, and solid tumors leads to bone metastases. Clin. Dev. Immunol. 2013, 315024 (2013).
Coleman, R. E., Gregory, W., Marshall, H., Wilson, C. & Holen, I. The metastatic microenvironment of breast cancer: clinical implications. Breast 22 (Suppl. 2), S50–S56 (2013).
Hanahan, D. & Weinberg, R. A. Hallmarks of cancer: the next generation. Cell 144, 646–674 (2011).
Klein, C. A. Parallel progression of primary tumours and metastases. Nat. Rev. Cancer 9, 302–312 (2009).
Ramaswamy, S., Ross, K. N., Lander, E. S. & Golub, T. R. A molecular signature of metastasis in primary solid tumors. Nat. Genet. 33, 49–54 (2003).
Kang, Y. et al. A multigenic program mediating breast cancer metastasis to bone. Cancer Cell 3, 537–549 (2003).
Minn, A. J. et al. Distinct organ-specific metastatic potential of individual breast cancer cells and primary tumors. J. Clin. Invest. 115, 44–55 (2005).
Bendre, M. S. et al. Expression of interleukin 8 and not parathyroid hormone-related protein by human breast cancer cells correlates with bone metastasis in vivo. Cancer Res. 62, 5571–5579 (2002).
Paget, S. The distribution of secondary growths in cancer of the breast. Lancet 133, 571–573 (1889).
Sosa, M. S., Bragado, P. & Aguirre-Ghiso, J. A. Mechanisms of disseminated cancer cell dormancy: an awakening field. Nat. Rev. Cancer 14, 611–622 (2014).
Jo, H., Jia, Y., Subramanian, K. K., Hattori, H. & Luo, H. R. Cancer cell-derived clusterin modulates the phosphatidylinositol 3'-kinase–Akt pathway through attenuation of insulin-like growth factor 1 during serum deprivation. Mol. Cell. Biol. 28, 4285–4299 (2008).
Schewe, D. M. & Aguirre-Ghiso, J. A. ATF6α–Rheb–mTOR signaling promotes survival of dormant tumor cells in vivo. Proc. Natl Acad. Sci. USA 105, 10519–10524 (2008).
Mani, S., Wang, C., Wu, K., Francis, R. & Pestell, R. Cyclin-dependent kinase inhibitors: novel anticancer agents. Expert Opin. Investig. Drugs 9, 1849–1870 (2000).
Romero, I., Garrido, F. & Garcia-Lora, A. M. Metastases in immune-mediated dormancy: a new opportunity for targeting cancer. Cancer Res. 74, 6750–6757 (2014).
Muller-Hermelink, N. et al. TNFR1 signaling and IFN-γ signaling determine whether T cells induce tumor dormancy or promote multistage carcinogenesis. Cancer Cell 13, 507–518 (2008).
Coleman, R. E. Clinical features of metastatic bone disease and risk of skeletal morbidity. Clin. Cancer Res. 12, 6243s–6249s (2006).
Kaplan, R. N., Psaila, B. & Lyden, D. Niche-to-niche migration of bone-marrow-derived cells. Trends Mol. Med. 13, 72–81 (2007).
Sheridan, C. et al. CD44+/CD24− breast cancer cells exhibit enhanced invasive properties: an early step necessary for metastasis. Breast Cancer Res. 8, R59 (2006).
Furusato, B., Mohamed, A., Uhlen, M. & Rhim, J. S. CXCR4 and cancer. Pathol. Int. 60, 497–505 (2010).
Cojoc, M. et al. Emerging targets in cancer management: role of the CXCL12/CXCR4 axis. Onco. Targets. Ther. 6, 1347–1361 (2013).
Leon, X., Quer, M., Orus, C., de Dios, E. & Recher, K. Treatment of neck nodes after induction chemotherapy in patients with primary advanced tumours. Eur. Arch. Otorhinolaryngol. 257, 521–525 (2000).
Patten, R. M., Shuman, W. P. & Teefey, S. Metastases from malignant melanoma to the axial skeleton: a CT study of frequency and appearance. AJR Am. J. Roentgenol. 155, 109–112 (1990).
Coussens, L. M. & Werb, Z. Inflammation and cancer. Nature 420, 860–867 (2002).
Stewart, A. F. et al. Quantitative bone histomorphometry in humoral hypercalcemia of malignancy: uncoupling of bone cell activity. J. Clin. Endocrinol. Metab. 55, 219–227 (1982).
Huang, Q. & Ouyang, X. Biochemical-markers for the diagnosis of bone metastasis: a clinical review. Cancer Epidemiol. 36, 94–98 (2012).
Demers, L. M., Costa, L. & Lipton, A. Biochemical markers and skeletal metastases. Clin. Orthop. Relat. Res. 415 (Suppl.) S138–S147 (2003).
Lipton, A. et al. Normalization of bone markers is associated with improved survival in patients with bone metastases from solid tumors and elevated bone resorption receiving zoledronic acid. Cancer 113, 193–201 (2008).
Coleman, R. et al. Bone markers and their prognostic value in metastatic bone disease: clinical evidence and future directions. Cancer Treat. Rev. 34, 629–639 (2008).
Washam, C. L. et al. Identification of PTHrP(12–48) as a plasma biomarker associated with breast cancer bone metastasis. Cancer Epidemiol. Biomarkers Prev. 22, 972–983 (2013).
Martin, T. J. Manipulating the environment of cancer cells in bone: a novel therapeutic approach. J. Clin. Invest. 110, 1399–1401 (2002).
