Abstract
The ultimate goal for vaccination is to stimulate protective immunological memory. Protection against infectious diseases not only relies on the magnitude of the humoral immune response, but more importantly on the quality and longevity of it. Adjuvants are critical components of most non-living vaccines. Although little attention has been given to qualitative aspects of the choice of vaccine adjuvant, emerging data demonstrate that this function may be central to vaccine efficacy. In this review we describe efforts to understand more about how adjuvants influence qualitative aspects of memory development. We describe recent advances in understanding how vaccines induce long-lived plasma and memory B cells, and focus our presentation on the germinal center reaction. As mucosal vaccination requires powerful adjuvants, we have devoted much attention to the adenosine diphosphate (ADP)-ribosylating cholera toxin and the CTA1-DD adjuvants as examples of how mucosal adjuvants can influence induction of long-term memory.
Similar content being viewed by others
Introduction
Memory is a hallmark of the adaptive immune system and results in faster, larger, and qualitatively better secondary responses compared with those seen in a primary response.1 All vaccines that induce lifelong memory are live attenuated viruses such as the measles, mumps, polio, rubella, yellow fever, and vaccinia virus vaccines.2 In contrast, no non-living vaccine, composed of whole cell or subcomponent proteins of pathogens, has been developed that also stimulates lifelong memory and protection against infection. Why is that? The answer may rest with the type of adjuvant critically required for these vaccines. Today, a very limited selection of adjuvants are used for commercial vaccine development and none of them have been evaluated from the point of view of how effective they are at promoting long-term B- and T-cell memory. Only few adjuvants have been approved for human use.3, 4 Of these, aluminum salts are by far the most commonly used, but more modern oil-in-water emulsions, such as MF59, are now being used in vaccines.5 For example, it was recently reported that an influenza vaccine containing MF59 efficiently primed memory B cells, suggesting that the choice of adjuvant critically influenced the longevity and the character of the response.6 The latter refers to that the adjuvant appeared to increase the cross-protective effect of the vaccine against different influenza strains, including seasonal- and H1N1 swine flu.7 Another recent example is the use of adjuvant to boost the effect of a formalin-inactivated respiratory syncytial virus vaccine, demonstrating that an adequate adjuvant greatly enhanced antibody affinity, thereby stimulating protective immunity in a vaccine that was thought to be very poor.8
Although live attenuated vaccines, which replicate in the host, stimulate the natural innate and adaptive immune responses, the non-living vaccine with its adjuvant component is designed to mimic these natural events. But, we do not have a clear understanding of the multitude of processes/events that initiate, maintain, and regulate natural long-term memory development. Recent attempts at taking a systems biology approach to understand the impact on innate immunity of the yellow fever attenuated vaccine YF-17D have provided promising and intriguing results that may be associated with long-term memory development.9 Little information is available on adjuvant effects and memory development in general and even less is known about mucosal adjuvant effects and memory responses.10, 11 Nevertheless, in this review we will discuss what is known about mucosal adjuvants and B-cell memory development. In particular, we will present recent data on the effect of enterotoxin-derived adjuvants and memory development, thereby hoping to inspire new interest in this quite neglected field of research. The bacterial enterotoxins elaborated by Vibrio cholerae (cholera toxin (CT)) and the closely related heat-labile toxin (LT) from Escherichia coli bacteria have been extensively studied and they exert exceptional adjuvant effects on both mucosal and systemic immune responses.12 Both toxins can be administered via mucosal or systemic routes and both dramatically augment a wide range of immune responses from antibody production to cytotoxic CD8 T-cell or CD4 T effector cell immunity.11 The protein–chemical structures are well known for these toxins and the unique adenosine diphosphate (ADP)-ribosylating ability is also well studied, although we still lack a detailed understanding of which cells and molecular events are involved in their adjuvant function.13
The Germinal Center (GC) Reaction Is Centralto Memory Development
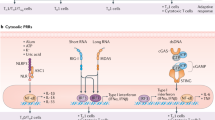
The formation of GCs during immune responses have a crucial role in both the development of high-affinity class-switched antibodies and formation of B-cell memory.14 Common also to other adjuvants, a particular feature of CT is its potent ability to stimulate large and enhanced numbers of GCs following immunizations (Figure 1). As the GC reaction progresses, class-switch recombination (CSR) and somatic hypermutations (SHMs) of the B-cell receptor (BCR) generates relatively higher-affinity variants from which memory B cells are selected.15 Following antigen (Ag) recognition, B cells will form GCs in the follicle together with follicular dendritic cells (FDCs), which are key elements in the reaction.16 B cells expand in the dark zone as centroblasts and later undergo positive selection in the light zone as centrocytes, interacting with Ag presented as immune complexes on the FDCs.17 There are a number of well-defined factors that are required for the GC reaction and selection of high-affinity memory B cells, including the presence of follicular helper CD4+ T cells (TFH).18 Whereas cognate recognition involving CD40–CD40L interaction is critical, receptors such as inducible co-stimulator (ICOS), CD28, CD80/CD86, and others are also needed for GCs to develop.19 Both humans and mice lacking CD40–CD40L interactions develop hyper-IgM syndrome, characterized by high levels of IgM but little switched antibodies in serum, no GC formation, and no T-dependent antigen responses. CD40 and CD40L interactions occur at the border between the B- and T-cell areas, where these cells meet after antigen-specific activation. This interaction could also promote GC maintenance, as blockade of CD40 appeared to disrupt established GCs.20 Moreover, earlier experiments suggested that signaling through CD40L was required for T-cell engagement in the GCs, as rudimentary GCs would form in response to anti-CD40L antibodies in CD40−/− mice.19, 21 Thus, CD40–CD40L signals appear critical for both B- and T-cell entry into GCs and in this way are critical for maintaining the GC reaction. Interestingly, human hyper-IgM patients with dysfunctional CD40–CD40L interactions have no class-switched memory cells but they maintain a population of IgM+CD27+-expressing cells with hypermutated V regions.22 It has been debated if these cells represent a bona fide memory cell population,23, 24 similar to IgM-expressing memory cells in mice,25 or if they rather represent a population of pre-diversified B cells through SHM, in analogy with the situation in sheep.26
Adenosine diphosphate (ADP)-ribosylating cholera toxin (CT) adjuvant strongly promotes germinal center (GC) formation and rapid CD86 upregulation. Mice were immunized intraperitoneally with nitrophenyl conjugated chicken gamma globulin (NP-CGG) and adjuvant and 10 days later GCs (GL7 fluorescein isothiocyanate (FITC); green) were detected in frozen sections of spleen (upper panels). Both CT and CTA1-DD adjuvants strongly promoted GC formation (middle panels), whereas the enzymatically inactive mutant CTA1R7K-DD did not (right panel). CT-ovalbumin (OVA) conjugates effectively stimulated CD86 (anti-CD86 phycoerythrin (PE); red) expression in CD11c+ dendritic cells (DCs) detectable in the T-cell zone (anti-CD3 FITC; green) of the spleen at 24 h following injection (right panel) of OVA-TCR transgenic DO.11.10 mice.
