Abstract
Selective serotonergic reuptake inhibitors (SSRIs) and cognitive therapies are effective in the treatment of anxiety and depression. Previous research suggests that both forms of treatments may work by altering cognitive biases in the processing of affective information. The current study assessed the effects of combining an SSRI with a cognitive intervention on measures of affective processing bias and resilience to external challenge. A total of 62 healthy participants were randomly assigned to receive either 7 days of citalopram (20 mg) or placebo capsules while also completing either an active or a control version of a computerized cognitive bias training task. After treatment, standard measures of affective processing bias were collected. Participants’ resilience to external stress was also tested by measuring the increase in negative symptoms induced by a negative mood induction. Participants who received both citalopram and the active cognitive bias training task showed a smaller alteration in emotional memory and categorization bias than did those who received either active intervention singly. The degree to which memory for negative information was altered by citalopram predicted participants’ resistance to the negative mood induction. These results suggest that co-administration of an SSRI and a cognitive training intervention can reduce the effectiveness of either treatment alone in terms of anxiety- and depression-relevant emotional processing. More generally, the findings suggest that pinpointing the cognitive actions of treatments may inform future development of combination strategies in mental health.
Similar content being viewed by others
INTRODUCTION
Cognitive models of anxiety and depression highlight the role of affective information-processing biases, such as the tendency to focus selectively on negative at the expense of positive information, in the etiology and maintenance of disorders (Beck et al, 1985; Mathews and MacLeod, 2005). These models predict that interventions that reduce negative processing biases will improve symptoms of emotional disorders by increasing resilience to challenging external events. Consistent with this proposal, antidepressant medications, which are effective in the treatment of anxiety and depression (NICE, 2007, 2009), have been demonstrated to reduce negative and to increase positive biases in non-clinical groups (Harmer et al, 2003; Murphy et al, 2009). The medications seem to have a very similar effect in clinical populations (Harmer et al, 2009; Tranter et al, 2009), suggesting that healthy volunteer studies may be usefully used as a model of the cognitive effects of pharmacological treatments in patients and thus be useful in testing and developing new therapeutic interventions (Harmer, 2008; Harmer et al, 2011).
Psychological treatments such as cognitive behavioral therapy (CBT) have also been reported to influence these kinds of emotional processing measures (Mathews et al, 1995). In addition, more targeted and often implicit cognitive training interventions (MacLeod et al, 2009) have recently been developed with the specific goal of reducing negative and increasing positive biases (see Figure 1c for a description of a cognitive bias training task). These simple, computer-based training tasks have been found to alter processing biases (eg, in attention) in both non-clinical (Browning et al, 2010b; MacLeod et al, 2002) and clinical groups (Amir et al, 2009) and, importantly, have also been found to reduce self-reported symptoms of anxiety and depression (Hakamata et al, 2010; Wells and Beevers, 2009). It is also more straightforward to devise neutral control tasks for training regimes than for complex psychotherapies, and thus training interventions lend themselves much better to the controlled investigations of treatment mechanisms.
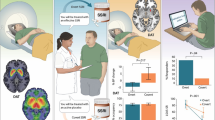
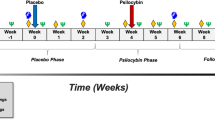
Study design and bias training task used. (a) Participants completed two assessment sessions, immediately before and after the period of treatment. The assessment measures completed during both sessions are listed. (b) Each participant was randomly assigned to one of four treatment groups using a factorial design. This design allows assessment of the main effects of both citalopram and training type, as well as the interaction of the two. (c) Two example trials from the attentional bias training task completed by participants. On each trial, two faces were presented, followed by a probe (one or two dots) to which participants had to respond. During positive training (shown), the probe appeared behind the more positive of the two faces on the majority of trials; the control training condition was identical in every respect other than that the probe was equally likely to appear behind either face.
The results reviewed above suggest that alteration of processing biases, from negative to positive, is a common factor in the therapeutic effects of both pharmacological and cognitive treatments for emotional disorders (Browning et al, 2010a). In the current study, we extended this work by examining how two specific forms of treatments interact; thus, we assessed whether combining a pharmacological and a cognitive treatment leads to an enhanced or diminished effect on processing bias when compared with individually administered treatments.
