Abstract
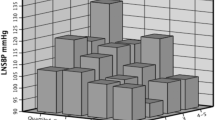
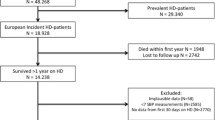
A recent study from the United Kingdom indicates an association between pre hemodialysis (HD) serum sodium (SNa+) and systolic and diastolic blood pressure (SBP and DBP) in chronic HD patients. We extend this analysis to an international cohort of incident HD patients. The Monitoring Dialysis Outcomes initiative encompasses patients from 41 countries. Over 2 years monthly pre-HD SNa+ levels were used as predictors of pre-HD SBP and DBP in a linear mixed model (LMM) adjusted for age, gender, interdialytic weight gain, diabetes, serum albumin and calcium. Similar models were constructed with DBP as outcome. Analyses were carried out stratified by continent (North and South America; Europe and Asia). LMMs were also constructed for the entire observation period of 2 years, and separately the first and the second year after HD initiation. We studied 17 050 incident patients and found SNa+ to have a significant slope estimate in the LMM predicting pre-HD SBP and DBP (ranging from 0.22 to 0.29 and 0.10 to 0.21 mm Hg per mEq l−1, respectively, between the continents). The findings were similar in subsets of SBP and SNa+ tertiles, and separately analyzed for the first and second year. Our analysis shows an independent association between SNa, SBP and DBP in a large intercontinental database, indicating that this relation is a profound biological phenomenon in incident and prevalent HD patients, generalizable to an international level and independent of SBP and DBP magnitude.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Intersalt Cooperative Research Group. Intersalt: an international study of electrolyte excretion and blood pressure. Results for 24 hour urinary sodium and potassium excretion. BMJ 1988; 297 (6644): 319–328.
Appel LJ, Moore TJ, Obarzanek E, Vollmer WM, Svetkey LP, Sacks FM et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. N Engl J Med 1997; 336 (16): 1117–1124.
Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med 2001; 344 (1): 3–10.
Guyton AC, Hall JE . Textbook of Medical Physiology 11th edn. Elsevier Saunders: Philadelphia, PA, USA, 2006.
du Cailar G, Mimran A, Fesler P, Ribstein J, Blacher J, Safar ME . Dietary sodium and pulse pressure in normotensive and essential hypertensive subjects. J Hypertens 2004; 22 (4): 697–703.
Suckling RJ, He FJ, Markandu ND, MacGregor GA . Dietary salt influences postprandial plasma sodium concentration and systolic blood pressure. Kidney Int 2012; 81 (4): 407–411.
Komiya I, Yamada T, Takasu N, Asawa T, Akamine H, Yagi N et al. An abnormal sodium metabolism in Japanese patients with essential hypertension, judged by serum sodium distribution, renal function and the renin-aldosterone system. J Hypertens 1997; 15 (1): 65–72.
Wannamethee G, Whincup PH, Shaper AG, Lever AF . Serum sodium concentration and risk of stroke in middle-aged males. J Hypertens 1994; 12 (8): 971–979.
DeVan AE, Eskurza I, Pierce GL, Walker AE, Jablonski KL, Kaplon RE et al. Regular aerobic exercise protects against impaired fasting plasma glucose-associated vascular endothelial dysfunction with aging. Clin Sci 2013; 124 (5): 325–331.
Diehl KJ, Templeton DL, Ma J, Weil BR, Greiner JJ, Stauffer BL et al. Impaired fasting blood glucose is associated with increased endothelin-1 vasoconstrictor tone. Atherosclerosis 2013; 229 (1): 130–133.
He FJ, Fan S, Macgregor GA, Yaqoob MM . Plasma sodium and blood pressure in individuals on haemodialysis. J Hum Hypertens 2013; 27 (2): 85–89.
Usvyat LA, Haviv YS, Etter M, Kooman J, Marcelli D, Marelli C et al. The MONitoring Dialysis Outcomes (MONDO) initiative. Blood Purif 2013; 35 (1-3): 37–48.
von Gersdorff GD, Usvyat L, Marcelli D, Grassmann A, Marelli C, Etter M et al. Monitoring Dialysis Outcomes across the World - The MONDO Global Database Consortium. Blood Purif 2013; 36 (3-4): 165–172.
R Development Core Team R: A Language and Environment for Statistical Computing, In: R Foundation for Statistical Computing: Vienna, Austria, 2010.
Tesfamariam B, Brown ML, Deykin D, Cohen RA . Elevated glucose promotes generation of endothelium-derived vasoconstrictor prostanoids in rabbit aorta. J Clin Invest 1990; 85 (3): 929–932.
Luft FC, Weinberger MH, Grim CE . Sodium sensitivity and resistance in normotensive humans. Am J Med 1982; 72 (5): 726–736.
