Abstract
We evaluated the effects of red ginseng consumption on blood pressure (BP) and the fasting plasma metabolome. This randomized, double-blind, placebo-controlled study included nonobese, nondiabetic, prehypertensive subjects consuming 10 capsules daily containing 5 g red ginseng (n=31) or placebo (n=31). Fasting plasma metabolome profiles were obtained using ultra performance liquid chromatography-linear trap quadrupole Orbitrap MS. After 12 weeks, participants consuming red ginseng showed reductions of 6.5 and 5.0 mm Hg in systolic and diastolic BP, respectively. Compared with controls, those consuming red ginseng showed greater reductions in changed values of systolic BP, diastolic BP and lipoprotein-associated phospholipase A2 (Lp-PLA2) activity, after adjusting for baseline values. In addition, the red ginseng group showed a greater increase in dihydrobiopterin levels and greater decrease in palmitic amide and lysophosphatidylcholines (lysoPCs). The change in diastolic BP positively correlated with changes in lysoPCs and Lp-PLA2 activity. The BP-lowering effect of red ginseng is associated with decreased Lp-PLA2 and lysoPCs and increased dihydrobiopterin levels in prehypertensive subjects (ClinicalTrials.gov: NCT02326766).
Similar content being viewed by others
Introduction
Although hypertension is a known risk factor for atherosclerosis and cardiovascular disease,1, 2, 3, 4 the mechanisms underlying this relationship are unclear. Prehypertension (slightly elevated blood pressure (BP)) can precede hypertension and atherosclerosis for decades, and is a condition that represents early cardiovascular disease. In 2003, the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure defined prehypertension as systolic BP of 120–139 mm Hg or diastolic BP of 80–89 mm Hg and strongly advocated lifestyle and behavioral modification for individuals with prehypertension.5 Therefore, researchers have investigated the potential benefits of dietary supplements and herbal medicine on circulating metabolic profiles.
In this study we focused on the effects of Korean red ginseng that belongs to the Panax family (Panax ginseng C.A. Meyer) and has various pharmacological and biological effects.6 Red and white ginseng are derived from the same species, but red ginseng is steamed and dried without peeling, whereas white ginseng is dried after peeling. Whereas fresh Korean ginseng is steamed and dried, ginsenosides in Korean ginseng are hydrolyzed and transformed. This alteration makes Korean red ginseng contain red ginseng-specific ginsenosides (20(S)-Rg3, 20(R)-Rg3, Rh4, Rk1, Rg5 and so on) that are not found in fresh Korean ginseng, and these ginsenosides have more beneficial effects than that of Korean ginseng.7 Previous studies evaluating the physiological effects of ginseng suggest that red ginseng is more beneficial than other types of ginseng. Several studies have reported that Korean red ginseng improves arterial stiffness in healthy individuals.8, 9, 10 However, results concerning the effect of red ginseng on BP have been mixed, with most studies showing either no substantial change11 or slight decreases in systolic and/or diastolic BP.12, 13 Slight increases in BP (1–4%) were also reported in a minority of studies evaluating the effects of ginseng; however, these increases were not significant.14, 15 This lack of convincing data demonstrating the effects of red ginseng on BP highlights the need for well-designed, randomized clinical trials. In this study we explored the effect of red ginseng extract on BP in nonobese, nondiabetic individuals with prehypertension. To identify metabolites contributing to phenotype differences, we compared the plasma metabolome profiles of participants before and after red ginseng supplementation using ultra performance liquid chromatography (UPLC) and linear trap quadrupole (LTQ) Orbitrap mass spectrometer (MS).
Methods
Study subjects
Prehypertensive individuals between 20 and 70 years of age were recruited by public advertisements from November 2011 to February 2012. Prehypertension was defined as systolic BP of 120–139 mm Hg or diastolic BP of 80–89 mm Hg. The screening identified nondiabetic, nonobese and prehypertensive individuals (56 men and 14 women) who remained within the range for prehypertension during repeated measurements in a 2-week preingestion period before supplementation. Exclusion criteria included previously diagnosed clinical hypertension, self-reported use of antihypertensive medication, the use of other medications (that is, lipid-lowering or antiplatelet medications, disease-related medications and so on), the use of dietary supplements, and history of cardiovascular disease, liver disease, kidney disease, cancer, thyroid disease, pituitary disease or any other serious life-threatening illness that required regular medical treatment. We also excluded women who were pregnant, breastfeeding or intending to become pregnant during the study period. Potential participants underwent health examinations, and those who satisfied the study criteria were asked to participate. Informed written consent was obtained from all participants, and the protocol was approved by the institutional review board of Yonsei University according to the Helsinki Declaration.
