Abstract
Guideline recommendations on the use of dual antiplatelet therapy (DAPT) in patients with acute coronary syndromes and in those undergoing percutaneous coronary intervention (PCI) have been formulated by both the ACC/AHA and the ESC. These recommendations are based primarily on large, phase III, randomized, controlled trials of the P2Y12 inhibitors clopidogrel, prasugrel, and ticagrelor. However, few East Asian patients have been included in the trials to assess the use of these agents, particularly the newer agents prasugrel and ticagrelor. Additionally, an increasing body of data suggests that East Asian patients have differing risk profiles for both thrombophilia and bleeding compared with white patients, and that a different 'therapeutic window' of on-treatment platelet reactivity might be appropriate in East Asian patients. Furthermore, a phenomenon referred to as the 'East Asian paradox' has been described, in which East Asian patients have a similar or even a lower rate of ischaemic events after PCI compared with white patients, despite a higher level of platelet reactivity during DAPT. Recognizing these concerns, the World Heart Federation has undertaken this evidence-based review and produced this expert consensus statement to determine the antiplatelet treatment strategies that are most appropriate for East Asian patients.
Similar content being viewed by others
Introduction
At the 65th World Health Assembly in May 2012, all 194 WHO member states endorsed a target to reduce premature deaths caused by noncommunicable diseases by 25% by 2025.1 Cardiovascular diseases are the leading cause of death and disability among the noncommunicable diseases.2 Therefore, effective treatment of patients with atherosclerotic coronary artery disease—both those with acute coronary syndrome (ACS) and those undergoing percutaneous coronary intervention (PCI)—is an important strategy to reduce the rate of premature death from cardiovascular disease as well as global mortality associated with noncommunicable diseases.
Compelling evidence supports the use of dual antiplatelet therapy (DAPT) in patients with ACS and also those with stable ischaemic heart disease undergoing PCI. In these clinical settings, the use of a P2Y12 inhibitor combined with aspirin is recommended in the ACC/AHA and ESC guidelines.3,4,5,6,7 These recommendations are based primarily on large, phase III, randomized, controlled trials of these agents. In addition, patients who are poor responders or who have a high on-treatment platelet reactivity to ADP during DAPT are at increased risk of ischaemic events after PCI.8 Multiple lines of evidence have suggested that low on-treatment platelet reactivity to ADP is associated with an increased risk of bleeding.8 Therefore, a 'therapeutic window' concept of platelet reactivity has been proposed for P2Y12-inhibitor therapy. However, the relationship between platelet reactivity and ischaemic or bleeding events might differ according to intrinsic thrombogenicity or disease activity.9
As with most cardiovascular drugs, P2Y12 inhibitors have shown marked interethnic differences in pharmacokinetic and pharmacodynamic profiles.9 Although East Asian ethnic groups are among the most populous (more than 1.5 billion people), very few East Asian patients have been included in the trials to assess the use of P2Y12 inhibitors, particularly the newer agents prasugrel and ticagrelor. Recognizing concerns about an increased incidence of haemorrhagic stroke and potential bleeding that might occur among East Asian patients receiving antithrombotic therapy,10,11 even in the absence of hypertension,12 the World Heart Federation has undertaken an evidence-based review and produced this expert consensus statement to determine the antiplatelet treatment strategies that are most appropriate for East Asian patients. This consensus statement (members of the expert panel are listed in Box 1) provides observations and recommendations addressing the regional clinical practice trends in East Asia and highlights the need for future research. The concepts discussed should contribute to the global strategy to reduce the rate of premature death from noncommunicable diseases by 25% by 2025.1
Current P2Y12 inhibitors
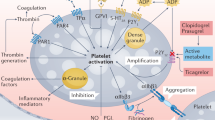
Clopidogrel replaced ticlopidine 2 decades ago as a part of DAPT for the prevention of stent thrombosis, and has subsequently been used in the majority of patients undergoing coronary stent implantation. Clopidogrel is established as a beneficial therapy in patients with ACS,13 and is recommended as part of the treatment of these patients.7 Clopidogrel is a thienopyridine prodrug, and its conversion to its active metabolite R-130964 requires a two-step process in the liver (Figure 1).8 Through biotransformation, R-130964 irreversibly inhibits platelet aggregation. Although numerous epigenetic factors influence generation of the active metabolite and platelet-reactivity phenotype,14,15,16 variation in the cytochrome P450 (CYP) allele, especially CYP2C19, has been shown to have the greatest influence.8 The clinical importance of these factors has been the subject of much research and debate.
The antiplatelet effect of P2Y12-receptor inhibitors might be modified by genetic variation in proteins involved in the absorption, metabolism, and target receptor. Bioavailability of the prodrug clopidogrel is determined by intestinal absorption, which might be limited by the efflux pump MDR1 (encoded by ABCB1). Subsequently, the majority of the prodrug is inactivated by ubiquitous esterases, but the remainder is activated in a two-step process by CYP isoenzymes in the liver. Genetic variation in the activity of CYP2C19 is particularly important in determining clopidogrel response. The bioactive metabolite irreversibly binds to P2Y12 receptors on platelets, and subsequently prevents ADP-induced stimulation of GPIIb/IIIa (encoded by ITGB3 and ITGA2B) and platelet activation. The prodrug prasugrel is hydrolysed to a thiolactone derivative in the intestine and is then oxidized to its active metabolite by CYP isoenzymes in the liver, but seems to be little affected by genetic variation in these enzymes. Ticagrelor is a direct-acting, reversible, P2Y12-receptor inhibitor, and seems to be little affected by genetic variation in the CYP isoenzymes. Abbreviations: CYP, cytochrome P450; GP, glycoprotein; hCE, human carboxylesterase; MDR1, multidrug resistance protein 1. Permission obtained from NPG © Ahmad, T. et al. Nat. Rev. Cardiol. 8, 560–571 (2011).