Mundy, G. R. Metastasis to bone: causes, consequences and therapeutic opportunities. Nat. Rev. Cancer 2, 584–593 (2002).
Weilbaecher, K. N., Guise, T. A. & McCauley, L. K. Cancer to bone: a fatal attraction. Nat. Rev. Cancer 11, 411–425 (2011).
Ganguly, S. S., Li, X. & Miranti, C. K. The host microenvironment influences prostate cancer invasion, systemic spread, bone colonization, and osteoblastic metastasis. Front. Oncol. 4, 364 (2014).
Bonewald, L. F. The amazing osteocyte. J. Bone Miner. Res. 26, 229–238 (2011).
Suva, L. J. Sclerostin and the unloading of bone. J. Bone Miner. Res. 24, 1649–1650 (2009).
Wijenayaka, A. R. et al. Sclerostin stimulates osteocyte support of osteoclast activity by a RANKL-dependent pathway. PLoS ONE 6, e25900 (2011).
Compton, J. T. & Lee, F. Y. A review of osteocyte function and the emerging importance of sclerostin. J. Bone Joint Surg. Am. 96, 1659–1668 (2014).
Zhou, J. Z. et al. Differential impact of adenosine nucleotides released by osteocytes on breast cancer growth and bone metastasis. Oncogene 34, 1831–42 (2015).
Henriksen, K., Karsdal, M. A. & Martin, T. J. Osteoclast-derived coupling factors in bone remodeling. Calcif. Tissue Int. 94, 88–97 (2014).
Xiong, J. & O'Brien, C. A. Osteocyte RANKL: new insights into the control of bone remodeling. J. Bone Miner. Res. 27, 499–505 (2012).
Boyde, A., Jones, S. J., Binderman, I. & Harell, A. Scanning electron microscopy of bone cells in culture. Cell Tissue Res. 166, 65–70 (1976).
Jones, S. J. & Boyde, A. Morphological changes of osteoblasts in vitro. Cell Tissue Res. 166, 101–107 (1976).
Gkotzamanidou, M. et al. Sclerostin: a possible target for the management of cancer-induced bone disease. Expert Opin. Ther. Targets. 16, 761–769 (2012).
Mendoza-Villanueva, D., Zeef, L. & Shore, P. Metastatic breast cancer cells inhibit osteoblast differentiation through the Runx2/CBFβ-dependent expression of the Wnt antagonist, sclerostin. Breast Cancer Res. 13, R106 (2011).
Tian, E. et al. The role of the Wnt-signaling antagonist DKK1 in the development of osteolytic lesions in multiple myeloma. N. Engl. J. Med. 349, 2483–2494 (2003).
Sezer, O., Heider, U., Zavrski, I., Kuhne, C. A. & Hofbauer, L. C. RANK ligand and osteoprotegerin in myeloma bone disease. Blood 101, 2094–2098 (2003).
Coluzzi, F., Di Bussolo, E., Mandatori, I. & Mattia, C. Bone metastatic disease: taking aim at new therapeutic targets. Curr. Med. Chem. 18, 3093–3115 (2011).
Terpos, E. et al. Elevated circulating sclerostin correlates with advanced disease features and abnormal bone remodeling in symptomatic myeloma: reduction post-bortezomib monotherapy. Int. J. Cancer 131, 1466–1471 (2012).
McClung, M. R. & Grauer, A. Romosozumab in postmenopausal women with osteopenia. N. Engl. J. Med. 370, 1664–1665 (2014).
McClung, M. R. et al. Romosozumab in postmenopausal women with low bone mineral density. N. Engl. J. Med. 370, 412–420 (2014).
Barbehenn, E. K., Lurie, P. & Wolfe, S. M. Osteosarcoma risk in rats using PTH 1–34. Trends Endocrinol. Metab. 12, 383 (2001).
Okazaki, R. Osteosarcoma in rats receiving long-term PTH injection [Japanese]. Clin. Calcium 13, 42–44 (2003).
Martinez, L. M. et al. Changes in the peripheral blood and bone marrow from untreated advanced breast cancer patients that are associated with the establishment of bone metastases. Clin. Exp. Metastasis 31, 213–232 (2014).
Stine, K. C. et al. Cisplatin inhibits bone healing during distraction osteogenesis. J. Orthop. Res. 32, 464–470 (2014).
Pritchard, C. C., Cheng, H. H. & Tewari, M. MicroRNA profiling: approaches and considerations. Nat. Rev. Genet. 13, 358–369 (2012).
Cortez, M. A. et al. MicroRNAs in body fluids—the mix of hormones and biomarkers. Nat. Rev. Clin. Oncol. 8, 467–477 (2011).
Aleckovic, M. & Kang, Y. Regulation of cancer metastasis by cell-free miRNAs. Biochim. Biophys. Acta 1855, 24–42 (2015).
Gururajan, M. et al. miR-154* and miR-379 in the DLK1–DIO3 microRNA mega-cluster regulate epithelial to mesenchymal transition and bone metastasis of prostate cancer. Clin. Cancer Res. 20, 6559–6569 (2014).
Lin, X., Wang, Z., Zhang, R. & Feng, W. High serum microRNA-335 level predicts aggressive tumor progression and unfavorable prognosis in pediatric acute myeloid leukemia. Clin. Transl Oncol. 17, 358–364 (2015).
