Abstract
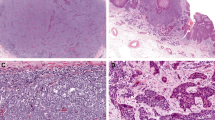
Merkel cell carcinoma (MCC) is a rare but highly aggressive skin cancer with neuroendocrine features. MCC pathogenesis is associated with either the presence of Merkel cell polyomavirus or chronic exposure to ultraviolet light (UV), which can cause a characteristic pattern of multiple DNA mutations. Notably, in the Northern hemisphere, the majority of MCC cases are of viral aetiology; by contrast, in areas with high UV exposure, UV-mediated carcinogenesis is predominant. The two aetiologies share similar clinical, histopathological and prognostic characteristics. MCC presents with a solitary cutaneous or subcutaneous nodule, most frequently in sun-exposed areas. In fact, UV exposure is probably involved in both viral-mediated and non-viral-mediated carcinogenesis, by contributing to immunosuppression or DNA damage, respectively. Confirmation of diagnosis relies on analyses of histological features and immunological marker expression profiles of the lesion. At primary diagnosis, loco-regional metastases are already present in ∼30% of patients. Excision of the tumour is the first-line therapy; if not feasible, radiotherapy can often effectively control the disease. Chemotherapy was the only alternative in advanced-stage or refractory MCC until several clinical trials demonstrated the efficacy of immune-checkpoint inhibitors.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 1 digital issues and online access to articles
$99.00 per year
only $99.00 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Toker, C. Trabecular carcinoma of the skin. Arch. Dermatol. 105, 107–110 (1972).
Maricich, S. M. et al. Merkel cells are essential for light-touch responses. Science 324, 1580–1582 (2009). This study demonstrates that Merkel cells are essential for gentle touch reception.
Lemos, B. D. et al. Pathologic nodal evaluation improves prognostic accuracy in Merkel cell carcinoma: analysis of 5823 cases as the basis of the first consensus staging system. J. Am. Acad. Dermatol. 63, 751–761 (2010).
Schrama, D. et al. Merkel cell polyomavirus status is not associated with clinical course of Merkel cell carcinoma. J. Invest. Dermatol. 131, 1631–1638 (2011).
Becker, J. C., Schrama, D. & zur Hausen, A. in Rook's Textbook of Dermatology, 9 Vol. 12 Ch. 145 (eds Griffiths, C., Barker, J., Bleiker, T., Chalmers, R. & Creamer, D. ) (John Wiley & Sons, Inc., 2016).
Kaae, J. et al. Merkel cell carcinoma: incidence, mortality, and risk of other cancers. J. Natl Cancer Inst. 102, 793–801 (2010).
Harms, P. W. et al. The distinctive mutational spectra of polyomavirus-negative Merkel cell carcinoma. Cancer Res. 75, 3720–3727 (2015). The first report to demonstrate the strong UV mutational signature in MCPyV− MCC and absence of UV mutational signature in MCPyV+ MCC.
Kukko, H. et al. Merkel cell carcinoma — a population-based epidemiological study in Finland with a clinical series of 181 cases. Eur. J. Cancer 48, 737–742 (2012).
Agelli, M. & Clegg, L. X. Epidemiology of primary Merkel cell carcinoma in the United States. J. Am. Acad. Dermatol. 49, 832–841 (2003).
Hodgson, N. C. Merkel cell carcinoma: changing incidence trends. J. Surg. Oncol. 89, 1–4 (2005).
Girschik, J., Thorn, K., Beer, T. W., Heenan, P. J. & Fritschi, L. Merkel cell carcinoma in Western Australia: a population-based study of incidence and survival. Br. J. Dermatol. 165, 1051–1057 (2011).
Zaar, O., Gillstedt, M., Lindelöf, B., Wennberg-Larkö, A.-M. & Paoli, J. Merkel cell carcinoma incidence is increasing in Sweden. J. Eur. Acad. Dermatol. Venereol. 30, 1708–1713 (2016).
Youlden, D. R., Soyer, H. P., Youl, P. H., Fritschi, L. & Baade, P. D. Incidence and survival for Merkel cell carcinoma in Queensland, Australia, 1993–2010. JAMA Dermatol. 150, 864–872 (2014).
Soltani, A. M., Allan, B. J., Best, M. J., Panthaki, Z. J. & Thaller, S. R. Merkel cell carcinoma of the hand and upper extremity: current trends and outcomes. J. Plast. Reconstr. Aesthet. Surg. 67, e71–e77 (2014).
Harms, K. L. et al. Analysis of prognostic factors from 9387 Merkel cell carcinoma cases forms the basis for the new 8 th edition AJCC staging system. Ann. Surg. Oncol. 23, 3564–3571 (2016).
Fields, R. C. et al. Five hundred patients with Merkel cell carcinoma evaluated at a single institution. Ann. Surg. 254, 465–473 (2011).
Miller, R. W. & Rabkin, C. S. Merkel cell carcinoma and melanoma: etiological similarities and differences. Cancer Epidemiol. Biomarkers Prev. 8, 153–158 (1999).
Howard, R. A., Dores, G. M., Curtis, R. E., Anderson, W. F. & Travis, L. B. Merkel cell carcinoma and multiple primary cancers. Cancer Epidemiol. Biomarkers Prev. 15, 1545–1549 (2006).