Gut Mucosal Immune Responses and GCs
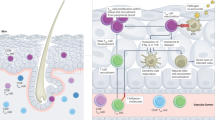
The constitutive GC formation that is observed in Peyer's patches (PP), and to a lesser extent in mesenteric lymph nodes, in mice and tonsils in humans may be driven through other signals than those critically important for GC reactions at systemic organized lymphoid tissues. This is suggested by the fact that GCs in the gut-associated lymphoid tissues (GALT) can form independently of BCR antigen signals.27 With this background, we analyzed what role CD40 signals may have in IgA B-cell differentiation and GC formation in the GALT and nonorganized lymphoid tissues of the lamina propria (LP). Unexpectedly, we found that CD40-deficient mice produced almost normal levels of total IgA in the complete absence of GCs in the GALT, including PP.28 This remarkable finding has also been confirmed in humans with hyper-IgM syndrome.29 However, contrary to these authors, we observed no evidence of IgA CSR in the gut LP. As T cell-dependent responses cannot be elicited by oral immunizations in CD40−/− mice, the IgA in the LP represented T-independent antigen responses. The IgA CSR was localized to the PP and found in B cells expressing intermediate levels of GL7, which were not detected in manifest GCs (Figure 2). We found that these cells had not acquired mutations, indicating that SHM and affinity maturation occurred only in fully mature GCs in the presence of CD40–CD40L cognate interactions. The GL7-intermediate (GL7int) B cells were found in both CD40−/− and wild-type mice, suggesting that IgA CSR normally precedes SHM. The latter required manifest GC reactions and could only be seen with GL7high cells.30 Thus, these GL7int B cells in the PP could undergo IgA CSR outside of GCs in both CD40-deficient and wild-type mice. In contrast, no evidence of IgA CSR was observed in the gut LP, using a panel of molecular markers for IgA CSR. This included a sensitive quantitative reverse transcriptase-PCR for detection of α-germline transcripts and activation-induced deaminase mRNA and a semi-quantitative PCR for the detection of switch α-CT molecular markers. Indeed, in wild-type mice after oral immunization with the 4-hydroxy-3-nitrophenyl (NP)-hapten bound to CT adjuvant (NP-CT), affinity-matured NP-specific IgA+ B cells were detected in the PP before they were observed in the mesenteric lymph nodes and gut LP, confirming that mucosal B-cell responses undergo selection processes and acquire SHMs before seeding the gut LP (M. Bemark et al., unpublished observation). Taken together, these data suggest a model where GCs in the GALT function differently from GCs at systemic lymphoid tissues. In the absence of CD40–CD40L interactions, systemic lymphoid tissues produce extrafollicular IgM, but do not support CSR, whereas the GALT, indeed, supports IgA CSR in PP B cells at a GL7int stage, that is, before manifest GC formations (Figure 3). The reason for this diverse activity could be local production of sufficient levels of BAFF (B cell-activating factor of the tumor necrosis factor) and APRIL (a proliferation-inducing ligand), known to promote CSR in the PP, whereas the levels of these factors may be too low at systemic secondary lymphoid tissues.30, 31, 32
Class switch recombination to T-independent antigens occurs in the absence of germinal centers (GCs) in the Peyer's patches (PP) of CD40-deficient mice. In wild-type (WT) mice, PP in the small intestine have large GCs that stain with GL7 fluorescein isothiocyanate (FITC; green) irrespective of whether the mice have been immunized or not (upper left). In CD40−/− mice, no GCs can be detected in the PP (upper right). Despite this, they demonstrate close to normal numbers of IgA (anti-IgA FITC; green) plasma cells in the gut lamina propria (LP). Of note, very few IgM (anti-IgM phycoerythrin (PE); red) cells are visible in the frozen section of small intestinal LP and a majority of these are found in small isolated lymphoid follicles (ILFs).
A schematic diagram depicting immunoglobulin heavy chain class switching in mucosal and systemic secondary lymphoid tissues. T-independent antigens stimulate the production of IgM antibodies during systemic responses, whereas T-independent activation induces CD40-independent IgA class switch recombination in gut-associated lymphoid tissues (GALT). Many of these IgA-switched cells subsequently enter into germinal centers (GCs) in a CD40-dependent manner, where they go through somatic hypermutation before seeding the intestine. Thus, although IgA-producing cells in the gut of CD40-deficient mice are unmutated, essentially all carry mutations in wild-type (WT) mice. It appears that a similar scenario is true during T-dependent responses in GALT in WT mice, as molecular markers for IgA class switch recombination are largely restricted to pre-germinal center cells expressing low levels of activation-induced deaminase (AID). CSR, class-switch recombination; SHM, somatic hypermutation; TCR, T cell receptor; TLR, Toll-like receptor.
Memory B-Cell Selection Occurs in the GC
It is thought that the selection of B cells is achieved by high-affinity binding of their BCR to Ag complexes on FDCs, which is dependent on the presence of complement receptors 1 and 2 (CR1/2) on the FDCs.33 Noteworthy is that CR1/2 appear not only to be required by the FDCs, as CR1/2 on the B cells facilitate their migration into and survival in the GCs.34 Recently, the TFH cells were added to the list of regulators of the selection process by providing competition for cytokines in the GCs.35 These are CD4+ T cells that express CXCR5 (C-X-C chemokine receptor type 5), which endows them with an ability to reposition in GCs. This localization of TFH cells to the GCs depended on ICOS ligand (ICOS-L) expressed on the B cells.36 It was found that GC B cell–TFH cell conjugates could be isolated and different cytokine secretion patterns correlated closely with CSR and SHM patterns in the B cells, which suggested a critical decision-making role of the TFH in the development of a memory B cell and plasma cell repertoire following immunization.35 Hence, competition for both FDC Ag complexes and TFH cytokines will influence B-cell differentiation and control the exit of plasma cells and memory B cells from the GCs. Moreover, enhanced survival rather than increased proliferation of high-affinity BCR-carrying cells has been found to be important for the selection process in the GCs; such effects could be achieved through the BCR, CD40L, ICOS, or other, presently unknown, factors.37 The production of interleukin-21 (IL-21) from TFH cells in the GCs and in ICOS-dependent helper CD4+ T cells at extrafollicular sites have been found essential for their function in CSR and IgG production.38, 39, 40 Clearly, adjuvants may strongly affect these processes, but relatively little is known at present.4
Most adjuvants act on antigen-presenting cells (APCs) by directly or indirectly augmenting their function, thereby enhancing their T-cell priming effects.11 In particular, potentiating and influencing the CD4+ T-cell response has been found critical. However, direct adjuvant effects on B and T cells cannot be excluded, but we lack evidence for that at present. Furthermore, the relative role of B cells as APCs for the generation of memory CD4+ T cells is much debated.41 A recent study demonstrated that B cells were critical in the contraction phase to generate CD4+, but not CD8+, memory T cells, an effect that was independent of antigen–antibody complexes.42 Such a role would provide B-cell acting adjuvants with special memory-modulating features as will be discussed later. Thus, a better understanding of these processes awaits to be gained as they are critical to adjuvant development and the rational design of future vaccines. However, already today some interesting aspects on adjuvants and the GC B-cell selection processes can be made.
Vaccines and Memory Development
Live attenuated vaccines stimulate lifelong memory that can be detected as protective serum antibody levels and maintained over ⩾50 years in a majority of vaccinated people.43, 44 Also, cell-mediated immunity was maintained in smallpox-immunized people for decades and, interestingly, booster doses did not change the increased frequencies of T- and B-cell memory.44 This is a remarkable finding and may serve as a hallmark of what a successful vaccine adjuvant should achieve. Whether this is a realistic goal or not cannot be answered at present. However, by studying the parameters of lifelong memory following vaccination with live attenuated vaccines, we may succeed in designing future vaccine adjuvants that promote such memory, also when using non-living vaccines. A major break-through in our knowledge about adjuvants would be if we could predict the impact on long-term memory development already at an early stage of an immune response. Efforts to establish the early impact of live attenuated vaccines on innate immunity using a systems biology approach have given support for this strategy.45, 46 These authors found that the yellow fever YF-17D vaccine targeted several Toll-like receptors and distinct subsets of DCs, which could explain why this vaccine effectively stimulated long-term memory. The early events in the priming and differentiation of CD4 T cells is another key factor in understanding memory development and long-term persistence of protective antibodies.6 Furthermore, identifying the major tissues for detection of the specific memory T and B cells would add to the features that could be used to describe different adjuvants. There is ample evidence in the literature that long-term plasma cells, but not memory B cells, reside in the bone marrow (BM), whereas memory B cells have primarily been located in the spleen in both mice and humans.47
A controversial question at present is whether memory B cells contribute to renewing the pool of long-term plasma cells in the BM or whether these populations function independently following vaccination.48, 49, 50 On the other hand, ample evidence indicate that memory B cells rapidly react to re-challenge with antigen, such that protection against infection is achieved. For example, using a mouse model for aluminum hydroxide adsorbed anthrax vaccine (AVA), specific serum antibody titers rose tenfold, from below protective levels to well above protective levels, within 3 days in mice primed 18 months earlier with AVA plus CpG-oligodeoxynucleotide (ODN) adjuvant. This was not seen in mice primed with AVA alone, clearly demonstrating the critical role of the CpG-ODN adjuvant for long-lived memory B-cell development.51 Serum IgG titers were kept at a protective level for 12 months in all mice given AVA+CpG-ODN, whereas mice given AVA alone had completely lost their anti-AVA IgG antibodies in serum. Thus, in this model the combination of plasma cells in the BM, failing to maintain protective serum antibody levels for >12 months, was complemented by rapidly responding high-affinity memory B cells. Hence, from this and other studies it is apparent that the adjuvant choice, in this case aluminum with or without CpG-ODN, could critically influence affinity maturation, presence of plasma cells in the BM, and development of AVA-specific memory B cells.