Prasugrel, is another thienopyridine that irreversibly inhibits platelet aggregation. Prasugrel requires a single, CYP-dependent oxidation step to its active metabolite (Figure 1). Compared with clopidogrel, administration of prasugrel results in faster and greater platelet inhibition, owing to rapid and efficient generation of the active metabolite, with less patient-to-patient variation.8,17,18
Ticagrelor is a nonthienopyridine, direct-acting, oral antagonist that binds reversibly to the P2Y12 receptor (Figure 1). The major metabolite of ticagrelor (AR-C124910XX), formed by metabolism via CYP3A4, is as potent as the parent compound ticagrelor. Compared with clopidogrel, ticagrelor results in faster and greater platelet inhibition, with less patient-to-patient variation (similar to prasugrel).8,19
Clinical evidence for DAPT
Clopidogrel
Several major studies of platelet P2Y12-receptor inhibitors involving patients with ACS and those undergoing PCI form the evidence base for the US and European guideline recommendations.3,4,5,6,7 In the CURE trial,20 12,562 patients with non-ST-segment elevation ACS were treated with clopidogrel (300 mg loading dose, 75 mg daily maintenance dose) plus aspirin (81–325 mg daily) or aspirin alone. At 12 months, clopidogrel plus aspirin was associated with a 20% relative reduction compared with aspirin alone (9.3% vs 11.4%; P = 0.00009) in the primary composite end point of cardiovascular death, nonfatal myocardial infarction (MI), and nonfatal stroke.20 In PCI-CURE,21 a prospective subgroup analysis of 2,658 patients from the CURE study who underwent PCI with a bare-metal stent, a 31% relative reduction in the composite end point was reported with clopidogrel plus aspirin compared with aspirin alone (8.8% vs 12.6%; P = 0.002). In the CREDO trial,22 which involved 2,116 patients undergoing elective PCI, the benefits of a preprocedural loading dose of clopidogrel, and of continuing clopidogrel for 12 months after PCI with a bare-metal stent, both in addition to aspirin therapy, were investigated. Treatment with clopidogrel in addition to aspirin for 12 months after PCI was associated with a 26.9% relative reduction in the composite end point of death, MI, and stroke compared with aspirin alone (8.5% vs 11.5%; P = 0.02).22 A subgroup analysis of the timing of the preprocedural loading dose suggested that clopidogrel 300 mg should be given ≥6 h, and ideally ≥15 h, before PCI.23 In the COMMIT trial24 of Chinese patients with suspected acute MI, short-term (in-hospital for up to 4 weeks) treatment with clopidogrel resulted in a 9% reduction in the composite ischaemic end point (P = 0.002), and a 7% reduction in all-cause mortality (P = 0.03). The results of these studies provided the basis for establishing the evidence-based guidelines for the early use of a P2Y12-receptor antagonist in patients with ACS or those undergoing PCI with a bare-metal stent.
Prasugrel
Subsequent to these early studies with clopidogrel, two newer P2Y12-receptor inhibitors have been studied in large trials to compare their efficacy with that of clopidogrel. In TRITON-TIMI 38,25 prasugrel was compared with clopidogrel in 13,608 patients with moderate-to-high-risk ACS who were referred for PCI. Prasugrel was associated with a 19% relative reduction in the primary combined end point of cardiovascular death, nonfatal MI, and nonfatal stroke compared with clopidogrel (9.9% vs 12.1%; P <0.001).25 The benefits were largely associated with a reduction in nonfatal MI, with no significant difference in cardiovascular death or nonfatal stroke. The rate of stent thrombosis was significantly reduced with prasugrel compared with clopidogrel (1.1% vs 2.4%; P <0.001).25 However, prasugrel was associated with a significant increase in the rate of TIMI (Thrombolysis In Myocardial Infarction) major haemorrhage and fatal bleeding.25 A post-hoc analysis suggested that patients with a history of stroke or transient ischaemic attack (TIA), those aged ≥75 years, or with a body mass <60 kg had an increased rate of bleeding. Patients with a history of stroke or TIA experienced net harm, whereas those aged ≥75 years or with a mass <60 kg derived no net benefit.25 Importantly, an unacceptable 2.5% rate of intracranial haemorrhage occurred in those with a history of stroke or TIA treated with prasugrel and, for this reason, prasugrel is contraindicated in these patients. By contrast, a subsequent subgroup analysis suggested that patients with a history of ST-segment elevation MI or diabetes mellitus derived greater relative benefit from prasugrel than clopidogrel therapy.26
The second major phase III study in which prasugrel was compared with clopidogrel was the TRILOGY ACS trial.27 This trial included a population of 9,326 patients with ACS who were being medically managed. The daily dose of prasugrel was reduced to 5 mg (instead of 10 mg) for patients aged ≥75 years and those with a body mass <60 kg. No significant difference in the primary combined end point of cardiovascular death, MI, and stroke was reported between treatment with prasugrel or clopidogrel.27 None of the safety end points was significantly different between the two study groups.
Ticagrelor
In the Platelet Inhibition and Patient Outcomes (PLATO) trial,28 18,624 patients hospitalized with ACS were randomly allocated to treatment with ticagrelor or clopidogrel, with all patients also receiving aspirin. Overall, 60.6% of patients underwent stent implantation. At 12 months, ticagrelor was associated with a 16% relative reduction (9.8% vs 11.7%; P = 0.0003) in the combined primary efficacy end point of cardiovascular death, MI, and stroke.28 Importantly, reductions in all-cause mortality (4.5% vs 5.9%; P <0.001) and definite stent thrombosis (1.3% vs 1.9%; P = 0.009) were observed with ticagrelor therapy.28 In the PLATO substudy29 of 5,216 patients with ACS who were prespecified by the enrolling physician before randomization to be noninvasively managed, the primary end point of cardiovascular death, MI, and stroke was lower among those treated with ticagrelor than among those treated with clopidogrel (12.0% vs 14.3%; P = 0.04). In the overall study population, no significant difference existed between ticagrelor and clopidogrel in the overall rate of PLATO major bleeding in patients undergoing CABG surgery, although ticagrelor was associated with a modestly increased rate of PLATO major bleeding not associated with coronary artery bypass graft (CABG) surgery (4.5% vs 3.8%; P =0.03).28 No increased risk of overall or intracranial bleeding existed with ticagrelor therapy in those with a history of stroke or TIA.30 Subsequent analysis of the trial, spurred by the finding of no benefit in the North American cohort of patients, revealed that the benefits of ticagrelor over clopidogrel for reduction in ischaemic events are observed only when the daily aspirin dose is ≤100 mg,31 which is now reflected in a recommendation on package labelling.32
US and European guidelines
ACC/AHA and ESC recommendations regarding DAPT and P2Y12 inhibitors for patients with ACS3,5,33 and those undergoing PCI4,34 are generally similar. Importantly, as discussed above, these guideline recommendations are based to a large extent on phase III randomized trials in which few, if any, East Asian patients (or those of East Asian descent) were enrolled. Neither ACC/AHA nor ESC guidelines make any specific recommendations according to ethnicity.