Starrett, G. J. et al. Merkel cell polyomavirus exhibits dominant control of the tumor genome and transcriptome in virus-associated merkel cell carcinoma. mBio 8, e02079-16 (2017).
Goh, G. et al. Mutational landscape of MCPyV-positive and MCPyV-negative Merkel cell carcinomas with implications for immunotherapy. Oncotarget 7, 3403–3415 (2016).
Heath, M. et al. Clinical characteristics of Merkel cell carcinoma at diagnosis in 195 patients: the AEIOU features. J. Am. Acad. Dermatol. 58, 375–381 (2008).
Ziprin, P., Smith, S., Salerno, G. & Rosin, R. D. Two cases of Merkel cell tumour arising in patients with chronic lymphocytic leukaemia. Br. J. Dermatol. 142, 525–528 (2000).
An, K. P. & Ratner, D. Merkel cell carcinoma in the setting of HIV infection. J. Am. Acad. Dermatol. 45, 309–312 (2001).
Engels, E. A., Frisch, M., Goedert, J. J., Biggar, R. J. & Miller, R. W. Merkel cell carcinoma and HIV infection. Lancet 359, 497–498 (2002).
Penn, I. & First, M. R. Merkel's cell carcinoma in organ recipients: report of 41 cases. Transplantation 68, 1717–1721 (1999).
Clarke, C. A. et al. Risk of Merkel cell carcinoma after solid organ transplantation. J. Natl Cancer Inst. 107, dju382 (2015).
Garrett, G. L. et al. Incidence of and risk factors for skin cancer in organ transplant recipients in the United States. JAMA Dermatol. 153, 296–303 (2017).
Paulson, K. G. et al. Systemic immune suppression predicts diminished Merkel cell carcinoma-specific survival independent of stage. J. Invest. Dermatol. 133, 642–646 (2013).
Sahi, H. et al. History of chronic inflammatory disorders increases the risk of Merkel cell carcinoma, but does not correlate with Merkel cell polyomavirus infection. Br. J. Cancer 116, 260–264 (2017).
Ho, S.-Y., Tsai, Y.-C., Lee, M.-C. & Guo, H.-R. Merkel cell carcinoma in patients with long-term ingestion of arsenic. J. Occup. Health 47, 188–192 (2005).
Popp, S., Waltering, S., Herbst, C., Moll, I. & Boukamp, P. UV-B-type mutations and chromosomal imbalances indicate common pathways for the development of Merkel and skin squamous cell carcinomas. Int. J. Cancer 99, 352–360 (2002).
Prasad, R. & Katiyar, S. K. Crosstalk among UV-induced inflammatory mediators, DNA damage and epigenetic regulators facilitates suppression of the immune system. Photochem. Photobiol. 93, 930–936 (2017).
Zur Hausen, A., Rennspiess, D., Winnepenninckx, V., Speel, E.-J. & Kurz, A. K. Early B-cell differentiation in Merkel cell carcinomas: clues to cellular ancestry. Cancer Res. 73, 4982–4987 (2013).
Tilling, T. et al. Immunohistochemical analyses point to epidermal origin of human Merkel cells. Histochem. Cell Biol. 141, 407–421 (2014).
Feng, H., Shuda, M., Chang, Y. & Moore, P. S. Clonal integration of a polyomavirus in human Merkel cell carcinoma. Science 319, 1096–1100 (2008). This study presents the discovery of MCPyV in MCC, highlighting the clonal integration of viral DNA, truncation of large T antigen and expression of the viral oncogene mRNA.
Gheit, T. et al. Isolation and characterization of a novel putative human polyomavirus. Virology 506, 45–54 (2017).
Tolstov, Y. L. et al. Asymptomatic primary Merkel cell polyomavirus infection among adults. Emerg. Infect. Dis. 17, 1371–1380 (2011).
Pastrana, D. V. et al. Quantitation of human seroresponsiveness to Merkel cell polyomavirus. PLoS Pathog. 5, e1000578 (2009).
Martel-Jantin, C. et al. Merkel cell polyomavirus infection occurs during early childhood and is transmitted between siblings. J. Clin. Virol. 58, 288–291 (2013).
Nicol, J. T. J. et al. Age-specific seroprevalences of merkel cell polyomavirus, human polyomaviruses 6, 7, and 9, and trichodysplasia spinulosa-associated polyomavirus. Clin. Vaccine Immunol. 20, 363–368 (2013).
Loyo, M. et al. Quantitative detection of Merkel cell virus in human tissues and possible mode of transmission. Int. J. Cancer 126, 2991–2996 (2010).
Ly, T. Y., Walsh, N. M. & Pasternak, S. The spectrum of Merkel cell polyomavirus expression in Merkel cell carcinoma, in a variety of cutaneous neoplasms, and in neuroendocrine carcinomas from different anatomical sites. Hum. Pathol. 43, 557–566 (2012).
Houben, R. et al. Merkel cell polyomavirus-infected Merkel cell carcinoma cells require expression of viral T antigens. J. Virol. 84, 7064–7072 (2010). This study provides the first evidence that the expression of T antigens is necessary for MCPyV+ MCC cell survival.
