Abstract
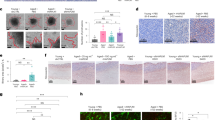
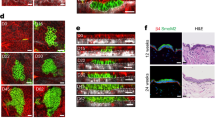
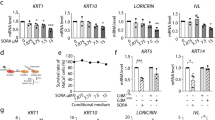
Angiogenesis is critical during tumour initiation and malignant progression1. Different strategies aimed at blocking vascular endothelial growth factor (VEGF) and its receptors have been developed to inhibit angiogenesis in cancer patients2. It has become increasingly clear that in addition to its effect on angiogenesis, other mechanisms including a direct effect of VEGF on tumour cells may account for the efficiency of VEGF-blockade therapies3. Cancer stem cells (CSCs) have been described in various cancers including squamous tumours of the skin4,5. Here we use a mouse model of skin tumours to investigate the impact of the vascular niche and VEGF signalling on controlling the stemness (the ability to self renew and differentiate) of squamous skin tumours during the early stages of tumour progression. We show that CSCs of skin papillomas are localized in a perivascular niche, in the immediate vicinity of endothelial cells. Furthermore, blocking VEGFR2 caused tumour regression not only by decreasing the microvascular density, but also by reducing CSC pool size and impairing CSC renewal properties. Conditional deletion of Vegfa in tumour epithelial cells caused tumours to regress, whereas VEGF overexpression by tumour epithelial cells accelerated tumour growth. In addition to its well-known effect on angiogenesis, VEGF affected skin tumour growth by promoting cancer stemness and symmetric CSC division, leading to CSC expansion. Moreover, deletion of neuropilin-1 (Nrp1), a VEGF co-receptor expressed in cutaneous CSCs, blocked VEGF’s ability to promote cancer stemness and renewal. Our results identify a dual role for tumour-cell-derived VEGF in promoting cancer stemness: by stimulating angiogenesis in a paracrine manner, VEGF creates a perivascular niche for CSCs, and by directly affecting CSCs through Nrp1 in an autocrine loop, VEGF stimulates cancer stemness and renewal. Finally, deletion of Nrp1 in normal epidermis prevents skin tumour initiation. These results may have important implications for the prevention and treatment of skin cancers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Kerbel, R. S. Tumor angiogenesis. N. Engl. J. Med. 358, 2039–2049 (2008)
Ferrara, N., Mass, R. D., Campa, C. & Kim, R. Targeting VEGF-A to treat cancer and age-related macular degeneration. Annu. Rev. Med. 58, 491–504 (2007)
Ellis, L. M. & Hicklin, D. J. VEGF-targeted therapy: mechanisms of anti-tumour activity. Nature Rev. Cancer 8, 579–591 (2008)
Lobo, N. A., Shimono, Y., Qian, D. & Clarke, M. F. The biology of cancer stem cells. Annu. Rev. Cell Dev. Biol. 23, 675–699 (2007)
Malanchi, I. et al. Cutaneous cancer stem cell maintenance is dependent on β-catenin signalling. Nature 452, 650–653 (2008)
Alam, M. & Ratner, D. Cutaneous squamous-cell carcinoma. N. Engl. J. Med. 344, 975–983 (2001)
Perez-Losada, J. & Balmain, A. Stem-cell hierarchy in skin cancer. Nature Rev. Cancer 3, 434–443 (2003)
Kemp, C. J. Multistep skin cancer in mice as a model to study the evolution of cancer cells. Semin. Cancer Biol. 15, 460–473 (2005)
Calabrese, C. et al. A perivascular niche for brain tumor stem cells. Cancer Cell 11, 69–82 (2007)
Butler, J. M., Kobayashi, H. & Rafii, S. Instructive role of the vascular niche in promoting tumour growth and tissue repair by angiocrine factors. Nature Rev. Cancer 10, 138–146 (2010)
Kiel, M. J. & Morrison, S. J. Maintaining hematopoietic stem cells in the vascular niche. Immunity 25, 862–864 (2006)
Witte, L. et al. Monoclonal antibodies targeting the VEGF receptor-2 (Flk1/KDR) as an anti-angiogenic therapeutic strategy. Cancer Metastasis Rev. 17, 155–161 (1998)
Miller, D. W. et al. Rapid vessel regression, protease inhibition, and stromal normalization upon short-term vascular endothelial growth factor receptor 2 inhibition in skin carcinoma heterotransplants. Am. J. Pathol. 167, 1389–1403 (2005)
Lichtenberger, B. M. et al. Autocrine VEGF signaling synergizes with EGFR in tumor cells to promote epithelial cancer development. Cell 140, 268–279 (2010)
Rossiter, H. et al. Loss of vascular endothelial growth factor A activity in murine epidermal keratinocytes delays wound healing and inhibits tumor formation. Cancer Res. 64, 3508–3516 (2004)
Hirakawa, S. et al. VEGF-A induces tumor and sentinel lymph node lymphangiogenesis and promotes lymphatic metastasis. J. Exp. Med. 201, 1089–1099 (2005)
Larcher, F., Murillas, R., Bolontrade, M., Conti, C. J. & Jorcano, J. L. VEGF/VPF overexpression in skin of transgenic mice induces angiogenesis, vascular hyperpermeability and accelerated tumor development. Oncogene 17, 303–311 (1998)