P2Y12 inhibitors in East Asian patients
Pharmacokinetics and pharmacodynamics
Although the degree of antiplatelet effect with clopidogrel treatment is dependent on multiple clinical and pharmacogenetic variables, the CYP2C19 loss-of-function alleles (*2–*8) are a main determinant of degree of platelet inhibition (Figure 1).35 Compared with white individuals, East Asian individuals have a higher prevalence of a CYP2C19 loss-of-function allele.35 Approximately 30% of white individuals are carriers of a CYP2C19 loss-of-function allele (mostly the *2 allele), whereas about 65% of East Asian individuals carry a CYP2C19 loss-of-function allele (mostly the *2 or *3 alleles).9,35 This finding has been correlated with a higher level of platelet reactivity during clopidogrel treatment in East Asian patients than in white patients.9
By contrast, the degree of platelet inhibition with prasugrel and ticagrelor is higher in East Asian patients than in white patients, but the underlying mechanisms for this finding remain unknown. In individual studies, the level of the prasugrel active metabolite was 30–47% higher in East Asian patients than in white patients after loading and maintenance doses.36,37,38,39,40 After adjusting for body mass, active metabolite exposure was still 19% higher in East Asian patients than in white patients,40 and this finding was more prominent (45–56% higher) in patients with a low body mass (<60 kg).38 The higher exposure of the prasugrel active metabolite in East Asian individuals than in white patients translates into the pharmacodynamic profile.36,37,38,39,40,41,42 In a single-centre study of healthy volunteers, the level of inhibition of platelet aggregation induced by 20 μmol/l ADP in East Asian individuals taking 5 mg of prasugrel daily did not differ from that in white individuals taking 10 mg of prasugrel daily (mean value at 4 h last-dose: 68.9% vs 70.1%).40 In Japanese patients undergoing PCI, 15 mg loading and 3.75 mg maintenance doses of prasugrel achieved a faster, higher, and more-consistent antiplatelet effect than 300 mg loading and 75 mg maintenance doses of clopidogrel.41 Likewise, the exposure of ticagrelor and its major active metabolite (AR-C124910XX) was higher in East Asian individuals than in white individuals after loading and maintenance doses.43,44,45 After a 200 mg loading dose of ticagrelor, Japanese volunteers had a higher exposure of ticagrelor and AR-C124910XX compared with white individuals (ratio of geometric means 1.18, 90% CI 0.76–1.84 for ticagrelor; and 1.28, 90% CI 1.01–1.62 for AR-C124910XX).44 After multiple doses of ticagrelor (100 mg twice daily), the exposure of ticagrelor and AR-C124910XX was 40% (90% CI 1.11–1.78) and 48% (90% CI 1.27–1.71) higher in Japanese volunteers than in white volunteers, which remained 20% and 24% higher in these groups after adjusting for body mass.44 During ticagrelor treatment (90 mg twice daily) in patients with ACS, the systemic exposure in East Asian patients was approximately 40% higher than in white patients.45 The higher exposure of ticagrelor and its major active metabolite in East Asian individuals compared with white individuals correlates with the level of platelet inhibition, especially during maintenance treatment.44 After ticagrelor administration (100 mg twice daily for 9 days), the maximal level of inhibition of platelet aggregation (final extent) in Japanese volunteers was significantly higher than that in white volunteers (99% vs 85%).44
Trial evidence for ACS or PCI
Other than from the COMMIT trial,24 into which investigators enrolled only Chinese patients, only minimal data are available from the major ACS and PCI studies on clopidogrel therapy (in addition to standard contemporaneous therapy) in East Asian patients (Table 1). Investigators in early trials, such as CURE,13 CREDO,46 and CLARITY-TIMI 28,47 did not enrol participants in Asia. Most of the Asian patients included in CHARISMA10 were from Hong Kong, Malaysia, Singapore, and Taiwan, but only a regional analysis was conducted.
Only limited data exist on the comparison between the newer P2Y12 inhibitors (prasugrel and ticagrelor) and clopidogrel in East Asian patients with ACS or undergoing PCI (Table 1). Investigators in TRITON-TIMI 38,25 in which prasugrel was compared with clopidogrel, enrolled <1% of patients from East Asia. In the PLATO trial,28 in which ticagrelor was compared with clopidogrel, only 644 patients were enrolled from East Asian countries (China, including Hong Kong; South Korea; and Taiwan; but not Japan), but a subgroup analysis of only these patients has not been reported. A comparison of outcomes in all Asian (n = 1,106) versus non-Asian (n = 17,515) patients has been reported in abstract form, and found no significant differences between the two groups in the primary composite outcome (cardiovascular death, MI, and stroke), major bleeding, or net clinical benefit.48
The relative efficacy and safety of the newer P2Y12 inhibitors compared with clopidogrel has been specifically examined in East Asian patients in only three modestly sized trials, one of which (the PRASFIT-ACS study49) has been published in a peer-reviewed journal. The results of two other trials cannot be considered to provide the same level of evidence.