Li, J. et al. Merkel cell polyomavirus large T antigen disrupts host genomic integrity and inhibits cellular proliferation. J. Virol. 87, 9173–9188 (2013).
Theiss, J. M. et al. A comprehensive analysis of replicating Merkel cell polyomavirus genomes delineates the viral transcription program and suggests a role for mcv-miR-M1 in episomal persistence. PLoS Pathog. 11, e1004974 (2015).
Laude, H. C. et al. Distinct merkel cell polyomavirus molecular features in tumour and non tumour specimens from patients with Merkel cell carcinoma. PLoS Pathog. 6, e1001076 (2010).
Nakamura, T. et al. Nuclear localization of Merkel cell polyomavirus large T antigen in Merkel cell carcinoma. Virology 398, 273–279 (2010).
Shuda, M. et al. T antigen mutations are a human tumor-specific signature for Merkel cell polyomavirus. Proc. Natl Acad. Sci. USA 105, 16272–16277 (2008). This study demonstrates that full-length large T antigen is not permissive in MCPyV+ MCC cell lines.
Shuda, M., Kwun, H. J., Feng, H., Chang, Y. & Moore, P. S. Human Merkel cell polyomavirus small T antigen is an oncoprotein targeting the 4E-BP1 translation regulator. J. Clin. Invest. 121, 3623–3634 (2011).
Cheng, J., Rozenblatt-Rosen, O., Paulson, K. G., Nghiem, P. & DeCaprio, J. A. Merkel cell polyomavirus large T antigen has growth-promoting and inhibitory activities. J. Virol. 87, 6118–6126 (2013).
Shuda, M. et al. Merkel cell polyomavirus small T antigen induces cancer and embryonic Merkel cell proliferation in a transgenic mouse model. PLoS ONE 10, e0142329 (2015).
Verhaegen, M. E. et al. Merkel cell polyomavirus small T antigen is oncogenic in transgenic mice. J. Invest. Dermatol. 135, 1415–1424 (2015).
Verhaegen, M. E. et al. Merkel cell polyomavirus small T antigen initiates Merkel cell carcinoma-like tumor development in mice. Cancer Res. 77, 3151–3157 (2017). The first in vivo demonstration of an MCC-like tumour in a murine model.
Kwun, H. J. et al. Merkel cell polyomavirus small T antigen controls viral replication and oncoprotein expression by targeting the cellular ubiquitin ligase SCFFbw7. Cell Host Microbe 14, 125–135 (2013).
Angermeyer, S., Hesbacher, S., Becker, J. C., Schrama, D. & Houben, R. Merkel cell polyomavirus-positive Merkel cell carcinoma cells do not require expression of the viral small T antigen. J. Invest. Dermatol. 133, 2059–2064 (2013).
Berrios, C. et al. Merkel cell polyomavirus small T antigen promotes pro-glycolytic metabolic perturbations required for transformation. PLoS Pathog. 12, e1006020 (2016).
Wong, S. Q. et al. UV-associated mutations underlie the etiology of MCV-negative Merkel cell carcinomas. Cancer Res. 75, 5228–5234 (2015).
González-Vela, M. D. C. et al. Shared oncogenic pathways implicated in both virus-positive and UV-induced merkel cell carcinomas. J. Invest. Dermatol. 137, 197–206 (2017).
Cimino, P. J. et al. Retinoblastoma gene mutations detected by whole exome sequencing of Merkel cell carcinoma. Mod. Pathol. 27, 1073–1087 (2014).
Fischer, M., Grossmann, P., Padi, M. & DeCaprio, J. A. Integration of TP53, DREAM, MMB-FOXM1 and RB-E2F target gene analyses identifies cell cycle gene regulatory networks. Nucleic Acids Res. 44, 6070–6086 (2016).
Borchert, S. et al. High-affinity Rb binding, p53 inhibition, subcellular localization, and transformation by wild-type or tumor-derived shortened Merkel cell polyomavirus large T antigens. J. Virol. 88, 3144–3160 (2014).
Hesbacher, S. et al. RB1 is the crucial target of the Merkel cell polyomavirus large T antigen in Merkel cell carcinoma cells. Oncotarget 7, 32956–32968 (2016).
Rodig, S. J. et al. Improved detection suggests all Merkel cell carcinomas harbor Merkel polyomavirus. J. Clin. Invest. 122, 4645–4653 (2012).
Houben, R. et al. Mechanisms of p53 restriction in Merkel cell carcinoma cells are independent of the Merkel cell polyoma virus T antigens. J. Invest. Dermatol. 133, 2453–2460 (2013).
Cohen, P. R. et al. Genomic portfolio of Merkel cell carcinoma as determined by comprehensive genomic profiling: implications for targeted therapeutics. Oncotarget 7, 23454–23467 (2016).
Hafner, C. et al. Activation of the PI3K/AKT pathway in Merkel cell carcinoma. PLoS ONE 7, e31255 (2012).
Paulson, K. G. et al. Transcriptome-wide studies of Merkel cell carcinoma and validation of intratumoral CD8+ lymphocyte invasion as an independent predictor of survival. J. Clin. Oncol. 29, 1539–1546 (2011).
Walsh, N. M. et al. A morphological and immunophenotypic map of the immune response in Merkel cell carcinoma. Hum. Pathol. 52, 190–196 (2016).