The mechanisms underlying treatment interactions are of obvious clinical interest as regimes combining pharmacological and psychological interventions are a recognized treatment option in both depression and anxiety (NICE, 2007, 2009). Interestingly, although some evidence from clinical trials in adults does suggest an acute advantage of combination over individually administered treatments (Keller et al, 2000), the advantage conferred seems to be somewhat inconsistent (Cuijpers et al, 2009a; Foa et al, 2002; Furukawa et al, 2007; Pampallona et al, 2004), particularly when the psychological intervention is CBT (Cuijpers et al, 2009b). Indeed, there is evidence to suggest that addition of antidepressants to CBT may reduce the durability of remission in panic disorder (Barlow et al, 2000). From a mechanistic perspective, the limited clinical impact of combination regimes indicates that the two forms of treatment are unlikely to interact synergistically, rather it suggests that either they act independently or actively interfere with each other. If, as hypothesized (Browning et al, 2010a), alterations of affective processing bias mediate the treatments’ clinical effects, then one of these patterns of interaction (independence or interference) should be observed when the impact of combined treatment on affective processing is studied.
This prediction was tested using a factorial experimental design (see Figure 1b) in which non-clinical participants were administered 7 days of the selective serotonin reuptake inhibitor (SSRI) citalopram or a placebo while completing either an active (positive) or a control cognitive bias training task, which was designed to alter attentional bias. In addition to measures of affective processing bias, the impact of interventions on emotional resilience was assessed using subjective ratings of depression and anxiety in response to a negative mood induction. The specific predictions tested were that each active intervention (ie, citalopram and positive cognitive bias training), when administered individually, would induce relatively positive processing biases and increase subsequent emotional resilience. As discussed above, the results from clinical trials suggest that a synergistic interaction between treatments is unlikely; therefore, we hypothesized either no interaction or active interference between the two interventions, although we had no strong rationale for selecting between these options.
MATERIALS AND METHODS
Participants
A total of 64, fluent English-speaking participants who were judged to be healthy on the basis of a medical screen and brief physical examination were recruited. Participants were also screened to exclude current or previous axis I psychiatric disorder or alcohol/substance misuse using the Structured Clinical Interview for the DSM-IV (Spitzer et al, 2002). Other exclusion criteria included taking any psychoactive medication, any significant neurological condition, familiarity with the tasks or stimuli used in the study, or any contraindication to taking SSRI medication. After complete description of the study to participants, written informed consent to the study, which had been approved by a Local NHS Research Ethics Committee, was obtained. Participants were randomized into one of the four treatment groups (see Figure 1b). Treatments were administered for 7 days. Participants were assessed immediately before and after treatment (see Figure 1a). Two participants in the citalopram group experienced side effects (one nausea and one insomnia), which prevented completion of the study and resulted in data being available for 62 participants. For female participants, the study was completed outside the premenstrual week.
Questionnaire Measures
Participants completed questionnaire assessments of depressive (Beck Depression Inventory (Beck et al, 1961)) and anxious symptomatology (Trait subscale of the State-Trait Anxiety Inventory (Spielberger et al, 1983)) as well as state measures of anxiety (state-STAI) and mood (Positive and Negative Affect Scale (PANAS); Watson et al, 1988) both before and after treatment.
Experimental Interventions
Pharmacological intervention. All participants were provided with 7 days supply of either citalopram 20 mg or lactose placebo capsules. The capsules were identical in appearance, and participants were instructed to take them every morning, starting on the following morning and including the day of post-treatment assessment.
Cognitive bias training. The cognitive bias training task used (Figure 1c) was a computerized, face-based, visual-probe training (MacLeod et al, 2002), which has been developed to alter attentional bias to emotional information. Similar tasks have been found to improve symptoms of anxiety and depression (Hakamata et al, 2010; Wells and Beevers, 2009). On the basis of the widely used dot-probe task (MacLeod et al, 1986), a pair of facial expressions (Lundqvist et al, 1998; Matsumoto and Ekman, 1988; Tottenham et al, 2009), was briefly presented and followed by a probe (one or two dots), which appeared behind one of the faces. The faces displayed positive (happy), neutral, or negative (fearful and angry) expressions with each trial of the task displaying faces from two different valences (vertical visual angle of stimuli ≈11°, vertical separation of stimuli ≈3.5°). This resulted in three possible face pair types: positive-neutral, positive-negative, and negative-neutral. The positive training condition included a majority (87.5%) of trials in which the probe replaced the relatively positive face (ie, during negative-neutral trials, the neutral face is relatively more positive, whereas during happy-neutral or happy-negative trials, the happy face is more positive). When completing the positive training, participants learn to deploy their attention toward the relatively positive face as this predicts the probe location; that is, they develop a positive attentional bias. Control training was identical in every respect other than the location of the probe, which was equally often found behind the positive and negative faces. A single session of the task involved two blocks of 48 trials each (each block included 16 trials of the three different face pair combinations). The blocks differed in the duration of time the stimuli were presented (500 or 1000 ms). Previous studies of attentional bias training have tended to use a more restricted range of stimuli valence and presentation durations. However, a concern with using only one type of training trial is that it will limit the degree to which the effects of training generalize from the laboratory to real-world experiences, which is believed to be essential if training is to have a meaningful clinical effect (MacLeod et al, 2009). This concern has prompted recent studies of attentional bias training to deploy various trial types (Hayes et al, 2010) and motivated the range of stimuli valence and presentation times used in the current study. All participants completed the training sessions twice daily at home (Blackwell and Holmes, 2010) using a laptop computer, which was supplied to them for the duration of the study.