Zhao, F. L. et al. Serum overexpression of microRNA-10b in patients with bone metastatic primary breast cancer. J. Int. Med. Res. 40, 859–866 (2012).
Schwarzenbach, H., Nishida, N., Calin, G. A. & Pantel, K. Clinical relevance of circulating cell-free microRNAs in cancer. Nat. Rev. Clin. Oncol. 11, 145–156 (2014).
Ell, B. et al. Tumor-induced osteoclast miRNA changes as regulators and biomarkers of osteolytic bone metastasis. Cancer Cell 24, 542–556 (2013).
Valencia, K. et al. miR-326 associates with biochemical markers of bone turnover in lung cancer bone metastasis. Bone 52, 532–539 (2013).
Van Poznak, C. H. et al. American Society of Clinical Oncology executive summary of the clinical practice guideline update on the role of bone-modifying agents in metastatic breast cancer. J. Clin. Oncol. 29, 1221–1227 (2011).
Burstein, H. J. et al. Adjuvant endocrine therapy for women with hormone receptor-positive breast cancer: American Society of Clinical Oncology clinical practice guideline focused update. J. Clin. Oncol. 32, 2255–2269 (2014).
Bines, J., Oleske, D. M. & Cobleigh, M. A. Ovarian function in premenopausal women treated with adjuvant chemotherapy for breast cancer. J. Clin. Oncol. 14, 1718–1729 (1996).
Bokemeyer, C., Berger, C. C., Kuczyk, M. A. & Schmoll, H. J. Evaluation of long-term toxicity after chemotherapy for testicular cancer. J. Clin. Oncol. 14, 2923–2932 (1996).
Hu, M. I., Gagel, R. F. & Jimenez, C. Bone loss in patients with breast or prostate cancer. Curr. Osteoporos. Rep. 5, 170–178 (2007).
Shahinian, V. B., Kuo, Y. F., Freeman, J. L. & Goodwin, J. S. Risk of fracture after androgen deprivation for prostate cancer. N. Engl. J. Med. 352, 154–164 (2005).
Ottewell, P. D. et al. Castration-induced bone loss triggers growth of disseminated prostate cancer cells in bone. Endocr. Relat. Cancer 21, 769–781 (2014).
Lipton, A., Smith, M. R., Ellis, G. K. & Goessl, C. Treatment-induced bone loss and fractures in cancer patients undergoing hormone ablation therapy: efficacy and safety of denosumab. Clin. Med. Insights Oncol. 6, 287–303 (2012).
Love, R. R. et al. Effects of tamoxifen on bone mineral density in postmenopausal women with breast cancer. N. Engl. J. Med. 326, 852–856 (1992).
Vehmanen, L., Elomaa, I., Blomqvist, C. & Saarto, T. Tamoxifen treatment after adjuvant chemotherapy has opposite effects on bone mineral density in premenopausal patients depending on menstrual status. J. Clin. Oncol. 24, 675–680 (2006).
Hadji, P. Aromatase inhibitor-associated bone loss in breast cancer patients is distinct from postmenopausal osteoporosis. Crit. Rev. Oncol. Hematol. 69, 73–82 (2009).
Suva, L. J. & Makhoul, I. Bone: Will breast cancer chemoprevention stand on 'solid bone'? Nat. Rev. Endocrinol. 11, 138–139 (2015).
Rizzoli, R. et al. Cancer-associated bone disease. Osteoporos. Int. 24, 2929–2953 (2013).
Ottewell, P. D. et al. Zoledronic acid has differential antitumor activity in the pre- and postmenopausal bone microenvironment in vivo. Clin. Cancer Res. 20, 2922–2932 (2014).
Hadji, P., Coleman, R. & Gnant, M. Bone effects of mammalian target of rapamycin (mTOR) inhibition with everolimus. Crit. Rev. Oncol. Hematol. 87, 101–111 (2013).
Sieber, P. R., Keiller, D. L., Kahnoski, R. J., Gallo, J. & McFadden, S. Bicalutamide 150 mg maintains bone mineral density during monotherapy for localized or locally advanced prostate cancer. J. Urol. 171, 2272–2276 (2004).
Eswaraka, J. et al. Axitinib and crizotinib combination therapy inhibits bone loss in a mouse model of castration resistant prostate cancer. BMC Cancer 14, 742 (2014).
Aleman, J. O., Farooki, A. & Girotra, M. Effects of tyrosine kinase inhibition on bone metabolism: untargeted consequences of targeted therapies. Endocr. Relat. Cancer 21, R247–R259 (2014).
Oh, D. & Huh, S. J. Insufficiency fracture after radiation therapy. Radiat. Oncol. J. 32, 213–220 (2014).
Lipton, A. et al. Advances in treating metastatic bone cancer: summary statement for the first Cambridge conference. Clin. Cancer Res. 12, 6209s–6212s (2006).
Guise, T. A. et al. Molecular mechanisms of breast cancer metastases to bone. Clin. Breast Cancer 5 (Suppl. 2), S46–S53 (2005).
Yong, M. et al. Survival in breast cancer patients with bone metastases and skeletal-related events: a population-based cohort study in Denmark (1999–2007). Breast Cancer Res. Treat. 129, 495–503 (2011).
Hortobagyi, G. N. et al. Long-term prevention of skeletal complications of metastatic breast cancer with pamidronate. Protocol 19 Aredia Breast Cancer Study Group. J. Clin. Oncol. 16, 2038–2044 (1998).