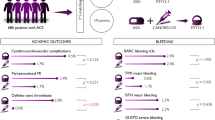
In the phase III, double-blind, randomized PRASFIT-ACS trial,49 the clinical efficacy and safety of low-dose prasugrel (20 mg loading and 3.75 mg daily maintenance) was compared with clopidogrel (300 mg loading and 75 mg daily maintenance) in 1,363 Japanese patients with ACS who were undergoing PCI. The incidence of the primary composite end point (cardiovascular death, nonfatal MI, and ischaemic stroke) was numerically lower with prasugrel than with clopidogrel, but this difference was not significant (9.4% vs 11.8%; HR 0.77, 95% CI 0.56–1.07, P = 0.12).49 TIMI major bleeding not associated with CABG surgery occurred in 1.9% of patients receiving prasugrel and 2.2% of those receiving clopidogrel (HR 0.82, 95% CI 0.39–1.73, P = 0.38).49 The incidence of TIMI major, minor, or clinically relevant bleeding was 9.6% in both groups.49
The results of PRASFIT-ELECTIVE study50 were presented in 2013, but have not been peer-reviewed or published. In this phase III study involving 742 Japanese patients with coronary artery disease (stable angina, previous MI, or silent myocardial ischaemia) and undergoing elective PCI, the incidence of the composite primary end point (cardiovascular death, nonfatal MI, and ischaemic stroke) was 4.1% with prasugrel and 6.7% with clopidogrel.50 The incidence of TIMI major, minor, or clinically relevant bleeding was 5.4% in the low-dose prasugrel group and 6.2% in the clopidogrel group.50 The incidence of TIMI major bleeding was 0% with prasugrel and 2.2% with clopidogrel.50
In the PHILO trial,45 guideline-recommended ticagrelor therapy (180 mg loading and 90 mg twice daily maintenance doses) was compared with clopidogrel therapy (300 mg loading and 75 mg daily maintenance doses) in 801 East Asian (predominantly Japanese) patients with ACS who were scheduled to undergo PCI. The study results are currently available online, but have not been formally presented, peer-reviewed, or published. The incidence of the composite primary end point (cardiovascular death, MI, and stroke) was 10.2% per year with ticagrelor and 8.1% per year with clopidogrel (HR 1.47, 95% CI 0.88–2.44).45 The incidence of the primary safety end point (PLATO major bleeding) was 10.3% per year for ticagrelor and 6.8% per year for clopidogrel (HR 1.54, 95% CI 0.94–2.53).45
The 'East Asian paradox'
Important differences in thrombogenicity, platelet P2Y12-receptor inhibition, and propensity for bleeding complications exist between white and East Asian patients. In the past decade, evidence from numerous clinical studies has demonstrated a strong association between high on-treatment platelet reactivity to ADP and ischaemic events after PCI, particularly stent thrombosis.8 The prevalence of high on-treatment platelet reactivity (assessed using criteria derived from a Western population), is higher among East Asian than among white patients.9 As discussed above, this observation might be primarily caused by a higher frequency of the CYP2C19 loss-of-function alleles in East Asian than in white individuals (∼65% vs ∼30%).35,51,52,53 In addition, multiple clinical studies from South Korea have suggested that different cut-off points for high on-treatment platelet reactivity might be appropriate in East Asian patients compared with white patients.8,54,55,56,57 On the basis of receiver-operating characteristic curve analysis, East Asian patients show a higher level of platelet reactivity than white patients (253–275 versus 208–240 P2Y12 reaction units, measured using the VerifyNow® P2Y12 assay [Accumetrics, USA]).9,55,56,57
Although East Asian patients have a higher prevalence of high on-treatment platelet reactivity during clopidogrel treatment than white patients,9,51 the incidence of adverse ischaemic outcomes or stent thrombosis after PCI is similar or lower than that in white patients.58,59,60,61 Analysis of data from the US National Cardiovascular Data Registry showed that Asian patients undergoing coronary stent implantation had a lower adjusted risk for the composite end point of death, MI, and repeat revascularization than white patients (HR 0.89, 95% CI 0.82–0.96, P value not given).58 In this analysis, the individual end point of death was slightly lower in Asian patients than in white patients, and the incidence of MI was similar in each group. The incidence of stent thrombosis reported in South Korean and Japanese registries (∼0.2% per year) is lower than that in Western registries (∼0.6% per year) after first-generation drug-eluting stent implantation.59,60,61 This finding of a higher prevalence of high on-treatment platelet reactivity, but a thrombotic event rate after PCI that is similar or lower in East Asian patients than in white patients, has been called the 'East Asian paradox'.9
Multiple factors are likely to be associated with the differences in thrombogenicity between East Asian and white individuals, and might explain the variation in propensity for thrombosis. Differences in genetic polymorphisms between ethnicities might partially account for the underlying mechanism.62 For example, factor V Leiden (G1691A) and prothrombin (G20210A) gene mutations are more common in white than in Asian individuals.62 Differences in levels of haemostatic factors (such as fibrinogen, D-dimer, and factor VIII) and plasma endothelial activation markers (such as von Willebrand factor, intercellular adhesion molecule 1, and E-selectin) might be additional factors contributing to the ethnic disparity. Investigators in MESA63 evaluated these factors in individuals from the USA. African-American individuals generally had the highest thrombogenic and dysfunctional endothelial profile, followed by Hispanic and white individuals, and finally East Asian individuals.63 In addition, multiple studies have suggested different levels of inflammatory markers between ethnicities.64 East Asian individuals seem to have lower levels of inflammatory markers (such as C-reactive protein) than white individuals.64 In a study in which thrombus formation and endogenous fibrinolytic capacity were measured using the Global Thrombosis Test (Thromboquest Ltd, UK), healthy Japanese individuals had a longer occlusion time than white British individuals (545 s vs 364 s; P <0.0001), suggesting a lower level of thrombogenicity in East Asian versus white individuals.65
Differences in the propensity for bleeding between East Asian and white populations have also been described.10,11,12 In an analysis of individuals from the USA with atrial fibrillation, Asian patients were at greater risk of warfarin-associated intracranial haemorrhage than white individuals, despite similar international normalized ratios between the two groups.11 In contrast to the risk of ischaemic events after PCI, the risk of serious bleeding in East Asian individuals seems to be greater than in white individuals. In a study of Japanese patients undergoing elective implantation of a drug-eluting stent and treated with aspirin plus a thienopyridine (200 mg daily of ticlopidine or 75 mg daily of clopidogrel), a notable 6.5% incidence of major bleeding was observed during the 16 months of DAPT.66 Major bleeding occurred more frequently in high-responders than in other groups (15.0% vs 4.2%; P = 0.02).66 The ACCEL-BLEED trial67 was designed to examine the relationship between platelet reactivity and bleeding episodes in South Korean patients treated with PCI. This study showed that East Asian patients might be more likely to have mild bleeding than white patients at the same level of on-treatment platelet reactivity, further supporting the hypothesis that the relationship between platelet reactivity and bleeding episodes might vary with ethnicity.