Compliance with interventions. Compliance with both pharmacological and bias training interventions was encouraged by providing participants with a log book in which they recorded the date and time that medication had been taken and training completed. In addition, participants were contacted by researchers on three occasions during the treatment week to check whether they were complying with the study protocol.
Assessment Tasks
Emotional word categorization task; assessing emotional bias for self referential information. In all, 60 personality characteristics selected to be extremely disagreeable (eg, hostile) or agreeable (honest; taken from the study by Anderson (1968)) were presented on the computer screen for 500 ms. These words were matched in terms of word length, ratings of frequency, and meaningfulness (Harmer et al, 2004). Participants were asked to categorize whether they would be pleased or upset if they overheard someone else referring to them as possessing the characteristic described by the words, so that the judgment was in part self-referring. Categorization bias is estimated by comparing the mean reaction times to categorize positive vs negative words.
Emotional memory task; assessing memory bias. Recognition and recall of the personality trait words presented in the emotional word categorization task was also assessed (Harmer et al, 2004). During the recognition task, volunteers were asked to indicate whether they recognized the word for each item on a list containing the 60 targets along with 60 matched distractors (30 likeable and 30 dislikeable). Recall was assessed simply by asking participants to list as many words as they could remember from the categorization task. Memory bias is reflected in the relative number of positive vs negative words correctly recognized or recalled.
Visual-probe task; assessing attentional bias. A face-based visual-probe task (MacLeod et al, 1986), was completed before and after treatment to ensure that the bias training intervention had altered attentional function. The task was similar to the bias training task in that attention to a novel set of positive, negative, and neutral faces were assessed (the set of face stimuli used in training vs testing was counterbalanced between participants). During the task, probe location was balanced between the relatively more negative and positive stimuli, and deployment of attention was assessed using blocks of trials in which the stimuli were presented for either 100 ms or for the durations used in training (500 and 1000 ms, order of blocks counterbalanced). This resulted in a total of 144 trials. Importantly, this task is able to assess whether the attentional bias training produced, as expected, a generalized tendency to divert attention away from negative and toward positive information as opposed to a more limited effect on a specific stimuli valence. The estimate of attentional bias is obtained by comparing the mean reaction time when the probe replaces the relatively negative vs positive face (Wilson and MacLeod, 2003).
Mood induction task; assessing emotional reactivity to external events. To assess emotional reactivity to external events, participants were required to complete a mood induction task (Clark, 1983; Velten, 1968). During the task (Holmes et al, 2009), participants listened to sad music (Russia under the Mongolian Yoke by Prokofiev played at 50% normal speed) while reading negative self-referent statements on the computer screen (‘It seems such an effort to do anything’). Such procedures have been reliably shown to produce increased negative mood in non-clinical groups (Clark, 1983). State measures of negative mood (negative-PANAS) and anxiety (state-STAI) were taken before and after the task with the critical outcome being the change in these scores induced by the task.
Statistical Analysis
Mixed model analyses of variance (ANOVAs) were constructed with the between-subject factors of medication (citalopram, placebo) and training (positive, control). This resulted in estimates of the effect of each active intervention (ie, main effects of training and medication) and, critically, an interaction term (medication × training), which assesses for the presence of positive or negative interactions. The emotional word categorization and memory tasks included a single within-subject factor, word valence (positive, negative). Addition of the within-subject factor of test time to the analyses of the questionnaire measures, visual probe, and mood induction tasks allowed changes in these outcomes across time to be assessed. The visual probe task included additional within-subject factors coding for the face pairs presented (positive-neutral, positive-negative, negative neutral). and the durations the face stimuli were presented for (100, 500, 1000 ms), which allowed assessment of whether the training effect was influenced by any of these factors. Baseline questionnaire and demographic measures were analyzed using univariate ANOVAs. After inspection of the data, extreme reaction times (outside 200–800 ms for the visual probe task and 200–1600 ms for the categorization task) were removed before calculating the mean.
