Abstract
The presence of two or more prostate cancer foci separated by intervening benign tissue in a single core is a well-recognized finding on prostate biopsy. Cancer involvement can be measured by including intervening benign tissue or only including the actual cancer involved area. Importantly, this parameter is a common enrollment criterion for active surveillance protocols. We hypothesized that spatially distinct prostate cancer foci in biopsies may arise from separate clones, impacting cancer involvement assessment. Hence, we used dual ERG/SPINK1 immunohistochemistry to determine the frequency of separate clones—when separate tumor foci showed discordant ERG and/or SPINK1 status—in discontinuously involved prostate biopsy cores from two academic institutions. In our cohort of 97 prostate biopsy cores with spatially discrete tumor foci (from 80 patients), discontinuous cancer involvement including intervening tissue ranged from 20 to 100% and Gleason scores ranged from 6 to 9. Twenty-four (25%) of 97 discontinuously involved cores harbored clonally distinct cancer foci by discordant ERG and/or SPINK1 expression status: 58% (14/24) had one ERG+ focus, and one ERG−/SPINK1− focus; 29% (7/24) had one SPINK1+ focus and one ERG−/SPINK1− focus; and 13% (3/24) had one ERG+ focus and one SPINK1+ focus. ERG and SPINK1 overexpression were mutually exclusive in all tumor foci. In summary, our results show that ~25% of discontinuously involved prostate biopsy cores showed tumor foci with discordant ERG/SPINK1 status, consistent with multiclonal disease. The relatively frequent presence of multiclonality in discontinuously involved prostate biopsy cores warrants studies on the potential clinical impact of clonality assessment, particularly in cases where tumor volume in a discontinuous core may impact active surveillance eligibility.
Similar content being viewed by others
Main
Although prostate cancer is the second leading cause of cancer-related deaths in men in the United States, early detection with serum prostate-specific antigen (PSA) has led to the over-detection and over-treatment of indolent prostate cancer.1, 2, 3 Recently, active surveillance, where men newly diagnosed with prostate cancer undergo serial biopsy, PSA and/or imaging to delay intervention until prompted by clinicopathological evidence of disease progression (or patient decision), has emerged as management strategy for low-risk prostate cancer that does not significantly decrease prostate cancer-specific mortality compared with immediate treatment.4, 5, 6
Despite advances in imaging and prognostic expression/protein assays, serum PSA and clinicopathological parameters are the only factors routinely used to assess prognosis at diagnosis.4, 6, 7, 8, 9, 10, 11 Although pathological inclusion criteria for active surveillance protocols vary by institution or group, almost all include Gleason score, number (or percentage) of positive cores and the tumor measurement/length or maximum percentage of tumor involvement in any core.4, 5, 11, 12, 13, 14, 15 In particular, >50% of tumor involvement in any given core is commonly considered as an exclusion criterion for most active surveillance protocols.4, 5, 11, 12, 13, 14, 15
However, when two or more foci of prostate cancer separated by intervening benign tissue are present in a single core biopsy, there is currently no consensus dictating the optimal method to report such a tumor involvement percentage. The pathologist can either (1) measure discontinuous foci as if they were one continuous tumor by including the benign intervening tissue, assuming they represent two sections of a unique tumor, or (2) only measure the areas actually involved by a tumor focus. The first option, which would report a higher percentage of tumor involvement of a core, has been proposed to be the optimal method by suggesting it is more representative of tumor volume at prostatectomy.16
Prostate cancer is known to be a multifocal disease,17 with most radical prostatectomy specimens actually harboring clonally distinct tumor foci, as supported by single-marker molecular subtyping and next-generation sequencing.18, 19, 20, 21, 22, 23, 24 Of note, approximately 50% of PSA-screened prostate cancer foci in predominantly Caucasian populations harbor chromosomal rearrangements that result in the fusion of the 5′ untranslated region of TMPRSS2 to ERG, an ETS transcription factor, which can be detected by fluorescence in situ hybridization (FISH) or immunohistochemistry.25, 26, 27 In addition, about 10% of prostate cancers show marked overexpression of SPINK1, which can be evaluated concurrently with ERG by dual immunohistochemistry.28, 29 Importantly, in these studies, ERG fusion status has been shown to be clonal in a given tumor focus, and SPINK1 and ERG show essentially mutually exclusive expression. Hence, dual ERG/SPINK1 immunohistochemistry represents a simple, rapid and inexpensive method to assess tumor clonality in routine specimens.