Adjuvants and Long-Term Memory Development
The terminology adjuvare is Latin and means “to help,” which is exactly what the adjuvants are doing. In most vaccines based on non-living material, there is insufficient ability to stimulate a significant immune response. This has led to a growing interest in adjuvant development. Over the last decade, our knowledge about different substances that exert adjuvant effects has grown immensely.11 Despite this, we must conclude that little information is available as to what adjuvants, in fact, do in vivo. The choice of adjuvant to be used is often as critical as which Ag or combination of Ag to include in a vaccine. All types of immune responses can be augmented, antibody formation as well as cell-mediated immunity, including cytotoxic T-cell activity. Adjuvants may use many different mechanisms to exert an augmenting effect on immune responses—from establishing an antigen depot in the tissue to direct or indirect immunomodulation and antigen-targeting effects. A more prominent theme of several studies today ascribe activation of the PYD-containing proteins inflammasome a critical function in many adjuvant formulations, as has been reported for Alum, probably through the release of uric acid.52 The linking of innate responses to the induction of adaptive immunity is the key to understanding how to construct effective adjuvants. Because of a more detailed understanding of how to trigger innate immunity, through specific receptor recognition, adjuvant research is increasingly focused on targeting the innate immune system. Targeting is also a way to restrict side effects, to reduce the dose of antigen, and to limit the risk of adverse reactions to vaccination. An adjuvant strategy that involves the specific delivery of an activation signal through a pattern recognition receptor in a given set of cells provides a unique opportunity to tailor the next generation of vaccine adjuvants with predicted action. DCs are considered the key APCs for priming of naive T cells.53, 54 That this is also the case at mucosal membranes has recently been documented by Fahlen-Yrlid et al.55 who demonstrated that intranasal or oral immunization with CT lost the priming ability in DC-depleted mice.
Immature DCs residing in tissues are known to take up Ag and, if maturation occurs, migrate to regional lymph nodes or the spleen.56, 57 In the secondary lymphoid tissues, the DC immigrants, expressing strong co-stimulation, may be inherently stimulatory. In fact, maturation results in phenotypic changes of the DCs, including increased production of major histocompatibility complex–peptide complexes, increased co-stimulation (CD40, CD80, CD86, notch ligands), and chemokines and/or cytokines production, such as IL-12 and type I interferons.58 The outcome of antigen presentation by the DCs is, thus, a function of the level of maturation; less mature DCs will more likely result in tolerance, whereas fully mature DCs will prime strong T-cell immunity. Attenuated live vaccines are known to activate multiple pathways that include Toll-like receptors, C-type lectin receptors, RIG-1-like receptors, and NOD-like receptors.59 These pattern recognition receptors are also differently expressed on a wide range of immune and non-immune cells, making the pattern for mimicking with adjuvant effects exceedingly complex. However, recent attempts to develop chip analysis of gene expression in innate immunity for vaccine adjuvant development may have a strong impact on future adjuvant design.9 Moreover, the relative difficulty in targeting DCs in vivo has limited our knowledge about the priming events that determine whether Ag stimulation will result in a tolerogenic or an immunogenic outcome.60 However, recent progress in this field has shown that antigen conjugated to DC-specific antibodies, such as monoclonal antibodies recognizing DEC205, 33D1, or CD11c, may be used to effectively target DCs, and it has been found to augment priming of T cells at least 100-fold more effective than antigen alone.61, 62 These conjugates had to be delivered together with a maturation signal, such as anti-CD40, to be adjuvant active, whereas in the absence of such stimulation, antigen-specific tolerance developed.56 In fact, different DC subsets express different membrane molecules and it appears, for example, that 33D1-antibody targeting gave better CD4 than CD8 T-cell priming and anti-DEC205 gave the opposite result.63, 64
The activation of naive CD4+ T cells can lead to the development of either Th1, Th2, Th17, TFH, or Treg cells, characterized by distinct transcription factors, cytokine production, and cell membrane phenotypes.65, 66 For example, modulation of the induction of TFH or Treg may, therefore, prove to be a promising avenue in search for future vaccine adjuvants.67 But, at present, few adjuvant strategies have included modulation of these CD4 T-cell subsets as a means to achieve long-term protective immunity.68, 69 Taken together, the identification of ways to modulate Th1, Th2 Th17, TFH, or Treg will most certainly be key to the successful development of novel vaccine adjuvants.
The ADP-Ribosylating Family of Bacterial Toxin Adjuvants
CT and LT are perhaps the best studied and most effective experimental adjuvants known today, but unfortunately they are also very toxic.70 There is a vast literature on their structure and function.71 They consist of an AB5 complex with the ADP-ribosyltransferase active A1 linked to a pentamer of B-subunits via the A2 fragment.72 The B-subunit of CT is responsible for binding to the GM1 receptor, a glycosphingolipid found ubiquitously on membranes of most mammalian cells. Several studies have shown that ADP-ribosyltransferase activity is required for optimal adjuvanticity, and that binding to cells of the immune system is mediated via the B-subunit.73, 74, 75 The mechanism of adjuvanticity of the ADP-ribosylating toxins has been the subject of considerable debate, although most investigators agree that both elements, binding and enzymatic activity, can contribute to immunomodulation. There is ample evidence in the literature to support this notion, and in particular studies with the closely related LT and derivatives thereof have documented this point. However, the ADP-ribosyltransferase activity appears to be key to an optimal immunoenhancing effect.76 Notwithstanding this, an alternative strategy to lowering the toxicity is to produce mutants of CT or LT holotoxins, which host no to minute enzymatic activity, but have retained substantial adjuvant function.77 These single-amino acid mutations, most frequently used, are located in the A1-subunit and, although dramatically less toxic, they have been found to retain substantial adjuvant function. The best mutants reported with adjuvant activity are LTK63, LTR72, CT112, and LT196.76, 78, 79 The latter mutation, which contrary to the other mutations does not involve the NAD-binding active site of A1, has recently been complemented by a second mutation in position 211 of the LTA1, rendering the double mutant trypsin resistant. Thus, the double mutant LT has proven effective even following oral administration and will be evaluated for clinical efficacy.78, 80
The adjuvant effects of the CT or LT are thought to involve the modulation of APCs, but it is poorly understood which APCs are functionally targeted by the holotoxins or derivatives thereof. All nucleated cells, including APCs, can bind the toxins via the GM1 ganglioside receptor present in the cell membrane. Previous reports have documented both pro- and anti-inflammatory effects of CT. From several studies, including our own work, it has been demonstrated that CT exposure of APCs has an augmenting effect on IL-1 and IL-6 production, whereas in other studies a downregulating effect on IL-12 and tumor necrosis factor-α, and a promoting effect on IL-10 production, have been reported.81, 82, 83, 84, 85, 86 Taken together, these effects would indicate both a pro-and anti-inflammatory function of CT on innate immunity. In an attempt to reconcile these conflicting observations that we recently found, using gene profiling by Affymetrix technology (Santa Clara, CA), CT-exposed B cells upregulated the expression of the STAT3 (signal transducer and activator of transcription 3) gene.87 This resulted in a higher sensitivity to IL-10 signaling, leading to augmented anti-inflammatory effects of IL-10, whereas IL-6 production was enhanced in CT-exposed B cells, promoting inflammatory processes. These findings may help explain the seemingly contradictory effects of CT on the innate immune system. Also, DCs have been found to be sensitive to STAT3 gene expression, as specific targeting of this gene revealed a negative regulatory function in DCs.88 Moreover, although CT adjuvant has been used to generate Th1-dominated responses, most reports have shown a bias for Th2 cells, and IL-10-producing regulatory Tr-1 cells were also reported to be increased after administration of CT.83, 89 Kelsall's group90 recently reported that CT strongly inhibited the function of the interferon regulatory factor 8 in CD8α+ DCs and in this way could inhibit the differentiation of Th1 cells in response to a Toxoplasma gondii infection, as pathway signaling of this regulatory factor is essential for IL-12 production. However, the strength of CT as an adjuvant is likely not explained by this type of blocking effect, and it should be pointed out that for other antigens CT adjuvant can effectively promote Th1-dominated responses as well as the fact that it exerts unimpaired adjuvant function in IL-12p40−/− mice.91, 92, 93 Yet, another study has documented the involvement of the nuclear factor-κB pathway in CT-targeted APCs, further suggesting effects on gene transcription associated with inflammatory responses.73 Whether nuclear factor-κB activation is also a prerequisite for an adjuvant effect was not investigated.
