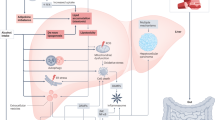
Abstract
Nonalcoholic fatty liver disease (NAFLD) is the most common liver disease in Western countries. It encompasses a wide spectrum of liver lesions, from pure steatosis to end-stage liver disease with cirrhosis and hepatocellular carcinoma. Nonalcoholic steatohepatitis corresponds only to one stage of NAFLD. As NAFLD can be considered a liver manifestation of the metabolic syndrome, its prevalence is high in obese people and in patients who have type 2 diabetes—insulin resistance is one of the key elements of the pathogenesis of NAFLD. This disease is often asymptomatic in the absence of decompensated cirrhosis, but should be suspected in patients with elevated aminotransferase levels or radiological evidence of a fatty liver or hepatomegaly. Liver fibrosis is associated with age over 50 years, obesity, diabetes and high triglyceride levels. Liver biopsy is the only way to assess the histologic features of necrotic inflammation and fibrosis that define nonalcoholic steatohepatitis and to determine its probable prognosis. The prognosis is good for pure steatosis, whereas the presence of necrotic inflammation is associated with a significant risk of progression to cirrhosis and, possibly, hepatocellular carcinoma. Lifestyle changes, such as dietary modifications and exercise, are recommended. To date, there have been very few randomized, placebo-controlled trials of drug treatments for NAFLD.
Key Points
-
Nonalcoholic fatty liver disease (NAFLD) is the leading cause of liver disease in Western countries
-
NAFLD can be considered as a liver manifestation of the metabolic syndrome
-
Clinical symptoms are nonspecific and are frequently absent in patients without cirrhosis
-
Liver biopsy remains the gold standard for evaluation of prognosis
-
NAFLD can progress to cirrhosis and hepatocellular carcinoma
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Ludwig J et al. (1980) Nonalcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease. Mayo Clin Proc 55: 434–438
Angulo P (2002) Nonalcoholic fatty liver disease. N Engl J Med 346: 1221–1231
Younossi ZM et al. (2002) Nonalcoholic fatty liver disease: an agenda for clinical research. Hepatology 35: 746–752
Clark JM et al. (2002) Nonalcoholic fatty liver disease. Gastroenterology 122: 1649–1657
Bellentani S et al. (1994) Prevalence of chronic liver disease in the general population of northern Italy: the Dionysos Study. Hepatology 20: 1442–1449
Bedogni G et al. (2005) Prevalence of and risk factors for nonalcoholic fatty liver disease: the Dionysos nutrition and liver study. Hepatology 42: 44–52
Poonawala A et al. (2000) Prevalence of obesity and diabetes in patients with cryptogenic cirrhosis: a case–control study. Hepatology 32: 689–692
Caldwell SH et al. (1999) Cryptogenic cirrhosis: clinical characterization and risk factors for underlying disease. Hepatology 29: 664–669
International Diabetes Federation: the IDF consensus worldwide definition of the metabolic syndrome [http://www.idf.org/webdata/docs/Metabolic_syndrome_definition.pdf] (accessed 29 March 2007)
Dixon JB et al. (2001) Nonalcoholic fatty liver disease: predictors of nonalcoholic steatohepatitis and liver fibrosis in the severely obese. Gastroenterology 121: 91–100
Knobler H et al. (1999) Fatty liver—an additional and treatable feature of the insulin resistance syndrome. QJM 92: 73–79
Hamaguchi M et al. (2005) The metabolic syndrome as a predictor of nonalcoholic fatty liver disease. Ann Intern Med 143: 722–728
McCullough AJ (2005) The epidemiology and risk factors of NASH. In Fatty Liver Disease. NASH and Related Disorders, 23–37 (Eds Farrell G et al.) Malden: Blackwell Publishing