Gerber, H. P. et al. VEGF is required for growth and survival in neonatal mice. Development 126, 1149–1159 (1999)
Lechler, T. & Fuchs, E. Asymmetric cell divisions promote stratification and differentiation of mammalian skin. Nature 437, 275–280 (2005)
Poulson, N. D. & Lechler, T. Robust control of mitotic spindle orientation in the developing epidermis. J. Cell Biol. 191, 915–922 (2010)
Williams, S. E., Beronja, S., Pasolli, H. A. & Fuchs, E. Asymmetric cell divisions promote Notch-dependent epidermal differentiation. Nature 470, 353–358 (2011)
Maes, C. et al. Increased skeletal VEGF enhances β-catenin activity and results in excessively ossified bones. EMBO J. 29, 424–441 (2010)
Soker, S., Takashima, S., Miao, H. Q., Neufeld, G. & Klagsbrun, M. Neuropilin-1 is expressed by endothelial and tumor cells as an isoform-specific receptor for vascular endothelial growth factor. Cell 92, 735–745 (1998)
Staton, C. A., Kumar, I., Reed, M. W. & Brown, N. J. Neuropilins in physiological and pathological angiogenesis. J. Pathol. 212, 237–248 (2007)
Pan, Q. et al. Blocking neuropilin-1 function has an additive effect with anti-VEGF to inhibit tumor growth. Cancer Cell 11, 53–67 (2007)
Vasioukhin, V., Bauer, C., Degenstein, L., Wise, B. & Fuchs, E. Hyperproliferation and defects in epithelial polarity upon conditional ablation of alpha-catenin in skin. Cell 104, 605–617 (2001)
Vasioukhin, V., Degenstein, L., Wise, B. & Fuchs, E. The magical touch: genome targeting in epidermal stem cells induced by tamoxifen application to mouse skin. Proc. Natl Acad. Sci. USA 96, 8551–8556 (1999)
Gerber, H. P. et al. VEGF is required for growth and survival in neonatal mice. Development 126, 1149–1159 (1999)
Gu, C. et al. Neuropilin-1 conveys semaphorin and VEGF signaling during neural and cardiovascular development. Dev. Cell 5, 45–57 (2003)
Abel, E. L., Angel, J. M., Kiguchi, K. & DiGiovanni, J. Multi-stage chemical carcinogenesis in mouse skin: fundamentals and applications. Nature Protocols 4, 1350–1362 (2009)
Acknowledgements
We thank Genetech for providing blocking anti-Nrp1 antibodies and H. Fujisawa, N. Ferrara and A. Nagy for providing the Nrp1fl/−, Vegffl/fl and ROSA26-VEGF-164 mice, respectively. C.B. is an investigator of Welbio. C.B. and P.A.S. are chercheur qualifié and B.B. is a chargé de recherche of the FRS/FNRS; Am.C. and G.M. are research fellows of the FRS/FRIA. G.D. is supported by the Brussels Region, B.D. and K.K.Y. by TELEVIE and. S.G. is a postdoctoral fellow of the Basic Science Research Foundation-Flanders (FWO). S.L. is funded by the Max-Eder group leader program of the Deutsche Krebshilfe, by the Hamburger Krebsgesellschaft and by the Roggenbuck Stiftung. P.C. is funded by Long-term structural Methusalem funding by the Flemish Government. This work was supported by the FNRS, the program d’excellence CIBLES of the Wallonia Region, a research grant from the Fondation Contre le Cancer, the ULB foundation and the fond Gaston Ithier, a starting grant of the European Research Council (ERC) and the EMBO Young Investigator Program.
Author information
Authors and Affiliations
Contributions
C.B., B.B., G.D., S.G., K.K.Y., P.C. and J.J.H. designed the experiments and performed data analysis. B.B., G.D., S.G., K.K.Y., G.L., S.L. and A.K. performed most of the experiments; P.A.S., Au.C., G.M. and B.D. contributed to mice treatment; S.D. and Am.C. provided technical support. C.B. and B.B. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Figures
The file contains Supplementary Figures 1-15 with legends. (PDF 5657 kb)
Rights and permissions
About this article
Cite this article
Beck, B., Driessens, G., Goossens, S. et al. A vascular niche and a VEGF–Nrp1 loop regulate the initiation and stemness of skin tumours. Nature 478, 399–403 (2011). https://doi.org/10.1038/nature10525
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature10525
This article is cited by
-
Cross-talk between cancer stem cells and immune cells: potential therapeutic targets in the tumor immune microenvironment
Molecular Cancer (2023)
-
Histone modifications in drug-resistant cancers: From a cancer stem cell and immune evasion perspective
Experimental & Molecular Medicine (2023)
-
Advances in cutaneous squamous cell carcinoma
Nature Reviews Cancer (2023)
-
VEGF/Nrp1/HIF-1α promotes proliferation of hepatocellular carcinoma through a positive feedback loop
Medical Oncology (2023)
-
Breast cancer stem cells generate immune-suppressive T regulatory cells by secreting TGFβ to evade immune-elimination
Discover Oncology (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.