Abstract
A central goal of regenerative medicine is to generate transplantable organs from cells derived or expanded in vitro. Although numerous studies have demonstrated the production of defined cell types in vitro1, the creation of a fully intact organ has not been reported. The transcription factor forkhead box N1 (FOXN1) is critically required for development of thymic epithelial cells2,3 (TECs), a key cell type of the thymic stroma4. Here, we show that enforced Foxn1 expression is sufficient to reprogramme fibroblasts into functional TECs, an unrelated cell type across a germ-layer boundary. These FOXN1-induced TECs (iTECs) supported efficient development of both CD4+ and CD8+ T cells in vitro. On transplantation, iTECs established a complete, fully organized and functional thymus, that contained all of the TEC subtypes required to support T-cell differentiation and populated the recipient immune system with T cells. iTECs thus demonstrate that cellular reprogramming approaches can be used to generate an entire organ, and open the possibility of widespread use of thymus transplantation to boost immune function in patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Graf, T. & Enver, T. Forcing cells to change lineages. Nature 462, 587–594 (2009).
Nehls, M. et al. Two genetically separable steps in the differentiation of thymic epithelium. Science 272, 886–889 (1996).
Blackburn, C. C. et al. The nu gene acts cell-autonomously and is required for differentiation of thymic epithelial progenitors. Proc. Natl Acad. Sci. USA 93, 5742–5746 (1996).
Ritter, M. A. & Boyd, R. L. Development in the thymus: It takes two to tango. Immunol. Today 14, 462–469 (1993).
Miller, J. F. A. P. Immunological function of the thymus. Lancet 2, 748–749 (1961).
Chinn, I. K., Blackburn, C. C., Manley, N. R. & Sempowski, G. D. Changes in primary lymphoid organs with aging. Semin. Immunol. 24, 309–320 (2012).
Lynch, H. E. et al. Thymic involution and immune reconstitution. Trends Immunol. 30, 366–373 (2009).
Manley, N. R., Richie, E. R., Blackburn, C. C., Condie, B. G. & Sage, J. Structure and function of the thymic microenvironment. Front. Biosci. 16, 2461–2477 (2011).
Nowell, C. S. et al. Foxn1 regulates lineage progression in cortical and medullary thymic epithelial cells but is dispensable for medullary sublineage divergence. PLoS Genet. 7, e1002348 (2011).
Bleul, C. C. et al. Formation of a functional thymus initiated by a postnatal epithelial progenitor cell. Nature 441, 992–996 (2006).
Markert, M. L. et al. Transplantation of thymus tissue in complete DiGeorge Syndrome. N. Engl. J. Med. 341, 1180–1189 (1999).
Lai, L. & Jin, J. Generation of thymic epithelial cell progenitors by mouse embryonic stem cells. Stem Cells 27, 3012–3020 (2009).
Lai, L. et al. Mouse embryonic stem cell-derived thymic epithelial cell progenitors enhance T-cell reconstitution after allogeneic bone marrow transplantation. Blood 118, 3410–3418 (2011).
Inami, Y. et al. Differentiation of induced pluripotent stem cells to thymic epithelial cells by phenotype. Immunol. Cell Biol. 89, 314–321 (2011).
Parent, A. V. et al. Generation of functional thymic epithelium from human embryonic stem cells that supports host T cell development. Cell Stem Cell 13, 219–229 (2013).
Sun, X. et al. Directed differentiation of human embryonic stem cells into thymic epithelial progenitor-like cells reconstitutes the thymic microenvironment in vivo. Cell Stem Cell 13, 230–236 (2013).
Mathis, D. & Benoist, C. Aire. Annu. Rev. Immunol. 27, 287–312 (2009).
Klug, D. B. et al. Interdependence of cortical thymic epithelial cell differentiation and T-lineage commitment. Proc. Natl Acad. Sci. USA 95, 11822–11827 (1998).