Theriault, R. L. et al. Pamidronate reduces skeletal morbidity in women with advanced breast cancer and lytic bone lesions: a randomized, placebo-controlled trial. Protocol 18 Aredia Breast Cancer Study Group. J. Clin. Oncol. 17, 846–854 (1999).
Rosen, L. S. et al. Long-term efficacy and safety of zoledronic acid compared with pamidronate disodium in the treatment of skeletal complications in patients with advanced multiple myeloma or breast carcinoma: a randomized, double-blind, multicenter, comparative trial. Cancer 98, 1735–1744 (2003).
Tombal, B. Assessing the benefit of bone-targeted therapies in prostate cancer, is the devil in the end point's definition? Ann. Oncol. 26, 257–258 (2015).
Parker, C. et al. Alpha emitter radium-223 and survival in metastatic prostate cancer. N. Engl. J. Med. 369, 213–223 (2013).
Smith, M. R. et al. Denosumab for the prevention of skeletal complications in metastatic castration-resistant prostate cancer: comparison of skeletal-related events and symptomatic skeletal events. Ann. Oncol. 26, 368–374 (2015).
Jung, K. & Lein, M. Bone turnover markers in serum and urine as diagnostic, prognostic and monitoring biomarkers of bone metastasis. Biochim. Biophys. Acta 1846, 425–438 (2014).
Barnadas, A. et al. Bone turnover markers as predictive indicators of outcome in patients with breast cancer and bone metastases treated with bisphosphonates: results from a 2-year multicentre observational study (ZOMAR study). Bone 68, 32–40 (2014).
Lara, P. N. Jr et al. Serum biomarkers of bone metabolism in castration-resistant prostate cancer patients with skeletal metastases: results from SWOG 0421. J. Natl Cancer Inst. 106, dju013 (2014).
Eisenhauer, E. A. et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur. J. Cancer 45, 228–247 (2009).
Baron, R., Ferrari, S. & Russell, R. G. Denosumab and bisphosphonates: different mechanisms of action and effects. Bone 48, 677–692 (2011).
Valachis, A. et al. Adjuvant therapy with zoledronic acid in patients with breast cancer: a systematic review and meta-analysis. Oncologist 18, 353–361 (2013).
Ottewell, P. D. et al. Combination therapy inhibits development and progression of mammary tumours in immunocompetent mice. Breast Cancer Res. Treat. 133, 523–536 (2012).
Insalaco, L. et al. Analysis of molecular mechanisms and anti-tumoural effects of zoledronic acid in breast cancer cells. J. Cell. Mol. Med. 16, 2186–2195 (2012).
Green, J. & Lipton, A. Anticancer properties of zoledronic acid. Cancer Invest. 28, 944–957 (2010).
Welton, J. L. et al. γδ T cells predict outcome in zoledronate-treated breast cancer patients. Oncologist 18, e22–e23 (2013).
Foroni, C. et al. Pure anti-tumor effect of zoledronic acid in naive bone-only metastatic and locally advanced breast cancer: proof from the “biological window therapy”. Breast Cancer Res. Treat. 144, 113–121 (2014).
Welton, J. L. et al. Monocytes and γδ T cells control the acute-phase response to intravenous zoledronate: insights from a phase IV safety trial. J. Bone Miner. Res. 28, 464–471 (2013).
Coleman, R. et al. Zoledronic acid (zoledronate) for postmenopausal women with early breast cancer receiving adjuvant letrozole (ZO-FAST study): final 60-month results. Ann. Oncol. 24, 398–405 (2013).
Gnant, M. et al. Adjuvant denosumab in breast cancer (ABCSG-18): a multicentre, randomised, double-blind, placebo-controlled trial. Lancet 386, 433–443 (2015).
Lester, J. E. et al. Prevention of anastrozole-induced bone loss with monthly oral ibandronate during adjuvant aromatase inhibitor therapy for breast cancer. Clin. Cancer Res. 14, 6336–6342 (2008).
Van Poznak, C. et al. Prevention of aromatase inhibitor-induced bone loss using risedronate: the SABRE trial. J. Clin. Oncol. 28, 967–975 (2010).
Smith, M. R. et al. Pamidronate to prevent bone loss during androgen-deprivation therapy for prostate cancer. N. Engl. J. Med. 345, 948–955 (2001).
Smith, M. R. et al. Denosumab in men receiving androgen-deprivation therapy for prostate cancer. N. Engl. J. Med. 361, 745–755 (2009).
Gnant, M. et al. Endocrine therapy plus zoledronic acid in premenopausal breast cancer. N. Engl. J. Med. 360, 679–691 (2009).
Coleman, R. E. et al. Breast-cancer adjuvant therapy with zoledronic acid. N. Engl. J. Med. 365, 1396–1405 (2011).
Powles, T. et al. Reduction in bone relapse and improved survival with oral clodronate for adjuvant treatment of operable breast cancer [ISRCTN83688026]. Breast Cancer Res. 8, R13 (2006).
Paterson, A. H. et al. Oral clodronate for adjuvant treatment of operable breast cancer (National Surgical Adjuvant Breast and Bowel Project protocol B–34): a multicentre, placebo-controlled, randomised trial. Lancet Oncol. 13, 734–742 (2012).
Denham, J. W. et al. Impact of androgen suppression and zoledronic acid on bone mineral density and fractures in the Trans-Tasman Radiation Oncology Group (TROG) 03.04 Randomised Androgen Deprivation and Radiotherapy (RADAR) randomized controlled trial for locally advanced prostate cancer. BJU Int. 114, 344–353 (2014).
