Abstract
Objective:
To evaluate asphyxial patterns in term encephalopathic newborns caused by chorioamnionitis or intrapartum blood loss that resulted in cerebral palsy and allegations of obstetrical professional liability.
Study Design:
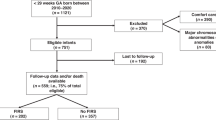
As an expert witness, JKM identified term newborns with profound neurologic impairment: 18 born in the presence of chorioamnionitis and 14 with significant anemia.
Result:
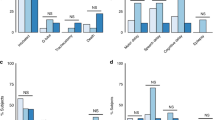
In both study groups, profound depression with low 10-min Apgars was associated with early-onset seizures (88%), multiorgan failure (94%) and a partial prolonged injury to the cortex and subcortical white matter (94%). A cord arterial pH>7.00 was noted in 68% and deep gray matter injury involving the basal ganglia and thalamus occurred in only 19% of the newborns studied.
Conclusion:
The cord arterial pH and pCO2 values, early-onset seizures and paucity of isolated deep gray matter injury support that significant injury occurred postnatally despite appropriate resuscitation. This unique pattern may refute allegations of obstetrical mismanagement in the intrapartum period.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
The American College of Obstetricians and Gynecologists. Neonatal encephalopathy and neurologic outcome, second edition. Report of the American College of Obstetricians and Gynecologists' task force on neonatal encephalopathy. Obstet Gynecol 2014; 123: 896–901.
Graham EM, Ruis KA, Hartman AL, Northington FJ, Fox HE . A systematic review of the role of intrapartum hypoxia–ischemia in the causation of neonatal encephalopathy. Am J Obstet Gynecol 2008; 199: 587–595.
Muraskas JK, Morrison JC . A proposed evidence-based neonatal work-up to confirm or refute allegations of intrapartum asphyxia. Obstet Gynecol 2010; 116: 261–268.
Gotsh F, Romero R, Kusanovic JP, Mazaki-Tavis S, Pineles BL, Erez O et al. The fetal inflammatory response syndrome. Clin Obstet Gynecol 2007; 50: 652–683.
Shalek LF, Perlman JM, Jackson GL, Laptook AR . Depression at birth in term infants exposed to maternal chorioamnionitis: dose neonatal fever play a role? J Perinatol 2005; 25: 447–452.
Wu YW, Escobar GJ, Grether JK, Croen LA, Greene JD, Newman TB . Chorioamnionitis and cerebral palsy in term and near-term infants. JAMA 2003; 290: 2677–2684.
Nelson KB, Grether JK . Potentially asphyxiating conditions and spastic cerebral palsy in infants of normal birth weight. Am J Obstet Gynecol 1998; 179: 507–513.
Rubad C, Deruelle P, Le Gaueff F, Tunez V, Fournier M, Subtil D . Long-term prognosis for infants after massive fetomaternal hemorrhage. Obstet Gynecol 2007; 110 (2P+1): 256–260.
Sheiner E, Shoham-Vardi I, Hallak M, Hadar A, Gortzak-Uzan L, Katz M et al. Placental abruption in term pregnancies: clinical significance and obstetric risk factors. J Matern Fetal Neonatal Med 2003; 13 (1): 45–49.
Johnston MV, Donn SM Hypoxic-ischemic encephalopathy and traumatic intracranial injuries. In: Donn SM, Fisher CW (eds). Risk Management Techniques in Perinatal and Neonatal Practice. Futura Publishing company: New York, NY, USA, 1996; p 453.
Sarnat HB, Sarnat MS . Neonatal encephalopathy following fetal distress: a clinical and electroencephalographic study. Arch Neurol 1976; 33: 696–705.
Kattwinkel J, Bloom R . Textbook of Neonatal Resuscitation, 2nd–6th edn. American Academy of Pediatrics and American Heart Association: Elk Grove Village, IL, 1990, 1994, 2000, 2006 and 2011.
Fong EA, Davies JI, Grey DE, Reid PJ, Erber WN . Detection of massive transplacental haemorrhage by flow cytometry. Clin Lab Haematol 2000; 22: 325–327.
Baergen RN . The placenta as witness. Clin Perinatol 2007; 34: 393–407.
Wylie BJ, D’Alton ME . Fetomaternal hemorrhage. Obstet Gynecol 2010; 115 (5): 1039–1051.
Christensen RD, Lambert DK, Baer VL, Richards DS, Bennett ST, Ilstrup SJ et al. Severe neonatal anemia from fetomaternal hemorrhage:report from a multihospital health-care system. J Perinatol 2013; 33: 429–434.
Rutherford M Neuroimaging of hypoxic ischemic encephalopathy. In: Donn SM, Sinha S, Chiswick M (eds). Birth Asphyxia and The Brain: Basic Science and Clinical Implications. Future Publishing Company: Armouk, NY, USA, 2002, pp 315–354.
Blickstein I, Green T . Umbilical cord blood gases. Clin Perinatol 2007; 34: 451–459.
Pomerance JJ Interpreting Umbilical Cord Blood Gases: For Clinicians Caring for the Fetus or Newborn BNMG: Pasedena, CA, USA, 2004, p 132.
Pearson HA . Anemia in the newborn: a diagnostic approach and challenge. Semin Perinatol 1991; 15: 2–8.
Leone TA, Finer NN . Shock: a common consequence of neonatal asphyxia. J Pediatr 2011; 158: e9–12.
Miller SP, Ramaswamy V, Michelson D, Barkovich J, Holshouser B, Wycliffe N et al. Patterns of brain injury in term neonatal encephalopathy. J Pediatr 2005; 146: 453–460.
Zimmerman RA, Bilaniuk LT . Neuroimaging evaluation of cerebral palsy. Clin Perinatol 2006; 33: 517–544.
Rademakers RP, van der Knapp MS, Verbeeten Jr, Barth PG, Valk J . Central cortico-subcortical involvement: a distinct pattern of brain damage caused by perinatal and postnatal asphyxia in term infants. J Comput Assist Tomogr 1995; 19: 256–263.
Pasternak JF, Gorey MT . The syndrome of acute near-total intrauterine asphyxia in the term infant. Pediatr Neurol 1998; 18: 391–398.
Pasternak JF, Predey TA, Mikhael MA . Neonatal asphyxia: vulnerability of the basal ganglia, thalamus and brainstem. Pediatr Neurol 1991; 7: 147–149.
Volpe J Hypoxic-ischemic encephalopathy: clinical aspects. In: Volpe J (ed). Neurology of the Newborn, 5th ed. WB Saunders: Philadelphia, PA, USA, 2008, pp 400–480.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Muraskas, J., Kelly, A., Nash, M. et al. The role of fetal inflammatory response syndrome and fetal anemia in nonpreventable term neonatal encephalopathy. J Perinatol 36, 362–365 (2016). https://doi.org/10.1038/jp.2015.214
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2015.214