Dowlatshahi, M. et al. Tumor-specific T cells in human Merkel cell carcinomas: a possible role for Tregs and T-cell exhaustion in reducing T-cell responses. J. Invest. Dermatol. 133, 1879–1889 (2013).
Yi, J. S., Cox, M. A. & Zajac, A. J. T-Cell exhaustion: characteristics, causes and conversion. Immunology 129, 474–481 (2010).
Ritter, C. et al. Epigenetic priming restores the HLA class-I antigen processing machinery expression in Merkel cell carcinoma. Sci. Rep. 7, 2290 (2017).
Gibney, G. T., Weiner, L. M. & Atkins, M. B. Predictive biomarkers for checkpoint inhibitor-based immunotherapy. Lancet. Oncol. 17, e542–e551 (2016).
Becker, J. C. et al. Merkel cell carcinoma: molecular pathogenesis, clinical features and therapy. J. Dtsch. Dermatol. Ges. 6, 709–719 (2008).
Llombart, B. et al. Clinicopathological and immunohistochemical analysis of 20 cases of Merkel cell carcinoma in search of prognostic markers. Histopathology 46, 622–634 (2005).
Schadendorf, D. et al. Merkel cell carcinoma: epidemiology, prognosis, therapy and unmet medical needs. Eur. J. Cancer 71, 53–69 (2017).
Sparks, J., Sparks, M. & Malone, J. C. Cutaneous Merkel cell carcinoma: multiple asynchronous primary lesions in a patient on immunosuppressive therapy. J. Cutan. Pathol. 44, 309–312 (2017).
Gupta, S. G. et al. Sentinel lymph node biopsy for evaluation and treatment of patients with Merkel cell carcinoma: the Dana-Farber experience and meta-analysis of the literature. Arch. Dermatol. 142, 685–690 (2006).
Foote, M., Veness, M., Zarate, D. & Poulsen, M. Merkel cell carcinoma: the prognostic implications of an occult primary in stage IIIB (nodal) disease. J. Am. Acad. Dermatol. 67, 395–399 (2012).
Walsh, N. M. Complete spontaneous regression of Merkel cell carcinoma: a 30 year perspective. J. Cutan. Pathol. 43, 1150–1154 (2016).
Chen, K. T. et al. A better prognosis for Merkel cell carcinoma of unknown primary origin. Am. J. Surg. 206, 752–757 (2013).
Bichakjian, C. K. et al. NCCN clinical practice guidelines in oncology (NCCN guidelines) Merkel cell carcinoma version 1. National Comprehensive Cancer Networkhttps://www.nccn.org/professionals/physician_gls/pdf/mcc.pdf (2017).
Lebbe, C. et al. Diagnosis and treatment of Merkel Cell Carcinoma. European consensus-based interdisciplinary guideline. Eur. J. Cancer 51, 2396–2403 (2015).
Becker, J. C. et al. Brief S2k guidelines — Merkel cell carcinoma. J. Dtsch. Dermatol. Ges. 11 (Suppl. 3), 29–36 (2013).
Llombart, B., Kindem, S. & Chust, M. Merkel cell carcinoma: an update of key imaging techniques, prognostic factors, treatment, and follow-up. Actas Dermosifiliogr. 108, 98–107 (2017).
Buder, K. et al. Somatostatin receptor expression in Merkel cell carcinoma as target for molecular imaging. BMC Cancer 14, 268 (2014).
Concannon, R., Larcos, G. S. & Veness, M. The impact of 18F-FDG PET-CT scanning for staging and management of Merkel cell carcinoma: results from Westmead Hospital, Sydney, Australia. J. Am. Acad. Dermatol. 62, 76–84 (2010).
Fried, I. & Cerroni, L. Merkel cell carcinoma [German]. Pathologe 35, 467–475 (2014).
Calder, K. B. & Smoller, B. R. New insights into merkel cell carcinoma. Adv. Anat. Pathol. 17, 155–161 (2010).
Brown, H. A., Sawyer, D. M. & Woo, T. Intraepidermal Merkel cell carcinoma with no dermal involvement. Am. J. Dermatopathol. 22, 65–69 (2000).
Narisawa, Y., Koba, S., Inoue, T. & Nagase, K. Histogenesis of pure and combined Merkel cell carcinomas: an immunohistochemical study of 14 cases. J. Dermatol. 42, 445–452 (2015).
Iacocca, M. V., Abernethy, J. L., Stefanato, C. M., Allan, A. E. & Bhawan, J. Mixed Merkel cell carcinoma and squamous cell carcinoma of the skin. J. Am. Acad. Dermatol. 39, 882–887 (1998).
Lai, J. H. et al. Pure versus combined Merkel cell carcinomas: immunohistochemical evaluation of cellular proteins (p53, Bcl-2, and c-kit) reveals significant overexpression of p53 in combined tumors. Hum. Pathol. 46, 1290–1296 (2015).
Ames, H. M. et al. Huntingtin-interacting protein 1: a Merkel cell carcinoma marker that interacts with c-Kit. J. Invest. Dermatol. 131, 2113–2120 (2011).
Fleming, K. E. et al. Support for p63 expression as an adverse prognostic marker in Merkel cell carcinoma: report on a Canadian cohort. Hum. Pathol. 45, 952–960 (2014).