Tombal, B. Zometa European Study (ZEUS): another failed crusade for the holy grail of prostate cancer bone metastases prevention? Eur. Urol. 67, 492–494 (2015).
Wirth, M. et al. Prevention of bone metastases in patients with high-risk nonmetastatic prostate cancer treated with zoledronic acid: efficacy and safety results of the Zometa European Study (ZEUS). Eur. Urol. 67, 482–491 (2015).
Smith, M. R. et al. Denosumab and bone-metastasis-free survival in men with castration-resistant prostate cancer: results of a phase 3, randomised, placebo-controlled trial. Lancet 379, 39–46 (2012).
Wong, M. H., Stockler, M. R. & Pavlakis, N. Bisphosphonates and other bone agents for breast cancer. Cochrane Database of Systematic Reviews, Issue 2, Art. No.: CD003474 http://dx.doi.org/10.1002/14651858.CD003474.pub3.
Coleman, R. et al. Adjuvant zoledronic acid in patients with early breast cancer: final efficacy analysis of the AZURE (BIG 01/04) randomised open-label phase 3 trial. Lancet Oncol. 15, 997–1006 (2014).
Todenhofer, T., Stenzl, A., Hofbauer, L. C. & Rachner, T. D. Targeting bone metabolism in patients with advanced prostate cancer: current options and controversies. Int. J. Endocrinol. 2015, 838202 (2015).
Saad, F., Karakiewicz, P. & Perrotte, P. The role of bisphosphonates in hormone-refractory prostate cancer. World J. Urol. 23, 14–18 (2005).
Berenson, J. R. et al. Zoledronic acid reduces skeletal-related events in patients with osteolytic metastases. Cancer 91, 1191–1200 (2001).
Saad, F. et al. A randomized, placebo-controlled trial of zoledronic acid in patients with hormone-refractory metastatic prostate carcinoma. J. Natl Cancer Inst. 94, 1458–1468 (2002).
Saad, F. et al. Long-term efficacy of zoledronic acid for the prevention of skeletal complications in patients with metastatic hormone-refractory prostate cancer. J. Natl Cancer Inst. 96, 879–882 (2004).
Fizazi, K. et al. Randomized phase II trial of denosumab in patients with bone metastases from prostate cancer, breast cancer, or other neoplasms after intravenous bisphosphonates. J. Clin. Oncol. 27, 1564–1571 (2009).
Henry, D. H. et al. Randomized, double-blind study of denosumab versus zoledronic acid in the treatment of bone metastases in patients with advanced cancer (excluding breast and prostate cancer) or multiple myeloma. J. Clin. Oncol. 29, 1125–1132 (2011).
Snedecor, S. J., Carter, J. A., Kaura, S. & Botteman, M. F. Cost-effectiveness of denosumab versus zoledronic acid in the management of skeletal metastases secondary to breast cancer. Clin. Ther. 34, 1334–1349 (2012).
Gralow, J. R. et al. NCCN Task Force report: bone health in cancer care. J. Natl Compr. Canc. Netw. 11 (Suppl. 3), S1–S50 (2013).
Suva, L. J., Brander, B. E. & Makhoul, I. Update on bone-modifying agents in metastatic breast cancer. Nat. Rev. Endocrinol. 7, 380–381 (2011).
Serafini, A. N. et al. Palliation of pain associated with metastatic bone cancer using samarium-153 lexidronam: a double-blind placebo-controlled clinical trial. J. Clin. Oncol. 16, 1574–1581 (1998).
Sartor, O., Reid, R. H., Bushnell, D. L., Quick, D. P. & Ell, P. J. Safety and efficacy of repeat administration of samarium Sm-153 lexidronam to patients with metastatic bone pain. Cancer 109, 637–643 (2007).
Longo, J., Lutz, S. & Johnstone, C. Samarium-153-ethylene diamine tetramethylene phosphonate, a β-emitting bone-targeted radiopharmaceutical, useful for patients with osteoblastic bone metastases. Cancer Manag. Res. 5, 235–242 (2013).
Silberstein, E. B., Eugene, L. & Saenger, S. R. Painful osteoblastic metastases: the role of nuclear medicine. Oncology (Williston Park) 15, 157–163 (2001).
Baczyk, M. Radioisotope therapy of bone metastases. Nucl. Med. Rev. Cent. East Eur. 14, 96–104 (2011).
Nilsson, S. et al. Two-year survival follow-up of the randomized, double-blind, placebo-controlled phase II study of radium-223 chloride in patients with castration-resistant prostate cancer and bone metastases. Clin. Genitourin. Cancer 11, 20–26 (2013).
Shirley, M. & McCormack, P. L. Radium-223 dichloride: a review of its use in patients with castration-resistant prostate cancer with symptomatic bone metastases. Drugs 74, 579–586 (2014).
Coleman, R. E. et al. Bone scan flare predicts successful systemic therapy for bone metastases. J. Nucl. Med. 29, 1354–1359 (1988).
Carducci, M. A. & Jimeno, A. Targeting bone metastasis in prostate cancer with endothelin receptor antagonists. Clin. Cancer Res. 12, 6296s–6300s (2006).
Clines, G. A. et al. Regulation of postnatal trabecular bone formation by the osteoblast endothelin A receptor. J. Bone Miner. Res. 26, 2523–2536 (2011).
Nelson, J. B. et al. Phase 3, randomized, controlled trial of atrasentan in patients with nonmetastatic, hormone-refractory prostate cancer. Cancer 113, 2478–2487 (2008).