We believe that an important strategy to learn more about the adjuvant mechanisms of the holotoxins and their mutant derivatives is to follow in vivo deposition of the adjuvants in the tissues following immunizations. We have used ovalbumin (OVA)-conjugated CT to study the deposition of the adjuvant in vivo.94 We found that after intravenous injections most of the OVA accumulated in the marginal zone of the spleen. No OVA could be detected in this zone when unconjugated OVA was used, even when very high doses were injected. We could also conclude that the deposition of CT-OVA was facilitated by GM1 ganglioside receptor binding, because a non-binding mutant toxin conjugate failed to deposit in the marginal zone. Ag concentrations in the targeted cells were very high and appeared to form a depot of OVA in the marginal zone for up to 48 h after injection. Already after 24 h, the concentration of OVA was reduced in the marginal zone, which coincided with the appearance of OVA-containing DCs in the T-cell zone. These DCs were high expressors of CD86, but not CD80, and appeared to provide enhanced APC function, as peptide-specific T cells greatly expanded in response to the CT-OVA conjugate (Figure 1). The observation of an improved co-stimulation, especially CD86 upregulation, is a feature shared with LT and is also reported for some of the mutant holotoxins.94, 95, 96
CT Promotes Long-Term Memory Development
We have been interested in memory development after oral immunization using CT adjuvant for many years and have published several studies on this topic in the 1980s and 1990s.97, 98, 99, 100, 101, 102 We reported on the longevity of antitoxin IgA responses in the gut intestinal LP following repeated oral immunizations with antigen and CT adjuvant. Not only were antitoxin IgA plasma cells present in the gut LP for >6 months after the oral immunization, but upon a re-challenge with CT, even after 24 months, a vigorous antitoxin IgA antibody response was observed in the gut LP, detectable within 24–48 h after the challenge (Figure 4). Antigen-specific memory B cells could be isolated from the spleen or mesenteric lymph nodes after 12 months and adoptively transferred to naive syngeneic recipient mice, which were subsequently challenged by oral CT. This elicited a strong recall IgA response in the gut LP, clearly demonstrating the presence of functional memory B cells in orally immunized mice.99 Adoptive transfer of a gut antitoxin IgA response was completely disrupted by deleting the B cells before transfer. Thus, memory B cells following oral immunizations with CT adjuvant reside in systemic tissues as well as in the GALT (Figure 4). Interestingly, although specific antibodies of all classes were recorded in serum after 1 month following oral priming immunizations, only IgM antibodies were specific after 1 year, suggesting that long-lived IgM plasma cells resided in the BM.101 The study also indicated that not all retained B cells following oral immunizations have undergone CSR to the downstream isotypes IgG and IgA. Rather, it appeared that IgM+ plasma cells were more persistent in the BM than the IgA plasma cells. Furthermore, the notion that not all memory B cells undergo CSR, but retain IgM expression, while accumulating SHMs and increased affinity maturation, is supported by a recent study by Dogan et al.,25 who investigated memory B cells following intraperitoneal immunizations with sheep red blood cells. These authors found that specific IgM+ memory B cells dominated the response for longer than IgG+ memory B cells. However, presently we lack definite proof for the existence of mutated IgM+ memory B cells after oral immunization with CT or any other adjuvant.103 It would appear, though, quite functional if memory IgM+ B cells could rapidly undergo CSR, either at an extrafollicular site or rather through re-entering a GC, and in this way ensure the ability to respond with IgA or IgG antibodies, whatever is most appropriate for protection. Re-entering of B cells into dynamic open GC has, in fact, recently been demonstrated.104 This would allow rapid mobilization of a protective response of appropriate quality and magnitude with IgA in the gut LP and IgG in serum.
Cholera toxin (CT) promotes the development of long-term memory B cells following oral immunizations. Mice were primed perorally three times with 10 days apart with 10 μg of CT, and at indicated intervals anti-CT-forming cells were analyzed in single cell suspensions of mononuclear cells isolated from the lamina propria of the small intestines from mice receiving no (blue bars) or a single oral booster immunization with CT (red) 8–10 days before analysis (left panel). Following oral priming immunizations with CT as described above, we waited 1 year before we adoptively transferred 2.5 × 106 B (red bars) or T (blue) cells from the mesenteric lymph nodes or B cells from the spleen (green bars) and challenged the recipients by an oral dose of CT and analyzed the response in various tissues (right panel). We found that CT adjuvant clearly promoted long-term memory B-cell development after oral immunizations. AFC, antibody-forming cell; LP, lamina propria; MLN, mesenteric lymph node; ND, not detected.
These previous observations using CT adjuvant raises a number of questions with regard to memory development following oral immunizations. Based on the results discussed above, the presence of long-lived plasma cells and memory B cells following oral immunization is an indisputable fact. But, presently we lack information about where these cells are generated or where they reside during long periods of time.105 Second, the question of whether SHMs are introduced to secure affinity maturation in specific IgA responses and whether all memory B cells undergo IgA CSR or whether they may also express IgG or IgM has not been adequately analyzed. A central event for memory development is the GC reaction. Unfortunately, no information is available on de novo formation of GCs following oral immunizations, probably because the PP, and to some extent the mesenteric lymph nodes, constantly host GCs as a consequence of luminal antigens in the form of bacterial flora and food antigens.28 This has made simple direct observations of the impact of oral immunization on GC formation in the GALT difficult. However, we have demonstrated that CT is particularly effective at stimulating large GC reactions in the spleen when given intraperitoneally or intravenously.106 Future studies will focus on the impact of toxin-based adjuvants on long-lived plasma and memory B-cell development.
The Non-Toxic CTA1-DD Adjuvant and Memory Development
A major limitation of the holotoxins is their promiscuous binding to the GM1 ganglioside receptors present on all nucleated cells, including epithelial cells and nerve cells, which precludes clinical use of these toxin adjuvants.107, 108 Indeed, a commercial intranasal Flu vaccine with LT as the adjuvant revealed increased incidence of cases with Bell's palsy in vaccinated subjects, and led to the withdrawal of the vaccine from the market.107, 109, 110 This uptake was dependent upon ganglioside GM1 receptor binding of the B-subunit, and all holotoxins or mutant molecules that can bind GM1 ganglioside, including the double mutant LTR196/211 or LTK63, potentially carry the risk of affecting the central nervous system following intranasal immunization.80, 111 Hence, one can anticipate that it will still be considerably difficult to separate adjuvanticity from toxicity in human vaccines because of the GM1-binding ability of these mutant holotoxins.