Stetsenko, G. Y. et al. p63 expression in Merkel cell carcinoma predicts poorer survival yet may have limited clinical utility. Am. J. Clin. Pathol. 140, 838–844 (2013).
Paulson, K. G. et al. CD8+ lymphocyte intratumoral infiltration as a stage-independent predictor of Merkel cell carcinoma survival: a population-based study. Am. J. Clin. Pathol. 142, 452–458 (2014).
Feldmeyer, L. et al. Density, distribution, and composition of immune infiltrates correlate with survival in Merkel cell carcinoma. Clin. Cancer Res. 22, 5553–5563 (2016).
Miller, N. J. et al. Tumor-infiltrating Merkel Cell polyomavirus-specific T cells are diverse and associated with improved patient survival. Cancer Immunol. Res. 5, 137–147 (2017).
Harms, K. L. et al. Increased expression of EZH2 in Merkel cell carcinoma is associated with disease progression and poorer prognosis. Hum. Pathol. 67, 78–84 (2017).
U.S. Preventive Services Task Force. Skin cancer: screening. Summary of recommendations and evidence. U.S. Preventive Services Task Forcehttp://www.uspreventiveservicestaskforce.org/uspstf09/skincancer/skincanrs.htm (2009).
U.S. Department of Health and Human Services. The Surgeon General's call to action to prevent skin cancer (U.S. Dept of Health and Human Services, 2014).
Locke, F. L., Rollison, D. E. & Sondak, V. K. Merkel cell carcinoma and immunosuppression: what we still need to know. J. Natl Cancer Inst. 107, dju422 (2015).
Zelenetz, A. D. et al. NCCN clinical practice guidelines in oncology (NCCN Guidelines) B-cell lymphomas version 4. National Comprehensive Cancer Networkhttps://www.nccn.org/professionals/physician_gls/pdf/b-cell.pdf (2017).
Kaufman, H. L. et al. Avelumab in patients with chemotherapy-refractory metastatic Merkel cell carcinoma: a multicentre, single-group, open-label, phase 2 trial. Lancet Oncol. 17, 1374–1385 (2016). This study shows the high response rate of MCPyV+ MCC and MCPyV− MCC to PDL1 inhibition as a second-line therapy.
Allen, P. J. et al. Merkel cell carcinoma: prognosis and treatment of patients from a single institution. J. Clin. Oncol. 23, 2300–2309 (2005).
Bichakjian, C. K. et al. Merkel cell carcinoma: critical review with guidelines for multidisciplinary management. Cancer 110, 1–12 (2007).
Hawryluk, E. B. et al. Positron emission tomography/computed tomography imaging in Merkel cell carcinoma: a study of 270 scans in 97 patients at the Dana-Farber/Brigham and Women's Cancer Center. J. Am. Acad. Dermatol. 68, 592–599 (2013).
Paulson, K. G. et al. Antibodies to merkel cell polyomavirus T antigen oncoproteins reflect tumor burden in merkel cell carcinoma patients. Cancer Res. 70, 8388–8397 (2010).
Paulson, K. G. et al. Viral oncoprotein antibodies as a marker for recurrence of Merkel cell carcinoma: a prospective validation study. Cancer 123, 1464–1474 (2017).
Mancebo, S. E., Hu, J. Y. & Wang, S. Q. Sunscreens: a review of health benefits, regulations, and controversies. Dermatol. Clin. 32, 427–438 (2014).
Samimi, M. et al. Vitamin D deficiency is associated with greater tumor size and poorer outcome in Merkel cell carcinoma patients. J. Eur. Acad. Dermatol. Venereol. 28, 298–308 (2014).
Dziunycz, P. J. et al. The oncogene ATF3 is potentiated by cyclosporine A and ultraviolet light A. J. Invest. Dermatol. 134, 1998–2004 (2014).
Becker, J. C., Houben, R., Vetter, C. S. & Bröcker, E. B. The carcinogenic potential of tacrolimus ointment beyond immune suppression: a hypothesis creating case report. BMC Cancer 6, 7 (2006).
Santana, A. L., Felsen, D. & Carucci, J. A. Interleukin-22 and cyclosporine in aggressive cutaneous squamous cell carcinoma. Dermatol. Clin. 35, 73–84 (2017).
Ellis, D. L. & Davis, R. S. Evidence-based management of primary and localized Merkel cell carcinoma: a review. Int. J. Dermatol. 52, 1248–1258 (2013).
Tai, P. A practical update of surgical management of merkel cell carcinoma of the skin. ISRN Surg. 2013, 850797 (2013).
Kline, L. & Coldiron, B. Mohs micrographic surgery for the treatment of Merkel cell carcinoma. Dermatol. Surg. 42, 945–951 (2016).
O’Connor, W. J., Roenigk, R. K. & Brodland, D. G. Merkel cell carcinoma. Comparison of Mohs micrographic surgery and wide excision in eighty-six patients. Dermatol. Surg. 23, 929–933 (1997).
Gunaratne, D. A., Howle, J. R. & Veness, M. J. Sentinel lymph node biopsy in Merkel cell carcinoma: a 15-year institutional experience and statistical analysis of 721 reported cases. Br. J. Dermatol. 174, 273–281 (2016).