Nelson, J. B. et al. Phase 3, randomized, placebo-controlled study of zibotentan (ZD4054) in patients with castration-resistant prostate cancer metastatic to bone. Cancer 118, 5709–5718 (2012).
Quinn, D. I. et al. Docetaxel and atrasentan versus docetaxel and placebo for men with advanced castration-resistant prostate cancer (SWOG S0421): a randomised phase 3 trial. Lancet Oncol. 14, 893–900 (2013).
Miller, K. et al. Phase III, randomized, placebo-controlled study of once-daily oral zibotentan (ZD4054) in patients with non-metastatic castration-resistant prostate cancer. Prostate Cancer Prostatic Dis. 16, 187–192 (2013).
Duong, L. T., Wesolowski, G. A., Leung, P., Oballa, R. & Pickarski, M. Efficacy of a cathepsin K inhibitor in a preclinical model for prevention and treatment of breast cancer bone metastasis. Mol. Cancer Ther. 13, 2898–2909 (2014).
Bonnick, S. et al. Effects of odanacatib on BMD and safety in the treatment of osteoporosis in postmenopausal women previously treated with alendronate: a randomized placebo-controlled trial. J. Clin. Endocrinol. Metab. 98, 4727–4735 (2013).
Jensen, A. B. et al. The cathepsin K inhibitor odanacatib suppresses bone resorption in women with breast cancer and established bone metastases: results of a 4-week, double-blind, randomized, controlled trial. Clin. Breast Cancer 10, 452–458 (2010).
Aftab, D. T. & McDonald, D. M. MET and VEGF: synergistic targets in castration-resistant prostate cancer. Clin. Transl. Oncol. 13, 703–709 (2011).
Zhang, S. et al. Vascular endothelial growth factor regulates myeloid cell leukemia-1 expression through neuropilin-1-dependent activation of c-MET signaling in human prostate cancer cells. Mol. Cancer 9, 9 (2010).
Kabbarah, O. et al. Integrative genome comparison of primary and metastatic melanomas. PLoS ONE 5, e10770 (2010).
Vergani, E. et al. Identification of MET and SRC activation in melanoma cell lines showing primary resistance to PLX4032. Neoplasia 13, 1132–1142 (2011).
Chu, G. C. et al. RANK- and c-Met-mediated signal network promotes prostate cancer metastatic colonization. Endocr. Relat. Cancer 21, 311–326 (2014).
Smith, M. R. et al. Cabozantinib in chemotherapy-pretreated metastatic castration-resistant prostate cancer: results of a phase II nonrandomized expansion study. J. Clin. Oncol. 32, 3391–3399 (2014).
Liu, P., Cheng, H., Roberts, T. M. & Zhao, J. J. Targeting the phosphoinositide 3-kinase pathway in cancer. Nat. Rev. Drug Discov. 8, 627–644 (2009).
Yue, W., Fan, P., Wang, J., Li, Y. & Santen, R. J. Mechanisms of acquired resistance to endocrine therapy in hormone-dependent breast cancer cells. J. Steroid Biochem. Mol. Biol. 106, 102–110 (2007).
Ma, J., Li, M., Hock, J. & Yu, X. Hyperactivation of mTOR critically regulates abnormal osteoclastogenesis in neurofibromatosis type 1. J. Orthop. Res. 30, 144–152 (2012).
Indo, Y. et al. Metabolic regulation of osteoclast differentiation and function. J. Bone Miner. Res. 28, 2392–2399 (2013).
Ory, B., Moriceau, G., Redini, F. & Heymann, D. mTOR inhibitors (rapamycin and its derivatives) and nitrogen containing bisphosphonates: bi-functional compounds for the treatment of bone tumours. Curr. Med. Chem. 14, 1381–1387 (2007).
Glantschnig, H., Fisher, J. E., Wesolowski, G., Rodan, G. A. & Reszka, A. A. M-CSF, TNFα and RANK ligand promote osteoclast survival by signaling through mTOR/S6 kinase. Cell Death Differ. 10, 1165–1177 (2003).
Kneissel, M. et al. Everolimus suppresses cancellous bone loss, bone resorption, and cathepsin K expression by osteoclasts. Bone 35, 1144–1156 (2004).
Gnant, M. et al. Effect of everolimus on bone marker levels and progressive disease in bone in BOLERO-2. J. Natl Cancer Inst. 105, 654–663 (2013).
Clevers, H., Loh, K. M. & Nusse, R. Stem cell signaling. An integral program for tissue renewal and regeneration: Wnt signaling and stem cell control. Science 346, 1248012 (2014).
Lehmann, B. D. et al. Identification of human triple-negative breast cancer subtypes and preclinical models for selection of targeted therapies. J. Clin. Invest. 121, 2750–2767 (2011).
Khramtsov, A. I. et al. Wnt/β-catenin pathway activation is enriched in basal-like breast cancers and predicts poor outcome. Am. J. Pathol. 176, 2911–2920 (2010).
Cui, Y. et al. Lrp5 functions in bone to regulate bone mass. Nat. Med. 17, 684–691 (2011).
Holmen, S. L. et al. Essential role of β-catenin in postnatal bone acquisition. J. Biol. Chem. 280, 21162–21168 (2005).
Goldring, S. R. & Goldring, M. B. Eating bone or adding it: the Wnt pathway decides. Nat. Med. 13, 133–134 (2007).