Manley, N. R. & Condie, B. G. Transcriptional regulation of thymus organogenesis and thymic epithelial cell differentiation. Prog. Mol. Biol. Transl. Sci. 92, 103–120 (2010).
Weiner, L. et al. Dedicated epithelial recipient cells determine pigmentation patterns. Cell 130, 932–942 (2007).
Allman, D. et al. Thymopoiesis independent of common lymphoid progenitors. Nat. Immunol. 4, 168–174 (2003).
Klug, D. B., Carter, C., Gimenez-Conti, I. B. & Richie, E. R. Cutting edge: thymocyte-independent and thymocyte-dependent phases of epithelial patterning in the fetal thymus. J. Immunol. 169, 2842–2845 (2002).
Revest, J. M., Suniara, R. K., Kerr, K., Owen, J. J. & Dickson, C. Development of the thymus requires signaling through the fibroblast growth factor receptor R2-IIIb. J. Immunol. 167, 1954–1961 (2001).
Rubin, J. S. et al. Purification and characterization of a newly identified growth factor specific for epithelial cells. Proc. Natl Acad. Sci. USA 86, 802–806 (1989).
Adolfsson, J. et al. Identification of Flt3+ lympho-myeloid stem cells lacking erythro-megakaryocytic potential. A revised road map for adult blood lineage commitment. Cell 121, 295–306 (2005).
Luc, S. et al. The earliest thymic T cell progenitors sustain B cell and myeloid lineage potential. Nat. Immunol. 13, 412–419 (2012).
Schmitt, T. M. et al. Induction of T cell development and establishment of T cell competence from embryonic stem cells differentiated in vitro. Nat. Immunol. 5, 410–417 (2004).
La Motte-Mohs, R. N., Herer, E. & Zuniga-Pflucker, J. C. Induction of T-cell development from human cord blood hematopoietic stem cells by Delta-like 1 in vitro. Blood 105, 1431–1439 (2005).
Bennett, A. R. et al. Identification and characterization of thymic epithelial progenitor cells. Immunity 16, 803–814 (2002).
Sheridan, J. M., Taoudi, S., Medvinsky, A. & Blackburn, C. C. A novel method for the generation of reaggregated organotypic cultures that permits juxtaposition of defined cell populations. Genesis 47, 346–351 (2009).
Auerbach, R. Morphogenetic interactions in the development of the mouse thymus gland. Dev. Biol. 2, 271–284 (1960).
Jenkinson, W. E., Rossi, S. W., Parnell, S. M., Jenkinson, E. J. & Anderson, G. PDGFRα-expressing mesenchyme regulates thymus growth and the availability of intrathymic niches. Blood 109, 954–960 (2007).
Abramson, J., Giraud, M., Benoist, C. & Mathis, D. Aire’s partners in the molecular control of immunological tolerance. Cell 140, 123–135 (2010).
Shakib, S. et al. Checkpoints in the development of thymic cortical epithelial cells. J. Immunol. 182, 130–137 (2009).
Murata, S. et al. Regulation of CD8+ T cell development by thymus-specific proteasomes. Science 316, 1349–1353 (2007).
Schmitt, T. M. & Zuniga-Pflucker, J. C. Induction of T cell development from hematopoietic progenitor cells by delta-like-1 in vitro. Immunity 17, 749–756 (2002).
Dervovic, D. D. et al. Cellular and molecular requirements for the selection of in vitro-generated CD8 T cells reveal a role for Notch. J. Immunol. 191, 1704–1715 (2013).
Hameyer, D. et al. Toxicity of ligand-dependent Cre recombinases and generation of a conditional Cre deleter mouse allowing mosaic recombination in peripheral tissues. Physiol. Genomics 31, 32–41 (2007).
Wallace, H. A. et al. Manipulating the mouse genome to engineer precise functional syntenic replacements with human sequence. Cell 128, 197–209 (2007).
Gray, D. H. et al. Unbiased analysis, enrichment and purification of thymic stromal cells. J. Immunol. Methods 329, 56–66 (2008).