In this study, we hypothesized that spatially distinct tumor foci in a given biopsy core may arise from separate clones, and sought to determine the frequency of such multiclonality. Thus, we used ERG/SPINK1 dual immunohistochemistry to determine whether discontinuous cancer foci truly represent the same tumor clone (uniform ERG/SPINK1 status in separate foci), or multiclonal disease (discordant ERG/SPINK1 status between foci). Results of this pilot study show multiclonality in 25% of discontinuously involved cores, supporting additional studies on whether clonality impacts the prognostic ability of tumor volume at biopsy and prostatectomy.
Materials and methods
Patient Population and Specimen Collection
Surgical pathology databases were searched for prostatic needle core biopsies containing ‘discontinuous prostatic adenocarcinoma’ diagnosed between 2010 and 2013 at two institutions, Weill Medical College of Cornell University and University of Michigan. This study was performed with institutional review board approval from each institution.
Determining Tumor Involvement
Two genitourinary pathologists reviewed the hematoxylin and eosin (H&E)-stained slides for each case; biopsies with confirmed discontinuous foci of prostatic adenocarcinoma were selected. Only biopsies with intact cores (measuring at least 1 cm) were included in the study. As there are no consensus criteria for determining ‘discontinuous foci’, in this study we considered biopsies with tumor foci separated by at least 2.5 mm or 25% of total core volume as discontinuously involved (Figures 1a–c). For each core, the Gleason score was verified, and we determined the maximum percentage of tumor involvement by (1) routine histomorphology (inclusive of discontinuous foci), as well as (2) tumor involvement measured after evaluating ERG/SPINK1 status (if discontinuously staining foci were present, we added the percentage of both foci (Figures 1a–c).
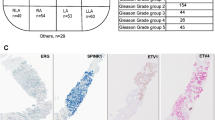
Clonal evaluation in prostate biopsies with discontinuous tumor foci through ERG/SPINK1 dual immunohistochemistry reveals relatively frequent multiclonality. (a) Discontinuously involved cores (black indicates cancer foci) can be assessed by including intervening benign tissue (ie, 80%, left side) or including only cancer (ie, 15%+5%, right side). (b) The former assumes that both foci are from the same tumor clone (biopsy core path schematically represented in orange) as visualized at radical prostatectomy (RP). The latter assumes the foci are from separate clones. (c) ERG+/SPINK1−, ERG−/SPINK1− and ERG−/SPINK1+ prostate cancer represent essentially mutually exclusive molecular prostate cancer subtypes. Hence, we hypothesized that dual ERG/SPINK1 expression by immunohistochemistry (IHC) can be used to assess clonality in discontinuous foci. Discordant ERG/SPINK1 status in spatially distinct foci would confirm the presence of smaller, clonally distinct tumors at RP (schematic representation of two molecularly distinct tumors in different colors according to the legend). (d) We performed dual ERG/SPINK1 immunohistochemistry on 97 discontinuously involved prostate biopsy cores. H&E staining and dual ERG/SPINK1 immunohistochemistry are shown from a discontinuously involved core. Both tumor foci (green and red boxes) were ERG+/SPINK1− consistent with concordant involvement and likely clonality. Note, whole core H&E and ERG/SPINK1 immunohistochemistry images are composites of two x2 original magnification photomicrographs; original magnification of individual tumor foci photomicrographs was x20 (insets of black dashed boxes shown at higher magnification). (e) Gleason score (G.S.), percent tumor involvement (% Inv.; inclusive of benign tissue) and ERG/SPINK1 staining in both foci of all assessed cores are shown in a heatmap according to the legend. Multiclonal cores, as evidenced by discordant ERG/SPINK1 staining between foci, are indicated by the red bracket.
