Abstract
Improvement in cardiovascular (CV) morbidity and mortality in the EMPA-REG OUTCOME study provides new insight into the therapeutic use of sodium-dependent glucose cotransporter 2 (SGLT2) inhibitors in patients with type 2 diabetes. Although SGLT2 inhibitors have several pleiotropic effects, the underlying mechanism responsible for their cardioprotective effects remains undetermined. In this regard, the absence of a nocturnal fall in blood pressure (BP), that is, non-dipping BP, is a common phenomenon in type 2 diabetes and has a crucial role in the pathogenesis of CV morbidity and mortality. In most clinical trials, SGLT2 inhibitors reduce both systolic BP (~3–5 mm Hg) and diastolic BP (~2 mm Hg) in patients with type 2 diabetes. In addition, recent clinical and animal studies have revealed that SGLT2 inhibitors enable the change in BP circadian rhythm from a non-dipper to a dipper type, which is possibly associated with the improvement in CV outcomes in patients with type 2 diabetes. In this review, recent data on the effect of SGLT2 inhibitors on the circadian rhythm of BP will be summarized. The possible underlying mechanisms responsible for the SGLT2 inhibitor-induced improvement in the circadian rhythm of BP will also be discussed.
Similar content being viewed by others
Introduction
The prevalence of cardiovascular disease (CVD) is greater among individuals with diabetes and obesity, which contributes to the major cause of mortality in these patients.1 Moreover, hypertension is found in two-thirds of patients with diabetes and is a significant contributing factor that adds a further layer of complexity to CVD in these patients.2 Therefore, several guidelines have emphasized the importance of blood pressure (BP) control to prevent the progression of cardiovascular (CV) complications in patients with type 2 diabetes.
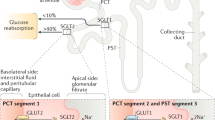
Recently, the EMPA-REG OUTCOME study provided new insight into the management of CV complications using a selective sodium-dependent glucose cotransporter 2 (SGLT2) inhibitor in patients with type 2 diabetes.3 SGLT2 inhibition prevents the reabsorption of glucose from the S1 segment of the proximal tubules of the kidney and thereby increases the urinary excretion of glucose.4 Although SGLT2 inhibitor-induced reduction in blood glucose levels occurs independently of β-cell functions and insulin,5 the underlying mechanism by which an SGLT2 inhibitor improves CV outcomes in type 2 diabetes remains undetermined. Accumulating evidence suggests that SGLT2 inhibitors have pleiotropic effects, including reduced body weight and BP, and improved vascular stiffness and insulin sensitivity as well as diuretic effects.6
Advance in ambulatory BP monitoring and home BP measurement have demonstrated the variability of BP.7, 8, 9 In healthy subjects, BP drops an average of 10–20% when transitioning from waking (active period) to sleeping (inactive period), and this phenomenon is referred to as dipper-type BP.7 Subjects in whom the nocturnal drop in BP is blunted or <10% are referred to as having a non-dipper BP pattern.9 The Ohasama study indicated that each 5% change in the decline in nocturnal systolic BP (SBP) and diastolic BP (DBP) was associated with an approximately 20% greater risk of CV mortality.9 It has also been shown that diminished nocturnal decline in BP is an important determinant of CV mortality independently of overall BP during a 24-h period.8, 9
Recent clinical studies have indicated that SGLT2 inhibitors improve nocturnal BP.10, 11 Thus the cardioprotective effects of SGLT2 inhibitors may be mediated by their effects on BP, especially their improvement of the circadian rhythm of BP. In this review, we summarize recent information regarding the effects of SGLT2 inhibitors on BP and its circadian rhythm. We also discuss the possible mechanisms underlying the SGLT2 inhibitor-induced improvement in the circadian rhythm of BP.
Hypothesis: improvement in CV events mediated by an SGLT2 inhibitor is associated with BP changes
The absence of physiological nocturnal dipping (non-dipping pattern) and an early morning BP surge confer a significantly worse prognosis in hypertensive patients with diabetes.12, 13 It has also been indicated that non-dipper hypertensive patients show a greater degree of insulin resistance and lower levels of adiponectin than do dipper hypertensive subjects.14 Importantly, a significant correlation has been shown between a disrupted circadian rhythm of BP and CV events or mortality.15, 16, 17 A meta-analysis that included data from 3468 patients from four prospective studies demonstrated that the dipping pattern and night–day BP ratio are significant and independent predictors of CV events and mortality in hypertensive patients without a history of major CVD.18 Moreover, Fogari et al.16 showed that the persistence of the non-dipper type of BP was associated with increased left ventricular hypertrophy and atherosclerotic CVD. It has also been shown that increases in CV morbidity and mortality are associated with a loss of the physiological circadian rhythm of BP in hypertensive patients with diabetes.19, 20
SGLT2 inhibition and cardiovascular events in type 2 diabetes
Patients with type 2 diabetes commonly develop CVD, which is responsible for approximately 80% of the mortality in type 2 diabetics.21 Although hyperglycemia is crucial for macrovascular complications to develop in diabetes, clinical studies have shown that intensive blood glucose control has little beneficial effect on CV morbidity and mortality in patients with type 2 diabetes.22, 23 Recently, the EMPA-REG OUTCOME study has shown that empagliflozin, an SGLT2 inhibitor, significantly reduces the primary composite outcome of CV events, which is driven by the 38% reduction in CV mortality.3 Moreover, meta-analyses of major adverse CV events in type 2 diabetes in 11 292 patients treated with empagliflozin24 and 9339 patients treated with dapagliflozin25 have revealed that the administration of SGLT2 inhibitors was not associated with an increased risk of major adverse CV events but rather had the potential for beneficial CV effects on the population with major adverse CV events or with a history of CVD. Several prospective clinical trials are ongoing with canagliflozin (CANVAS)26, dapagliflozin (Declare-TIMI 5827 REFORM28) and ertugliflozin (VERTIS)29 in patients with type 2 diabetes with either established or multiple high-risk factors for CVD. In db/db mice, empagliflozin ameliorated CV injury, including cardiac interstitial fibrosis and remodeling as well as vascular dysfunction.30 These data are consistent with the hypothesis that an SGLT2 inhibitor has the potential to improve CV morbidity and mortality in subjects with type 2 diabetes.