To eliminate the toxicity of CT, we generated a gene fusion protein, CTA1-DD, that completely lacks the cholera toxin B-subunit ganglioside-receptor binding pentamer. Instead, CTA1-DD is a fusion protein consisting of the ADP-ribosylating CTA1 subunit linked to two Ig binding D domains from Staphylococcus aureus protein A.112, 113 This way it retains the potent adjuvant function of CT, but lacks its toxic side effects and does not accumulate in the central nervous system.106, 110, 113, 114, 115, 116 Mice and monkeys have been given high doses of >200 μg of CTA1-DD without any apparent side effects or signs of reactogenicity, whereas similar doses of CT are known to be lethal to mice. It is noteworthy that humans can get overt diarrhea from doses as low as 5–10 μg of CT.108 Thus, CTA1-DD appears to be a safe and non-toxic mucosal vaccine adjuvant, although it carries equal ADP-ribosylating ability as CT holotoxin. Although CTA1-DD binds to the BCR on B cells, it still functions as an adjuvant for priming T cells in the absence of B cells, as seen in B cell- deficient mice.117 Used alone, CTA1-DD promotes a wide range of specific immune responses, augmenting antibody levels and priming CD4+ and CD8+ T cells to a large variety of antigens, including those from pathogens such as rotavirus, Helicobacter pylori, Mycobacterium tuberculosis, Chlamydia trachomatis, HIV, and influenza A virus.117, 118, 119, 120, 121, 122 It should be emphasized that the adjuvant effect is achieved simply by admixing the vaccine antigen to CTA1-DD.
Although CTA1-DD has been found to be an excellent adjuvant for intranasal, intraperitoneal, intravenous, subcutaneous, and rectal immunizations, it has failed to work for oral administration. Because of the poor oral effect, we developed a new combined vector by incorporating CTA1-DD into ISCOMS (immune-stimulating complexes).123, 124 In doing so, we achieved a more stable vaccine adjuvant that was also efficacious when given orally. The combined vector proved highly effective in mice for stimulating, for example, tuberculosis-specific protective immunity in the lung using Ag85B-ESAT-6 mixed with CTA1-DD/ISCOMs as adjuvant.118
The CTA1-DD molecular platform has provided us with a unique tool to uncover regulatory mechanisms that govern mucosal immune responses. Not only have we discovered unique functions of ADP-ribosylation at mucosal membranes, but we have also gained information about such fundamental aspects of vaccination as memory development or mechanism for antibacterial or antiviral protection. We have found that CTA1-DD stimulated GC formations in a dose-dependent fashion and effectively generated long-term plasma cell populations in the BM and long-lived memory B cells, primarily located to the spleen. These effects were obtained in the absence of polyclonal B-cell activation as assessed by an unaltered concentration of IgG in serum, although specific titers increased by >100-fold. Thus, the CTA1-DD adjuvant had significant effects on the GC reaction, both with regard to frequency and size, and promoted SHM and long-term high-affinity memory B-cell development. Most notably, compared with the adjuvant effects exerted by Ribi (monophosphoryl lipid A (MPL)) or Alum, CTA1-DD adjuvant promoted antigen-specific serum IgG responses that were maintained for 2–3-fold longer time (Figure 5). After 18 months, we could transfer splenic B cells to naive recipient mice and challenge these mice with antigen. Remarkably, we found that a secondary type of IgG-specific responses was elicited by a challenge immunization, clearly documenting the presence of functional memory cells after a single immunization with the CTA1-DD adjuvant. Further studies will address the mechanisms behind this memory-promoting potential of the CTA1-DD adjuvant. Furthermore, the augmenting effect on SHM and affinity maturation may partly explain why a recent report on the use of CTA1-DD together with chlamydial major outer membrane protein greatly promoted high-affinity antibacterial-neutralizing antibodies, an effect that also conferred resistance in the oviduct to the immunopathology induced by live chlamydia infection.119 Finally, because CTA1-DD can bind to the BCR on B cells, it may directly influence the activities in the GC, especially as we have found that CTA1-DD/ISCOMS accumulate in the B-cell follicle already 2 h after immunization.123 Ongoing studies will dissect these mechanisms in more detail to gain insight into why CTA1-DD appears to be a strong inducer of long-term plasma and memory B-cell responses.
Long-term serum antibody responses are retained twice as long following immunizations with CTA1-DD when compared with Alum or Ribi/monophosphoryl lipid A (MPL) adjuvants. Mice were immunized with a single priming dose intraperitoneally with nitrophenyl conjugated chicken gamma globulin together with CTA1-DD, Ribi, or Alum as adjuvants, and the decline of serum antibody titers was monitored for 25 weeks. Serum was analyzed for 4-hydroxy-3-nitrophenyl (NP)-specific IgG log10 titers by enzyme-linked immunosorbent assay (ELISA). Strikingly, CTA1-DD adjuvant preserved the highest titers and these were reduced less than twofold from 5 to 25 weeks, whereas Alum and Ribi/MPL lost more than fivefold in anti-NP IgG titers in that time.
Concluding Remarks
A major area of research should be devoted to identifying whether there exists predictive correlates of protection using different or combinations of adjuvants in defined vaccines, such that we can design vaccines that meet the demand for long-term protection against infection. For example, is the presence of a high specific serum antibody titer at 10 or 20 weeks following vaccination a good correlate of long-term protection? Is the size of GC a correlate of long-term memory and affinity maturation? Does the presence of high numbers of TFH cells reflect the induction of long-term memory? Is the generation of long-term plasma cells and memory B cells controlled by the same factors and to what extent can we identify adjuvants that promote the latter rather than the former? The list of questions can be made long, but overall we can conclude that at present we do not have the knowledge to evaluate these aspects of candidate vaccine adjuvants. However, by employing new technologies and in particular real-time two-photon microscopy, we may be able to dissect the complex network of processes that adjuvants employ to enhance immune responses following vaccination.
References
Ahmed, R. & Gray, D. Immunological memory and protective immunity: understanding their relation. Science 272, 54–60 (1996).
Amanna, I.J., Carlson, N.E. & Slifka, M.K. Duration of humoral immunity to common viral and vaccine antigens. N. Engl. J. Med. 357, 1903–1915 (2007).
Lambrecht, B.N., Kool, M., Willart, M.A. & Hammad, H. Mechanism of action of clinically approved adjuvants. Curr. Opin. Immunol. 21, 23–29 (2009).
Tagliabue, A. & Rappuoli, R. Vaccine adjuvants: the dream becomes real. Hum. Vaccin. 4, 347–349 (2008).
Kenney, R.T. & Cross, A.S. Adjuvants for the future. In New Generation Vaccines, 4th edn. (Levine, M.M., ed) 250–262 ( Informa Healthcare USA, New York, NY, 2010 ).
Galli, G. et al. Fast rise of broadly cross-reactive antibodies after boosting long-lived human memory B cells primed by an MF59 adjuvanted prepandemic vaccine. Proc. Natl. Acad. Sci. USA 106, 7962–7967 (2009).
Castellino, F., Galli, G., Del Giudice, G. & Rappuoli, R. Generating memory with vaccination. Eur. J. Immunol. 39, 2100–2105 (2009).
Delgado, M.F. et al. Lack of antibody affinity maturation due to poor Toll-like receptor stimulation leads to enhanced respiratory syncytial virus disease. Nat. Med. 15, 34–41 (2009).
Pulendran, B. Learning immunology from the yellow fever vaccine: innate immunity to systems vaccinology. Nat. Rev. Immunol. 9, 741–747 (2009).
Harandi, A.M. & Medaglini, D. Mucosal Adjuvants. Curr. HIV Res 8, 330–335 (2010).
Lycke, N. Mechanisms of adjuvant action. In Vaccine Adjuvants and Delivery Systems. (Singh, M., ed) 53–79 ( Wiley, Hoboken, NJ, 2007 ).
Freytag, L.C., Clements, J.D., Grdic Eliasson, D. & Lycke, N. Use of genetically or chemically detoxified mutants of cholera and Escherichia coli heat-labile enterotoxins as mucosal adjuvants. In New Generation Vaccines, 4th edn. (Levine, M.M., ed) 273–283 ( Informa Healthcare USA, New York, NY, 2010 ).
