Abstract
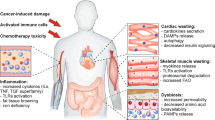
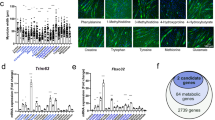
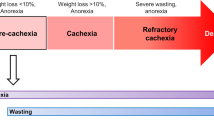
Cachexia is a devastating muscle-wasting syndrome that occurs in patients who have chronic diseases. It is most commonly observed in individuals with advanced cancer1,2, presenting in 80% of these patients, and it is one of the primary causes of morbidity and mortality associated with cancer3,4,5. Additionally, although many people with cachexia show hypermetabolism3,6, the causative role of metabolism in muscle atrophy has been unclear. To understand the molecular basis of cachexia-associated muscle atrophy, it is necessary to develop accurate models of the condition. By using transcriptomics and cytokine profiling of human muscle stem cell–based models and human cancer-induced cachexia models in mice, we found that cachectic cancer cells secreted many inflammatory factors that rapidly led to high levels of fatty acid metabolism and to the activation of a p38 stress-response signature in skeletal muscles, before manifestation of cachectic muscle atrophy occurred. Metabolomics profiling revealed that factors secreted by cachectic cancer cells rapidly induce excessive fatty acid oxidation in human myotubes, which leads to oxidative stress, p38 activation and impaired muscle growth. Pharmacological blockade of fatty acid oxidation not only rescued human myotubes, but also improved muscle mass and body weight in cancer cachexia models in vivo. Therefore, fatty acid–induced oxidative stress could be targeted to prevent cancer-induced cachexia.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Tisdale, M.J. Cachexia in cancer patients. Nat. Rev. Cancer 2, 862–871 (2002).
von Haehling, S. & Anker, S.D. Cachexia as a major underestimated and unmet medical need: facts and numbers. J. Cachexia Sarcopenia Muscle 1, 1–5 (2010).
Fearon, K.C., Glass, D.J. & Guttridge, D.C. Cancer cachexia: mediators, signaling, and metabolic pathways. Cell Metab. 16, 153–166 (2012).
Fearon, K., Arends, J. & Baracos, V. Understanding the mechanisms and treatment options in cancer cachexia. Nat. Rev. Clin. Oncol. 10, 90–99 (2013).
Cohen, S., Nathan, J.A. & Goldberg, A.L. Muscle wasting in disease: molecular mechanisms and promising therapies. Nat. Rev. Drug Discov. 14, 58–74 (2015).
Zuijdgeest-van Leeuwen, S.D. et al. Lipolysis and lipid oxidation in weight-losing cancer patients and healthy subjects. Metabolism 49, 931–936 (2000).
Guttridge, D.C., Mayo, M.W., Madrid, L.V., Wang, C.Y. & Baldwin, A.S. Jr. NF-κB-induced loss of MyoD messenger RNA: possible role in muscle decay and cachexia. Science 289, 2363–2366 (2000).
McFarlane, C. et al. Myostatin induces cachexia by activating the ubiquitin proteolytic system through an NF-κB-independent, FoxO1-dependent mechanism. J. Cell. Physiol. 209, 501–514 (2006).
Mori, M. et al. Cancer cachexia syndrome developed in nude mice bearing melanoma cells producing leukemia-inhibitory factor. Cancer Res. 51, 6656–6659 (1991).
Bouhadir, K.H. et al. Degradation of partially oxidized alginate and its potential application for tissue engineering. Biotechnol. Prog. 17, 945–950 (2001).
Silva, E.A., Kim, E.S., Kong, H.J. & Mooney, D.J. Material-based deployment enhances efficacy of endothelial progenitor cells. Proc. Natl. Acad. Sci. USA 105, 14347–14352 (2008).
Bernet, J.D. et al. p38 MAPK signaling underlies a cell-autonomous loss of stem cell self-renewal in skeletal muscle of aged mice. Nat. Med. 20, 265–271 (2014).
Cosgrove, B.D. et al. Rejuvenation of the muscle stem cell population restores strength to injured aged muscles. Nat. Med. 20, 255–264 (2014).
Das, S.K. et al. Adipose triglyceride lipase contributes to cancer-associated cachexia. Science 333, 233–238 (2011).
Kawakami, M. et al. Human recombinant TNF suppresses lipoprotein lipase activity and stimulates lipolysis in 3T3-L1 cells. J. Biochem. 101, 331–338 (1987).
Feingold, K.R., Doerrler, W., Dinarello, C.A., Fiers, W. & Grunfeld, C. Stimulation of lipolysis in cultured fat cells by tumor necrosis factor, interleukin-1, and the interferons is blocked by inhibition of prostaglandin synthesis. Endocrinology 130, 10–16 (1992).
Green, A., Dobias, S.B., Walters, D.J. & Brasier, A.R. Tumor necrosis factor increases the rate of lipolysis in primary cultures of adipocytes without altering levels of hormone-sensitive lipase. Endocrinology 134, 2581–2588 (1994).
van Hall, G. et al. Interleukin-6 stimulates lipolysis and fat oxidation in humans. J. Clin. Endocrinol. Metab. 88, 3005–3010 (2003).
Argilés, J.M., Busquets, S., Toledo, M. & López-Soriano, F.J. The role of cytokines in cancer cachexia. Curr. Opin. Support. Palliat. Care 3, 263–268 (2009).