Study design and intervention
In this 12-week, double-blind, placebo-controlled, randomized study, the participants were divided into two groups according to treatment: red ginseng (n=35) or placebo (n=35) (ClinicalTrials.gov: NCT02326766; http://www.clinicaltrials.gov). Red ginseng treatment consisted of daily consumption of 10 capsules containing red ginseng (Panax ginseng C.A. Meyer, total 5 g), and placebo treatment consisted of daily consumption of red ginseng-flavored capsules containing corn starch (total 5 g). Participants were assigned to intervention groups in a 1:1 ratio by computer-generated block randomization. Red ginseng and placebo capsules were provided by the Korea Ginseng Corporation (Daejeon, Korea). The red ginseng capsules contained 16.58 mg g−1 total ginsenosides, and the ratio of protopanaxadiol ginsenosides (Rb1, Rb2, Rc, Rd and Rg3) to protopanaxatriol ginsenosides (Rg1, Re and Rf) was 1.65:1. Ginsenosides were analyzed in quadruplicate using standard High-performance liquid chromatography–ultraviolet techniques16 at the Korean Ginseng Research Institute in Daejeon, Korea. The study was divided into two periods: 2-week preingestion period in which the subjects did not ingest red ginseng or placebo, followed by the 12-week ingestion period. Subjects met with the investigational team at five different time points: screening (week −2), rechecking BP (week −1), randomization and baseline measurements (week 0), midpoint of the ingestion period (week 6) and treatment end point (week 12). Daily dietary intake was estimated using the 24-h recall method and 3-day food record (2 week days and 1 weekend), and physical activity was measured at baseline, midpoint and endpoint of the ingestion period. Compliance with study instructions and capsule consumption were monitored by daily documentation by subjects on individualized study calendars and end-study count of returned capsule. Of the 70 subjects, 8 (placebo group, n=4; red ginseng group, n=4) discontinued the study for personal reasons or because of poor compliance. No adverse reactions (that is, fever, hot flush, nausea, vomiting, diarrhea) were observed among the 62 subjects who completed the study.
Assessment of food intake and physical activity
Typical food intake was assessed by the 24-h recall method that consists of a semiquantitative food frequency questionnaire. All subjects received written and oral instructions from a dietitian regarding completion of the 3-day dietary record (2 weekdays and 1 weekend day) in which subjects recorded the types and amounts of food consumed. Participants were interviewed to monitor adherence to the program. Dietary energy values and nutrient content were calculated from the complete 3-day dietary records using the Computer-Aided Nutritional Analysis Program (CAN-pro 3.0, Korean Nutrition Society, Seoul, Korea). Total energy expenditure (kcal per day) was calculated from the basal metabolic rate, 24-h physical activity17 and specific dynamic action of food. The basal metabolic rate for each subject was calculated with the Harris–Benedict equation.18
Anthropometric parameters, BP and blood collection
To calculate body mass index, body weight and height were measured in the morning with subjects unclothed and without shoes. Waist circumference was measured at the umbilical level at the end of normal expiration while standing. BP was measured with an automatic BP monitor (FT-200S, Jawon Medical, Gyeongsan, Korea) in both the arms using appropriately sized cuffs after a 20-min rest. We recorded measurements obtained from the arm with the higher BP. Three BP measurements were obtained at each visit, and differences among the three systolic BP readings were always <5 mm Hg. Participants were instructed not to smoke or drink alcohol for at least 30 min before BP measurement and to fast for 12 h before the initial blood draw and before follow-up visits. Venous blood specimens were collected in EDTA-coated and plain tubes and then centrifuged to yield plasma or serum, respectively, that was stored at −70 °C until analysis.
Serum lipid, fasting glucose and insulin levels
Fasting levels of total cholesterol and triglycerides were measured using commercially available kits and a Hitachi 7600 autoanalyzer (Hitachi, Tokyo, Japan). Apolipoprotein B-containing lipoproteins were precipitated with dextran sulfate–magnesium, and high-density lipoprotein cholesterol concentrations in serum samples were measured enzymatically. For subjects with serum triglyceride levels <400 mg dl−1, low-density lipoprotein (LDL) cholesterol concentrations were estimated indirectly using the Friedewald formula: LDL cholesterol=total cholesterol−(high-density lipoprotein cholesterol+(triglycerides/5)). For subjects with serum triglyceride levels ⩾400 mg dl−1, LDL cholesterol concentrations were measured directly using an enzymatic method on a Hitachi 7600 autoanalyzer. Fasting glucose levels were analyzed by the hexokinase method using a Hitachi 7600 autoanalyzer. Insulin levels were measured by using an immunoradiometric assay kit (DIAsource ImmunoAssays S.A., Louvain, Belgium).
Serum high-sensitivity C-reactive protein and Lp-PLA2 activity
Serum high-sensitivity C-reactive protein was measured with an ADVIA 2400 Clinical Chemistry System (Siemens, Tarrytown, NY, USA) using a commercially available, high-sensitivity C-reactive protein-Latex(II) X2 kit (Denka Seiken, Tokyo, Japan). The activity of lipoprotein-associated phospholipase A2 (Lp-PLA2) was determined using a modification of a previously described, high-throughput radiometric activity assay.19
Nitric oxide and oxidized LDL
Serum total nitric oxide (NO) was determined based on the enzymatic conversion of nitrate to nitrite by nitrate reductase, as analyzed using the Total NO/Nitrite/Nitrate Parameter Assay kit (R&D Systems, Minneapolis, MN, USA). The resulting color reaction was read using a VERSAmax microplate reader (Molecular Devices, Sunnyvale, CA, USA) at 540 nm. Plasma oxidized LDL (ox-LDL) was measured using an enzyme immunoassay (Mercodia AB, Uppsala, Sweden). The resulting color reaction was monitored at 450 nm with a Wallac 1420 Victor2 multilabel counter (PerkinElmer Life Sciences, Boston, MA, USA).