O'neal, C.J., Amaya, E.I., Jobling, M.G., Holmes, R.K. & Hol, W.G. Crystal structures of an intrinsically active cholera toxin mutant yield insight into the toxin activation mechanism. Biochemistry 43, 3772–3782 (2004).
Tangye, S.G. & Tarlinton, D.M. Memory B cells: effectors of long-lived immune responses. Eur. J. Immunol. 39, 2065–2075 (2009).
Berek, C., Berger, A. & Apel, M. Maturation of the immune response in germinal centers. Cell 67, 1121–1129 (1991).
Schwickert, T.A. et al. In vivo imaging of germinal centres reveals a dynamic open structure. Nature 446, 83–87 (2007).
Allen, C.D., Okada, T. & Cyster, J.G. Germinal-center organization and cellular dynamics. Immunity 27, 190–202 (2007).
Yu, D., Batten, M., Mackay, C.R. & King, C. Lineage specification and heterogeneity of T follicular helper cells. Curr. Opin. Immunol. 21, 619–625 (2009).
Vinuesa, C.G., Sanz, I. & Cook, M.C. Dysregulation of germinal centres in autoimmune disease. Nat. Rev. Immunol. 9, 845–857 (2009).
Han, S. et al. Cellular interaction in germinal centers. Roles of CD40 ligand and B7-2 in established germinal centers. J. Immunol. 155, 556–567 (1995).
Van Essen, D., Kikutani, H. & Gray, D. CD40 ligand-transduced co-stimulation of T cells in the development of helper function. Nature 378, 620–623 (1995).
Weller, S. et al. CD40-CD40L independent Ig gene hypermutation suggests a second B cell diversification pathway in humans. Proc. Natl. Acad. Sci. USA 98, 1166–1170 (2001).
Seifert, M. & Kuppers, R. Molecular footprints of a germinal center derivation of human IgM+(IgD+)CD27+ B cells and the dynamics of memory B cell generation. J. Exp. Med. 206, 2659–2669 (2009).
Tangye, S.G. & Good, K.L. Human IgM+CD27+ B cells: memory B cells or “memory” B cells? J. Immunol. 179, 13–19 (2007).
Dogan, I. et al. Multiple layers of B cell memory with different effector functions. Nat. Immunol. 10, 1292–1299 (2009).
Weller, S. et al. Somatic diversification in the absence of antigen-driven responses is the hallmark of the IgM+ IgD+ CD27+ B cell repertoire in infants. J. Exp. Med. 205, 1331–1342 (2008).
Casola, S. et al. B cell receptor signal strength determines B cell fate. Nat. Immunol. 5, 317–327 (2004).
Bergqvist, P., Gardby, E., Stensson, A., Bemark, M. & Lycke, N.Y. Gut IgA class switch recombination in the absence of CD40 does not occur in the lamina propria and is independent of germinal centers. J. Immunol. 177, 7772–7783 (2006).
He, B. et al. Intestinal bacteria trigger T cell-independent immunoglobulin A(2) class switching by inducing epithelial-cell secretion of the cytokine APRIL. Immunity 26, 812–826 (2007).
Bergqvist, P., Stensson, A., Lycke, N.Y. & Bemark, M. T cell-independent IgA class switch recombination is restricted to the GALT and occurs prior to manifest germinal center formation. J. Immunol. 184, 3545–3553 (2010).
Barone, F., Patel, P., Sanderson, J.D. & Spencer, J. Gut-associated lymphoid tissue contains the molecular machinery to support T-cell-dependent and T-cell-independent class switch recombination. Mucosal. Immunol. 2, 495–503 (2009).
Litinskiy, M.B. et al. DCs induce CD40-independent immunoglobulin class switching through BLyS and APRIL. Nat. Immunol. 3, 822–829 (2002).
Fang, Y., Xu, C., Fu, Y.X., Holers, V.M. & Molina, H. Expression of complement receptors 1 and 2 on follicular dendritic cells is necessary for the generation of a strong antigen-specific IgG response. J. Immunol. 160, 5273–5279 (1998).
Fischer, M.B. et al. Dependence of germinal center B cells on expression of CD21/CD35 for survival. Science 280, 582–585 (1998).
Reinhardt, R.L., Liang, H.E. & Locksley, R.M. Cytokine-secreting follicular T cells shape the antibody repertoire. Nat. Immunol. 10, 385–393 (2009).
Nurieva, R.I. et al. Generation of T follicular helper cells is mediated by interleukin-21 but independent of T helper 1, 2, or 17 cell lineages. Immunity 29, 138–149 (2008).
Anderson, S.M. et al. Taking advantage: high-affinity B cells in the germinal center have lower death rates, but similar rates of division, compared to low-affinity cells. J. Immunol 183, 7314–7325 (2009).
Odegard, J.M. et al. ICOS-dependent extrafollicular helper T cells elicit IgG production via IL-21 in systemic autoimmunity. J. Exp. Med. 205, 2873–2886 (2008).
Ozaki, K. et al. A critical role for IL-21 in regulating immunoglobulin production. Science 298, 1630–1634 (2002).
Vogelzang, A. et al. A fundamental role for interleukin-21 in the generation of T follicular helper cells. Immunity 29, 127–137 (2008).
Seder, R.A. & Ahmed, R. Similarities and differences in CD4+ and CD8+ effector and memory T cell generation. Nat. Immunol. 4, 835–842 (2003).
Whitmire, J.K. et al. Requirement of B cells for generating CD4+ T cell memory. J. Immunol. 182, 1868–1876 (2009).
Crotty, S. et al. Cutting edge: long-term B cell memory in humans after smallpox vaccination. J. Immunol. 171, 4969–4973 (2003).
Hammarlund, E. et al. Duration of antiviral immunity after smallpox vaccination. Nat. Med. 9, 1131–1137 (2003).
Querec, T. et al. Yellow fever vaccine YF-17D activates multiple dendritic cell subsets via TLR2, 7, 8, and 9 to stimulate polyvalent immunity. J. Exp. Med. 203, 413–424 (2006).
Querec, T.D. et al. Systems biology approach predicts immunogenicity of the yellow fever vaccine in humans. Nat. Immunol. 10, 116–125 (2009).
Mamani-Matsuda, M. et al. The human spleen is a major reservoir for long-lived vaccinia virus-specific memory B cells. Blood 111, 4653–4659 (2008).
Ahuja, A., Anderson, S.M., Khalil, A. & Shlomchik, M.J. Maintenance of the plasma cell pool is independent of memory B cells. Proc. Natl. Acad. Sci. USA 105, 4802–4807 (2008).
Bernasconi, N.L., Traggiai, E. & Lanzavecchia, A. Maintenance of serological memory by polyclonal activation of human memory B cells. Science 298, 2199–2202 (2002).
Slifka, M.K. & Ahmed, R. Long-lived plasma cells: a mechanism for maintaining persistent antibody production. Curr. Opin. Immunol. 10, 252–258 (1998).
Tross, D. & Klinman, D.M. Effect of CpG oligonucleotides on vaccine-induced B cell memory. J. Immunol. 181, 5785–5790 (2008).
Kool, M. et al. Cutting edge: alum adjuvant stimulates inflammatory dendritic cells through activation of the NALP3 inflammasome. J. Immunol. 181, 3755–3759 (2008).
Itano, A.A. & Jenkins, M.K. Antigen presentation to naive CD4 T cells in the lymph node. Nat. Immunol. 4, 733–739 (2003).
Iwasaki, A. & Medzhitov, R. Toll-like receptor control of the adaptive immune responses. Nat. Immunol. 5, 987–995 (2004).
Fahlen-Yrlid, L. et al. CD11c(high )dendritic cells are essential for activation of CD4+ T cells and generation of specific antibodies following mucosal immunization. J. Immunol. 183, 5032–5041 (2009).