Rankin LI, Luft FC, Henry DP, Gibbs PS, Weinberger MH . Sodium intake alters the effects of norepinephrine on blood pressure. Hypertension 1981; 3 (6): 650–656.
Skrabal F, Herholz H, Neumayr M, Hamberger L, Ledochowski M, Sporer H et al. Salt sensitivity in humans is linked to enhanced sympathetic responsiveness and to enhanced proximal tubular reabsorption. Hypertension 1984; 6 (2 Pt 1): 152–158.
Keen ML, Gotch FA . The association of the sodium "setpoint" to interdialytic weight gain and blood pressure in hemodialysis patients. Int J Artif Org 2007; 30 (11): 971–979.
Hecking M, Karaboyas A, Rayner H, Saran R, Sen A, Inaba M et al. Dialysate sodium prescription and blood pressure in hemodialysis patients. Am J Hypertens 2014; 27 (9): 1160–1169.
Oberleithner H, Ludwig T, Riethmuller C, Hillebrand U, Albermann L, Schafer C et al. Human endothelium: target for aldosterone. Hypertension 2004; 43 (5): 952–956.
Oberleithner H, Riethmuller C, Ludwig T, Hausberg M, Schillers H . Aldosterone remodels human endothelium. Acta Physiol 2006; 187 (1-2): 305–312.
Oberleithner H, Riethmuller C, Ludwig T, Shahin V, Stock C, Schwab A et al. Differential action of steroid hormones on human endothelium. J Cell Sci 2006; 119 (Pt 9): 1926–1932.
Oberleithner H, Riethmuller C, Schillers H, MacGregor GA, de Wardener HE, Hausberg M . Plasma sodium stiffens vascular endothelium and reduces nitric oxide release. Proc Natl Acad Sci USA 2007; 104 (41): 16281–16286.
Warnock DG, Kusche-Vihrog K, Tarjus A, Sheng S, Oberleithner H, Kleyman TR et al. Blood pressure and amiloride-sensitive sodium channels in vascular and renal cells. Nat Rev Nephrol 2014; 10 (3): 146–157.
Fleming I, Busse R . Molecular mechanisms involved in the regulation of the endothelial nitric oxide synthase. Am J Physiol Regul Integr Comp Physiol 2003; 284 (1): R1–12.
Li J, White J, Guo L, Zhao X, Wang J, Smart EJ et al. Salt inactivates endothelial nitric oxide synthase in endothelial cells. J Nutr 2009; 139 (3): 447–451.
Perez FR, Venegas F, Gonzalez M, Andres S, Vallejos C, Riquelme G et al. Endothelial epithelial sodium channel inhibition activates endothelial nitric oxide synthase via phosphoinositide 3-kinase/Akt in small-diameter mesenteric arteries. Hypertension 2009; 53 (6): 1000–1007.
Fujiwara N, Osanai T, Kamada T, Katoh T, Takahashi K, Okumura K . Study on the relationship between plasma nitrite and nitrate level and salt sensitivity in human hypertension: modulation of nitric oxide synthesis by salt intake. Circulation 2000; 101 (8): 856–861.
Yee-Moon Wang A, Lu Y, Cheung S, Hiu-Shuen Chan I, Wai-Kei Lam C . Plasma sodium and subclinical left atrial enlargement in chronic kidney disease. Nephrol Dial Transplant 2013; 28 (9): 2319–2328.
Du Cailar G, Ribstein J, Daures JP, Mimran A . Sodium and left ventricular mass in untreated hypertensive and normotensive subjects. Am J Physiol 1992; 263 (1 Pt 2): H177–H181.
Kupari M, Koskinen P, Virolainen J . Correlates of left ventricular mass in a population sample aged 36 to 37 years. Focus on lifestyle and salt intake. Circulation 1994; 89 (3): 1041–1050.
Hecking M, Karaboyas A, Antlanger M, Saran R, Wizemann V, Chazot C et al. Significance of interdialytic weight gain versus chronic volume overload: consensus opinion. Am J Nephrol 2013; 38 (1): 78–90.
Acknowledgements
The results presented in this paper have not been published previously in whole or part, except for presentation as a poster at the Renal Week 2013 of the American Society of Nephrology in Atlanta, GA, USA.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
Drs Bernard Canaud, Peter Kotanko and Nathan W Levin hold stock in Fresenius Medical Care. The remaining authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Journal of Human Hypertension website
Rights and permissions
About this article
Cite this article
Raimann, J., Canaud, B., Etter, M. et al. Association between pre hemodialysis serum sodium concentration and blood pressure: results from a retrospective analysis from the international monitoring dialysis outcomes (MONDO) initiative. J Hum Hypertens 30, 442–448 (2016). https://doi.org/10.1038/jhh.2015.79
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2015.79