Stokes, J. B. et al. Patients with Merkel cell carcinoma tumors < or = 1.0 cm in diameter are unlikely to harbor regional lymph node metastasis. J. Clin. Oncol. 27, 3772–3777 (2009).
Servy, A. et al. Merkel cell carcinoma: value of sentinel lymph-node status and adjuvant radiation therapy. Ann. Oncol. 27, 914–919 (2016).
Prieto, I. et al. Merkel cell carcinoma: an algorithm for multidisciplinary management and decision-making. Crit. Rev. Oncol. Hematol. 98, 170–179 (2016).
Fang, L. C., Lemos, B., Douglas, J., Iyer, J. & Nghiem, P. Radiation monotherapy as regional treatment for lymph node-positive Merkel cell carcinoma. Cancer 116, 1783–1790 (2010).
Hasan, S., Liu, L., Triplet, J., Li, Z. & Mansur, D. The role of postoperative radiation and chemoradiation in Merkel cell carcinoma: a systematic review of the literature. Front. Oncol. 3, 276 (2013).
Bhatia, S. et al. Adjuvant radiation therapy and chemotherapy in Merkel cell carcinoma: survival analyses of 6908 cases from the National Cancer Data Base. J. Natl Cancer Inst. 108, djw042 (2016). A register study that demonstrates the value of adjuvant radiotherapy.
Veness, M. & Howle, J. Radiotherapy alone in patients with Merkel cell carcinoma: the Westmead Hospital experience of 41 patients. Australas. J. Dermatol. 56, 19–24 (2015).
Iyer, J. G. et al. Single-fraction radiation therapy in patients with metastatic Merkel cell carcinoma. Cancer Med. 4, 1161–1170 (2015).
Jouary, T. et al. Adjuvant prophylactic regional radiotherapy versus observation in stage I Merkel cell carcinoma: a multicentric prospective randomized study. Ann. Oncol. 23, 1074–1080 (2012).
Porceddu, S. V., Veness, M. J. & Guminski, A. Nonmelanoma cutaneous head and neck cancer and Merkel cell carcinoma: current concepts, advances, and controversies. J. Clin. Oncol. 33, 3338–3345 (2015).
Nghiem, P. et al. Systematic literature review of efficacy, safety and tolerability outcomes of chemotherapy regimens in patients with metastatic Merkel cell carcinoma. Future Oncol. 13, 1263–1279 (2017). A meta-analysis that demonstrates the limited clinical value of chemotherapy in advanced-stage MCC.
Iyer, J. G. et al. Response rates and durability of chemotherapy among 62 patients with metastatic Merkel cell carcinoma. Cancer Med. 5, 2294–2301 (2016).
Becker, J. C. et al. Evaluation of real-world treatment outcomes in patients with distant metastatic Merkel cell carcinoma following second-line chemotherapy in Europe. Oncotargethttp://dx.doi.org/10.18632/oncotarget.19218 (2017).
Topalian, S. L., Drake, C. G. & Pardoll, D. M. Immune checkpoint blockade: a common denominator approach to cancer therapy. Cancer Cell 27, 451–461 (2015).
Lyngaa, R. et al. T-Cell responses to oncogenic Merkel cell polyomavirus proteins distinguish patients with merkel cell carcinoma from healthy donors. Clin. Cancer Res. 20, 1768–1778 (2014). A study that shows the detection of T antigen-specific T cell responses in the majority of patients with MCC.
Afanasiev, O. K. et al. Merkel polyomavirus-specific T cells fluctuate with Merkel cell carcinoma burden and express therapeutically targetable PD-1 and Tim-3 exhaustion markers. Clin. Cancer Res. 19, 5351–5360 (2013).
Nghiem, P. T. et al. PD-1 blockade with pembrolizumab in advanced Merkel-cell carcinoma. N. Engl. J. Med. 374, 2542–2552 (2016). A study that shows the high response rate of MCPyV+ MCC and MCPyV− MCC to PD1 inhibition as a first-line therapy.
Topalian, S. et al. Non-comparative, open-label, multiple cohort, phase 1/2 study to evaluate nivolumab (NIVO) in patients with virus-associated tumors (CheckMate 358): efficacy and safety in Merkel cell carcinoma [abstract]. Cancer Res. 77 (13 Suppl.), CT074 (2017).
D’Angelo, S. P. et al. First-line (1L) avelumab treatment in patients (pts) with metastatic Merkel cell carcinoma (mMCC): preliminary data from an ongoing study [abstract]. J. Clin. Oncol. 35 (Suppl. 15), 9530 (2017).
Terheyden, P. & Becker, J. C. New developments in the biology and the treatment of metastatic Merkel cell carcinoma. Curr. Opin. Oncol. 29, 221–226 (2017).
Ferrat, E. et al. Performance of four frailty classifications in older patients with cancer: prospective elderly cancer patients cohort study. J. Clin. Oncol. 35, 766–777 (2017).
Gorayski, P., Tripcony, L. & Poulsen, M. Chemotherapy compliance in high-risk Merkel cell carcinoma treated with chemoradiotherapy. Australas. J. Dermatol. 58, 35–41 (2017).