Acknowledgements
We thank O. Rodrigues and C. Cryer for cell sorting, V. Berno for imaging, F. H. Stenhouse and C. D. Peddie for technical assistance and J. Mee for kidney grafting, R. Zamoyska, R. Brownlie and G. Cowan for advice, V. Wilson, K. Kaji, A. G. Smith, I. Chambers and N. Hastie for comments on the manuscript, and the Biological Research Facility staff for animal care. The research leading to these results received funding from Leukaemia and Lymphoma Research (C.C.B. and N.B.), the Darwin Trust of Edinburgh (S.U.), the School of Biological Sciences, University of Edinburgh (H.J.V.), the Medical Research Council (C.C.B.), the European Union Seventh Framework Programme (FP7/2007–2013) collaborative projects EuroSyStem (C.C.B. and N.B.) and ThymiStem (C.C.B., S.U., K.E.O’N) under grant agreement numbers 200720 and 602587, respectively, and NIH/NIAID grant no. R01 AI082127 (N.R.M.).
Author information
Authors and Affiliations
Contributions
N.B. generated the iFoxn1 allele, conceived and designed experiments, performed experiments, analysed the data and contributed to writing the manuscript; N.R.M. contributed to experimental design and to writing the manuscript; S.U., K.E.O’N and H.J.V. performed experiments and contributed to analysis of the data; C.C.B. conceived the original idea, designed experiments, contributed to analysis of the data and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 (related to Figure 1). Generation of transgenic Rosa26CAG−STOP−Foxn1−IRES−GFP mice.
(a) The CAG-STOP-Foxn1 cassette shown in Fig. 1 was introduced into the Rosa26 locus in mouse E14tg2a ES cells by homologous recombination using standard procedures, generating the Rosa26CAG−NeoR−STOP−Foxn1−IRES−GFP allele. This cassette contained a cDNA encoding Foxn1 under control of the CAG compound promoter and downstream of a LoxP-flanked CMAZ stop cassette plus an IRES–GFP component to permit monitoring of Foxn1 expression. Neomycin-resistant colonies were picked and screened for targeted insertion by Southern blotting, using the strategy shown in (a) above. The position of restriction enzyme sites and Southern blot hybridization probes are shown for the wild type and transgenic Rosa26locus. EcoRI, EcoRV and PacI restriction enzyme digests were used for 5’, 3’ and internal Southern blot analyses, respectively. (b) Correctly targeted colonies were identified and used to generate chimeric mice via blastocyst injection. Germline transmission was confirmed from two independent ES cell lines (L1 and L2). Founders from each of these Rosa26CAG−NeoR−STOP−Foxn1−IRES−GFP lines were crossed with Tg(CAG-FLPe) mice39 in order to remove the neomycin resistance cassette (NeoR). These lines were then backcrossed to C57BL/6 mice for five generations before analysis.
Supplementary Figure 2 (related to Figure 1). Absence of tamoxifen-independent Cre-recombinase activity in Rosa26CAG−STOP−Foxn1−IRES−GFP MEFs.
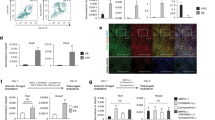
MEFs of the genotypes shown were isolated and treated with 1μM 4OHT or carrier solution for 48 hours, then (A) analyzed by flow cytometry for expression of GFP and EpCam after a further 4 days in culture, or (B) analyzed for Foxn1mRNA expression by RT-qPCR (without further culture). Data in (B) show Foxn1mRNA expression relative to the geometric mean of 2 housekeepers, determined for two Foxn1 primer/ UPL probe sets, Foxn1 68 and Foxn1 32. No GFP or Foxn1expression was detected in the absence of tamoxifen/4OHT, indicating that leakiness caused by ligand-independent Cre-recombinase activity did not occur in this system.
Supplementary Figure 3 (related to Figure 2). iFoxn1TEC are responsive to Fgf7 in vitro.