Begriche K et al. (2006) Mitochondrial dysfunction in NASH: causes, consequences and possible means to prevent it. Mitochondrion 6: 1–28
Schaffler A et al. (2005) Mechanisms of disease: adipocytokines and visceral adipose tissue—emerging role in nonalcoholic fatty liver disease. Nat Clin Pract Gastroenterol Hepatol 2: 273–280
Tilg H and Hotamisligil GS (2006) Nonalcoholic fatty liver disease: cytokine–adipokine interplay and regulation of insulin resistance. Gastroenterology 131: 934–945
Bugianesi E et al. (2005) Plasma adiponectin in nonalcoholic fatty liver is related to hepatic insulin resistance and hepatic fat content, not to liver disease severity. J Clin Endocrinol Metab 90: 3498–3504
Xu A et al. (2003) The fat-derived hormone adiponectin alleviates alcoholic and nonalcoholic fatty liver diseases in mice. J Clin Invest 112: 91–100
Kadowaki T et al. (2006) Adiponectin and adiponectin receptors in insulin resistance, diabetes, and the metabolic syndrome. J Clin Invest 116: 1784–1792
Faggioni R et al. (2000) Leptin-deficient (ob/ob) mice are protected from T cell-mediated hepatotoxicity: role of tumor necrosis factor α and IL-18. Proc Natl Acad Sci USA 97: 2367–2372
Fantuzzi G and Faggioni R (2000) Leptin in the regulation of immunity, inflammation, and hematopoiesis. J Leukoc Biol 68: 437–446
Marra F (2002) Leptin and liver fibrosis: a matter of fat. Gastroenterology 122: 1529–1532
Montez JM et al. (2005) Acute leptin deficiency, leptin resistance, and the physiologic response to leptin withdrawal. Proc Natl Acad Sci USA 102: 2537–2542
Lehrke M et al. (2004) An inflammatory cascade leading to hyperresistinemia in humans. PLoS Med 1: e45
Pagano C et al. (2006) Increased serum resistin in nonalcoholic fatty liver disease is related to liver disease severity and not to insulin resistance. J Clin Endocrinol Metab 91: 1081–1086
Fukuhara A et al. (2005) Visfatin: a protein secreted by visceral fat that mimics the effects of insulin. Science 307: 426–430
Hida K et al. (2005) Visceral adipose tissue-derived serine protease inhibitor: a unique insulin-sensitizing adipocytokine in obesity. Proc Natl Acad Sci USA 102: 10610–10615
Ailhaud G (2006) Adipose tissue as a secretory organ: from adipogenesis to the metabolic syndrome. C R Biol 329: 570–577
Fantuzzi G (2005) Adipose tissue, adipokines, and inflammation. J Allergy Clin Immunol 115: 911–919
Hotamisligil GS et al. (1994) Tumor necrosis factor α inhibits signaling from the insulin receptor. Proc Natl Acad Sci USA 91: 4854–4858
Ofei F et al. (1996) Effects of an engineered human anti-TNF-α antibody (CDP571) on insulin sensitivity and glycemic control in patients with NIDDM. Diabetes 45: 881–885
Kanda H et al. (2006) MCP-1 contributes to macrophage infiltration into adipose tissue, insulin resistance, and hepatic steatosis in obesity. J Clin Invest 116: 1494–1505
Perez-Carreras M et al. (2003) Defective hepatic mitochondrial respiratory chain in patients with nonalcoholic steatohepatitis. Hepatology 38: 999–1007
Browning JD and Horton JD (2004) Molecular mediators of hepatic steatosis and liver injury. J Clin Invest 114: 147–152
Esterbauer H et al. (1991) Chemistry and biochemistry of 4-hydroxynonenal, malonaldehyde and related aldehydes. Free Radic Biol Med 11: 81–128
Bissell DM et al. (2001) Transforming growth factor β and the liver. Hepatology 34: 859–867
Li Z et al. (2004) Norepinephrine regulates hepatic innate immune system in leptin-deficient mice with nonalcoholic steatohepatitis. Hepatology 40: 434–441
Brun P et al. (2007) Increased intestinal permeability in obese mice: new evidences in the pathogenesis of nonalcoholic steatohepatitis. Am J Physiol Gastrointest Liver Physiol 292: G518–G525
