Abstract
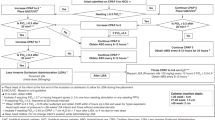
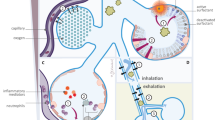
Passage of fetal bowel movement (meconium) is common (in about one out of six births), and in some the staining of the amniotic fluid is a sign of fetal distress. Inhalation of meconium (aspiration syndrome, in upto one out of five to eight such births) just before or at birth may be preventable by a coordinated approach by well-trained and informed birth attendants. Respiratory failure secondary to meconium aspiration syndrome (MAS) remains a major cause of morbidity and mortality in the neonatal population. Infants with hypoxemic respiratory failure because of MAS, persistent pulmonary hypertension of the newborn and pneumonia/sepsis have an increased survival with extracorporeal membrane oxygenation (ECMO). Other treatment options earlier limited to inotropic support, continuous airway pressure (CPAP), conventional ventilatory management, respiratory alkalosis, paralysis and intravenous vasodilators have been replaced by synchronized intermittent mandatory ventilation (SIMV), high-frequency oscillatory ventilation (HFOV), surfactant and inhaled nitric oxide (iNO). HFOV has been advocated for use to improve lung inflation while potentially decreasing lung injury through volutrauma. Other reports describe the enhanced efficacy of HFOV when combined with iNO. Subsequent to studies reporting that surfactant deficiency or inactivation may contribute to neonatal respiratory failure, exogenous surfactant therapy has been implemented with apparent success. Recent studies have shown that iNO therapy in the neonate with hypoxemic respiratory failure can result in improved oxygenation and decreased need for ECMO. However, these innovative interventions are costly, require a sophisticated infrastructure and are not universally accessible. In this paper, a context of systems-approach for prenatal, natal and postnatal management of babies delivered through meconium stained amniotic fluid (MSAF) so that adverse outcomes are minimized and the least number of babies require innovative ventilatory support is described. Previously reported data from a single urban perinatal center (Philadelphia, PA, USA), over a 6-year period (1995–2000), demonstrated that 14.5% (3370/23175 of live births babies were delivered with MSAF. These data also showed that 4.6% of babies (155/3370) with MSAF sustained MAS. Overall, 26% of babies (40/155) with MAS needed ventilatory support (or 0.17% of all live births); of these, only 20% (8/40 or 0.035% of live births) needed innovative ventilatory support. None died or needed ECMO. These data describe the components for a systems approach to prevent and manage adverse outcomes related to MSAF at the regional level II or III perinatal center. Replication of a similar strategy may be more relevant to cost containment and be a safer approach for neonates at risk for MAS-related respiratory failure. This paper assess the evidence for pivotal steps needed to prevent MAS and ensuing neonatal death and disease in the context of diverse perinatal health services.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Usta IM, Mercer BM, Sibai BM . Predictive risk factors for meconium aspiration syndrome. Obstet Gynecol 1996; 86: 230–234.
International Liaison Committee on Resuscitation (ILCOR). Consensus on science with treatment recommendations for pediatric and neonatal patients: part 7—neonatal resuscitation. Pediatrics 2006; 117: e978–e988.
National Neonatal-Perinatal Database (NNPD). Morbidity and mortality among outborn neonates at 10 tertiary care institutions in India during the year 2000. J Trop Pediatr 2004; 50: 170–174.
Dooley SL, Pesavento DJ, Depp R, Socol ML, Tamura RK, Wiringa KS . Meconium below the vocal cords at delivery: correlation with intrapartum events. Am J Obstet Gynecol 1985; 153: 767–770.
Davis RO, Philips III JB, Harris Jr BA, Wilson ER, Huddleston JF . Fatal meconium aspiration syndrome occurring despite airway management considered appropriate. Am J Obstet Gynecol 1985; 151: 731–736.
Wiswell TE, Henley MA . Intratracheal suctioning, systemic infection, and the meconium aspiration syndrome. Pediatrics 1992; 89: 203–206.
Chaturvedi P, Yadav B, Bharambe MS . Delivery room management of neonates born through meconium stained amniotic fluid. Indian Pediatr 2000; 37: 1251–1255.
Mahomed K, Nyoni R, Masona D . Meconium staining of the liquor in a low-risk population. Paediatr Perinat Epidemiol 1994; 8: 292–300.
Ziadeh SM, Sunna E . Obstetric and perinatal outcome of pregnancies with term labour and meconium-stained amniotic fluid. Arch Gynecol Obstet 2000; 264: 84–87.
Falciglia HS . Failure to prevent meconium aspiration syndrome. Obstet Gynecol 1988; 71: 349–353.
Yoder BA . Meconium-stained amniotic fluid and respiratory complications: impact of selective tracheal suction. Obstet Gynecol 1994; 83: 77–84.
Vidyasagar D, Harris V, Pildes RS . Assisted ventilation in infants with meconium aspiration syndrome. Pediatrics 1975; 56: 208–213.
Rossi EM, Philipson EH, Williams TG, Kalhan SC . Meconium aspiration syndrome: intrapartum and neonatal attributes. Am J Obstet Gynecol 1989; 161: 1106–1110.
Falciglia HS, Henderschott C, Potter P, Helmchen R . Does DeLee suction at the perineum prevent meconium aspiration syndrome? Am J Obstet Gynecol 1992; 167: 1243–1249.
Bhutani VK, Chima R, Sivieri EM . Innovative neonatal ventilation and meconium aspiration syndrome. Indian J Pediatr 2003; 70: 421–427.
Carson BS, Losey RW, Bowes Jr WA, Simmons MA . Combined obstetric and pediatric approach to prevent meconium aspiration syndrome. Am J Obstet Gynecol 1976; 126: 712–715.
Wiswell TE, Gannon CM, Jacob J, Goldsmith L, Szyld E, Weiss K et al. Delivery room management of the apparently vigorous meconium-stained neonate: results of the multicenter, international collaborative trial. Pediatrics 2000; 105: 1–7.
Vain NE, Szyld EG, Prudent LM, Wiswell TE, Aguilar AM, Vivas NI . Oropharyngeal and nasopharyngeal suctioning of meconium-stained neonates before delivery of their shoulders: multicentre, randomised controlled trial. Lancet 2004; 364: 597–602.
Lawn JE, Cousens S, Zupan J . 4 million neonatal deaths: when? Where? Why? Lancet 2005; 365: 891–900.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure
The author has declared no financial interests.
Rights and permissions
About this article
Cite this article
Bhutani, V. Developing a systems approach to prevent meconium aspiration syndrome: lessons learned from multinational studies. J Perinatol 28 (Suppl 3), S30–S35 (2008). https://doi.org/10.1038/jp.2008.159
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2008.159
This article is cited by
-
Blood lactate level and meconium aspiration syndrome
Archives of Gynecology and Obstetrics (2015)