Abstract
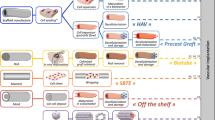
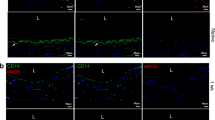
Arterial conduits are increasingly preferred for surgical bypass because of inherent functional properties conferred by arterial endothelial cells, especially nitric oxide production in response to physiologic stimuli. Here we tested whether endothelial progenitor cells (EPCs) can replace arterial endothelial cells and promote patency in tissue-engineered small-diameter blood vessels (4 mm). We isolated EPCs from peripheral blood of sheep, expanded them ex vivo and then seeded them on decellularized porcine iliac vessels. EPC-seeded grafts remained patent for 130 days as a carotid interposition graft in sheep, whereas non-seeded grafts occluded within 15 days. The EPC-explanted grafts exhibited contractile activity and nitric-oxide–mediated vascular relaxation that were similar to native carotid arteries. These results indicate that EPCs can function similarly to arterial endothelial cells and thereby confer longer vascular-graft survival. Due to their unique properties, EPCs might have other general applications for tissue-engineered structures and in treating vascular diseases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Tu, J.V. et al. Use of cardiac procedures and outcomes in elderly patients with myocardial infarction in the United States and Canada. N. Engl. J. Med. 336, 1500–1505 (1997).
Weinberg, C.B. & Bell, E. A blood vessel model constructed from collagen and cultured vascular cells. Science 213, 397–399 (1986).
L'Heureux, N., Paquet, S., Labbe, R., Germain, L. & Auger, F.A. A completely biological tissue-engineered human blood vessel. FASEB J. 12, 47–56 (1998).
Niklason, L.E. et al. Functional arteries grown in vitro. Science 284, 489–493 (1999).
T. Huynh et al. Remodeling of an acellular collagen graft into a physiologically responsive neovessel. Nature Biotechnol. 17, 1083–1086 (1999).
Schmidt, C.E. & Baier, J.E. Acellular vascular tissues: natural biomaterials for tissue repair and tissue engineering. Biomaterials 21, 2215–2231 (2000).
Sullivan, S.J. & Brockbank, K.G.M. in Principles of Tissue-Engineering. (eds. Langer, R. & Vacanti, J.) 447–454 (Academic Press, New York, 2000).
Davids, L., Dower, T. & Zilla, P. in Tissue Engineering of Prosthetic Vascular Grafts. (eds. Zilla, P. & Griesler, H.P.) 3–45 (R.G. Landes, Austin, Texas, 1999).
Asahara, T. et al. Isolation of putative progenitor endothelial cells for angiogenesis. Science 275, 964–967 (1997).
Yin, A. et al. AC133, a novel maker for human hematopoietic stem and progenitor cells. Blood 90, 5002–5012 (1997).
Shi, Q. et al. Evidence for circulating bone marrow-derived endothelial cells. Blood 92, 362–367 (1998).
Gehling, U.M. et al. In vitro differentiation of endothelial cells from AC133-positive progenitor cells. Blood 95, 3106–3112 (2000).
Lin, Y., Weisdorf, D.J., Solovey, A. & Hebbel, R.R. Origins of circulating endothelial cells and endothelial outgrowth from blood. J. Clin Invest. 105, 71–77 (2000).
Takahashi, T. et al. Ischemia- and cytokine-induced mobilization of bone marrow-derived endothelial progenitor cells for neovascularization. Nature Med. 5, 434–438 (1999).
Asahara, T. et al. Bone marrow origin of endothelial progenitor cells responsible for postnatal vasculogenesis in physiological and pathological neovascularization. Circul. Res. 85, 221–228 (1999).
Asahara, T. et al. VEGF contributes to postnatal neovascularization by mobilizing bone marrow-derived endothelial progenitor cells. EMBO J. 18, 3964–3972 (1999).
Kalka, C. et al. Transplantation of ex vivo expanded endothelial progenitor cells for therapeutic neovascularization. Proc. Natl. Acad. Sci. USA 97, 3422–3427 (2000).
Kalka, C. et al. Vascular endothelial growth factor165 gene transfer augments circulating endothelial progenitor cells in human subjects. Circul. Res. 86, 1198–1202 (2000).
Kalka, C. et al. VEGF gene transfer mobilizes endothelial progenitor cells in patients with inoperable coronary disease. Ann. Thorac. Surg. 70, 829–834 (2000).
Bhattacharya, V. et al. Enhanced endothelialization and microvessel formation in polyester grafts seeded with CD34+ bone marrow cells. Blood 95, 581–585 (2000).
Crosby, J.R. et al. Endothelial cells of hematopoietic origin make a significant contribution to adult blood vessel formation. Circul. Res. 87, 728–730 (2000).
Murohara, T. et al. Transplanted cord blood-derived endothelial precursor cells augment post-natal neovascularization. J. Clin. Invest. 105, 1527–1536 (2000).
Peichev, M. et al. Expression of VEGFR-2 and AC133 by circulating human CD34+ cells identifies a population of functional endothelial precursors. Blood 95, 952–958 (2000).
Ortenwall, P., Bylock, A., Kjellstrom, B.T. & Risberg, B. Seeding of ePTFE carotid interposition grafts in sheep and dogs: Species-dependent results. Surgery 103, 199–205 (1987).