Evaluation of Tumor Clonality by ERG/SPINK1 Dual Immunohistochemistry
Dual ERG/SPINK1 immunohistochemistry staining28 was performed on 5-μm-thick unstained slides. These corresponded to intervening unstained levels generated as part of the standard diagnostic workup, or de-stained H&E slides when unstained slides were not available or tissue was exhausted from the block. Immunohistochemistry was performed either on the BenchMark ULTRA or the DISCOVERY XT automated staining systems (Ventana Medical System, Inc., Tucson, AZ, USA). A monoclonal rabbit anti-ERG primary antibody from Ventana Medical Systems (EPR3864) and a mouse primary anti-SPINK1 4D4 antibody (Abnova, Taiwan) were used, as previously described.26, 28, 29, 30 Brown and red chromogens were used for ERG and SPINK1, respectively.
Tumor foci with intense (2+ or 3+) and diffuse (at least 90% of cancer cells) nuclear ERG staining were considered as ERG positive (ERG+). Endothelial cell nuclear staining was used as a positive internal control. Tumor foci with intense (2+ or 3+) cytoplasmic SPINK1 staining in >10% of cancer cells were considered SPINK1 positive (SPINK1+).
Biopsies were considered multiclonal if they harbored spatially distinct foci with discrepant ERG and/or SPINK1 status (ie, one ERG+/SPINK1− focus and one ERG−/SPINK1− focus; one ERG−/SPINK1− focus and one ERG−/SPINK1+ focus; or one ERG+/SPINK1− focus and one ERG−/SPINK1+ focus). Biopsies with uniform ERG or SPINK1 staining of tumor foci were considered clonal (Figures 1a–d).
Results
Ninety-seven prostate needle biopsies from 80 patients fulfilled our criteria for discontinuous involvement by prostatic adenocarcinoma (Table 1). Gleason scores ranged from 6 to 9. Maximum tumor involvement, including benign intervening tissue, ranged from 20 to 100% of core length. Overall, ERG+ and SPINK1+ frequency (assessed per core) was 38% (37/97) and 12% (12/97), respectively. ERG and SPINK1 expression was mutually exclusive in all evaluated tumor foci. ERG/SPINK1 immunohistochemistry status, Gleason score and maximum tumor involvement for all evaluated cores are shown in a heatmap in Figure 1e. Benign prostate tissue was negative for ERG or SPINK1 expression, consistent previous reports of exceptionally rare staining for either antigen in benign prostate tissue.23, 24, 26, 28, 30
Of the 97 biopsies with discontinuous tumor, 24 (25%) showed discrepant ERG/SPINK1 status between spatially distinct foci (Table 2). Within these 24 multiclonal biopsies, 14 (58%) harbored one ERG+/SPINK− focus and one ERG−/SPINK1− focus; 7 (29%) harbored one ERG−/SPINK1+ focus and one ERG−/SPINK1− focus; and 3 (13%) showed one ERG+/SPINK1− focus and one ERG−/SPINK1+ focus (examples of discordant foci are shown in Figure 2). When determining clonality by only considering ERG status, 17 (17.5%) had discordant ERG status between foci, consistent with multiclonal disease.
Identification of two clonally distinct tumor foci on discontinuously involved prostate needle biopsy cores by dual ERG/SPINK1 immunohistochemistry. H&E staining identifies two separate tumors that discontinuously involve 80% of one core in these two cases. Immunohistochemistry staining shows discordant ERG/SPINK1 status between foci (ERG, brown chromogen, nuclear localization; SPINK1, red chromogen, cytoplasmic localization). One focus is ERG+/SPINK− (right) and the other one is ERG−/SPINK1− (left). One focus is ERG−/SPINK1+ (right) and the other is ERG−/SPINK1− (left), consistent with distinct clonal origin. Original images from whole slide imager scanned slides; insets of solid and dashed black boxes shown at higher magnification.