SGLT2 inhibitors and BP
Several clinical trials have demonstrated that SGLT2 inhibitors, as either monotherapy or add-on therapy, are clearly associated with a significant reduction in BP in patients with type 2 diabetes. A recent network meta-analysis of 33 randomized control trials in 17 600 participants with type 2 diabetes showed a reduction in office seated SBP (maximum reduction of −4.9 mm Hg) and DBP (maximum reduction of −2.0 mm Hg) by SGLT2 inhibitors.31
Ambulatory BP measurement is better than office seated BP.32 Moreover, ambulatory 24-h BP is a more significant predictor of CV events than conventional office seated BP in patients with type 2 diabetes.33 It has been suggested that the circadian rhythm of BP is a possible target for treatment with SGLT2 inhibitors in patients with type 2 diabetes.34 Tikkanen et al.10 demonstrated a significant reduction in 24-h ambulatory SBP and DBP with either 10 mg (−3.44 and −1.36 mm Hg, respectively) or 25 mg (−4.16 and −1.72 mm Hg, respectively) empagliflozin for 12 weeks in hypertensive patients with type 2 diabetes. In a randomized, placebo-controlled, double-blind trial with 75 subjects with type 2 diabetes, 12 weeks of treatment with dapagliflozin (10 mg day−1) caused a significant reduction in 24-h ambulatory BP (5.6 mm Hg), although the change was greater in daytime BP (8.8 mm Hg) and less in the nocturnal BP (1.9 mm Hg).35 Amin et al.36 showed that ertugliflozin consistently reduced ambulatory mean daytime, but not nocturnal, SBP. In a subgroup analysis of a phase III randomized trial of the EMPA-REG OUTCOME study, empagliflozin significantly reduced 24- h SBP in dipper (sleep-time mean SBP⩽90% of awake-time mean; n=417) and non-dipper (sleep-time mean SBP>90% of awake-time mean; n=350) hypertensive patients with type 2 diabetes.37 Moreover, in a randomized, double-blind placebo-controlled phase III study, dapagliflozin consistently decreased 24-h ambulatory SBP, whereas greater reductions in daytime ambulatory SBP was shown in type 2 hypertensive diabetic patients who already received a β-blocker.38 In a case report of a patient with type 2 diabetes, Mori et al.11 showed that dapagliflozin caused decreases in both 24-h SBP and DBP from 131/87 to 127/83 mm Hg at day 14, with a particular decrease in nocturnal BP from 123/84 to 116/75 mm Hg (the nocturnal BP dip increased from 9.6% to 12.8%), respectively. These data suggest that dapagliflozin changed the circadian rhythm of BP from a non-dipper to dipper pattern in these patients with type 2 diabetes.
We have recently shown that empagliflozin administration changed the circadian rhythm of BP from a non-dipper to dipper profile in salt-treated, obese Otsuka Long Evans Tokushima Fatty (OLETF) rats.39 In this study, 4 weeks of salt treatment elevated BP and abolished the differences in BP between dark and light periods, suggesting a non-dipper type of hypertension. Interestingly, 5-week treatment with empagliflozin (10 mg kg−1 day−1) reduced BP with a normalization of the circadian rhythm of BP to a dipper pattern. Obesity, impaired glucose metabolism, insulin resistance and hypertension are common features of metabolic syndrome.40, 41 Furthermore, metabolic syndrome is also associated with the development of type 2 diabetes and CVD, as well as a disrupted circadian rhythm of BP.42, 43 In this regard, we have shown that 5-week treatment with luseogliflozin (10 mg kg−1 day−1) not only blunted the development of hypertension but also restored the circadian rhythm of BP from a non-dipper to dipper type in SHR/NDmcr-cp(+/+) rats, a model of metabolic syndrome.44 Taken together, these data strongly indicate that BP reduction by an SGLT2 inhibitor is associated with the restoration of a disrupted circadian rhythm of BP from a non-dipper to dipper pattern in hypertensive subjects with impaired glucose metabolism and insulin resistance.