Global (nontargeted) metabolic profiling of plasma
Sample preparation and analysis
Before analysis, 800 μl of 80% cold acetonitrile was added to 100 μl plasma that was then incubated at 4 °C for 10 min, mixed by vortexing and centrifuged at 10 000 r.p.m. for 5 min at 4 °C. The supernatant (820 μl) was dried with N2, and the resulting pellet was dissolved in 100 μl cold 10% methanol. After vortexing for 1 min, the sample was centrifuged at 10 000 r.p.m. for 5 min at 4 °C. The supernatant (85 μl) was transferred to a vial.
UPLC-LTQ Orbitrap XL MS
The plasma extract samples (4 μl) were injected into an Acquity UPLC-BEH-C18 column (2.1 × 50 mm, 1.7 μm; Waters, Milford, MA, USA) coupled with a UPLC system (Waters). The injected samples were equilibrated with water containing 0.1% formic acid (solvent A) and then eluted with an acetonitrile gradient containing 0.1% formic acid (solvent B) at a flow rate of 0.35 ml min−1 for 20 min. The gradient was 0 min, 1% B; 1 min, 1% B; 7 min, 20% B; 15 min, 99% B; 16 min, 99% B; 16.2 min, 1% B; and 20 min, 1% B. Metabolites were separated by UPLC and then analyzed by LTQ Orbitrap XL MS (Thermo Fisher Scientific, Waltham, MA, USA). The MS was operated in electrospray ionization-positive mode, full-scan mode and Fourier transform mode. The MS was operated at a resolution of 30 000 and spray voltage of 5 kV. Flow rates of the nitrogen sheath gas and auxiliary gas were 50 and 5 (arbitrary units), respectively. The capillary voltage, tube-lens voltage and capillary temperature were maintained at 35 V, 80 V and 370 °C, respectively. Orbitrap data were collected in the range of m/z 50−1000. For quality control, a mixture of four standard compounds (acetaminophen, sulfadimethoxine, terfenadine and reserpine) was injected in 1 of every 10 samples. The tandem MS (MS/MS) spectra of the metabolites were obtained by a collision-energy ramp from 55 to 65 eV.
Data processing and metabolite identification
All MS data including retention times, m/z and ion intensities were extracted by SIEVE software (Thermo Fisher Scientific) incorporated into the instrument, and the resulting MS data were assembled into a matrix. SIEVE parameters were set as follows: m/z range 50−1000; m/z width 0.02; retention time width 2.5; and m/z tolerance 0.005. Metabolites were identified using the following databases: ChemSpider (www.chemspider.com), Human Metabolome (www.hmdb.ca), Lipid MAPS (www.lipidmaps.org), Kyoto Encyclopedia of Genes and Genomes (www.genome.jp/kegg) and MassBank (www.massbank.jp). To confirm putative metabolites, MS/MS was performed. The MS/MS spectra were exported from Xcalibur 2.1 software (Thermo Fisher Scientific) to MS Frontier software (Thermo Fisher Scientific), and then compared with reference metabolites in the MS Frontier software database or Human Metabolome, Lipid MAPS and MassBank MS/MS spectra databases.
Statistical analysis
Statistical analyses were performed using SPSS v. 21.0 (IBM SPSS Statistics 21, Chicago, IL, USA). Skewed variables were logarithmically transformed for statistical analyses, but untransformed values are presented for descriptive purposes. Results are expressed as mean±s.d. A two-tailed P-value of <0.05 was considered significant. Clinical variables at the 12-week follow-up were compared between groups using Student’s t-test for independent samples. General linear models were used to compare changes in variables between the two groups after adjusting for baseline values. Paired t-tests were used to evaluate differences between measurements at baseline and the 12-week follow-up within each group. Pearson’s correlation coefficients were used to examine the relationships between variables. False discovery rate-corrected q-values were computed using the R package ‘fdrtool’. Heat maps were created to visualize and evaluate relationships among metabolites and BP measurements in the study population.