In the 24 multiclonal biopsies, Gleason scores were 3+3=6 in 54% (13/24), 3+4=7 in 21% (5/24), 4+3=7 in 17% (4/24) and 4+4=8 in 12% (2/24) of cores. There were no multiclonal cores with Gleason score ≥9 in our cohort. Maximum tumor involvement percentage in multiclonal biopsies, including intervening benign tissue, ranged from 20 to 100%. After incorporating multiclonal assessment (collapsing involvement to the summed tumor lengths of foci with discordant ERG/SPINK1 status), maximum tumor involvement percentage fell under under 50% in 22/24 biopsies (92%).
Discussion
Recent consensus statements recommend reporting the amount of cancer in prostate biopsies by estimating the percentage of tumor involvement in the core with the greatest tumor extent.11, 31 Importantly, this pathology parameter has been shown to be correlated with tumor volume at prostatectomy.32 Although measuring the percentage of involvement in a core may seem straightforward, it can be challenging for the pathologist when assessing biopsy cores with discontinuous tumor separated by benign intervening tissue, which is a well-recognized finding on prostate biopsies. There is currently no consensus on the best method—including or excluding intervening benign tissue—when reporting tumor percent involvement in a discontinuously involved core. The choice of method remains controversial between pathologists, and both techniques are being utilized clinically.33, 34, 35
Brimo et al34 reported no significant difference using either tumor content estimation technique on predicting pathologic outcome at prostatectomy, although they included cases in which the amount of intervening benign tissue was <5 mm.
However, recent studies propose reporting the maximum tumor involvement, including the benign intervening tissue, assuming that the separate foci represent the same tumor coming in and out of the core section. Karram et al16 showed that this measurement method better correlated with stage and margin positivity in cases with Gleason 6 on biopsy with no upgrade at radical prostatectomy. Schultz et al35 further supported this finding in a private practice setting.
Multiclonality/multifocality is well recognized at prostatectomy, as spatially distinct tumor foci are routinely appreciated. Importantly, molecular evidence supporting true multiclonality of distinct tumor foci has been demonstrated by our groups and others using ERG status (by FISH or immunohistochemistry as a surrogate) to identify distinct foci.18, 19, 20, 23, 24 A recent study assessed clonality between biopsies in patients with multiple positive biopsy cores, using ERG immunohistochemistry as a clonal marker. In that study, Mertz et al36 showed that approximately 12% of prostate needle biopsy sets in their cohort of patients with indolent prostate cancer showed heterogeneous ERG staining. In this study, we show that 25% of discontinuously involved prostate biopsies harbor clonally distinct tumors, revealed by discrepant ERG and/or SPINK1 immunohistochemistry status between foci. To our knowledge, this represents the first study to interrogate prostate cancer clonality in core needle biopsies with discontinuous tumor involvement. Although associations with disease burden at prostatectomy must be established in cases where the discontinuously involved core drives management, we hypothesize that reporting tumor volume by excluding intervening benign tissue (instead of including intervening benign tissue) will be more appropriate in cores with multiclonal discontinuous involvement. Hence, ERG/SPINK1 evaluation in such cases would be expected to increase the number of men eligible for active surveillance by identifying those with multiclonal involvement.
In our study, the frequency of ERG and SPINK1 overexpression was comparable to previous studies at 38% (37/97) and 12% (12/97), respectively. As expected, ERG status was therefore the major driver in determining clonality, as 17/24 (71%) of multiclonal cases showed at least one ERG+ focus. However, incorporating SPINK1 in a dual staining with ERG adds further data to support distinct clonal origin, as ERG+ and SPINK1+ represent distinct molecular prostate cancer subclasses and their expression is essentially mutually exclusive.23, 29, 37, 38, 39 Although other molecular subtypes have been identified (eg, SPOP mutated), routine assays to identify them in situ (or surrogate tissue-based markers) are not yet available.40, 41 Although heterogeneous SPINK1 status has been observed within the same tumor focus,42 in our experience with prostatectomy specimens this usually represents discrepant staining between the leading edge and center of a given focus.23, 28 Thus, although we interpret discordant SPINK1 staining between two discontinuous foci on biopsy as evidence of multiclonality (as a leading edge of both can be appreciated), this will require further validation using alternative techniques.