RESULTS
Demographic and Baseline Data
The groups were well matched in terms of age, gender, and baseline scores on mood and anxiety measures (see Table 1), indicating that randomization had been successful. There was no effect of either intervention or their interaction on change in any of the baseline measures listed in Table 1 (all p>0.14).
Effects of Interventions on Emotional Biases
Emotional memory. As shown in Figure 2a, the individual interventions of positive training plus placebo or control training plus citalopram produced a relative increase in the number of positive vs negative words recognized, compared with control training plus placebo. In contrast, co-administration of the interventions (positive training plus citalopram) produced no change in memory bias at all. Thus, there was interference between the two interventions for the emotional memory task (Figure 2a; training × medication × emotion; F=5.1, df=1,58, p=0.03).
Effects of interventions on measures of cognitive bias. (a) Emotional memory bias, calculated as the relative accuracy in the recognition of positive vs negative words. An interference pattern is seen (F=5.1, df=1,58, p=0.03); when compared with the baseline group (control placebo) both interventions, administered singly, produce a relative increase in positive memory bias, whereas the combination treatment does not. (b) The interference effect is apparent in the mean number of negative words recognized (F=12.6, df=1,58, p=0.001). Both citalopram and positive training significantly decrease recognition of negative words, whereas the combination of interventions does not differ from the baseline group and shows increased memory of negative words compared with the singly administered interventions. The results of the post hoc pairwise comparisons are shown, *p<0.05, ^p<0.1. (c) Emotional bias when categorizing self-referent words, calculated as the relative reaction time to classify negative vs positive words. A negative interference pattern is again seen (F=4.5, df=1,58, p=0.038), with each intervention administered singly reducing the relative reaction time difference between negative and positive words, whereas the combination of interventions again has very little effect. All graphs display mean scores with error bars reporting SE.
This effect on overall emotional bias was driven by a pronounced training × medication interaction for recognition of negative words (Figure 2b; F=12.6, df=1,58, p=0.001), with a similar pattern being found, to a significantly reduced extent, for the recognition of positive words (not illustrated; F=4.4, df=1,58 p=0.04). Post hoc analysis (Figure 2b) revealed that each intervention on its own produced a significant reduction in the number of negative words recognized, whereas the combination of interventions produced no change from baseline. Indeed, the combined intervention group displayed increased recognition memory for negative words when compared with the individual intervention groups.
Analysis of the number of words recalled, as opposed to recognized, revealed no significant effects of either intervention or their interaction (all p>0.38).
Emotional word categorization. The speed of word categorization also displayed an interference effect with a similar pattern to that displayed in word recognition (Figure 2c; training × medication × emotion; F=4.5, df=1,58, p=0.04). Thus, participants who received a single active intervention displayed a decrease in the reaction time to categorize negative vs positive words, whereas the combination group displayed less effect. Post hoc analysis comparing the differences between the groups did not reach statistical significance.
Did Bias Training Alter Attentional Function?
As expected, positive attentional bias training, when compared with control training, led to a general increase in attentional bias toward positive faces (training × time × probe location; F=7.0, df=1,58, p=0.01). This effect was not modified by the duration at which the stimuli were presented, the face pair types which were presented, or the medication group (all p>0.3). For further analysis of the visual probe data, see Supplementary Methods.
Did the Interventions Alter Resilience to the Mood Induction?
Citalopram protected participants against the negative effects of the mood induction task (Figure 3). Relative to participants who received placebo, those who took citalopram (NB both the citalopram control and citalopram-positive groups) displayed a smaller average increase in negative-PANAS score (time × drug; F=6.9, df=1,58, p=0.01). The cognitive bias training group (positive vs control) did not influence emotional resilience (time × training; F=0.9, df=1,58, p=0.35) and there was no interaction between the interventions (time × drug × training; F=0.7, df=1,58, p=0.39). The results from the emotional bias tasks suggest that the protective effect of citalopram should be eroded in the group which also completed positive bias training and, although an overall interaction effect was not found in the omnibus ANOVA, inspection of Figure 3 suggests such a pattern. Statistical comparison of the citalopram control and citalopram-positive groups indicated that this predicted effect was present at a trend level (F=3.6, df=1, 29, p=0.07).
Effects of the interventions on emotional reactivity across the mood induction procedure. Measures of negative affect (negative-PANAS) were taken before and after the mood induction task. As can be seen, participants in the citalopram-treated groups (control citalopram and positive citalopram) displayed a smaller increase in negative symptoms than did those in the placebo groups (time × drug; F=6.9, df=1,58, p=0.01). Direct comparison between the two citalopram-treated groups revealed a trend level effect of training (F=3.6, df=1, 29, p=0.07). Consistent with the effects of the interventions on emotional biases, the addition of positive bias training to citalopram tended to reduce the protective effect of the drug.