Multivariate statistical analysis was performed using SIMCA-P+ software version 12.0 (Umetrics, Umeå, Sweden). Partial least-squares discriminant analysis (PLS-DA) was used as the classification method to differentiate between groups by visualizing the score plot or S-plot using the first and second PLS components. PLS-DA consists of a classical PLS regression, where the dependent variable y is categorical and represents class membership. The large number of peaks in these spectra, which are all potential biomarkers, create modeling and validation challenges. The PLS-DA score plot involves projection of the data in two dimensions, with each data point in the score plot representing a spectrum. The plot summarizes the relationships among the samples (samples that are close to each other are similar, and those that are distant are dissimilar). Goodness of the fit was quantified by R2Y, and predictive ability was quantified by Q2Y. R2Y describes how well the data in the training set are mathematically reproduced and ranges from 0 to 1 (with 1 indicating a model with a perfect fit). Models with Q2Y⩾0.5 are considered to have good predictive ability. The S-plot is used to visualize both covariance and correlation between metabolites from the PLS-DA model in a scatter plot. In the S-plot, the p[1] axis represents the magnitude of each variable in X, and the p(corr)[1] axis represents the reliability of each variable in X. High reliability refers to high magnitude and lower uncertainty for the putative biomarker and high variable importance in the projection (VIP) values. The PLS-DA model was validated using a sevenfold validation procedure, and the reliability of the model was further validated by a permutation test (n=200).
Results
Effects of 12-week consumption of red ginseng on clinical and biochemical characteristics
Table 1 shows the general and biochemical characteristics of subjects receiving red ginseng or placebo for 12 weeks. Baseline values for the two groups did not differ significantly regarding age, gender distribution, smoking, alcohol consumption, body mass index, serum lipid profiles or levels of high-sensitivity C-reactive protein, glucose or insulin. Similarly, physical activity, estimated total calorie intake and intake of protein, fat and carbohydrates as percent of total daily calories did not differ significantly between groups. In red ginseng group, total NO levels were significantly increased and ox-LDL concentrations were significantly decreased at 12-week follow-up compared with baseline (P=0.031 and P=0.032, respectively). After the 12-week intervention, individuals receiving red ginseng showed a decrease of 6.5 mm Hg in systolic BP compared with baseline (133.5±2.37 vs. 127.0±1.81 mm Hg; P<0.01) and decrease of 5.0 mm Hg in diastolic BP (85.2±1.20 vs. 80.2±1.21 mm Hg; P<0.01) (Figure 1). In addition, Lp-PLA2 activity appeared to be lower among those receiving red ginseng (30.3±1.56 vs. 28.8±1.35 nmol ml−1 min−1), but this difference was not significant (P=0.087). In contrast, the placebo group did not show significant changes in systolic BP (133.8±2.47 vs. 131.2±1.80 mm Hg), diastolic BP (85.6±1.37 vs. 84.7±1.19 mm Hg) or Lp-PLA2 activity (30.9±0.99 vs. 32.1±0.97 nmol ml−1 min−1).
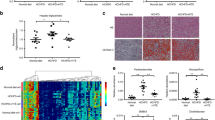
Systolic blood pressure (BP), diastolic BP, and lipoprotein-associated phospholipase A2 (Lp-PLA2) activity at baseline (□) and 12-week follow-up (▪) in subjects receiving red ginseng (n=31) or placebo (n=31). Results are presented as mean±s.d. §Groups were compared using logarithmically transformed data. Pa-values (changes in values, independent t-test); Pb-values (changes in values, adjusting for baseline). ††P<0.01 (red ginseng vs. placebo at 12-week follow-up). ‡P<0.1, **P<0.01 (red ginseng vs. placebo at baseline, paired t-test).
Compared with the placebo group, the red ginseng group showed lower diastolic BP at the 12-week follow-up (P=0.009). A comparison of biochemical parameter changes from baseline between groups revealed that individuals consuming red ginseng had greater reductions in systolic BP (P=0.042), diastolic BP (P=0.005) and Lp-PLA2 activity (P=0.010) after adjusting for baseline values (Figure 1).
Plasma metabolic profiling using UPLC-LTQ Orbitrap MS
Nontargeted metabolic pattern analysis
The MS data of plasma metabolites were analyzed using a PLS-DA score plot for the following comparisons: (1) placebo group vs. red ginseng group at baseline; and (2) placebo group vs. red ginseng group at 12-week follow-up. The two-component PLS-DA scatter plots of plasma metabolites did not show distinct clustering or clear separation between groups at baseline (R2X(cum)=0.448, R2Y(cum)=0.532, Q2Y(cum)=0.0704) (data not shown). However, distinct clustering and clear separation between groups was observed at 12 weeks (R2X(cum)=0.410, R2Y(cum)=0.673, Q2Y(cum)=0.527) (Figure 2a). Validation of the PLS-DA model was carried out by permutation testing that gave an R2Y intercept value of 0.466 and Q2Y intercept value of 0.0427. To identify differentiating metabolites, S-plots of p(1) and p(corr)(1) were generated using centroid scaling (Figure 2b). The S-plots revealed that metabolites with higher or lower p(corr) values were better able to discriminate between the two groups.