Given that this study represents, to our knowledge, the first assessment of multiclonality in discontinuously involved cores, we included cores from cases where tumor content of the discontinuous core would not have impacted potential active surveillance inclusion (eg, the discontinuously involved core or other core had high-grade/volume disease or numerous other cores were positive). However, our cohort did include cases where evaluation of the discontinuously involved core may have had a key role in clinical management. For example, one core was from a patient diagnosed with Gleason 3+3=6 prostate cancer in 1 of 12 cores, with cancer discontinuously involved 80% of the core (Figure 3). This case was reviewed by an expert genitourinary pathologist at an outside institution, who agreed with high volume discontinuous involvement, and the patient underwent surgery. At radical prostatectomy, only a single, small (0.7 cm in greatest dimension) focus of Gleason score 6, organ confined prostate cancer was present, consistent with clinically insignificant disease by standard Epstein criteria.43 ERG/SPINK1 dual immunohistochemistry on the involved biopsy core demonstrated discordant ERG/SPINK1 status between the foci (Figure 3), and hence clonality assessment would support this patient as having two small foci (occupying a total of ~20% (~15 and <5% individually) of the core), warranting consideration for active surveillance.
Multiclonality in a patient with a single involved biopsy core who had insignificant disease at prostatectomy. Rarely, a discontinuously involved core can impact management in men potentially eligible for active surveillance. An example from a patient diagnosed with Gleason score 3+3=6 prostate cancer in 1 of 12 cores, with tumor discontinuously involving 80% of the core is shown. At prostatectomy, a single, small focus of Gleason score 6, organ confined cancer was present, consistent with clinically insignificant disease. Retrospective ERG/SPINK1 dual immunohistochemistry on the involved biopsy core demonstrated discordant ERG/SPINK1 status between the foci (green and red boxes), and hence clonality assessment on the biopsy would support this patient as having two small foci (occupying ~15 and <5% of the core), rather than a single focus involving 80% of the core. Original magnification: whole cores x2, green tumor focus x10, red tumor focus x20; insets of dashed black boxes shown at higher magnification.
Of interest, Arias-Stella et al44 recently assessed a cohort of 40 patients where a discontinuously involved prostate biopsy core (when including intervening benign tissue) represented the maximally involved core and patients underwent prostatectomy. In their cohort, although 78% of patients had a single tumor focus in the corresponding region at prostatectomy, 22% had multiple small cancer foci.44 These results, when combined with our identification of multiclonality in ~25% of discontinuous foci on biopsy, further support the need to determine whether clonality assessment at biopsy can be used to stratify disease involvement before prostatectomy.
There are several limitations to acknowledge in our study. First, we are likely underestimating the true rate of multiclonality, given that concordant discontinuous foci may still represent distinct tumor clones that cannot be resolved using currently available in situ assays. For example, in a biopsy with two discontinuous tumor foci that are ERG− and SPINK1−, they may still represent two different clones (as would be supported if SPOP mutant and SPOP wild type). Second, we assessed a relatively small cohort, which may reflect that not all pathologists at our institutions have adopted the approach of reporting ‘discontinuous’ cancer involvement on needle core biopsies, particularly in cases where it is unlikely to drive management. Similarly, we included cases where the discontinuous core did not drive management (eg, the discontinuous core or other positive cores had Gleason score >6, there were multiple other positive cores or other high volume involved cores). Our study is a proof of principle study assessing the frequency of multiclonality across prostate biopsies with discontinuous tumor foci. Therefore, further validation on larger study sets including prospectively collected cohorts (eg, active surveillance) is essential. Confirmation of our hypothesis would provide compelling evidence that multifocal disease is common in biopsies with discontinuous tumor, supporting the opportunity to refine key histopathological parameters through incorporating multiclonality assessment to provide more accurate prognostic information. Similarly, assessment of the prognostic impact on assigned Gleason scores in discontinuously involved cores may also be of interest (eg, a discontinuous Gleason score 3+4=7 foci may actually represent separate Gleason score 4+4=8 and 3+3=6 foci). We expect that assessment of ERG/SPINK1 for clonality may also have utility in selected scenarios at prostatectomy. For example, we are assessing whether incorporation of ERG/SPINK1 in Gleason score 7 tumors may improve the prognostic ability of routine pathologic parameters (eg, Gleason score and tumor size) through identifying tumors that are collisions of foci with distinct ERG/SPINK1 status. Examples of prostatectomy cases where a single tumor focus by morphology are composed of foci with discordant ERG/SPINK1 status are shown in Supplementary Figure S1.