Participants’ anxious symptoms, as measured by the state-STAI, were not influenced by either intervention or their interaction (all p>0.5).
Were the Cognitive Effects of the Interventions Related to their Effects on Emotional Reactivity?
If, as predicted (Harmer, 2008), the cognitive effects of the interventions mediate their impact on emotional vulnerability, the emotional bias and vulnerability measures should correlate within a treatment group. Consistent with this, a significant positive correlation within citalopram-treated participants was found between the number of negative words recognized during the memory task and the subsequent increase in the negative-PANAS score induced by mood induction (r=0.44, p=0.01). No correlation was found between these measures for the positive bias training group (r=−0.29, p=0.39).
DISCUSSION
The current study is the first to explore the interaction between an SSRI and positive cognitive bias training on biomarker measures relevant to depression and anxiety. In line with predictions, concurrent administration of the pharmacological and psychological active interventions was found to produce an interference effect on measures of emotional memory and categorization bias. Citalopram, but not positive bias training, was found to protect against the effects of the negative mood induction with the degree of protection being predicted by the extent to which the drug reduced memory for negative words. These results provide a conceptual framework for starting to compare and understand the mechanisms of treatment associated with drugs on the one hand and aspects of psychological therapy on the other, for emotional disorders.
The current study used an experimental medicine model to test specific predictions about the mechanisms of treatment interaction within a tightly controlled laboratory setting (Browning et al, 2010a). In line with previous work, both citalopram (Harmer et al, 2004; Murphy et al, 2009) and positive cognitive bias training (Browning et al, 2010b; MacLeod et al, 2002) on their own produced relatively positive changes in emotional bias, consistent with the idea that this may be a common process in treatments of emotional disorders (Harmer, 2008). However, the critical result from the current study is that combining the SSRI with training of positive emotional bias reduced the effect of either alone. As suggested in the ‘Introduction’ section, this cognitive interference effect may provide a plausible mechanism for the modest clinical impact of such combination treatments. More generally, it suggests that laboratory-based assessment of affective processing biases, which is sensitive to the effects of both pharmacological and psychological interventions, presents a valuable opportunity to investigate the mechanisms underlying the interaction between disparate treatments for anxiety and depression.
Using a biomarker model, the results from the current study suggest that combining cognitive bias training of attention with an SSRI may not be a useful intervention strategy for depression and anxiety. Such an effect is consistent with the hypothesis that intact amygdala function is necessary for cognitive bias training to occur and that SSRIs interfere with training by impairing amygdala function (Browning et al, 2010a). However, this mechanism does not explain why cognitive bias training was also found to interfere with the effects of citalopram. If replicated, such a pattern of results may indicate that generalization of the effect of SSRIs to measures of mood and emotional memory only occur when the medication is able to influence participants’ interpretation of emotionally ambiguous events. In other words, if individuals are presented only with positive information (as is the case with positive training), there may be no opportunity for the medication to alter a maladaptive appraisal of the information and thus to improve mood.
It is difficult to generalize these results to the combination of SSRIs with full therapist-delivered CBT. However, adopting an experimental psychopathology approach to CBT suggests that it can be decomposed into theory-driven constituent parts, which may be individually tested. Given this, alteration of attentional processing bias, modeled in the current study using the bias training task, is likely to be only one of the many mechanisms by which complex psychotherapies such as CBT improve mood and anxiety and thus, other facets of CBT may be independent of, or even interact synergistically with, SSRIs. For example, although the current cognitive training regime has targeted attentional bias, it would be interesting to consider whether alteration of the other key biases associated with anxiety and depression, such as interpretation bias (Mathews and MacLeod, 2005), may complement the effects of SSRIs.
More broadly, other forms of pharmacotherapy may interact positively with cognitive bias training regimes. Indeed, an interesting recent study provides some evidence that D-cycloserine may enhance the basic attentional bias training effect (Behar et al, 2010). Perhaps the most promising application of the experimental approach used in the current study will involve identifying the specific combinations of pharmacological and psychological interventions which complement each other, and then testing whether treatment regimes that show potential in the laboratory go on to deliver benefit in the clinic.