Ebadi, M., Baracos, V.E., Bathe, O.F., Robinson, L.E. & Mazurak, V.C. Loss of visceral adipose tissue precedes subcutaneous adipose tissue and associates with n-6 fatty acid content. Clin. Nutr. S0261-5614(16)00071-6 (2016).
Son, Y., Kim, S., Chung, H.T. & Pae, H.O. Reactive oxygen species in the activation of MAP kinases. Methods Enzymol. 528, 27–48 (2013).
Mastrocola, R. et al. Muscle wasting in diabetic and in tumor-bearing rats: role of oxidative stress. Free Radic. Biol. Med. 44, 584–593 (2008).
Waning, D.L. et al. Excess TGF-β mediates muscle weakness associated with bone metastases in mice. Nat. Med. 21, 1262–1271 (2015).
Gao, S. & Carson, J.A. Lewis lung carcinoma regulation of mechanical stretch-induced protein synthesis in cultured myotubes. Am. J. Physiol. Cell Physiol. 310, C66–C79 (2016).
Trendelenburg, A.U., Meyer, A., Jacobi, C., Feige, J.N. & Glass, D.J. TAK-1/p38/nNFκB signaling inhibits myoblast differentiation by increasing levels of Activin A. Skelet. Muscle 2, 3 (2012).
Min-Wen, J.C., Jun-Hao, E.T. & Shyh-Chang, N. Stem cell mitochondria during aging. Semin. Cell Dev. Biol. 52, 110–118 (2016).
Woods, M.N. et al. Effect of a dietary intervention and n-3 fatty acid supplementation on measures of serum lipid and insulin sensitivity in persons with HIV. Am. J. Clin. Nutr. 90, 1566–1578 (2009).
Horowitz, J.D., Chirkov, Y.Y., Kennedy, J.A. & Sverdlov, A.L. Modulation of myocardial metabolism: an emerging therapeutic principle. Curr. Opin. Cardiol. 25, 329–334 (2010).
Lopatin, Y.M. et al. Rationale and benefits of trimetazidine by acting on cardiac metabolism in heart failure. Int. J. Cardiol. 203, 909–915 (2016).
Skuk, D. et al. Intramuscular transplantation of human postnatal myoblasts generates functional donor-derived satellite cells. Mol. Ther. 18, 1689–1697 (2010).
Khaw, S.L., Min-Wen, C., Koh, C.G., Lim, B. & Shyh-Chang, N. Oocyte factors suppress mitochondrial polynucleotide phosphorylase to remodel the metabolome and enhance reprogramming. Cell Rep. 12, 1080–1088 (2015).
Selvarasu, S. et al. Combined in silico modeling and metabolomics analysis to characterize fed-batch CHO cell culture. Biotechnol. Bioeng. 109, 1415–1429 (2012).
Tan, A.H.M. et al. Aberrant presentation of self-lipids by autoimmune B cells depletes peripheral iNKT cells. Cell Rep. 9, 24–31 (2014).
Acknowledgements
We thank all our respective lab mates for their helpful discussion, and E. Peh for technical assistance with mass spectrometry. This work was supported by the Agency for Science Technology and Research (ASTAR) Joint Council Office grant 1431AFG128 (N.S.-C.), the Singapore National Medical Research Council grants NMRC/STaR/0024/2014 and NMRC/GMS/CIRG/1332/2012, Duke-NUS Medical School, and National Cancer Centre Singapore (all to B.T.T.), Polaris program grant SPF2012/001 under the ASTAR Strategic Positioning Fund (Y.S.H.) and the Genome Institute of Singapore (I.B.T. and N.S.-C.).
Author information
Authors and Affiliations
Contributions
T.F., I.B.T., B.T.T. and N.S.-C. designed the study. T.F., B.C.Y.-J., J.C.M.-W., D.H., C.-N.Q., P.O., Z.L. and H.K. performed experiments in vivo. T.F., B.C.Y.-J., J.C.M.-W., E.T.J.-H., D.H. and P.O. performed experiments in vitro. W.J.L., J.H.L., C.C., H.S.O., K.-K.T. and I.B.T. provided the clinical samples. S.C., S.Y.M. and Y.S.H. performed mass-spectrometry experiments. R.E.M. and R.R.W. performed quantitative phase imaging. T.F., I.B.T., B.T.T. and N.S.-C. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–8 and Supplementary Tables 1–4 (PDF 7313 kb)
Rights and permissions
About this article
Cite this article
Fukawa, T., Yan-Jiang, B., Min-Wen, J. et al. Excessive fatty acid oxidation induces muscle atrophy in cancer cachexia. Nat Med 22, 666–671 (2016). https://doi.org/10.1038/nm.4093
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4093
This article is cited by
-
Cytokine release syndrome was an independent risk factor associated with hypoalbuminemia for patients with relapsed/refractory hematological malignancies after CAR-T cell therapy
BMC Cancer (2023)
-
Interleukin-17 as a key player in neuroimmunometabolism
Nature Metabolism (2023)
-
The interplay of immunology and cachexia in infection and cancer
Nature Reviews Immunology (2022)
-
An integrative transcriptome study reveals Ddit4/Redd1 as a key regulator of cancer cachexia in rodent models
Cell Death & Disease (2021)
-
Diversity and versatility of p38 kinase signalling in health and disease
Nature Reviews Molecular Cell Biology (2021)