Taken together, these data suggest that clinically important differences in thrombogenicity and propensity for bleeding complications might exist between white patients, on whom most study data and guidelines are based, and East Asian patients. The findings also suggest that the optimal 'therapeutic window' of platelet reactivity might differ between white and East Asian patients (Figure 2). Considering these apparent differences in thrombogenicity and response to P2Y12-receptor inhibitors, extrapolation of major trials of DAPT, as well as guidelines based on these trials, might not be applicable to East Asian patients.
Selected national guideline recommendations
China
Between September 2004 and May 2006, <20% of patients with ACS in China were estimated to have received 12 months of DAPT.68 In a large, multinational, Asian registry of patients with ACS, of whom most were Chinese, 51.4% of those with a final diagnosis of ACS were classified as having ST-segment elevation MI.69 Chinese cardiologists largely follow the ACC/AHA guidelines when treating patients with ACS, and the Chinese recommendations for antiplatelet therapy in patients with ACS70,71 are generally similar to those of the ACC/AHA.
Japan
In contrast to Western countries, the incidence of ST-segment elevation MI in Japan is greater than that of non-ST-segment elevation MI.72 Clopidogrel was approved in Japan in 2006, but only for stroke prevention. Before October 2007, clopidogrel was not used in Japanese patients with ACS. Instead, ticlopidine was widely used. However, on the basis of a study in Japanese patients with ACS in which clopidogrel was shown to have a better safety profile than ticlopidine,73 clopidogrel has subsequently been adopted for the treatment of these patients. Japanese doctors have reduced the dose of ticlopidine (100 mg twice daily instead of the usual 250 mg twice daily) to decrease bleeding complications, and this strategy has been extrapolated to clopidogrel therapy. Therefore, both 75 mg and 25 mg tablets of clopidogrel are available for Japanese patients. In Japanese patients treated with clopidogrel, the dose of clopidogrel is often reduced from 75 mg daily during the first 3 months of treatment, to 50 mg daily from 3 months to 1 year, most commonly in patients with stable coronary artery disease who have undergone PCI. After 1 year of treatment with clopidogrel, the dose if often further reduced to 25 mg. As of February 2014, both 5.00 mg and 3.75 mg doses of prasugrel are approved for patients with either ACS or stable coronary artery disease who are undergoing PCI, on the basis of several phase III trials conducted in Japan.49,50 Ticagrelor is not currently approved in Japan.
South Korea
The South Korean guidelines74 for antiplatelet therapy in patients with ACS mostly parallel recommendations in the ACC/AHA and ESC guidelines on antiplatelet therapy. Interestingly, cilostazol is recommended as an adjunct to DAPT with aspirin and clopidogrel in selected patients, because many pharmacodynamic and clinical studies have demonstrated its clinical efficacy and safety in South Korean patients with ACS.74 In South Korea, prasugrel and ticagrelor are now available and reimbursed for the treatment of patients with ACS. Although clopidogrel has been used as the first-line antiplatelet treatment, the use of prasugrel and ticagrelor is becoming increasingly common. However, many South Korean physicians have suggested that the recommended doses of prasugrel and ticagrelor might be too high for South Korean patients and have expressed concerns about an increased risk of bleeding. Furthermore, many physicians in South Korea have adopted a selective and limited approach using genotyping and platelet-function testing.
Conclusions
A summary of observations and conclusions that can be made from the available study data is given in Box 2. At present, few randomized data on the efficacy and safety of P2Y12-receptor inhibitors for the treatment of East Asian patients with ACS or undergoing PCI, other than those from the COMMIT trial,24 have been published. No data specific to East Asian patients are available to demonstrate the superiority of prasugrel or ticagrelor over clopidogrel, which will be an important area for future research. The 'East Asian paradox' describes a phenomenon in which, despite a higher level of platelet reactivity during clopidogrel treatment, East Asian patients have a similar or lower rate of ischaemic events after PCI compared with white patients. These observations and conclusions should be taken into consideration during the development of regional and national guidelines for East Asian patients with ACS or undergoing PCI.
References
WHO. 65th World Health Assembly closes with new global health measures [online], (2012).
WHO. Global status report on noncommunicable diseases 2010 [online], (2010).
Hamm, C. W. et al. ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: the Task Force for the Management of Acute Coronary Syndromes (ACS) in Patients Presenting Without Persistent ST-segment Elevation of the European Society of Cardiology (ESC). Eur. Heart J. 32, 2999–3054 (2011).
Levine, G. N. et al. 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. Circulation 124, e574–e651 (2011).
O'Gara, P. T. et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 61, e78–e140 (2013).
Wijns, W. et al. Guidelines on myocardial revascularization: the Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS). Eur. Heart J. 31, 2501–2555 (2010).
Jneid, H. et al. 2012 ACCF/AHA focused update of the guideline for the management of patients with unstable angina/non-ST-elevation myocardial infarction (updating the 2007 guideline and replacing the 2011 focused update): a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 126, 875–910 (2012).
Tantry, U. S. et al. Consensus and update on the definition of on-treatment platelet reactivity to adenosine diphosphate associated with ischemia and bleeding. J. Am. Coll. Cardiol. 62, 2261–2273 (2013).
Jeong, Y.-H. “East Asian paradox”: challenge for the current antiplatelet strategy of “one-guideline-fits-all races” in acute coronary syndrome. Curr. Cardiol. Rep. 16, 485 (2014).
Mak, K. H. et al. Ethnic variation in adverse cardiovascular outcomes and bleeding complications in the Clopidogrel for High Atherothrombotic Risk and Ischemic Stabilization, Management, and Avoidance (CHARISMA) study. Am. Heart J. 157, 658–665 (2009).