Identification of plasma metabolites
Among 4514 plasma metabolites, those that played important roles in the separation between the groups were selected according to VIP values, with values of >1.0 considered more important for discrimination between groups. Of the 107 metabolites selected, 18 metabolites had been previously identified (Table 2), and 89 metabolites were unknown. Our results show that baseline concentrations of the 18 previously identified metabolites did not differ between groups. However, at the 12-week follow-up metabolite concentrations were altered in the red ginseng group, whereas the placebo group did not show significant changes any of the 18 metabolites. In the red ginseng group dihydrobiopterin was significantly increased, and the following 14 metabolites were significantly decreased: palmitic amide and lysophosphatidylcholines (lysoPCs) C14:0, C15:0, C16:1, C16:0, C17:0, C18:3, C18:2, C18:1, C18:0, C20:5, C20:4, C20:3 and C22:6 (Table 2). Next, we compared the plasma metabolite changes from baseline between groups, and found that individuals consuming red ginseng showed a greater increase in dihydrobiopterin (q=0.049) and greater reductions in palmitic amide (q=0.044), lysoPC(14:0) (q=0.003), lysoPC(15:0) (q=0.002), lysoPC(16:1) (q=0.004), lysoPC(16:0) (q=0.001), lysoPC(17:0) (q=0.003), lysoPC(18:3) (q=0.001), lysoPC(18:2) (q=0.003), lysoPC(18:1) (q=0.001), lysoPC(18:0) (q=0.001), lysoPC(20:4) (q=0.001), lysoPC(20:3) (q=0.001) and lysoPC(22:6) (q=0.009) (Table 2).
Relationships among changes in BP, plasma Lp-PLA2 activity and plasma metabolite levels
Correlations among changes in systolic and diastolic BP, plasma Lp-PLA2 activity and major plasma metabolite levels were determined in all subjects (Figure 3). We found that change in (△) systolic BP positively correlated with △diastolic BP and △lysoPCs containing C14:0, C15:0, C16:0, C17:0, C18:1, C20:5 and C20:4, and negatively correlated with △ total NO. In addition, △diastolic BP positively correlated with △Lp-PLA2 activity and △lysoPCs containing C14:0, C15:0, C16:1, C16:0, C17:0, C18:1, C18:0, C20:5, C20:4, C20:3 and C22:6. Interestingly, △Lp-PLA2 activity correlated negatively with △dihydrobiopterin, and positively with △ox-LDL, △palmitic amide and △lysoPCs containing C14:0, C15:0, C16:1, C16:0, C17:0, C18:3, C18:2, C18:1, C18:0, C20:5, C20:4, C20:3 and C22:6 (Figure 3).
Correlation matrix of changes in systolic and diastolic blood pressure (BP), plasma lipoprotein-associated phospholipase A2 (Lp-PLA2) activity and levels of major plasma metabolites in all subjects. Pearson’s correlation coefficients were used to examine relationships between these parameters. Red represents a positive correlation, and blue represents a negative correlation.
Discussion
Approximately 200 substances including ginsenosides, ginsenosides, polysaccharides, polyacetylenes, peptides, amino acids and phenol compounds exist in Korean ginseng. Among them, ginsenosides are major bioactive component.20 While Korean ginseng undergoes steaming and drying process, the physiological effects of ginsenosides are improved. In the present study, we used Korean red ginseng powder that contains 16.58 mg g−1 total ginsenosides in order to verify its effect on BP and the fasting plasma metabolome. Our previous study reported that consumption of red ginseng (same amount and composition of Korean red ginseng used in this study) showed a significant improvement on serum glucose level and glucose-related biomarkers in subjects with impaired fasting glucose, impaired glucose tolerance and type 2 diabetes mellitus.21
Our study showed that a 12-week intervention consisting of daily ingestion of 5 g Korean red ginseng powder significantly reduced systolic and diastolic BP in individuals with prehypertension. As the subjects who participated in this study did not take any medication and dietary supplement, and there were no significant differences regarding food intake (that is, total calorie intake and intake of protein, fat and carbohydrate), we expected that the effects of medication/dietary habits on the present findings were minimized. This result is in agreement with a recent paper describing the BP-lowering effect of Panax ginseng extract in adults with systolic BP of 120–159 mm Hg or diastolic BP of 80–99 mm Hg.12 Similarly, Caron et al.13 reported that daily consumption of 200 mg Panax ginseng extract decreased diastolic BP in healthy adults compared with those who received a placebo. In another double-blind placebo-controlled study, Mucalo et al.22 reported that daily consumption of 3 g American ginseng (Panax quinquefolius L.) for 12 weeks lowered systolic BP by 11.7% (P<0.001) in subjects with type 2 diabetes and concomitant hypertension.
Several possible mechanisms have been suggested to explain the physiological effects of red ginseng. Ginseng increases NO concentrations and has papaverine-like effects, causing smooth muscle relaxation that could lower BP.23, 24 Recent studies have also suggested that Panax ginseng C.A. Meyer may be a potent modulator of vascular function. For example, Jovanovski et al.8, 9 showed that ingestion of Panax ginseng extract acutely improved endothelial function and lowered central and peripheral arterial pressure in healthy individuals.25 Park et al.10 also found that red ginseng dose-dependently increased phosphorylation of endothelial NO synthase and NO production in endothelial cells. Consistent with these results, our study showed that 12-week supplementation of red ginseng increased NO concentrations, and changes in NO from baseline correlated negatively with changes in systolic BP. In addition, dihydrobiopterin also increased in red ginseng group, and it is an oxidation product of tetrahydrobiopterin that is essential for NO synthase-catalyzed oxidation of arginine to citrulline and NO.26 These results imply that lowered BP in red ginseng group may be mediated through increased NO production that is partly associated with dihydrobiopterin.