Cope K et al. (2000) Increased gastrointestinal ethanol production in obese mice: implications for fatty liver disease pathogenesis. Gastroenterology 119: 1340–1347
Diehl AM et al. (1988) Alcohollike liver disease in nonalcoholics. A clinical and histologic comparison with alcohol-induced liver injury. Gastroenterology 95: 1056–1062
Angulo P et al. (1999) Independent predictors of liver fibrosis in patients with nonalcoholic steatohepatitis. Hepatology 30: 1356–1362
Mofrad P et al. (2003) Clinical and histologic spectrum of nonalcoholic fatty liver disease associated with normal ALT values. Hepatology 37: 1286–1292
Bonkovsky HL et al. (1999) Non-alcoholic steatohepatitis and iron: increased prevalence of mutations of the HFE gene in non-alcoholic steatohepatitis. J Hepatol 31: 421–429
Chitturi S et al. (2002) HFE mutations, hepatic iron, and fibrosis: ethnic-specific association of NASH with C282Y but not with fibrotic severity. Hepatology 36: 142–149
Saadeh S et al. (2002) The utility of radiological imaging in nonalcoholic fatty liver disease. Gastroenterology 123: 745–750
Fishbein M et al. (2005) Hepatic MRI for fat quantitation: its relationship to fat morphology, diagnosis, and ultrasound. J Clin Gastroenterol 39: 619–625
Szczepaniak LS et al. (2005) Magnetic resonance spectroscopy to measure hepatic triglyceride content: prevalence of hepatic steatosis in the general population. Am J Physiol Endocrinol Metab 288: E462–E468
Kleiner DE et al. (2005) Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 41: 1313–1321
Brunt EM (2004) Nonalcoholic steatohepatitis. Semin Liver Dis 24: 3–20
Bugianesi E et al. (2002) Expanding the natural history of nonalcoholic steatohepatitis: from cryptogenic cirrhosis to hepatocellular carcinoma. Gastroenterology 123: 134–140
Younossi ZM et al. (2004) Nonalcoholic fatty liver disease in patients with type 2 diabetes. Clin Gastroenterol Hepatol 2: 262–265
Ratziu V et al. (2000) Liver fibrosis in overweight patients. Gastroenterology 118: 1117–1123
Ratziu V et al. (2006) Diagnostic value of biochemical markers (FibroTest–FibroSURE) for the prediction of liver fibrosis in patients with non-alcoholic fatty liver disease. BMC Gastroenterol 6: 6
Kelleher TB and Afdhal N (2005) Noninvasive assessment of liver fibrosis. Clin Liver Dis 9: 667–683
Foucher J et al. (2006) Prevalence and factors associated with failure of liver stiffness measurement using FibroScan in a prospective study of 2,114 examinations. Eur J Gastroenterol Hepatol 18: 411–412
Adams LA et al. (2005) The natural history of nonalcoholic fatty liver disease: a population-based cohort study. Gastroenterology 129: 113–121
Dam-Larsen S et al. (2004) Long term prognosis of fatty liver: risk of chronic liver disease and death. Gut 53: 750–755
Day CP (2005) Natural history of NAFLD: remarkably benign in the absence of cirrhosis. Gastroenterology 129: 375–378
Fassio E et al. (2004) Natural history of nonalcoholic steatohepatitis: a longitudinal study of repeat liver biopsies. Hepatology 40: 820–826
Matteoni CA et al. (1999) Nonalcoholic fatty liver disease: a spectrum of clinical and pathological severity. Gastroenterology 116: 1413–1419
Hui JM et al. (2003) Long-term outcomes of cirrhosis in nonalcoholic steatohepatitis compared with hepatitis C. Hepatology 38: 420–427
Ratziu V et al. (2002) Survival, liver failure, and hepatocellular carcinoma in obesity-related cryptogenic cirrhosis. Hepatology 35: 1485–1493
Perlemuter G et al. (2002) Hepatitis C virus core protein inhibits microsomal triglyceride transfer protein activity and very low density lipoprotein secretion: a model of viral-related steatosis. FASEB J 16: 185–194
Hourigan LF et al. (1999) Fibrosis in chronic hepatitis C correlates significantly with body mass index and steatosis. Hepatology 29: 1215–1219