Citalopram, but not positive cognitive bias training, was found to protect participants from the effects of a negative mood induction. This is the first demonstration, to our knowledge, that an SSRI can protect healthy volunteers from the effects of negative mood induction in the laboratory and critically, this effect was predicted by the degree to which the medication reduced memory for negative words. Therefore, these results are consistent with the proposal that alterations in affective processing mediate the therapeutic effect of the medication (Harmer, 2008). However, contrary to expectations, the change in bias produced by cognitive training was not sufficient to alter mood resilience and did not mimic the protective effects of the SSRI. A possible explanation for this lack of effect is that the negative mood induction procedure used in the current study may be more suited to investigating depressive rather than anxious vulnerability. Consistent with this, the protective effect of citalopram was evident on a scale of negative affect (the negative-PANAS) rather than a specific measure of anxiety (state-STAI). Although there is evidence that attentional cognitive bias training does ameliorate symptoms of depression, this literature is less consistent (Baert et al, 2010; Wells et al, 2009) than that demonstrating an anxiolytic effect (Hakamata et al, 2010). Thus, the specific emotional challenge used may not be optimal in detecting the impact of training on subjective emotional experience.
Finally, some of the caveats in interpreting the results of this study should be acknowledged. We have suggested that our results may have clinical implications; however, extrapolating these laboratory results to the clinic requires two assumptions. First, it assumes that the degree of affective bias change induced by a treatment is a reasonable proxy for the clinical efficacy of that treatment, and second, it assumes that the cognitive effects of the interventions demonstrated in this study of healthy volunteers are an accurate reflection of their effects in clinical populations. Support for these assumptions is provided by previous work, which has demonstrated that the initial effects of antidepressants on affective bias predict later clinical response (Tranter et al, 2009) and by the similarity between the effects of the treatments on affective biases in non-clinical and clinical populations (Harmer et al, 2004, 2009). Furthermore, the finding that the cognitive effects of citalopram predicted its protective effect during the mood induction task supports a link between affective bias and subjective mood. However, a more direct test of these assumptions would obviously be provided by replicating the current findings in a clinical sample. A second caveat is that the stability and persistence of any cognitive bias training is likely to be influenced both by the reliability of the measures of cognitive bias (see Supplementary Materials and Schmukle, 2005) and by the variability in the induced bias itself (MacLeod et al, 2009; Schlam, 2008). As our study was designed to test the immediate impact of interventions on cognitive functioning and mood reactivity, we did not assess the degree to which the induced biases persisted and remained stable after completion of the treatment. Future studies may be able to address this limitation by retesting the effects of the treatments at later time points. Third, we monitored compliance with the pharmacological aspect of treatment using participants’ self-report only. It would have been reassuring also to have access to serum citalopram levels to objectively confirm compliance. Fourth, we did not collect detailed information on participants’ family history of depression. Given the previous finding that this factor is associated with more pronounced negative mood effects of tryptophan depletion (Klaassen et al, 1999), it would be interesting to investigate whether it also mediated the protective effects of citalopram found during the mood induction task. Finally, it should also be acknowledged that the sample sizes used in the study were relatively modest. Thus, although the study was able to identify significant interactions between the two treatments, other treatment effects may not have been detected because of insufficient power.
The current study has used an experimental medicine approach to investigate how specific psychological and pharmacological interventions for the emotional disorders interact at the cognitive level. The results suggest that active interference occurs between these two interventions such that administering them concurrently produces a smaller effect than when they are administered separately. This provides a plausible conceptual framework for beginning to investigate the modest clinical results seen when the two forms of treatment are combined in clinical settings and suggests that pinpointing the cognitive actions of treatments may inform future development of combination strategies in mental health.
References
Amir N, Beard C, Burns M, Bomyea J (2009). Attention modification program in individuals with generalized anxiety disorder. J Abnorm Psychol 118: 28–33.
Anderson N (1968). Likableness ratings of 555 personality trait words. J Pers Soc Psychol 9: 272–279.
Baert S, De Raedt R, Schacht R, Koster EH (2010). Attentional bias training in depression: therapeutic effects depend on depression severity. J Behav Ther Exp Psychiatry 41: 265–274.
Barlow DH, Gorman JM, Shear MK, Woods SW (2000). Cognitive-behavioral therapy, imipramine, or their combination for panic disorder: a randomized controlled trial. JAMA 283: 2529–2536.
Beck AT, Emery G, Greenberg RL (1985). Anxiety Disorders and Phobias: A Cognitive Perspective. Basic Books: New York.
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J (1961). An inventory for measuring depression. Arch Gen Psychiatry 4: 53–63.
Behar E, McHugh RK, Peckham A, Otto MW (2010). D-cycloserine for the augmentation of an attentional training intervention for trait anxiety. J Anxiety Disord 24: 440–445.