In addition to its BP-lowering effect, we found that red ginseng decreased plasma Lp-PLA2 activity and lysoPCs, some of the main products of Lp-PLA2 hydrolytic activity.27 Similarly, serum levels of lysoPCs were also reduced by 6-week red ginseng supplementation in rats.28 A metabonomic study in spontaneously hypertensive rats29 showed that lysoPCs may be useful as biomarkers of hypertension and suggested that changes in lysoPCs were involved in the therapeutic effects of traditional Chinese medicine for hypertension. In addition, the association between β-blocker treatment and lower levels of Lp-PLA2 and lysoPCs containing C16:0, C18:0 and C18:1 has been reported.30 Our study also identified lysoPC(16:0) (VIP: 39.3052), lysoPC(18:0) (VIP: 15.2275) and lysoPC(18:1) (VIP: 9.1432) as the best predictors among the plasma lysoPCs for discriminating between the placebo and red ginseng groups at 12 weeks.
Recently, prehypertension was found to be associated with increased Lp-PLA2 activity and elevated levels of circulating lysoPCs and ox-LDL; a positive correlation between lysoPCs and BP was also reported.31 Our study also showed strong positive associations among changes in BP, Lp-PLA2 activity and lysoPCs. Although lysoPCs constitute only 1–5% of the total phosphatidylcholine content of non-ox-LDL, as much as 40–50% of the phosphatidylcholine contained within the LDL molecule is converted to lysoPC during LDL oxidation.32 A previous study demonstrated that consumption of red ginseng (3 or 6 g per day) for 8 weeks resulted in greater reductions in plasma ox-LDL concentrations in healthy individuals as compared with placebo.6 In accordance with the previous studies, red ginseng group showed a significant reduction in ox-LDL, and this reduction positively correlated with changes in Lp-PLA2 activity. However, classic lipid measures, which are associated with hypertension by increasing blood viscosity,33 were not changed in our study. Therefore, the decreased plasma Lp-PLA2 activity and lysoPCs in the red ginseng group in our study may be because of decreased ox-LDL levels, rather than altered lipid profiles such as LDL, high-density lipoprotein or triglycerides. Our results also showed that individuals consuming red ginseng exhibited a greater decrease in palmitic amide at 12 weeks than those receiving the placebo. Palmitic amide is a primary fatty acid amide derived from palmitic acid; however, the mechanism by which palmitic amide is produced and degraded in biological systems is unknown.
Although results of studies evaluating red ginseng intake on BP have been mixed, we found that daily ingestion of 5 g Korean red ginseng powder for 12 weeks by prehypertensive subjects lowered systolic BP by 4.9%, diastolic BP by 5.9% and plasma Lp-PLA2 activity by 5.0% compared with placebo. The relatively small sample size used in this study may not be large enough to detect all red ginseng intake-associated metabolic changes. To support our data more accurately, a large-scale further study using several doses of red ginseng is required. This further study may also prove the dose-dependent effect of red ginseng. Despite these limitations, our approach using UPLC-LTQ Orbitrap MS-based metabolomics and multivariate data analysis revealed a greater increase in dihydrobiopterin and greater reduction in palmitic amide and lysoPCs containing C14:0, C15:0, C16:1, C16:0, C17:0, C18:3, C18:2, C18:1, C18:0, C20:4, C20:3 and C22:6 in individuals consuming red ginseng for 12 weeks compared with those receiving the placebo.
Our study provides evidence for a beneficial role of red ginseng supplementation against prehypertension-related increases in specific metabolites, especially lysoPCs and palmitic amide. The decreased lysoPC levels and Lp-PLA2 activity and increased dihydrobiopterin level may provide valuable clues regarding the mechanism underlying decreased BP with red ginseng supplementation that did not significantly alter classic lipid measures. In conclusion, we suggest that the BP-lowering effect of Korean red ginseng may be partly associated with reductions in circulating Lp-PLA2 activity and lysoPC levels and an increase in dihydrobiopterin level in nonobese, nondiabetic, prehypertensive subjects. These results imply the potential usefulness of lysoPC levels as biomarkers of hypertension and for evaluating the effects of therapies on BP.
References
Danaei G, Finucane MM, Lin JK, Singh GM, Paciorek CJ, Cowan MJ, Farzadfar F, Stevens GA, Lim SS, Riley LM, Ezzati M ; Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group (Blood Pressure). National, regional, and global trends in systolic blood pressure since 1980: systematic analysis of health examination surveys and epidemiological studies with 786 country-years and 5·4 million participants. Lancet 2011; 377: 568–577.