Bu, G. et al. Breast cancer-derived Dickkopf1 inhibits osteoblast differentiation and osteoprotegerin expression: implication for breast cancer osteolytic bone metastases. Int. J. Cancer 123, 1034–1042 (2008).
Sukhdeo, K. et al. Targeting the β-catenin/TCF transcriptional complex in the treatment of multiple myeloma. Proc. Natl Acad. Sci. USA 104, 7516–7521 (2007).
Fulciniti, M. et al. Anti-DKK1 mAb (BHQ880) as a potential therapeutic agent for multiple myeloma. Blood 114, 371–379 (2009).
Zhou, X. L., Qin, X. R., Zhang, X. D. & Ye, L. H. Downregulation of Dickkopf-1 is responsible for high proliferation of breast cancer cells via losing control of Wnt/β-catenin signaling. Acta Pharmacol. Sin. 31, 202–210 (2010).
Krause, U., Ryan, D. M., Clough, B. H. & Gregory, C. A. An unexpected role for a Wnt-inhibitor: Dickkopf-1 triggers a novel cancer survival mechanism through modulation of aldehyde-dehydrogenase-1 activity. Cell Death Dis. 5, e1093 (2014).
Kim, H. et al. Regulation of Wnt signaling activity for growth suppression induced by quercetin in 4T1 murine mammary cancer cells. Int. J. Oncol. 43, 1319–1325 (2013).
Zhang, H. et al. Parathyroid hormone-related protein inhibits DKK1 expression through c-Jun-mediated inhibition of β-catenin activation of the DKK1 promoter in prostate cancer. Oncogene 33, 2464–2477 (2014).
Thudi, N. K. et al. Dickkopf-1 (DKK-1) stimulated prostate cancer growth and metastasis and inhibited bone formation in osteoblastic bone metastases. Prostate 71, 615–625 (2011).
Rougraff, B. T., Kneisl, J. S. & Simon, M. A. Skeletal metastases of unknown origin. A prospective study of a diagnostic strategy. J. Bone Joint Surg. Am. 75, 1276–1281 (1993).
Issack, P. S., Kotwal, S. Y. & Lane, J. M. Management of metastatic bone disease of the acetabulum. J. Am. Acad. Orthop. Surg. 21, 685–695 (2013).
Gainor, B. J. & Buchert, P. Fracture healing in metastatic bone disease. Clin. Orthop. Relat. Res. 178, 297–302 (1983).
Mirels, H. Metastatic disease in long bones. A proposed scoring system for diagnosing impending pathologic fractures. Clin. Orthop. Relat. Res. 249, 256–264 (1989).
Bickels, J., Dadia, S. & Lidar, Z. Surgical management of metastatic bone disease. J. Bone Joint Surg. Am. 91, 1503–1516 (2009).
Scolaro, J. A. & Lackman, R. D. Surgical management of metastatic long bone fractures: principles and techniques. J. Am. Acad. Orthop. Surg. 22, 90–100 (2014).
Ward, W. G., Holsenbeck, S., Dorey, F. J., Spang, J. & Howe, D. Metastatic disease of the femur: surgical treatment. Clin. Orthop. Relat. Res. 415 (Suppl.), S230–S244 (2003).
Damron, T. A. et al. Critical evaluation of Mirels' rating system for impending pathologic fractures. Clin. Orthop. Relat. Res. 415 (Suppl.), S201–S207 (2003).
Sampson, E., Brierley, J. D., Le, L. W., Rotstein, L. & Tsang, R. W. Clinical management and outcome of papillary and follicular (differentiated) thyroid cancer presenting with distant metastasis at diagnosis. Cancer 110, 1451–1456 (2007).
Baloch, K. G., Grimer, R. J., Carter, S. R. & Tillman, R. M. Radical surgery for the solitary bony metastasis from renal-cell carcinoma. J. Bone Joint Surg. Br. 82, 62–67 (2000).
Lutz, S. T., Jones, J. & Chow, E. Role of radiation therapy in palliative care of the patient with cancer. J. Clin. Oncol. 32, 2913–2919 (2014).
Townsend, P. W., Rosenthal, H. G., Smalley, S. R., Cozad, S. C. & Hassanein, R. E. Impact of postoperative radiation therapy and other perioperative factors on outcome after orthopedic stabilization of impending or pathologic fractures due to metastatic disease. J. Clin. Oncol. 12, 2345–2350 (1994).
Tomita, K. et al. Surgical strategy for spinal metastases. Spine (Phila. Pa 1976) 26, 298–306 (2001).
Fourney, D. R. et al. Spinal instability neoplastic score: an analysis of reliability and validity from the spine oncology study group. J. Clin. Oncol. 29, 3072–3077 (2011).
Tokuhashi, Y., Matsuzaki, H., Oda, H., Oshima, M. & Ryu, J. A revised scoring system for preoperative evaluation of metastatic spine tumor prognosis. Spine (Phila. Pa 1976) 30, 2186–2191 (2005).
Berenson, J. et al. Balloon kyphoplasty versus non-surgical fracture management for treatment of painful vertebral body compression fractures in patients with cancer: a multicentre, randomised controlled trial. Lancet Oncol. 12, 225–235 (2011).
Kaloostian, P. E., Yurter, A., Zadnik, P. L., Sciubba, D. M. & Gokaslan, Z. L. Current paradigms for metastatic spinal disease: an evidence-based review. Ann. Surg. Oncol. 21, 248–262 (2014).