Hawiger, D. et al. Dendritic cells induce peripheral T cell unresponsiveness under steady state conditions in vivo. J. Exp. Med. 194, 769–779 (2001).
Mempel, T.R., Henrickson, S.E. & Von Andrian, U.H. T-cell priming by dendritic cells in lymph nodes occurs in three distinct phases. Nature 427, 154–159 (2004).
Steinman, R.M. Dendritic cells: understanding immunogenicity. Eur. J. Immunol. 37, S53–60 (2007).
Manicassamy, S. & Pulendran, B. Modulation of adaptive immunity with Toll-like receptors. Semin. Immunol. 21, 185–193 (2009).
Pulendran, B., Banchereau, J., Maraskovsky, E. & Maliszewski, C. Modulating the immune response with dendritic cells and their growth factors. Trends. Immunol. 22, 41–47 (2001).
Bonifaz, L. et al. Efficient targeting of protein antigen to the dendritic cell receptor DEC-205 in the steady state leads to antigen presentation on major histocompatibility complex class I products and peripheral CD8+ T cell tolerance. J. Exp. Med. 196, 1627–1638 (2002).
Boscardin, S.B. et al. Antigen targeting to dendritic cells elicits long-lived T cell help for antibody responses. J. Exp. Med. 203, 599–606 (2006).
Dudziak, D. et al. Differential antigen processing by dendritic cell subsets in vivo. Science 315, 107–111 (2007).
Soares, H. et al. A subset of dendritic cells induces CD4+ T cells to produce IFN-gamma by an IL-12-independent but CD70-dependent mechanism in vivo. J. Exp. Med. 204, 1095–1106 (2007).
Lefrancois, L. Development, trafficking, and function of memory T-cell subsets. Immunol. Rev. 211, 93–103 (2006).
Sallusto, F., Mackay, C.R. & Lanzavecchia, A. The role of chemokine receptors in primary, effector, and memory immune responses. Annu. Rev. Immunol. 18, 593–620 (2000).
Bluestone, J.A. & Abbas, A.K. Natural versus adaptive regulatory T cells. Nat. Rev. Immunol. 3, 253–257 (2003).
Baecher-Allan, C. & Anderson, D.E. Immune regulation in tumor-bearing hosts. Curr. Opin. Immunol. 18, 214–219 (2006).
Berrih-Aknin, S., Fuchs, S. & Souroujon, M.C. Vaccines against myasthenia gravis. Expert Opin. Biol. Ther. 5, 983–995 (2005).
Lewis, D.J. et al. Transient facial nerve paralysis (Bell's palsy) following intranasal delivery of a genetically detoxified mutant of Escherichia coli heat labile toxin. PLoS One 4, e6999 (2009).
Fan, E. et al. Structural biology and structure-based inhibitor design of cholera toxin and heat-labile enterotoxin. Int. J. Med. Microbiol. 294, 217–223 (2004).
Holmgren, J. & Czerkinsky, C. Mucosal immunity and vaccines. Nat. Med. 11, S45–53 (2005).
Kawamura, Y.I. et al. Cholera toxin activates dendritic cells through dependence on GM1-ganglioside which is mediated by NF-kappaB translocation. Eur. J. Immunol. 33, 3205–3212 (2003).
Rappuoli, R., Pizza, M., Douce, G. & Dougan, G. Structure and mucosal adjuvanticity of cholera and Escherichia coli heat-labile enterotoxins. Immunol. Today 20, 493–500 (1999).
Soriani, M., Bailey, L. & Hirst, T.R. Contribution of the ADP-ribosylating and receptor-binding properties of cholera-like enterotoxins in modulating cytokine secretion by human intestinal epithelial cells. Microbiology 148, 667–676 (2002).
Giuliani, M.M. et al. Mucosal adjuvanticity and immunogenicity of LTR72, a novel mutant of Escherichia coli heat-labile enterotoxin with partial knockout of ADP-ribosyltransferase activity. J. Exp. Med. 187, 1123–1132 (1998).
Douce, G. et al. Mucosal immunogenicity of genetically detoxified derivatives of heat labile toxin from Escherichia coli. Vaccine 16, 1065–1073 (1998).
Dickinson, B.L. & Clements, J.D. Dissociation of Escherichia coli heat-labile enterotoxin adjuvanticity from ADP-ribosyltransferase activity. Infect. Immun. 63, 1617–1623 (1995).
Hagiwara, Y. et al. Effects of intranasal administration of cholera toxin (or Escherichia coli heat-labile enterotoxin) B subunits supplemented with a trace amount of the holotoxin on the brain. Vaccine 19, 1652–1660 (2001).
Summerton, N.A. et al. Toward the development of a stable, freeze-dried formulation of Helicobacter pylori killed whole cell vaccine adjuvanted with a novel mutant of Escherichia coli heat-labile toxin. Vaccine 28, 1404–1411 (2010).
Braun, M.C., He, J., Wu, C.Y. & Kelsall, B.L. Cholera toxin suppresses interleukin (IL)-12 production and IL-12 receptor beta1 and beta2 chain expression. J. Exp. Med. 189, 541–552 (1999).
Cong, Y., Oliver, A.O. & Elson, C.O. Effects of cholera toxin on macrophage production of co-stimulatory cytokines. Eur. J. Immunol. 31, 64–71 (2001).
Lavelle, E.C. et al. Effects of cholera toxin on innate and adaptive immunity and its application as an immunomodulatory agent. J. Leukoc. Biol. 75, 756–763 (2004).
Lavelle, E.C. et al. Cholera toxin promotes the induction of regulatory T cells specific for bystander antigens by modulating dendritic cell activation. J. Immunol. 171, 2384–2392 (2003).
Lycke, N. From toxin to adjuvant: basic mechanisms for the control of mucosal IgA immunity and tolerance. Immunol. Lett. 97, 193–198 (2005).
Williamson, E., Westrich, G.M. & Viney, J.L. Modulating dendritic cells to optimize mucosal immunization protocols. J. Immunol. 163, 3668–3675 (1999).
Sjöblom-Hallén, A. et al. Gene expression profiling identifies STAT3 as a novel pathway for immunomodulation by cholera toxin adjuvant. Mucosal. Immunol. 3, 374–386 (2010).
Melillo, J.A. et al. Dendritic cell (DC)-specific targeting reveals Stat3 as a negative regulator of DC function. J. Immunol. 184, 2638–2645 (2010).
Lycke, N. Targeted vaccine adjuvants based on modified cholera toxin. Curr. Mol. Med. 5, 591–597 (2005).
La Sala, A. et al. Cholera toxin inhibits IL-12 production and CD8alpha+ dendritic cell differentiation by cAMP-mediated inhibition of IRF8 function. J. Exp. Med. 206, 1227–1235 (2009).
Akhiani, A.A. et al. Protection against Helicobacter pylori infection following immunization is IL-12-dependent and mediated by Th1 cells. J. Immunol. 169, 6977–6984 (2002).
Grdic, D. et al. The mucosal adjuvant effects of cholera toxin and immune-stimulating complexes differ in their requirement for IL-12, indicating different pathways of action. Eur. J. Immunol. 29, 1774–1784 (1999).
Hornquist, E. & Lycke, N. Cholera toxin adjuvant greatly promotes antigen priming of T cells. Eur. J. Immunol. 23, 2136–2143 (1993).
Grdic, D. et al. Splenic marginal zone dendritic cells mediate the cholera toxin adjuvant effect: dependence on the ADP-ribosyltransferase activity of the holotoxin. J. Immunol. 175, 5192–5202 (2005).
Martin, M., Sharpe, A., Clements, J.D. & Michalek, S.M. Role of B7 costimulatory molecules in the adjuvant activity of the heat-labile enterotoxin of Escherichia coli. J. Immunol. 169, 1744–1752 (2002).
Yamamoto, M. et al. Enterotoxin adjuvants have direct effects on T cells and antigen-presenting cells that result in either interleukin-4-dependent or -independent immune responses. J. Infect. Dis. 182, 180–190 (2000).