Roger VL, Go AS, Lloyd-Jones DM, Adams RJ, Berry JD, Brown TM, Carnethon MR, Dai S, de Simone G, Ford ES, Fox CS, Fullerton HJ, Gillespie C, Greenlund KJ, Hailpern SM, Heit JA, Ho PM, Howard VJ, Kissela BM, Kittner SJ, Lackland DT, Lichtman JH, Lisabeth LD, Makuc DM, Marcus GM, Marelli A, Matchar DB, McDermott MM, Meigs JB, Moy CS, Mozaffarian D, Mussolino ME, Nichol G, Paynter NP, Rosamond WD, Sorlie PD, Stafford RS, Turan TN, Turner MB, Wong ND, Wylie-Rosett J . American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2011 update: a report from the American Heart Association. Circulation 2011; 123: e18–e209.
Su TC, Jeng JS, Chien KL, Sung FC, Hsu HC, Lee YT . Hypertension status is the major determinant of carotid atherosclerosis: a community-based study in Taiwan. Stroke 2001; 32: 2265–2271.
Glasser SP, Khodneva Y, Lackland DT, Prineas R, Safford MM . Prehypertension and incident acute coronary heart disease in the Reasons for Geographic and Racial Differences in Stroke (REGARDS) study. Am J Hypertens 2014; 27: 245–251.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, Jones DW, Materson BJ, Oparil S, Wright JT Jr, Roccella EJ ; National Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National High Blood Pressure Education Program Coordinating Committee. The seventh report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Kim JY, Park JY, Kang HJ, Kim OY, Lee JH . Beneficial effects of Korean red ginseng on lymphocyte DNA damage, antioxidant enzyme activity, and LDL oxidation in healthy participants: a randomized, double-blind, placebo-controlled trial. Nutr J 2012; 11: 47.
Jin Y, Kim YJ, Jeon JN, Wang C, Min JW, Noh HY, Yang DC . Effect of white, red and black ginseng on physicohemical properties and ginsenosides. Plant Foods Hum Nutr 2015; 70: 141–145.
Jovanovski E, Jenkins A, Dias AG, Peeva V, Sievenpiper J, Arnason JT, Rahelic D, Josse RG, Vuksan V . Effects of Korean red ginseng (Panax ginseng C.A. Mayer) and its isolated ginsenosides and polysaccharides on arterial stiffness in healthy individuals. Am J Hypertens 2010; 23: 469–472.
Jovanovski E, Peeva V, Sievenpiper JL, Jenkins AL, Desouza L, Rahelic D, Sung MK, Vuksan V . Modulation of endothelial function by Korean red ginseng (Panax ginseng C.A. Meyer) and its components in healthy individuals: a randomized controlled trial. Cardiovasc Ther 2014; 32: 163–169.
Park JB, Kwon SK, Nagar H, Jung SB, Jeon BH, Kim CS, Oh JH, Song HJ, Kim CS . Rg3-enriched Korean red ginseng improves vascular function in spontaneously hypertensive rats. J Ginseng Res 2014; 38: 244–250.
Rhee MY, Kim YS, Bae JH, Nah DY, Kim YK, Lee MM, Kim HY . Effect of Korean red ginseng on arterial stiffness in subjects with hypertension. J Altern Complement Med 2011; 17: 45–49.
Rhee MY, Cho B, Kim KI, Kim J, Kim MK, Lee EK, Kim HJ, Kim CH . Blood pressure lowering effect of Korea ginseng derived ginseol K-g1. Am J Chin Med 2014; 42: 605–618.
Caron MF, Hotsko AL, Robertson S, Mandybur L, Kluger J, White CM . Electrocardiographic and hemodynamic effects of Panax ginseng. Ann Pharmacother 2002; 36: 758–763.
Siegel RK . Ginseng and high blood pressure. JAMA 1980; 243: 32.
Buettner C, Yeh GY, Phillips RS, Mittleman MA, Kaptchuk TJ . Systematic review of the effects of ginseng on cardiovascular risk factors. Ann Pharmacother 2006; 40: 83–95.
Fitzloff JF, Yat P, Lu ZZ, Awang DVC, Amason JT, Van Breemen RB, Hall T, Blumenthal M, Fong HHS . Perspectives on the quality assurance of ginseng products in North America. Proceedings of the 7th International Ginseng Symposium, Seoul, Korea 1998, 138–145.
Christian JL, Greger JL (eds). Nutrition for Living4th edn.Benjamin/Cummings Publishing Co.: Redwood City, CA, USA. 1994, 242–266.
Shils ME, Shike M, Ross AC, Caballero B, Cousins RJ (eds). Modern Nutrition in Health and Disease10th edn.Lippincott Williams & Wilkins: Philadelphia, PA, USA. 2006, 136–148.
Wilensky RL, Shi Y, Mohler ER 3rd, Hamamdzic D, Burgert ME, Li J, Postle A, Fenning RS, Bollinger JG, Hoffman BE, Pelchovitz DJ, Yang J, Mirabile RC, Webb C, Zhang L, Zhang P, Gelb MH, Walker MC, Zalewski A, Macphee CH . Inhibition of lipoprotein-associated phospholipase A2 reduces complex coronary atherosclerotic plaque development. Nat Med 2008; 14: 1059–1066.
