Abstract
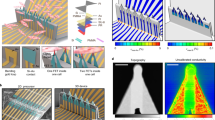
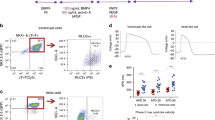
Real-time mapping and manipulation of electrophysiology in three-dimensional (3D) tissues could have important impacts on fundamental scientific and clinical studies, yet realization is hampered by a lack of effective methods. Here we introduce tissue-scaffold-mimicking 3D nanoelectronic arrays consisting of 64 addressable devices with subcellular dimensions and a submillisecond temporal resolution. Real-time extracellular action potential (AP) recordings reveal quantitative maps of AP propagation in 3D cardiac tissues, enable in situ tracing of the evolving topology of 3D conducting pathways in developing cardiac tissues and probe the dynamics of AP conduction characteristics in a transient arrhythmia disease model and subsequent tissue self-adaptation. We further demonstrate simultaneous multisite stimulation and mapping to actively manipulate the frequency and direction of AP propagation. These results establish new methodologies for 3D spatiotemporal tissue recording and control, and demonstrate the potential to impact regenerative medicine, pharmacology and electronic therapeutics.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Change history
21 July 2016
In the version of this Article originally published online, in Fig. 1e, the traces for devices (1,2) and (2,3) were incorrect. This has now been corrected in all versions of the Article. In addition, the original data for Fig. 1d (from which Fig. 1e was extracted) is now provided as Supplementary Data.
References
Langer, R. & Vacanti, J. P. Tissue engineering. Science 260, 920–926 (1993).
Eschenhagen, T. & Zimmermann, W. H. Engineering myocardial tissue. Circ. Res. 97, 1220–1231 (2005).
Shimizu, T. et al. Fabrication of pulsatile cardiac tissue grafts using a novel 3-dimensional cell sheet manipulation technique and temperature-responsive cell culture surfaces. Circ. Res. 90, e40 (2002).
Dvir, T., Timko, B. P., Kohane, D. S. & Langer, R. Nanotechnological strategies for engineering complex tissues. Nature Nanotech. 6, 13–22 (2011).
Papadaki, M. et al. Tissue engineering of functional cardiac muscle: molecular, structural, and electrophysiological studies. Am. J. Physiol. Heart Circ. Physiol. 280, 168–178 (2001).
Hansen, A. et al. Development of a drug screening platform based on engineered heart tissue. Circ. Res. 107, 35–44 (2010).
Grosberg, A., Alford, P. W., McCain, M. L. & Parker, K. K. Ensembles of engineered cardiac tissues for physiological and pharmacological study: heart on a chip. Lab Chip 11, 4165–4173 (2011).
Natarajan, A. et al. Patterned cardiomyocytes on microelectrode arrays as a functional, high information content drug screening platform. Biomaterials 32, 4267–4274 (2011).
Griffith, L. G. & Naughton, G. Tissue engineering-current challenges and expanding opportunities. Science 295, 1009–1014 (2002).
Furuta, A. et al. Pulsatile cardiac tissue grafts using a novel three-dimensional cell sheet manipulation technique functionally integrates with the host heart, in vivo. Circ. Res. 98, 705–712 (2006).
Zimmermann, W. H. et al. Engineered heart tissue grafts improve systolic and diastolic function in infarcted rat hearts. Nature Med. 12, 452–458 (2006).
St-Pierre, F. et al. High-fidelity optical reporting of neuronal electrical activity with an ultrafast fluorescent voltage sensor. Nature Neurosci. 17, 884–889 (2014).
Herron, T. J., Lee, P. & Jalife, J. Optical imaging of voltage and calcium in cardiac cells & tissues. Circ. Res. 110, 609–623 (2012).
Kralj, J. M., Douglass, A. D., Hochbaum, D. R., Maclaurin, D. & Cohen, A. E. Optical recording of action potentials in mammalian neurons using a microbial rhodopsin. Nat. Methods 9, 90–95 (2012).
Huisken, J., Swoger, J., Del Bene, F., Wittbrodt, J. & Stelzer, E. H. K. Optical sectioning deep inside live embryos by selective plane illumination microscopy. Science 305, 1007–1009 (2004).
Kim, D. H. et al. Materials for multifunctional balloon catheters with capabilities in cardiac electrophysiological mapping and ablation therapy. Nature Mater. 10, 316–323 (2011).
Cohen-Karni, T., Timko, B. P., Weiss, L. E. & Lieber, C. M. Flexible electrical recording from cells using nanowire transistor arrays. Proc. Natl Acad. Sci. USA 106, 7309–7313 (2009).
Viventi, J. et al. A conformal, bio-interfaced class of silicon electronics for mapping cardiac electrophysiology. Sci. Transl. Med. 2, 24ra22 (2010).