Blackwell SE, Holmes EA (2010). Modifying interpretation and imagination in clinical depression: a single case series using cognitive bias modification. Appl Cogn Psychol 24: 338–350.
Browning M, Holmes EA, Harmer CJ (2010a). The modification of attentional bias to emotional information: a review of the techniques, mechanisms, and relevance to emotional disorders. Cogn Affect Behav Neurosci 10: 8–20.
Browning M, Holmes EA, Murphy SE, Goodwin GM, Harmer CJ (2010b). Lateral prefrontal cortex mediates the cognitive modification of attentional bias. Biol Psychiatry 67: 919–925.
Clark DM (1983). On the induction of depressed mood in the laboratory: evaluation and comparison of the velten and musical procedures. Behav Res Ther 5: 27.
Cuijpers P, Dekker J, Hollon SD, Andersson G (2009a). Adding psychotherapy to pharmacotherapy in the treatment of depressive disorders in adults: a meta-analysis. J Clin Psychiatry 70: 1219–1229.
Cuijpers P, van Straten A, Warmerdam L, Andersson G (2009b). Psychotherapy versus the combination of psychotherapy and pharmacotherapy in the treatment of depression: a meta-analysis. Depress Anxiety 26: 279–288.
Foa EB, Franklin ME, Moser J (2002). Context in the clinic: how well do cognitive-behavioral therapies and medications work in combination? Biol Psychiatry 52: 987–997.
Furukawa TA, Watanabe N, Churchill R (2007). Combined psychotherapy plus antidepressants for panic disorder with or without agoraphobia. Cochrane Database of Systematic Reviews Article number: CD004364.
Hakamata Y, Lissek S, Bar-Haim Y, Britton JC, Fox NA, Leibenluft E et al (2010). Attention bias modification treatment: a meta-analysis toward the establishment of novel treatment for anxiety. Biol Psychiatry 68: 982–990.
Harmer CJ (2008). Serotonin and emotional processing: does it help explain antidepressant drug action? Neuropharmacology 55: 1023–1028.
Harmer CJ, Bhagwagar Z, Perrett DI, Vollm BA, Cowen PJ, Goodwin GM (2003). Acute SSRI administration affects the processing of social cues in healthy volunteers. Neuropsychopharmacology 28: 148–152.
Harmer CJ, Cowen PJ, Goodwin GM (2011). Efficacy markers in depression. J Psychopharmacol, print copy in press (originally published online 8 June 2010, at http://jop.sagepub.com/content/early/2010/06/04/0269881110367722).
Harmer CJ, O’Sullivan U, Favaron E, Massey-Chase R, Ayres R, Reinecke A et al (2009). Effect of acute antidepressant administration on negative affective bias in depressed patients. Am J Psychiatry 166: 1178–1184.
Harmer CJ, Shelley NC, Cowen PJ, Goodwin GM (2004). Increased positive versus negative affective perception and memory in healthy volunteers following selective serotonin and norepinephrine reuptake inhibition. Am J Psychiatry 161: 1256–1263.
Hayes S, Hirsch CR, Mathews A (2010). Facilitating a benign attentional bias reduces negative thought intrusions. J Abnorm Psychol 119: 235–240.
Holmes EA, Lang TJ, Shah DM (2009). Developing interpretation bias modification as a “cognitive vaccine” for depressed mood: imagining positive events makes you feel better than thinking about them verbally. J Abnorm Psychol 118: 76–88.
Keller MB, McCullough JP, Klein DN, Arnow B, Dunner DL, Gelenberg AJ et al (2000). A comparison of nefazodone, the cognitive behavioral-analysis system of psychotherapy, and their combination for the treatment of chronic depression. N Engl J Med 342: 1462–1470.
Klaassen T, Riedel WJ, van Someren A, Deutz NE, Honig A, van Praag HM (1999). Mood effects of 24-hour tryptophan depletion in healthy first-degree relatives of patients with affective disorders. Biol Psychiatry 46: 489–497.
Lundqvist D, Flykt A, Ohman A (1998). KDEF. Karolinska Hospital: Stockholm.
MacLeod CM, Koster EH, Fox E (2009). Whither cognitive bias modification research? Commentary on the special section articles. J Abnorm Psychol 118: 89–99.
MacLeod CM, Mathews A, Tata P (1986). Attentional bias in emotional disorders. J Abnorm Psychol 95: 15–20.
MacLeod CM, Rutherford E, Campbell L, Ebsworthy G, Holker L (2002). Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol 111: 107–123.
Mathews A, MacLeod C (2005). Cognitive vulnerability to emotional disorders. Ann Rev Clin Psychol 1: 167–195.