Kraling, B.M. & Bischoff, J. A simplified method for growth of human microvascular endothelial cells results in decreased senescence and continued responsiveness to cytokines and growth factors. In Vitro Cell. Dev. Biol. 33, 308–315 (1998).
Rosenman, J.E., Kempczinski, R.F., Pearce, W.H. & Silberstein, E.B. Kinetics of endothelial cell seeding. J. Vasc. Surg. 2, 778–784 (1995).
Miyata, T. et al. Delayed exposure to pulsatile shear stress improves retention of human saphenous vein endothelial cells on seeded ePTFE grafts. J. Surg. Res. 50, 485–493 (1991).
Keaney Jr, J.F. & Vita, J.A. Atherosclerosis, oxidative stress, and antioxidant protection in endothelium-derived relaxing factor action. Prog. Cardiovasc. Dis. 38, 129–154 (1995).
Quyyumi, A.A. et al. Nitric oxide activity in the human coronary circulation. Impact of risk factors for coronary atherosclerosis. J. Clin. Invest. 95, 1747–1755 (1995).
Azuma, H., Ishikawa, M. & Sekizaki, S. Endothelium-dependent inhibition of platelet aggregation. Br. J. Pharmacol. 88, 411–415 (1986).
Radomski, M.W., Palmer, R.M. & Moncada, S. The role of nitric oxide and cGMP in platelet adhesion to vascular endothelium. Biochem. Biophys. Res. Commun. 148, 1482–1489 (1987).
Kubes, P., Kurose, I. & Granger, D.N. NO donors prevent integrin-induced leukocyte adhesion but not P-selectin-dependent rolling in postischemic venules. Am. J. Physiol. 267, H931–937 (1994).
Marks, D.S. et al. Inhibition of neointimal proliferation in rabbits after vascular injury by a single treatment with a protein adduct of nitric oxide. J. Clin. Invest. 96, 2630–2638 (1995).
Luscher, T.F. et al. Difference between endothelium-dependent relaxation in arterial and in venous coronary bypass grafts. N. Engl. J. Med. 319, 462–467 (1988).
Pearson, P.J., Evora, P.R.B. & Schaff, H.V. Bioassay of EDRF from internal mammary arteries: Implications for early and late bypass graft patency. J. Thorac. Surg. 54, 1078–1084 (1992).
Shapira, O.M. et al. Enhanced nitric oxide-mediated vascular relaxation in radial artery compared with internal mammary artery or saphenous vein. Circulation 100, 322–326 (1999).
Shimizu, K. et al. Host bone marrow cells are a source of donor intimal smooth muscle-like cells in the murine aortic transplant arteriopathy. Nature Med. 7, 738–741 (2001).
Deutsch, M., Meinhart, J. & Zilla, P. in Tissue Engineering of Prosthetic Vascular Grafts (eds. Zilla, P. & Griesler, H.P.) 180–187 (R.G. Landes, Austin, Texas, 1999).
Shen, B. et al. Homologous up-regulation of KDR/Flk-1 receptor expression by vascular endothelial growth factor in vitro. J. Biol. Chem. 273, 29979–29985 (1998).
Shen, B.-Q. et al. Hepatocyte growth factor stimulates the differentiation of human tracheal epithelia in vitro. Am. J. Phys. 272, L1115–1120 (1997).
Dardik, A., Liu, A. & Ballermann, B.J. Chronic in vivo shear stress stimulates endothelial cell retention on prosthetic vascular grafts and reduces subsequent in vivo neointimal thickness. J. Vasc. Biol. 29, 157–167 (1999).
Acknowledgements
We thank D. Zvagelsky for technical assistance with preparing tissue sections; E. Rhee for providing the arteriograms; Sulzer Carbomedics for providing the vessel bioreactor; K. Gullage and J. Fox for preparation of the figures; and J. Folkman, C. Lowenstein, S. Roth and J. Schneider for critically reading the manuscript. This work was supported by RO1 HL 60490 (J.B.) and RO1 HL 60463 (J.E.M. Jr) from the National Heart, Lung and Blood Institute and the Sarnoff Foundation (S.K.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaushal, S., Amiel, G., Guleserian, K. et al. Functional small-diameter neovessels created using endothelial progenitor cells expanded ex vivo. Nat Med 7, 1035–1040 (2001). https://doi.org/10.1038/nm0901-1035
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/nm0901-1035
This article is cited by
-
Challenges and advances in materials and fabrication technologies of small-diameter vascular grafts
Biomaterials Research (2023)
-
Decellularized Human Umbilical Artery Exhibits Adequate Endothelialization in Xenogenic Transplantation
Biotechnology and Bioprocess Engineering (2023)
-
Cyclic pressure induced decellularization of porcine descending aortas
Journal of Materials Science: Materials in Medicine (2023)
-
A Comparative Study of an Anti-Thrombotic Small-Diameter Vascular Graft with Commercially Available e-PTFE Graft in a Porcine Carotid Model
Tissue Engineering and Regenerative Medicine (2022)
-
Mechano-regulated cell–cell signaling in the context of cardiovascular tissue engineering
Biomechanics and Modeling in Mechanobiology (2022)