Lycke, N. & Holmgren, J. Intestinal mucosal memory and presence of memory cells in lamina propria and Peyer's patches in mice 2 years after oral immunization with cholera toxin. Scand. J. Immunol. 23, 611–616 (1986).
Lycke, N. & Holmgren, J. Long-term cholera antitoxin memory in the gut can be triggered to antibody formation associated with protection within hours of an oral challenge immunization. Scand. J. Immunol. 25, 407–412 (1987).
Lycke, N. & Holmgren, J. Adoptive transfer of gut mucosal antitoxin memory by isolated B cells 1 year after oral immunization with cholera toxin. Infect. Immun. 57, 1137–1141 (1989).
Vajdy, M. & Lycke, N. Stimulation of antigen-specific T- and B-cell memory in local as well as systemic lymphoid tissues following oral immunization with cholera toxin adjuvant. Immunology 80, 197–203 (1993).
Vajdy, M. & Lycke, N. Mucosal memory B cells retain the ability to produce IgM antibodies 2 years after oral immunization. Immunology 86, 336–342 (1995).
Vajdy, M. & Lycke, N.Y. Cholera toxin adjuvant promotes long-term immunological memory in the gut mucosa to unrelated immunogens after oral immunization. Immunology 75, 488–492 (1992).
Soenawan, E. et al. Maintenance of long-term immunological memory by low avidity IgM-secreting cells in bone marrow after mucosal immunizations with cholera toxin adjuvant. Vaccine 22, 1553–1563 (2004).
Schwickert, T.A., Alabyev, B., Manser, T. & Nussenzweig, M.C. Germinal center reutilization by newly activated B cells. J. Exp. Med. 206, 2907–2914 (2009).
Benner, R., Hijmans, W. & Haaijman, J.J. The bone marrow: the major source of serum immunoglobulins, but still a neglected site of antibody formation. Clin. Exp. Immunol. 46, 1–8 (1981).
Agren, L.C., Ekman, L., Lowenadler, B., Nedrud, J.G. & Lycke, N.Y. Adjuvanticity of the cholera toxin A1-based gene fusion protein, CTA1-DD, is critically dependent on the ADP-ribosyltransferase and Ig-binding activity. J. Immunol. 162, 2432–2440 (1999).
Fujihashi, K., Koga, T., Van Ginkel, F.W., Hagiwara, Y. & Mcghee, J.R. A dilemma for mucosal vaccination: efficacy versus toxicity using enterotoxin-based adjuvants. Vaccine 20, 2431–2438 (2002).
Levine, M.M. et al. Evaluation in humans of attenuated Vibrio cholerae El Tor Ogawa strain Texas Star-SR as a live oral vaccine. Infect. Immun. 43, 515–522 (1984).
Glueck, R. Pre-clinical and clinical investigation of the safety of a novel adjuvant for intranasal immunization. Vaccine 20, S42–44 (2001).
Mutsch, M. et al. Use of the inactivated intranasal influenza vaccine and the risk of Bell's palsy in Switzerland. N. Engl. J. Med. 350, 896–903 (2004).
Partidos, C.D., Salani, B.F., Pizza, M. & Rappuoli, R. Heat-labile enterotoxin of Escherichia coli and its site-directed mutant LTK63 enhance the proliferative and cytotoxic T-cell responses to intranasally co-immunized synthetic peptides. Immunol. Lett. 67, 209–216 (1999).
Agren, L., Lowenadler, B. & Lycke, N. A novel concept in mucosal adjuvanticity: the CTA1-DD adjuvant is a B cell-targeted fusion protein that incorporates the enzymatically active cholera toxin A1 subunit. Immunol. Cell. Biol. 76, 280–287 (1998).
Agren, L.C., Ekman, L., Lowenadler, B. & Lycke, N.Y. Genetically engineered nontoxic vaccine adjuvant that combines B cell targeting with immunomodulation by cholera toxin A1 subunit. J. Immunol. 158, 3936–3946 (1997).
Agren, L. et al. The ADP-ribosylating CTA1-DD adjuvant enhances T cell-dependent and independent responses by direct action on B cells involving anti-apoptotic Bcl-2- and germinal center-promoting effects. J. Immunol. 164, 6276–6286 (2000).
Eriksson, A.M., Schon, K.M. & Lycke, N.Y. The cholera toxin-derived CTA1-DD vaccine adjuvant administered intranasally does not cause inflammation or accumulate in the nervous tissues. J. Immunol. 173, 3310–3319 (2004).
van Ginkel, F.W., Jackson, R.J., Yuki, Y. & Mcghee, J.R. Cutting edge: the mucosal adjuvant cholera toxin redirects vaccine proteins into olfactory tissues. J. Immunol. 165, 4778–4782 (2000).
Akhiani, A.A., Stensson, A., Schon, K. & Lycke, N. The nontoxic CTA1-DD adjuvant enhances protective immunity against Helicobacter pylori infection following mucosal immunization. Scand. J. Immunol. 63, 97–105 (2006).
Andersen, C.S. et al. The combined CTA1-DD/ISCOMs vector is an effective intranasal adjuvant for boosting prior Mycobacterium bovis BCG immunity to Mycobacterium tuberculosis. Infect. Immun. 75, 408–416 (2007).
Cunningham, K.A., Carey, A.J., Lycke, N., Timms, P. & Beagley, K.W. CTA1-DD is an effective adjuvant for targeting anti-chlamydial immunity to the murine genital mucosa. J. Reprod. Immunol. 81, 34–38 (2009).
Eliasson, D.G. et al. CTA1-M2e-DD: a novel mucosal adjuvant targeted influenza vaccine. Vaccine 26, 1243–1252 (2008).
Mcneal, M.M. et al. Intrarectal immunization of mice with VP6 and either LT(R192G) or CTA1-DD as adjuvant protects against fecal rotavirus shedding after EDIM challenge. Vaccine 25, 6224–6231 (2007).
Sundling, C. et al. CTA1-DD adjuvant promotes strong immunity against human immunodeficiency virus type 1 envelope glycoproteins following mucosal immunization. J. Gen. Virol. 89, 2954–2964 (2008).
Helgeby, A. et al. The combined CTA1-DD/ISCOM adjuvant vector promotes priming of mucosal and systemic immunity to incorporated antigens by specific targeting of B cells. J. Immunol. 176, 3697–3706 (2006).
Smith, R.E., Donachie, A.M., Grdic, D., Lycke, N. & Mowat, A.M. Immune-stimulating complexes induce an IL-12-dependent cascade of innate immune responses. J. Immunol. 162, 5536–5546 (1999).
Acknowledgements
We thank Dr Dubravka Eliasson for excellent help in preparing this manuscript. These studies were not possible without the generous grant support from the European commission (grants QLK2-CT-2001-01702, QLK2-CT-1999-00228, and LSHP-CT-2003-503240), The Swedish Research Council, SIDA, The Swedish Foundation for Strategic Research (SSF), LUA/ALF, and The Cancer Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Rights and permissions
About this article
Cite this article
Lycke, N., Bemark, M. Mucosal adjuvants and long-term memory development with special focus on CTA1-DD and other ADP-ribosylating toxins. Mucosal Immunol 3, 556–566 (2010). https://doi.org/10.1038/mi.2010.54
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2010.54
This article is cited by
-
Pharmaceutical and Immunological Evaluation of Cholera Toxin A1 Subunit as an Adjuvant of Hepatitis B Vaccine Microneedles
Pharmaceutical Research (2023)
-
Edible Vaccines: Promises and Challenges
Molecular Biotechnology (2020)
-
Proteomic analysis of cholera toxin adjuvant-stimulated human monocytes identifies Thrombospondin-1 and Integrin-β1 as strongly upregulated molecules involved in adjuvant activity
Scientific Reports (2019)
-
Activated T follicular helper-like cells are released into blood after oral vaccination and correlate with vaccine specific mucosal B-cell memory
Scientific Reports (2018)
-
The regulation of gut mucosal IgA B-cell responses: recent developments
Mucosal Immunology (2017)