Kanz, B. A. et al. Safety and efficacy of anti-PD-1 in patients with baseline cardiac, renal, or hepatic dysfunction. J. Immunother. Cancer 4, 60 (2016).
Sauer, C. M. et al. Reviewing the current evidence supporting early B-cells as the cellular origin of Merkel cell carcinoma. Crit. Rev. Oncol. Hematol. 116, 99–105 (2017).
Liu, W. et al. Identifying the target cells and mechanisms of Merkel cell polyomavirus infection. Cell Host Microbe 19, 775–787 (2016).
Tolstov, Y. L. et al. Human Merkel cell polyomavirus infection II. MCV is a common human infection that can be detected by conformational capsid epitope immunoassays. Int. J. Cancer 125, 1250–1256 (2009).
Cassler, N. M., Merrill, D., Bichakjian, C. K. & Brownell, I. Merkel cell carcinoma therapeutic update. Curr. Treat. Opt. Oncol. 17, 36 (2016).
APCure. LTvax, the first therapeutic product targeting Merkel cell polyomavirus-associated cancers. APCurehttp://www.apcure.com/en/pipeline/ltvax (2017)
Paulson, K. G. et al. Downregulation of MHC-I expression is prevalent but reversible in Merkel cell carcinoma. Cancer Immunol. Res. 2, 1071–1079 (2014).
Willmes, C. et al. Type I and II IFNs inhibit Merkel cell carcinoma via modulation of the Merkel cell polyomavirus T antigens. Cancer Res. 72, 2120–2128 (2012).
Ritter, C. et al. Reversal of epigenetic silencing of MHC class I chain-related protein A and B improves immune recognition of Merkel cell carcinoma. Sci. Rep. 6, 21678 (2016).
Gross, L. A filterable agent, L. recovered from Ak leukemic extracts, causing salivary gland carcinomas in C3H mice. Proc. Soc. Exp. Biol. Med. 83, 414–421 (1953).
Calvignac-Spencer, S. et al. A taxonomy update for the family Polyomaviridae. Arch. Virol. 161, 1739–1750 (2016).
IARC Working Group on the Evaluation of Carcinogenic Risks to Humans. Malaria and some polyomaviruses (SV40, BK, JC, and Merkel cell viruses). IARC monographs on the evaluation of carcinogenic risks to humans, no. 104 (International Agency for Research on Cancer, 2014).
Schowalter, R. M., Pastrana, D. V., Pumphrey, K. A., Moyer, A. L. & Buck, C. B. Merkel cell polyomavirus and two previously unknown polyomaviruses are chronically shed from human skin. Cell Host Microbe 7, 509–515 (2010).
Schrama, D., Buck, C. B., Houben, R. & Becker, J. C. No evidence for association of HPyV6 or HPyV7 with different skin cancers. J. Invest. Dermatol. 132, 239–241 (2012).
Nguyen, K. D. et al. Human polyomavirus 6 and 7 are associated with pruritic and dyskeratotic dermatoses. J. Am. Acad. Dermatol. 76, 932–940.e3 (2017).
van der Meijden, E. et al. Discovery of a new human polyomavirus associated with trichodysplasia spinulosa in an immunocompromized patient. PLoS Pathog. 6, e1001024 (2010).
van der Meijden, E. et al. Primary polyomavirus infection, not reactivation, as the cause of trichodysplasia spinulosa in immunocompromised patients. J. Infect. Dis. 215 jiw403 (2016).
Gardner, S. D., Field, A. M., Coleman, D. V. & Hulme, B. New human papovavirus (B.K.) isolated from urine after renal transplantation. Lancet 297, 1253–1257 (1971).
Padgett, B. L., Zurhein, G. M., Walker, D. L., Eckroade, R. J. & Dessel, B. H. Cultivation of papova-like virus from human brain with progressive multifocal leucoencephalopathy. Lancet 297, 1257–1260 (1971).
Bowen, L. N., Smith, B., Reich, D., Quezado, M. & Nath, A. HIV-associated opportunistic CNS infections: pathophysiology, diagnosis and treatment. Nat. Rev. Neurol. 12, 662–674 (2016).
Koralnik, I. J. et al. JC virus granule cell neuronopathy: a novel clinical syndrome distinct from progressive multifocal leukoencephalopathy. Ann. Neurol. 57, 576–580 (2005).
Allander, T. et al. Identification of a third human polyomavirus. J. Virol. 81, 4130–4136 (2007).
Gaynor, A. M. et al. Identification of a novel polyomavirus from patients with acute respiratory tract infections. PLoS Pathog. 3, e64 (2007).
Siebrasse, E. A. et al. WU polyomavirus in respiratory epithelial cells from lung transplant patient with Job syndrome. Emerg. Infect. Dis. 21, 103–106 (2015).
Buck, C. B. et al. Complete genome sequence of a tenth human polyomavirus. J. Virol. 86, 10887 (2012).
Lim, E. S. et al. Discovery of STL polyomavirus, a polyomavirus of ancestral recombinant origin that encodes a unique T antigen by alternative splicing. Virology 436, 295–303 (2013).
Mishra, N. et al. Identification of a novel polyomavirus in a pancreatic transplant recipient with retinal blindness and vasculitic myopathy. J. Infect. Dis. 210, 1595–1599 (2014).