Kim DH . Chemical diversity of Panax ginseng, Pnanx quinquifolium, and Panax natoginseng. J Ginseng Res 2012; 36: 1–15.
Bang H, Kwak JH, Ahn HY, Shin DY, Lee JH . Korean red ginseng improves glucose control in subjects with impaired fasting glucose, impaired glucose tolerance or newly diagnosed type 2 diabetes mellitus. J Med Food 2014; 17: 128–134.
Mucalo I, Jovanovski E, Rahelić D, Božikov V, Romić Z, Vuksan V . Effect of American ginseng (Panax quinquefolius L.) on arterial stiffness in subjects with type-2 diabetes and concomitant hypertension. J Ethnopharmacol 2013; 150: 148–153.
Jellin JM, Batz F, Hitchens K (eds). Pharmacist’s Letter/Prescriber’s Letter Natural Medicines Comprehensive Database. Therapeutic Research Faculty: Stockton, CA, USA. 1999.
Sung J, Han KH, Zo JH, Park HJ, Kim DH, Oh BH . Effects of red ginseng upon vascular endothelial function in patients with essential hypertension. Am J Chin Med 2000; 28: 205–216.
Jovanovski E, Bateman EA, Bhardwaj J, Fairgrieve C, Mucalo I, Jenkins AL, Vuksan V . Effect of Rg3-enriched Korean red ginseng (Panax ginseng) on arterial stiffness and blood pressure in healthy individuals: a randomized controlled trial. J Am Soc Hypertens 2014; 8: 537–541.
Suckling CJ, Gibson CL, Huggan JK, Morthala RR, Clarke B, Kununthur S, Wadsworth RM, Daff S, Papale D . 6-Acetyl-7,7-dimethyl-5,6,7,8-tetrahydropterin is an activator of nitric oxide synthases. Bioorg Med Chem Lett 2008; 18: 1563–1566.
Reddy KJ, Singh M, Bangit JR, Batsell RR . The role of lipoprotein-associated phospholipase A2 on cardiovascular disease risk assessment and plaque rupture: a clinical review. J Clin Lipidol 2009; 3: 85–93.
Kim HJ, Cho CW, Hwang JT, Son N, Choi JH, Shim GS, Han CK . LC-MS-based metabolomic analysis of serum and livers from red ginseng-fed rats. J Ginseng Res 2013; 37: 371–378.
Jiang H, Nie L, Li Y, Xie J . Application of ultra-performance liquid chromatography coupled with mass spectrometry to metabonomic study on spontaneously hypertensive rats and intervention effects of Ping Gan prescription. J Sep Sci 2012; 35: 483–489.
Giuseppe A, Andreas E, Nuno VD, Jan N, Prehn C, Adamski J, Gonçalves I . Treatment with beta-blockers is associated with lower levels of Lp-PLA2 and suPAR in carotid plaques. Cardiovasc Pathol 2013; 22: 438–443.
Kim M, Jung S, Kim SY, Lee SH, Lee JH . Prehypertension-associated elevation in circulating lysophosphatidlycholines, Lp-PLA2 activity, and oxidative stress. PLoS ONE 2014; 9: e96735.
Matsumoto T, Kobayashi T, Kamata K . Role of lysophosphatidylcholine (LPC) in atherosclerosis. Curr Med Chem 2007; 14: 3209–3220.
Takiwaki M, Tomoda F, Koike T, Taki T, Inoue H, Kigawa M, Kitajima I, Uji Y . Increased levels of small dense low-density lipoprotein cholesterol associated with hemorheological abnormalities in untreated, early-stage essential hypertensives. Hypertens Res 2014; 37: 1008–1013.
Acknowledgements
We thank the research volunteers who participated in the studies and the technical assistants of the Yonsei Center for Research Facilities for assistance with LC-MS (LTQ Orbitrap (micro-LC)) analyses. This research was supported by the Bio & Medical Technology Development Program (NRF-2012M3A9C4048762) funded by the Ministry of Science, ICT & Future Planning, Republic of Korea.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Cha, T., Kim, M., Kim, M. et al. Blood pressure-lowering effect of Korean red ginseng associated with decreased circulating Lp-PLA2 activity and lysophosphatidylcholines and increased dihydrobiopterin level in prehypertensive subjects. Hypertens Res 39, 449–456 (2016). https://doi.org/10.1038/hr.2016.7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.7
Keywords
This article is cited by
-
Positive influence of gut microbiota on the effects of Korean red ginseng in metabolic syndrome: a randomized, double-blind, placebo-controlled clinical trial
EPMA Journal (2021)
-
Mechanisms of action of Panax notoginseng ethanolic extract for its vasodilatory effects and partial characterization of vasoactive compounds
Hypertension Research (2019)
-
Impact of 8-week linoleic acid intake in soy oil on Lp-PLA2 activity in healthy adults
Nutrition & Metabolism (2017)
-
Distinct urine metabolome after Asian ginseng and American ginseng intervention based on GC-MS metabolomics approach
Scientific Reports (2016)