In summary, in our study, nearly 25% of prostate core biopsies with discontinuous tumor involvement harbored spatially molecularly distinct cancer foci, as indicated by discrepant ERG and/or SPINK1 status. Here we demonstrate that assessment of tumor clonality by ERG/SPINK1 dual immunohistochemistry in biopsies with discontinuous involvement of prostate cancer is an effective tool to refine histopathological parameters, specifically estimation of tumor involvement when discontinuous foci are present in prostate biopsies. Incorporation of this inexpensive ancillary test may have significant impact on routine practice as it could potentially increase the number of eligible patients for active surveillance. Clinical application of ERG/SPINK1 dual immunohistochemistry is an important area for continued study.
References
Etzioni R, Penson DF, Legler JM et al. Overdiagnosis due to prostate-specific antigen screening: lessons from U.S. prostate cancer incidence trends. J Natl Cancer Inst 2002;94:981–990.
Etzioni RD, Thompson IM . What do the screening trials really tell us and where do we go from here? Urol Clin North Am 2014;41:223–228.
Siegel RL, Miller KD, Jemal A . Cancer statistics, 2015. CA Cancer J Clin 2015;65:5–29.
Dall'Era MA, Albertsen PC, Bangma C et al. Active surveillance for prostate cancer: a systematic review of the literature. Eur Urol 2012;62:976–983.
Singer EA, Kaushal A, Turkbey B et al. Active surveillance for prostate cancer: past, present and future. Curr Opin Oncol 2012;24:243–250.
Glass AS, Punnen S, Cooperberg MR . Divorcing diagnosis from treatment: contemporary management of low-risk prostate cancer. Korean J Urol 2013;54:417–425.
Cary KC, Cooperberg MR . Biomarkers in prostate cancer surveillance and screening: past, present, and future. Ther Adv Urol 2013;5:318–329.
Nguyen HG, Welty CJ, Cooperberg MR . Diagnostic associations of gene expression signatures in prostate cancer tissue. Curr Opin Urol 2015;25:65–70.
Kristiansen G . Diagnostic and prognostic molecular biomarkers for prostate cancer. Histopathology 2012;60:125–141.
Heidenreich A, Bastian PJ, Bellmunt J et al. EAU guidelines on prostate cancer. part 1: screening, diagnosis, and local treatment with curative intent-update 2013. Eur Urol 2014;65:124–137.
Delahunt B, Hammond E, Egevad L et al. Active surveillance for prostate cancer: the role of the pathologist. Pathology 2015;47:1–3.
Klotz L . Active surveillance: patient selection. Curr Opin Urol 2013;23:239–244.
Bul M, Zhu X, Valdagni R et al. Active surveillance for low-risk prostate cancer worldwide: the PRIAS study. Eur Urol 2013;63:597–603.
Buethe DD, Pow-Sang J . Enrollment criteria controversies for active surveillance and triggers for conversion to treatment in prostate cancer. J Natl Compr Canc Netw 2012;10:1101–1110.
Tosoian JJ, Trock BJ, Landis P et al. Active surveillance program for prostate cancer: an update of the Johns Hopkins experience. J Clin Oncol 2011;29:2185–2190.
Karram S, Trock BJ, Netto GJ et al. Should intervening benign tissue be included in the measurement of discontinuous foci of cancer on prostate needle biopsy? Correlation with radical prostatectomy findings. Am J Surg Pathol 2011;35:1351–1355.