Daily, K. et al. Assessment of cancer cell line representativeness using microarrays for Merkel cell carcinoma. J. Invest. Dermatol. 135, 1138–1146 (2015).
Houben, R. et al. Activation of the MAP kinase pathway induces apoptosis in the Merkel cell carcinoma cell line UISO. J. Invest. Dermatol. 127, 2116–2122 (2007).
Spurgeon, M. E., Cheng, J., Bronson, R. T., Lambert, P. F. & DeCaprio, J. A. Tumorigenic activity of merkel cell polyomavirus T antigens expressed in the stratified epithelium of mice. Cancer Res. 75, 1068–1079 (2015).
Lee, S. et al. Identification and validation of a novel mature microRNA encoded by the Merkel cell polyomavirus in human Merkel cell carcinomas. J. Clin. Virol. 52, 272–275 (2011).
Carter, J. J. et al. Identification of an overprinting gene in Merkel cell polyomavirus provides evolutionary insight into the birth of viral genes. Proc. Natl Acad. Sci. USA 110, 12744–12749 (2013).
Feng, H. et al. Cellular and viral factors regulating Merkel cell polyomavirus replication. PLoS ONE 6, e22468 (2011).
Harrison, C. J. et al. Asymmetric assembly of Merkel cell polyomavirus large T-antigen origin binding domains at the viral origin. J. Mol. Biol. 409, 529–542 (2011).
Yardimci, H. et al. Bypass of a protein barrier by a replicative DNA helicase. Nature 492, 205–209 (2012).
Shuda, M. et al. CDK1 substitutes for mTOR kinase to activate mitotic cap-dependent protein translation. Proc. Natl Acad. Sci. USA 112, 5875–5882 (2015).
Bichakjian, C. K., Nghiem, P., Johnson, T., Wright, C. L. & Sober, A. J. in AJCC Cancer Staging Manual 8 th Edition Ch. 46 (eds Amin, M. B. et al.) (American Joint Committee on Cancer, 2016).
Acknowledgements
J.C.B. is funded by the European Commission Grant Agreement #277775/IMMOMEC, the BMBF 03VP01062/CTCelect and the Hiege Stiftung. A.S. receives a grant from the German Federal Ministry of Education and Science (BMBF), grant number 01ER1305. J.A.D. was supported in part by US Public Health Service grants R01CA63113, R01CA173023, P01CA050661 and P01CA203655, the DFCI Helen Pappas Merkel Cell Research Fund and the Claudia Adams Barr Program in Cancer Research. P.N. was supported in part by US Public Health Service grants K24-CA139052 and RO1-CA176841 and the University of Washington MCC Gift Fund.
Author information
Authors and Affiliations
Contributions
Introduction (J.C.B.); Epidemiology (A.S.); Mechanisms/pathophysiology (J.A.D. and J.C.B.); Diagnosis, screening and prevention (L.C.); Management (C.L., P.N., M.V. and J.C.B.); Quality of life (M.V.); Outlook (J.C.B.); Overview of Primer (J.C.B.).
Corresponding author
Ethics declarations
Competing interests
J.C.B. has received speaker honoraria from Amgen, Merck Serono and Pfizer; he has received advisory board honoraria from Amgen, CureVac, eTheRNA, Lytix, Merck Serono, Novartis, Rigontec, and Takeda; and he has received research funding from Boehringer Ingelheim, Bristol-Myers Squibb (BMS) and Merck Serono. J.C.B.'s activities with BMS, Merck Serono and Pfizer are related to the submitted report (therapy for advanced-stage MCC). A research project in J.A.D.'s laboratory is supported by Constellation Pharmaceuticals. C.L. has received honoraria from Amgen, BMS, MSD, Novartis and Roche, and research funding from BMS and Roche; she has a consulting or advisory role for Amgen, BMS, MSD, Novartis and Roche; she is part of speakers’ bureaus for Amgen, BMS, Novartis and Roche; and she has received compensation for travel, accommodation and expenses from Amgen, BMS, Novartis and Roche. P.N. has served as a consultant for EMD Serono, Merck and Pfizer and has received research support to his institution from BMS. A.S., L.C. and M.V. declare no competing interests.
Rights and permissions
About this article
Cite this article
Becker, J., Stang, A., DeCaprio, J. et al. Merkel cell carcinoma. Nat Rev Dis Primers 3, 17077 (2017). https://doi.org/10.1038/nrdp.2017.77
Published:
DOI: https://doi.org/10.1038/nrdp.2017.77
This article is cited by
-
Diagnosis and treatment of malignant eyelid tumors
Die Ophthalmologie (2024)
-
Selinexor targets expression of metabolic genes in Merkel cell carcinoma cells
Archives of Dermatological Research (2024)
-
Adamantinoma-like ewing sarcoma arising in the pancreatic tail: a case report of a rare entity and review of the literature
Diagnostic Pathology (2023)
-
HLA-G expression in Merkel cell carcinoma and the correlation with Merkel cell polyomavirus infection
Immunogenetics (2023)
-
Merkel Cell Carcinoma with Gastric Metastasis, a Rare Presentation: Case Report and Literature Review
Journal of Gastrointestinal Cancer (2023)