Patchell, R. A. et al. Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: a randomised trial. Lancet 366, 643–648 (2005).
Paice, J. A. & Ferrell, B. The management of cancer pain. CA Cancer J. Clin. 61, 157–182 (2011).
Howell, D. D. et al. Single-fraction radiotherapy versus multifraction radiotherapy for palliation of painful vertebral bone metastases-equivalent efficacy, less toxicity, more convenient: a subset analysis of Radiation Therapy Oncology Group trial 97–14. Cancer 119, 888–896 (2013).
Ejima, Y., Matsuo, Y. & Sasaki, R. The current status and future of radiotherapy for spinal bone metastases. J. Orthop. Sci. 20, 585–592 (2015).
Lutz, S. et al. Palliative radiotherapy for bone metastases: an ASTRO evidence-based guideline. Int. J. Radiat. Oncol. Biol. Phys. 79, 965–976 (2011).
Barlogie, B. et al. Treatment of multiple myeloma. Blood 103, 20–32 (2004).
Zangari, M. et al. A prospective evaluation of the biochemical, metabolic, hormonal and structural bone changes associated with bortezomib response in multiple myeloma patients. Haematologica 96, 333–336 (2011).
Roodman, G. D. Bone-breaking cancer treatment. Nat. Med. 13, 25–26 (2007).
Manso, L. et al. Use of bevacizumab as a first-line treatment for metastatic breast cancer. Curr. Oncol. 22, e51–e60 (2015).
Moreno-Aspitia, A. et al. Phase II trial of sorafenib in patients with metastatic breast cancer previously exposed to anthracyclines or taxanes: North Central Cancer Treatment Group and Mayo Clinic Trial N0336. J. Clin. Oncol. 27, 11–15 (2009).
Curigliano, G. et al. Randomized phase II study of sunitinib versus standard of care for patients with previously treated advanced triple-negative breast cancer. Breast 22, 650–656 (2013).
Coleman, R. E. Risks and benefits of bisphosphonates. Br. J. Cancer 98, 1736–1740 (2008).
Lipton, A. et al. Randomized active-controlled phase II study of denosumab efficacy and safety in patients with breast cancer-related bone metastases. J. Clin. Oncol. 25, 4431–4437 (2007).
Coombes, R. C. et al. An open-label study of lapatinib in women with HER-2-negative early breast cancer: the lapatinib pre-surgical study (LPS study). Ann. Oncol. 24, 924–930 (2013).
Small, E. J. et al. Placebo-controlled phase III trial of immunologic therapy with sipuleucel-T (APC8015) in patients with metastatic, asymptomatic hormone refractory prostate cancer. J. Clin. Oncol. 24, 3089–3094 (2006).
Madan, R. A. et al. Ipilimumab and a poxviral vaccine targeting prostate-specific antigen in metastatic castration-resistant prostate cancer: a phase 1 dose-escalation trial. Lancet Oncol. 13, 501–508 (2012).
van den Eertwegh, A. J. et al. Combined immunotherapy with granulocyte-macrophage colony-stimulating factor-transduced allogeneic prostate cancer cells and ipilimumab in patients with metastatic castration-resistant prostate cancer: a phase 1 dose-escalation trial. Lancet Oncol. 13, 509–517 (2012).
Telli, M. L. et al. Phase II Study of gemcitabine, carboplatin, and iniparib as neoadjuvant therapy for triple-negative and BRCA1/2 mutation-associated breast cancer with assessment of a tumor-based measure of genomic instability: PrECOG 0105. J. Clin. Oncol. 33, 1895–1901 (2015).
Dittrich, C. et al. A phase II multicenter study of two different dosages of pemetrexed given in combination with cyclophosphamide as first-line treatment in patients with locally advanced or metastatic breast cancer. Cancer Invest. 30, 309–316 (2012).
Smith, J. W. 2nd et al. Results of a phase II open-label, nonrandomized trial of oral satraplatin in patients with metastatic breast cancer. Breast Cancer Res. Treat. 118, 361–367 (2009).
Dagher, R. et al. Approval summary: docetaxel in combination with prednisone for the treatment of androgen-independent hormone-refractory prostate cancer. Clin. Cancer Res. 10, 8147–8151 (2004).
Villanueva, C. et al. A multicentre dose-escalating study of cabazitaxel (XRP6258) in combination with capecitabine in patients with metastatic breast cancer progressing after anthracycline and taxane treatment: a phase I/II study. Eur. J. Cancer 47, 1037–1045 (2011).
Acknowledgements
The authors' work on the mechanisms driving tumour progression and the development of bone metastases is supported by the NIH (grant R01 CA166060 to L.J.S.) and the Carl L. Nelson Endowed Chair in Orthopaedic Creativity (L.J.S.).
Author information
Authors and Affiliations
Contributions
I.M., C.O.M., D.G. and L.J.S. researched data for the article, made substantial contributions to discussions of the content, wrote the article and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Makhoul, I., Montgomery, C., Gaddy, D. et al. The best of both worlds — managing the cancer, saving the bone. Nat Rev Endocrinol 12, 29–42 (2016). https://doi.org/10.1038/nrendo.2015.185
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrendo.2015.185
This article is cited by
-
Bisphosphonate use in the horse: what is good and what is not?
BMC Veterinary Research (2019)
-
Hallmarks of Bone Metastasis
Calcified Tissue International (2018)
-
Therapy for bone metastasis from different cancers ⁎
Oncology and Translational Medicine (2016)