Shen, A. Y., Yao, J. F., Brar, S. S., Jorgensen, M. B. & Chen, W. Racial/ethnic differences in the risk of intracranial hemorrhage among patients with atrial fibrillation. J. Am. Coll. Cardiol. 50, 309–315 (2007).
Kitamura, A. et al. Proportions of stroke subtypes among men and women > or = 40 years of age in an urban Japanese city in 1992, 1997, and 2002. Stroke 37, 1374–1378 (2006).
Mehta, S. R. & Yusuf, S. The Clopidogrel in Unstable angina to prevent Recurrent Events (CURE) trial programme; rationale, design and baseline characteristics including a meta-analysis of the effects of thienopyridines in vascular disease. Eur. Heart J. 21, 2033–2041 (2000).
Krishna, V., Diamond, G. A. & Kaul, S. Do platelet function testing and genotyping improve outcome in patients treated with antithrombotic agents? The role of platelet reactivity and genotype testing in the prevention of atherothrombotic cardiovascular events remains unproven. Circulation 125, 1288–1303 (2012).
Gurbel, P. A. & Tantry, U. S. Do platelet function testing and genotyping improve outcome in patients treated with antithrombotic agents? Platelet function testing and genotyping improve outcome in patients treated with antithrombotic agents. Circulation 125, 1276–1287 (2012).
Gurbel, P. A., Becker, R. C., Mann, K. G., Steinhubl, S. R. & Michelson, A. D. Platelet function monitoring in patients with coronary artery disease. J. Am. Coll. Cardiol. 50, 1822–1834 (2007).
Bhatt, D. L. Prasugrel in clinical practice. N. Engl. J. Med. 361, 940–94 (2009).
Wiviott, S. D. et al. Prasugrel compared with high loading- and maintenance-dose clopidogrel in patients with planned percutaneous coronary intervention: the Prasugrel in Comparison to Clopidogrel for Inhibition of Platelet Activation and Aggregation—Thrombolysis in Myocardial Infarction 44 trial. Circulation 116, 2923–2932 (2007).
Bhatt, D. L. Antiplatelet therapy: Ticagrelor in ACS—what does PLATO teach us? Nat. Rev. Cardiol. 6, 737–738 (2009).
Yusuf, S. et al. Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation. N. Engl. J. Med. 345, 494–502 (2001).
Mehta, S. R. et al. Effects of pretreatment with clopidogrel and aspirin followed by long-term therapy in patients undergoing percutaneous coronary intervention: the PCI-CURE study. Lancet 358, 527–533 (2001).
Steinhubl, S. R. et al. Early and sustained dual oral antiplatelet therapy following percutaneous coronary intervention: a randomized controlled trial. JAMA 288, 2411–2420 (2002).
Steinhubl, S. R., Berger, P. B., Brennan, D. M. & Topol, E. J. Optimal timing for the initiation of pre-treatment with 300 mg clopidogrel before percutaneous coronary intervention. J. Am. Coll. Cardiol. 47, 939–943 (2006).
Chen, Z. M. et al. Addition of clopidogrel to aspirin in 45,852 patients with acute myocardial infarction: randomised placebo-controlled trial. Lancet 366, 1607–1621 (2005).
Wiviott, S. D. et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N. Engl. J. Med. 357, 2001–2015 (2007).
Wiviott, S. D. et al. Greater clinical benefit of more intensive oral antiplatelet therapy with prasugrel in patients with diabetes mellitus in the Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet Inhibition with Prasugrel—Thrombolysis in Myocardial Infarction 38. Circulation 118, 1626–1636 (2008).
Roe, M. T. et al. Prasugrel versus clopidogrel for acute coronary syndromes without revascularization. N. Engl. J. Med. 367, 1297–1309 (2012).
Wallentin, L. et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N. Engl. J. Med. 361, 1045–1057 (2009).
James, S. K. et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes intended for non-invasive management: substudy from prospective randomised PLATelet inhibition and patient Outcomes (PLATO) trial. BMJ 342, d3527 (2011).
James, S. K. et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes and a history of stroke or transient ischemic attack. Circulation 125, 2914–2921 (2012).
Mahaffey, K. W. et al. Ticagrelor compared with clopidogrel by geographic region in the Platelet Inhibition and Patient Outcomes (PLATO) trial. Circulation 124, 544–554 (2011).
Center for Drug Evaluation and Research. Brilinta REMS document. NDA 22-433 [online], (2011).
Anderson, J. L. et al. 2012 ACCF/AHA focused update incorporated into the ACCF/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-elevation myocardial infarction. Circulation 127, e663–e828 (2013).
Kolh, P. et al. Guidelines on myocardial revascularization: the Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS) Eur. Heart J. 31, 2501–2555 (2010).
Scott, S. A. et al. Clinical Pharmacogenetics Implementation Consortium guidelines for CYP2C19 genotype and clopidogrel therapy: 2013 update. Clin. Pharmacol. Ther. 94, 317–323 (2013).
Yu, K. S. et al. Pharmacokinetic and pharmacodynamic effects of prasugrel in healthy Korean males. J. Cardiovasc. Pharmacol. 62, 72–77 (2013).
Cui, Y. M. et al. Pharmacokinetics and pharmacodynamics of single and multiple doses of prasugrel in healthy native Chinese subjects. Acta Pharmacol. Sin. 33, 1395–1400 (2012).
Small, D. S., et al. Integrated analysis of pharmacokinetic data across multiple clinical pharmacology studies of prasugrel, a new thienopyridine antiplatelet agent. J. Clin. Pharmacol. 51, 321–332 (2011).
Small, D. S. et al. Pharmacodynamics and pharmacokinetics of single doses of prasugrel 30 mg and clopidogrel 300 mg in healthy Chinese and white volunteers: an open-label trial. Clin. Ther. 32, 365–379 (2010).
Small, D. S. et al. The pharmacokinetics and pharmacodynamics of prasugrel in healthy Chinese, Japanese, and Korean subjects compared with healthy Caucasian subjects. Eur. J. Clin. Pharmacol. 66, 127–135 (2010).