Plots show flow cytometric analysis of CD45+ cells following co-culture on iTEC for 12 days in the presence or absence of Fgf7. iTEC (five days after induction of Foxn1) were plated at low density (5 × 104 cells per well) or high density (2 × 105 cells per well) into a 24-well plate. Following a further 2 days each well was seeded with 3 × 103 ETP thymocytes (CD45+Lin−CD25−C-Kit+) isolated from E14.5 fetal thymi and cultured for 12 days before analysis.
Supplementary Figure 4 (related to Figure 2). Comparison of the kinetics of T cell development in vitro from ETP seeded onto iTEC or OP9-DL1 cells.
ETP were isolated from E14.5 fetal thymi and seeded at a density of 3000 cells per well onto OP9-DL1 cells (plated the previous day at a density of 2 × 104 per well) or iTEC (density 2 × 105) in 24 well plates. The OP9-DL1/ETP co-cultures were subsequently cultured in medium containing IL7 (5 ng ml−1) and Flt3L (5 ng ml−1) (Porrit et al., 2004) until day 6 of culture, then IL7 (1 ng ml−1) and Flt3L (5 ng ml−1) until the end of the experiment, while the iTEC/ETP and control MEF/ETP co-cultures were cultured in medium containing IL7 (1 ng ml−1) and Flt3L (5 ng ml−1) throughout. Cultures were analyzed by flow cytometry with the markers shown after 4, 8 or 12 days of co-culture. n = 1. Note that the iTEC used for the above experiments were made by isolating MEFs from E13.5 Rosa26CAG−STOP−Foxn1−IRES−GFP embryos; these MEFs were expanded in culture for 4 days, then treated with 1 μM 4OHT for 48 hours. The following day, GFP+ cells were isolated by flow cytometric cell sorting, then plated into 24 well plates at a density of 2 × 105 cells per well. They were seeded with ETPs 3 days later. This protocol differs slightly from the protocol used in Fig. 2.
Supplementary Figure 5 (related to Figure 5). Haplotype analysis demonstrates the presence of donor-derived T cells in iTEC-graft recipients.
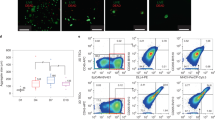
Representative analysis of splenocytes from iTEC-grafted or control-grafted nu/nu mice seven weeks post-transplantation, and wild type (WT) C57BL/6xCBA F1 mice. Plots show staining for H2Kk on CD4+ and CD8+ splenocytes after gating on live cells. The donor ETP within the iTEC and control grafts were from C57BL/6xCBA F1 embryos and therefore expressed b and k haplotypes of MHC Class I and II antigens. The recipient mice were CD1nu/nu, which are of undetermined haplotype, but do not express H2Kk as shown. Most splenic T cells in the iTEC recipients are donor-derived (i.e. express H2Kk).
Supplementary information
Supplementary Information
Supplementary Information (PDF 682 kb)
Rights and permissions
About this article
Cite this article
Bredenkamp, N., Ulyanchenko, S., O’Neill, K. et al. An organized and functional thymus generated from FOXN1-reprogrammed fibroblasts. Nat Cell Biol 16, 902–908 (2014). https://doi.org/10.1038/ncb3023
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncb3023
This article is cited by
-
De novo construction of T cell compartment in humanized mice engrafted with iPSC-derived thymus organoids
Nature Methods (2022)
-
Limits to in vivo fate changes of epithelia in thymus and parathyroid by ectopic expression of transcription factors Gcm2 and Foxn1
Scientific Reports (2022)
-
Epigenetic modifications in thymic epithelial cells: an evolutionary perspective for thymus atrophy
Clinical Epigenetics (2021)
-
T cell regeneration after immunological injury
Nature Reviews Immunology (2021)
-
The role of the thymus in allogeneic bone marrow transplantation and the recovery of the peripheral T-cell compartment
Seminars in Immunopathology (2021)