Clouston AD et al. (2001) Steatosis and chronic hepatitis C: analysis of fibrosis and stellate cell activation. J Hepatol 34: 314–320
Naveau S et al. (1997) Excess weight risk factor for alcoholic liver disease. Hepatology 25: 108–111
Raynard B et al. (2002) Risk factors of fibrosis in alcohol-induced liver disease. Hepatology 35: 635–638
Palmer M and Schaffner F (1990) Effect of weight reduction on hepatic abnormalities in overweight patients. Gastroenterology 99: 1408–1413
Padwal R et al. (2003) Long-term pharmacotherapy for overweight and obesity: a systematic review and meta-analysis of randomized controlled trials. Int J Obes Relat Metab Disord 27: 1437–1446
Mathurin P et al. (2006) The evolution of severe steatosis after bariatric surgery is related to insulin resistance. Gastroenterology 130: 1617–1624
Uygun A et al. (2004) Metformin in the treatment of patients with non-alcoholic steatohepatitis. Aliment Pharmacol Ther 19: 537–544
Bugianesi E et al. (2005) A randomized controlled trial of metformin versus vitamin E or prescriptive diet in nonalcoholic fatty liver disease. Am J Gastroenterol 100: 1082–1090
Galli A et al. (2002) Antidiabetic thiazolidinediones inhibit collagen synthesis and hepatic stellate cell activation in vivo and in vitro. Gastroenterology 122: 1924–1940
Caldwell SH et al. (2001) A pilot study of a thiazolidinedione, troglitazone, in nonalcoholic steatohepatitis. Am J Gastroenterol 96: 519–525
Neuschwander-Tetri BA et al. (2003) Improved nonalcoholic steatohepatitis after 48 weeks of treatment with the PPAR-γ ligand rosiglitazone. Interim results of a pilot study demonstrating the early effects of the PPAR-γ ligand rosiglitazone on insulin sensitivity, aminotransferases, hepatic steatosis and body weight in patients with non-alcoholic steatohepatitis. Hepatology 38: 1008–1017
Promrat K et al. (2004) A pilot study of pioglitazone treatment for nonalcoholic steatohepatitis. Hepatology 39: 188–196
Belfort R et al. (2006) A placebo-controlled trial of pioglitazone in subjects with nonalcoholic steatohepatitis. N Engl J Med 355: 2297–2307
Lindor KD et al. (2004) Ursodeoxycholic acid for treatment of nonalcoholic steatohepatitis: results of a randomized trial. Hepatology 39: 770–778
Lavine JE (2000) Vitamin E treatment of nonalcoholic steatohepatitis in children: a pilot study. J Pediatr 136: 734–738
Harrison SA et al. (2003) Vitamin E and vitamin C treatment improves fibrosis in patients with nonalcoholic steatohepatitis. Am J Gastroenterol 98: 2485–2490
Sanyal AJ et al. (2004) A pilot study of vitamin E versus vitamin E and pioglitazone for the treatment of nonalcoholic steatohepatitis. Clin Gastroenterol Hepatol 2: 1107–1115
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Perlemuter, G., Bigorgne, A., Cassard-Doulcier, AM. et al. Nonalcoholic fatty liver disease: from pathogenesis to patient care. Nat Rev Endocrinol 3, 458–469 (2007). https://doi.org/10.1038/ncpendmet0505
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpendmet0505
This article is cited by
-
Role of exercise in the mechanisms ameliorating hepatic steatosis in non-alcoholic fatty liver disease
Sport Sciences for Health (2018)
-
“Non alcoholic fatty liver disease and eNOS dysfunction in humans”
BMC Gastroenterology (2017)
-
Characterisation of Agomelatine-Induced Increase in Liver Enzymes: Frequency and Risk Factors Determined from a Pooled Analysis of 7605 Treated Patients
CNS Drugs (2016)
-
Chlorogenic Acid Improves High Fat Diet-Induced Hepatic Steatosis and Insulin Resistance in Mice
Pharmaceutical Research (2015)
-
Synthetic FXR Agonist GW4064 Prevents Diet-Induced Hepatic Steatosis and Insulin Resistance
Pharmaceutical Research (2013)