Yokoi, H., Kimura, T., Isshiki, T., Ogawa, H. & Ikeda, Y. Pharmacodynamic assessment of a novel P2Y12 receptor antagonist in Japanese patients with coronary artery disease undergoing elective percutaneous coronary intervention. Thromb. Res. 129, 623–628 (2012).
Kim, M. H., Zhang, H. Z. & Jung, D. K. Pharmacodynamic comparisons for single loading doses of prasugrel (30 mg) and clopidogrel (600 mg) in healthy Korean volunteers. Circ. J. 77, 1253–1259 (2013).
Li, H., Butler, K., Yang, L., Yang, Z. & Teng R. Pharmacokinetics and tolerability of single and multiple doses of ticagrelor in healthy Chinese subjects: an open-label, sequential, two-cohort, single-centre study. Clin. Drug Investig. 32, 87–97 (2012).
Teng, R. & Butler, K. Pharmacokinetics, pharmacodynamics, and tolerability of single and multiple doses of ticagrelor in Japanese and Caucasian volunteers. Int. J. Clin. Pharmacol. Ther. 52, 478–491 (2014).
AstraZeneca. Study to assess safety and efficacy of ticagrelor (AZD6140) versus clopidogrel in Asian/Japanese patients with non-ST or ST elevation acute coronary syndromes (ACS) [online], (2014).
Beinart, S. C. et al. Long-term cost effectiveness of early and sustained dual oral antiplatelet therapy with clopidogrel given for up to one year after percutaneous coronary intervention results: from the Clopidogrel for the Reduction of Events During Observation (CREDO) trial. J. Am. Coll. Cardiol. 46, 761–769 (2005).
Sabatine, M. S., McCabe, C. H., Gibson, C. M. & Cannon, C. P. Design and rationale of Clopidogrel as Adjunctive Reperfusion Therapy-Thrombolysis in Myocardial Infarction (CLARITY-TIMI) 28 trial. Am. Heart J. 149, 227–233 (2005).
Kang, H.-J. et al. Net clinical benefits of ticagrelor compared with clopidogrel in Asian acute coronary syndrome patients: a PLATO sub-study [abstract]. Circulation 128, A17001 (2013).
Saito, S. et al. Efficacy and safety of adjusted-dose prasugrel compared with clopidogrel in Japanese patients with acute coronary syndrome: the PRASFIT-ACS study. Circ. J. 78, 1684–1692 (2014).
Nakamura, M. et al. PRASugrel For Japanese PatIenTs with Coronary Artery Disease Undergoing Elective PCI (PRASFIT-Elective) study. Presented at the 22nd Annual Meeting of the Japanese Association of Cardiovascular Intervention and Therapeutics (2013).
Kim, I. S., Choi, B. R., Jeong, Y. H., Kwak, C. H. & Kim, S. The CYP2C19*2 and CYP2C19*3 polymorphisms are associated with high post-treatment platelet reactivity in Asian patients with acute coronary syndrome. J. Thromb. Haemost. 7, 897–899 (2009).
Liang, Z. Y. et al. The impact of gene polymorphism and high on-treatment platelet reactivity on clinical follow-up: outcomes in patients with acute coronary syndrome after drug-eluting stent implantation. EuroIntervention 9, 316–327 (2013).
Wei, W. et al. Prevalence of CYP2C19 polymorphisms involved in clopidogrel metabolism in Fujian Han population [Chinese]. Zhonghua Yi Xue Yi Chuan Xue Za Zhi 29, 420–425 (2012).
Price, M. J. et al. Platelet reactivity and cardiovascular outcomes after percutaneous coronary intervention: a time-dependent analysis of the Gauging Responsiveness with a VerifyNow P2Y12 assay: Impact on Thrombosis and Safety (GRAVITAS) trial. Circulation 124, 1132–1137 (2011).
Ko, Y. G. et al. Comparison of 2 point-of-care platelet function tests, VerifyNow assay and multiple electrode platelet aggregometry, for predicting early clinical outcomes in patients undergoing percutaneous coronary intervention. Am. Heart J. 161, 383–390 (2011).
Suh, J. W. et al. Multicenter randomized trial evaluating the efficacy of cilostazol on ischemic vascular complications after drug-eluting stent implantation for coronary heart disease: results of the CILON-T (influence of CILostazol-based triple antiplatelet therapy ON ischemic complication after drug-eluting stenT implantation) trial. J. Am. Coll. Cardiol. 57, 280–289 (2011).
Ahn, S. G. et al. Different prognostic significance of high on-treatment platelet reactivity as assessed by the VerifyNow P2Y12 assay after coronary stenting in patients with and without acute myocardial infarction. JACC Cardiovasc. Interv. 5, 259–267 (2012).
Kumar, R. S. et al. Effect of race and ethnicity on outcomes with drug-eluting and bare metal stents: results in 423,965 patients in the linked National Cardiovascular Data Registry and centers for Medicare & Medicaid services payer databases. Circulation 127, 1395–1403 (2013).
Daemen, J. et al. Early and late coronary stent thrombosis of sirolimus-eluting and paclitaxel-eluting stents in routine clinical practice: data from a large two-institutional cohort study. Lancet 369, 667–678 (2007).
Kimura, T. et al. Antiplatelet therapy and stent thrombosis after sirolimus-eluting stent implantation. Circulation 119, 987–995 (2009).
Park, D. W. et al. Stent thrombosis, clinical events, and influence of prolonged clopidogrel use after placement of drug-eluting stent data from an observational cohort study of drug-eluting versus bare-metal stents. JACC Cardiovasc. Interv. 1, 494–503 (2008).
Ye, Z. et al. Seven haemostatic gene polymorphisms in coronary disease: meta-analysis of 66,155 cases and 91,307 controls. Lancet 367, 651–658 (2006).
Lutsey, P. L. et al. Plasma hemostatic factors and endothelial markers in four racial/ethnic groups: the MESA study. J. Thromb. Haemost. 4, 2629–2635 (2006).