Tian, B. Z. et al. Macroporous nanowire nanoelectronic scaffolds for synthetic tissues. Nature Mater. 11, 986–994 (2012).
Place, E. S., George, J. H., Williams, C. K. & Stevens, M. M. Synthetic polymer scaffolds for tissue engineering. Chem. Soc. Rev. 38, 1139–1151 (2009).
Zhang, D. et al. Tissue-engineered cardiac patch for advanced functional maturation of human ESC-derived cardiomyocytes. Biomaterials 34, 5813–5820 (2013).
Yelbuz, T. M., Choma, M. A., Thrane, L., Kirby, M. L. & Izatt, J. A. Optical coherence tomography – a new high-resolution imaging technology to study cardiac development in chick embryos. Circulation 106, 2771–2774 (2002).
Miragoli, M., Gaudesius, G. & Rohr, S. Electrotonic modulation of cardiac impulse conduction by myofibroblasts. Circ. Res. 98, 801–810 (2006).
Khademhosseini, A. et al. Microfluidic patterning for fabrication of contractile cardiac organoids. Biomed. Microdev. 9, 149–157 (2007).
Timko, B. P., Cohen-Karni, T., Qing, Q., Tian, B. & Lieber, C. M. Design and implementation of functional nanoelectronic interfaces with biomolecules, cells, and tissue using nanowire device arrays. IEEE Trans. Nanotechnol. 9, 269–280 (2010).
Zhang, J. H. et al. Functional cardiomyocytes derived from human induced pluripotent stem cells. Circ. Res. 104, e30 (2009).
Laflamme, M. A. et al. Cardiomyocytes derived from human embryonic stem cells in pro-survival factors enhance function of infarcted rat hearts. Nature Biotechnol. 25, 1015–1024 (2007).
Myles, R. C., Wang, L. G., Kang, C. Y., Bers, D. M. & Ripplinger, C. M. Local beta-adrenergic stimulation overcomes source-sink mismatch to generate focal arrhythmia. Circ. Res. 110, 1454–1464 (2012).
Iravanian, S. et al. Functional reentry in cultured monolayers of neonatal rat cardiac cells. Am. J. Physiol. Heart Circ. Physiol. 285, 449–456 (2003).
Liu, J. et al. Syringe-injectable electronics. Nature Nanotech. 10, 629–636 (2015).
Garbern, J. C. & Lee, R. T. Cardiac stem cell therapy and the promise of heart regeneration. Cell Stem Cell 12, 689–698 (2013).
Wobma, H. & Vunjak-Novakovic, G. Tissue engineering and regenerative medicine 2015: a year in review. Tissue Eng. Part B Rev. 22, 101–113 (2016).
Wong, A. D. et al. The blood-brain barrier: an engineering perspective. Front. Neuroeng. 6, 7 (2013).
Wang, X. Y. et al. Engineering interconnected 3D vascular networks in hydrogels using molded sodium alginate lattice as the sacrificial template. Lab Chip 14, 2709–2716 (2014).
McAlpine, M. C., Ahmad, H., Wang, D. W. & Heath, J. R. Highly ordered nanowire arrays on plastic substrates for ultrasensitive flexible chemical sensors. Nature Mater. 6, 379–384 (2007).
Annabi, N. et al. Hydrogel-coated microfluidic channels for cardiomyocyte culture. Lab Chip 13, 3569–3577 (2013).
Wang, C. et al. User-interactive electronic skin for instantaneous pressure visualization. Nature Mater. 12, 899–904 (2013).
Huang, Y., Duan, X. & Lieber, C. M. Nanowires for integrated multicolor nanophotonics. Small 1, 142–147 (2005).
Takei, K. et al. Nanowire active-matrix circuitry for low-voltage macroscale artificial skin. Nature Mater. 9, 821–826 (2010).
Acknowledgements
The authors thank R. Liao and D. Zhang for the inspiring discussion on cardiac electrophysiology and tissue engineering. The authors thank J. L. Huang for the assistance on instrumentation. This work was supported by National Institutes of Health Director's Pioneer and National Security Science and Engineering Faculty Fellow awards (to C.M.L.).
Author information
Authors and Affiliations
Contributions
X.D., W.Z. and C.M.L. conceived and designed the experiments. X.D., W.Z., T.G. and J.L. performed the experiments and analysed the data. X.D., W.Z. and C.M.L. co-wrote the paper. All authors discussed the results and commented on the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information
Supplementary information (PDF 3485 kb)
Supplementary Data
Supplementary Data (ZIP 10312 kb)
Rights and permissions
About this article
Cite this article
Dai, X., Zhou, W., Gao, T. et al. Three-dimensional mapping and regulation of action potential propagation in nanoelectronics-innervated tissues. Nature Nanotech 11, 776–782 (2016). https://doi.org/10.1038/nnano.2016.96
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nnano.2016.96