Arora R, Koch MO, Eble JN et al. Heterogeneity of Gleason grade in multifocal adenocarcinoma of the prostate. Cancer 2004;100:2362–2366.
Barry M, Perner S, Demichelis F et al. TMPRSS2-ERG fusion heterogeneity in multifocal prostate cancer: clinical and biologic implications. Urology 2007;70:630–633.
Furusato B, Gao CL, Ravindranath L et al. Mapping of TMPRSS2-ERG fusions in the context of multi-focal prostate cancer. Mod Pathol 2008;21:67–75.
Mehra R, Han B, Tomlins SA et al. Heterogeneity of TMPRSS2 gene rearrangements in multifocal prostate adenocarcinoma: molecular evidence for an independent group of diseases. Cancer Res 2007;67:7991–7995.
Cooper CS, Eeles R, Wedge DC et al. Analysis of the genetic phylogeny of multifocal prostate cancer identifies multiple independent clonal expansions in neoplastic and morphologically normal prostate tissue. Nat Genet 2015;47:367–372.
Boutros PC, Fraser M, Harding NJ et al. Spatial genomic heterogeneity within localized, multifocal prostate cancer. Nat Genet 2015;47:736–745.
Smith SC, Palanisamy N, Zuhlke KA et al. HOXB13 G84E-related familial prostate cancers: a clinical, histologic, and molecular survey. Am J Surg Pathol 2014;38:615–626.
Young A, Palanisamy N, Siddiqui J et al. Correlation of urine TMPRSS2:ERG and PCA3 to ERG+ and total prostate cancer burden. Am J Clin Pathol 2012;138:685–696.
Furusato B, Tan SH, Young D et al. ERG oncoprotein expression in prostate cancer: clonal progression of ERG-positive tumor cells and potential for ERG-based stratification. Prostate Cancer Prostatic Dis 2010;13:228–237.
Park K, Tomlins SA, Mudaliar KM et al. Antibody-based detection of ERG rearrangement-positive prostate cancer. Neoplasia 2010;12:590–598.
Tomlins SA, Rhodes DR, Perner S et al. Recurrent fusion of TMPRSS2 and ETS transcription factor genes in prostate cancer. Science 2005;310:644–648.
Bhalla R, Kunju LP, Tomlins SA et al. Novel dual-color immunohistochemical methods for detecting ERG-PTEN and ERG-SPINK1 status in prostate carcinoma. Mod Pathol 2013;26:835–848.
Tomlins SA, Rhodes DR, Yu J et al. The role of SPINK1 in ETS rearrangement-negative prostate cancers. Cancer Cell 2008;13:519–528.
Tomlins SA, Palanisamy N, Siddiqui J et al. Antibody-based detection of ERG rearrangements in prostate core biopsies, including diagnostically challenging cases: ERG staining in prostate core biopsies. Arch Pathol Lab Med 2012;136:935–946.
Amin MB, Lin DW, Gore JL et al. The critical role of the pathologist in determining eligibility for active surveillance as a management option in patients with prostate cancer: consensus statement with recommendations supported by the College of American Pathologists, International Society of Urological Pathology, Association of Directors of Anatomic and Surgical Pathology, the New Zealand Society of Pathologists, and the Prostate Cancer Foundation. Arch Pathol Lab Med 2014;138:1387–1405.
Poulos CK, Daggy JK, Cheng L . Prostate needle biopsies: multiple variables are predictive of final tumor volume in radical prostatectomy specimens. Cancer 2004;101:527–532.
Egevad L, Allsbrook WC Jr, Epstein JI . Current practice of diagnosis and reporting of prostate cancer on needle biopsy among genitourinary pathologists. Hum Pathol 2006;37:292–297.
Brimo F, Vollmer RT, Corcos J et al. Prognostic value of various morphometric measurements of tumour extent in prostate needle core tissue. Histopathology 2008;53:177–183.