Kelley-Hedgepeth, A. et al. Ethnic differences in C-reactive protein concentrations. Clin. Chem. 54, 1027–1037 (2008).
Gorog, D. A. et al. First direct comparison of platelet reactivity and thrombolytic status between Japanese and Western volunteers: possible relationship to the “Japanese paradox”. Int. J. Cardiol. 152, 43–48 (2011).
Tsukahara, K. et al. Impact of high-responsiveness to dual antiplatelet therapy on bleeding complications in patients receiving drug-eluting stents. Circ. J. 74, 679–685 (2010).
Jeong, Y.-H. et al. Correlation between platelet reactivity and type of post-discharge bleeding events in PCI-treated patients: result of the ACCEL-BLEED study [abstract]. J. Am. Coll. Cardiol. 58 (Suppl. 1), B221 (2011).
US National Library of Medicine. ClinicalTrials.gov[online], (2013).
Huo, Y. et al. Contemporary pre-hospital management of acute coronary syndromes patients: results from the EPICOR Asia study [abstract]. Circulation 128, A14546 (2013).
Chinese Society of Cardiology. Guidelines for the management of acute STEMI. Chin. J. Cardiol. 38, 675–690 (2010).
Chinese Society of Cardiology. Guidelines for the management of NSTE ACS. Chin. J. Cardiol. 40, 353–367 (2012).
Miyauchi, K. & Daida, H. One-year follow-up data of a 2-year study in patients initially hospitalized with acute coronary syndrome: PACIFIC [online], (2011).
Goto, S. & Toda, E. Antiplatelet therapy after coronary intervention in Asia and Japan: the Asian perspective of antiplatelet intervention. Hamostaseologie 29, 321–325 (2009).
Korean guideline for antiplatelet selection in ACS patients [online], (2014).
Sabatine, M. S. et al. Addition of clopidogrel to aspirin and fibrinolytic therapy for myocardial infarction with ST-segment elevation. N. Engl. J. Med. 352, 1179–1189 (2005).
Sabatine, M. S. et al. Effect of clopidogrel pretreatment before percutaneous coronary intervention in patients with ST-elevation myocardial infarction treated with fibrinolytics: the PCI-CLARITY study. JAMA 294, 1224–1232 (2005).
Schömig, A. et al. A randomized comparison of antiplatelet and anticoagulant therapy after the placement of coronary-artery stents. N. Engl. J. Med. 334, 1084–1089 (1996).
Leon, M. B. et al. A clinical trial comparing three antithrombotic-drug regimens after coronary-artery stenting. N. Engl. J. Med. 339, 1665–1671 (1998).
Mehta, S. R. et al. Double-dose versus standard-dose clopidogrel and high-dose versus low-dose aspirin in individuals undergoing percutaneous coronary intervention for acute coronary syndromes (CURRENT-OASIS 7): a randomised factorial trial. Lancet 376, 1233–1243 (2010).
AstraZeneca. Ticagrelor: NDA 22-433: briefing document for Cardiovascular and Renal Drugs Advisory Committee meeting [online], (2010).
Price, M. J. et al. Standard- vs high-dose clopidogrel based on platelet function testing after percutaneous coronary intervention: the GRAVITAS randomized trial. JAMA 305, 1097–1105 (2011).
Collet, J. P. et al. Bedside monitoring to adjust antiplatelet therapy for coronary stenting. N. Engl. J. Med. 367, 2100–2109 (2012).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Y.-H.J. has received honoraria for lectures from AstraZeneca, Daiichi Sankyo/Lilly, Haemonetics, Nanosphere, Otsuka, and Sanofi-Aventis; and research grants or support from Accumetrics, Boehringer-Ingelheim, Han-mi Pharmaceuticals, Haemonetics, and Otsuka. S.G. has received honoraria from Asteras, AstraZeneca, Bayer, Daiichi-Sankyo, Eisai, Medtronic-Japan, Mochida, MSD, Novartis, Otsuka, Pfizer, Sanofi-Aventis, Takeda, and Tanabe-Mitsubishi. He is an advisory board member for AstraZeneca, Bayer, MSD, and Pfizer/BMS. He is an investigator on a study or trial sponsored by AstraZeneca, Bayer, MSD, and Pfizer/BMS. J.L.A. served on an Acute Coronary Syndrome (ACS) Expert Panel to generate a position paper on advances in ACS therapy that was funded by an unrestricted educational grant from Sanofi-Aventis (France). J.L.M. served as an investigator on a study or trial sponsored by Accumetrics, AstraZeneca, Bayer Healthcare, Bristol-Myers Squibb, Daiichi Sankyo, Eli Lilly, Johnson & Johnson, Nanosphere, and Sanofi-Aventis. G.N.L., Y.H., K.T., and S.C.S. declare no competing interests.
Rights and permissions
About this article
Cite this article
Levine, G., Jeong, YH., Goto, S. et al. World Heart Federation expert consensus statement on antiplatelet therapy in East Asian patients with ACS or undergoing PCI. Nat Rev Cardiol 11, 597–606 (2014). https://doi.org/10.1038/nrcardio.2014.104
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2014.104
This article is cited by
-
Ticagrelor Steady-State Trough Concentration in Chinese Patients Undergoing Percutaneous Coronary Intervention
European Journal of Drug Metabolism and Pharmacokinetics (2024)
-
Diagnostic ability of Japanese version of high bleeding risk criteria for ischemic outcomes in patients with acute myocardial infarction
Heart and Vessels (2024)
-
Real-world evidence of switching P2Y12 receptor–inhibiting therapies to prasugrel after PCI in patients with ACS: results from EFF-K registry
BMC Cardiovascular Disorders (2023)
-
Impact of Low-Dose Prasugrel on Platelet Reactivity in Chronic Phase of Post-Percutaneous Coronary Intervention (CHAPERON): a Prospective Cohort Study
Cardiovascular Drugs and Therapy (2023)
-
Early Guideline-Directed Medical Therapy and in-Hospital Major Bleeding Risk in ST-Elevation Myocardial Infarction Patients Treated with Percutaneous Coronary Intervention: Findings from the CCC-ACS Project
Cardiovascular Drugs and Therapy (2023)