Mathews A, Mogg K, Kentish J, Eysenck M (1995). Effect of psychological treatment on cognitive bias in generalized anxiety disorder. Behav Res Ther 33: 293–303.
Matsumoto D, Ekman P (1988). Japanese and Caucasian Facial Expressions of Emotion and Neutral Faces (JACFEE and JACNeuF). Human Interaction Laboratory, University of California: San Francisco.
Murphy SE, Yiend J, Lester KJ, Cowen PJ, Harmer CJ (2009). Short-term serotonergic but not noradrenergic antidepressant administration reduces attentional vigilance to threat in healthy volunteers. Int J Neuropsychopharmacol 12: 169–179.
NICE (2007). Management of Anxiety (Panic Disorder, with or without Agoraphobia, and Generalised Anxiety Disorder) in Adults in Primary, Secondary and Community Care (Amended). NICE: London.
NICE (2009). Treatment and Management of Depression in Adults, Including Adults with a Chronic Physical Health Problem. NICE: London.
Pampallona S, Bollini P, Tibaldi G, Kupelnick B, Munizza C (2004). Combined pharmacotherapy and psychological treatment for depression: a systematic review. Arch Gen Psychiatry 61: 714–719.
Schlam TR (2008). The effect of attention training on emotional vulnerability and food consumption following a stressor. Ph.D. thesis, The State University of New-Jersey, Rutgers.
Schmukle SC (2005). Unreliability of the dot probe task. Eur J Pers 19: 595–605.
Spielberger CD, Gorsuch RL, Lushene RD (1983). Manual for the State-Trait Anxiety Inventory (STAI). Consulting Psychologists Press: Palo Alto, CA.
Spitzer RL, Williams JB, Gibbon M (2002). Structured Clinical Interview for the DSM-IV. New York State Psychiatric Institute: New York.
Tottenham N, Tanaka JW, Leon AC, McCarry T, Nurse M, Hare TA et al (2009). The NimStim set of facial expressions: judgments from untrained research participants. Psychiatry Res 168: 242–249.
Tranter R, Bell D, Gutting P, Harmer CJ, Healy D, Anderson IM (2009). The effect of serotonergic and noradrenergic antidepressants on face emotion processing in depressed patients. J Affect Disord 118: 87–93.
Velten Jr E (1968). A laboratory task for induction of mood states. Behav Res Ther 6: 473–482.
Watson D, Clark LA, Tellegen A (1988). Development and validation of brief measures of positive and negative affect: the PANAS scales. J Pers Soc Psychol 54: 1063–1070.
Wells TT, Beevers CG (2009). Biased attention and dysphoria: manipulating selective attention reduces subsequent depressive symptoms. Cogn Emot 24: 719–728.
Wilson E, MacLeod CM (2003). Contrasting two accounts of anxiety-linked attentional bias: selective attention to varying levels of stimulus threat intensity. J Abnorm Psychol 112: 212–218.
Acknowledgements
This research was supported by a Wellcome Trust Fellowship to Dr Browning (081672). Dr Holmes was supported by a Wellcome Trust Clinical Fellowship (088217).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
GMG has held grants from Bailly Thomas, Sanofi-Aventis, and Servier, received honoraria for speaking or chairing educational meetings from AstraZeneca, Bristol-Meyers Squibb, Eisai, Lundbeck, Sanofi-Aventis, and Servier, and advised AstraZeneca, Bristol-Meyers Squibb, Boehringer Ingelheim, Cephalon, Hoffman-Laroche, Janssen-Cilag, Lilly, Lundbeck, P1vital, Roche, Sanofi-aventis, Shering Plough, Servier, and Wyeth. He holds shares in P1vital and acted as expert witness for Lilly and Servier. CJH is on the advisory board of P1vital Ltd and holds shares in this company. She is a company director and holds shares in Oxford Psychologists Ltd. The other authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Neuropsychopharmacology website
Supplementary information
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Browning, M., Grol, M., Ly, V. et al. Using an Experimental Medicine Model to Explore Combination Effects of Pharmacological and Cognitive Interventions for Depression and Anxiety. Neuropsychopharmacol 36, 2689–2697 (2011). https://doi.org/10.1038/npp.2011.159
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2011.159
Keywords
This article is cited by
-
Cognitive neuropsychological theory of antidepressant action: a modern-day approach to depression and its treatment
Psychopharmacology (2021)
-
Attention Bias Modification Training Via Smartphone to Reduce Social Anxiety: A Randomized, Controlled Multi-Session Experiment
Cognitive Therapy and Research (2014)