Schultz L, Maluf CE, da Silva RC et al. Discontinuous foci of cancer in a single core of prostatic biopsy: when it occurs and performance of quantification methods in a private-practice setting. Am J Surg Pathol 2013;37:1831–1836.
Mertz KD, Horcic M, Hailemariam S et al. Heterogeneity of ERG expression in core needle biopsies of patients with early prostate cancer. Hum Pathol 2013;44:2727–2735.
Tomlins SA, Alshalalfa M, Davicioni E et al. Characterization of 1577 primary prostate cancers reveals novel biological and clinicopathologic insights into molecular subtypes. Eur Urol 2015;68:555–567.
Grupp K, Diebel F, Sirma H et al. SPINK1 expression is tightly linked to 6q15- and 5q21-deleted ERG-fusion negative prostate cancers but unrelated to PSA recurrence. Prostate 2013;73:1690–1698.
Brooks JD, Wei W, Hawley S et al. Evaluation of ERG and SPINK1 by immunohistochemical staining and clinicopathological outcomes in a multi-institutional radical prostatectomy cohort of 1067 patients. PLoS One 2015;10:e0132343.
Barbieri CE, Tomlins SA . The prostate cancer genome: perspectives and potential. Urol Oncol 2014;32:53.
Blattner M, Lee DJ, O'Reilly C et al. SPOP mutations in prostate cancer across demographically diverse patient cohorts. Neoplasia 2014;16:14–20.
Flavin RJ, Pettersson A, Hendrickson WK et al. SPINK1 protein expression and prostate cancer progression. Clin Cancer Res 2014;20:4904–4911.
Epstein JI, Netto GJ . Biopsy Interpretation of the Prostate 4th (edn). Wolters Kluwer Health/Lippincott Williams & Wilkins: Philadelphia, 2008, x 358 pp.
Arias-Stella JA 3rd, Varma KR, Montoya-Cerrillo D et al. Does discontinuous involvement of a prostatic needle biopsy core by adenocarcinoma correlate with a large tumor focus at radical prostatectomy? Am J Surg Pathol 2015;39:281–286.
Acknowledgements
This work was supported in part by the Department of Defense PC130652 (to SAT) and the Early Detection Research Network 5U01 CA11275-07 (MAR and JMM) and by the Translational Research Program at WCMC Pathology and Laboratory Medicine. SAT and NP were supported by University of Michigan Prostate SPORE (P50 CA186786) Career Development Awards. SAT is supported by the A Alfred Taubman Medical Research Institute (no grant number).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The University of Michigan has been issued a patent on ETS gene fusions in prostate on which RM, MAR and SAT are co-inventors, and has applied for a patent on SPINK1 in prostate cancer. The diagnostic field of use has been licensed to Hologic/Gen-Probe, Inc., which has sublicensed rights to Ventana Medical Systems, Inc. SAT and NP have consulted for, and received honoraria from Ventana Medical Systems. JMM and MAR have had a sponsored research agreement with Ventana Medical Systems, Inc. The ERG/SPINK1 antibodies used herein were provided by Ventana Medical Systems, Inc. SAT has consulted for Astellas/Medivation and Janssen.
Additional information
Presented at the 103rd Annual Meeting of the United States and Canadian Academy of Pathology in San Diego, CA, USA, March 2014.
Supplementary Information accompanies the paper on Modern Pathology website
Supplementary information
Rights and permissions
About this article
Cite this article
Fontugne, J., Davis, K., Palanisamy, N. et al. Clonal evaluation of prostate cancer foci in biopsies with discontinuous tumor involvement by dual ERG/SPINK1 immunohistochemistry. Mod Pathol 29, 157–165 (2016). https://doi.org/10.1038/modpathol.2015.148
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/modpathol.2015.148
This article is cited by
-
Genomic and phenotypic heterogeneity in prostate cancer
Nature Reviews Urology (2021)
-
Standardization of reporting discontinuous tumor involvement in prostatic needle biopsy: a systematic review
Virchows Archiv (2021)
-
Targetable gene fusions and aberrations in genitourinary oncology
Nature Reviews Urology (2020)