Possible mechanisms underlying the SGLT2 inhibitor-induced normalization of the BP dipping pattern
Body weight
Body weight gain is associated with impaired glucose homeostasis as well as BP regulation, including a disrupted circadian rhythm of BP.45, 46 Moreover, it has been shown that visceral fat accumulation is an independent risk factor for the disruption of the circadian rhythm of BP in Japanese patients.47 Clinical studies have shown that treatment with SGLT2 inhibitors decreased body weight in subjects with type 2 diabetes.35, 48, 49 Moreover, the SGLT2 inhibitor-induced reduction in body weight is associated with reduction in body fat mass.50, 51 Therefore, it is possible that SGLT2 inhibitor-induced changes in body weight are accompanied by improvement in the circadian rhythm of BP in subjects with type 2 diabetes. However, it has been shown that the SGLT2 inhibitor-induced reduction in BP was not correlated with body weight changes.51, 52 Furthermore, BP reduction and BP circadian rhythm improvement were not associated with body weight reduction during treatment with SGLT2 inhibitors in obese animals.39, 44 Therefore, SGLT2 inhibitor-induced BP reduction and BP dipping pattern improvement may not be solely explained by body weight reduction.
Blood glucose
The prevalence of a non-dipping BP pattern was significantly higher in subjects with impaired glucose tolerance.53 Glycated hemoglobin levels exhibited a strong association with the variability of nocturnal SBP and DBP in patients with type 2 diabetes.54 However, the SGLT2 inhibitor-induced reduction in BP was not correlated with glycated hemoglobin levels.51, 52 Furthermore, the potential relationship between blood glucose levels and changes in the dipping pattern of BP has not been reported in diabetic patients whose blood sugar levels are controlled by any other antidiabetic drugs. Collectively, it seems unlikely that the improvement in circadian rhythm is mediated by blood sugar control.
Insulin sensitivity
Insulin induces BP elevation through multiple mechanisms, and insulin resistance has a pivotal role in the pathogenesis of type 2 diabetes mellitus with CV complications as well as a non-dipping pattern of BP.5, 55 Blood glucose control with an SGLT2 inhibitor is independently mediated by β-cell function and endogenous insulin.5 It has been shown that treatment with an SGLT2 inhibitor improves insulin resistance in patients with type 2 diabetes.56 Euglycemic insulin clamp test results have also indicated that dapagliflozin treatment for 2 weeks improved whole-body insulin-induced glucose uptake by 20–25%.57 We also showed that treatment with SGLT2 inhibitors significantly improved insulin sensitivity in an oral glucose tolerance test in obese rats.39, 44 Thus it is possible that the improvement in insulin resistance contributes to BP reduction by an SGLT2 inhibitor. Further studies will be needed to determine the direct relationship between insulin resistance improvement and BP reduction during treatment with an SGLT2 inhibitor.
Natriuresis
Sodium retention has an important role in the development of hypertension in patients with diabetes58 and metabolic syndrome59 and contributes to the development of a disrupted circadian rhythm of BP.60 Of note, a non-dipping pattern of BP can be transformed to a dipping pattern of BP by a sodium-restricted diet61 or diuretics62 in sodium-sensitive hypertensive patients. Lambers et al.35 showed that dapagliflozin caused a 7% reduction in plasma volume in patients with type 2 diabetes, indicating a diuretic effect possibly owing to enhanced sodium excretion or to osmotic diuresis as a result of increased urinary glucose excretion. It has also been shown that urinary sodium excretion tended to be increased in the early period of canagliflozin administration in patients with type 2 diabetes.63 These effects of an SGLT2 inhibitor are similar to those of diuretics such as chlorothiazide, which increases urinary sodium excretion for only a few days because of a compensatory mechanism against body fluid loss.63 A case report of a patient with type 2 diabetes showed that a 2-week regimen of the SGLT2 inhibitor dapagliflozin changed the BP pattern from a non-dipper to a dipper type possibly resulting from the increased urinary excretion of sodium. In this study, the sodium excretion rate rose from 0.37% at day 0 to 0.68% at day 8, although this change was not statistically significant.11
In OLETF rats with type 2 diabetes that were treated with a high-salt diet, empagliflozin-induced changes in the dipping pattern of BP were associated with increased urinary sodium excretion.39 Moreover, the SGLT2 inhibitor luseogliflozin-induced shifting of the circadian rhythm of BP from a non-dipper to a dipper pattern was associated with increased urinary excretion of sodium in SHR/NDmcr-cp(+/+) rats with metabolic syndrome. In this study, luseogliflozin treatment caused a significantly negative sodium balance in comparison with the vehicle-treated animals, suggesting a reduction in sodium retention by treatment with an SGLT2 inhibitor.44 Based on these data, it can be speculated that SGLT2 inhibitors induce natriuresis, which has an important role in the improvement in the circadian rhythm of BP in subjects with type 2 diabetes. Recent studies have suggested that sodium is accumulated in the muscle and skin in patients with hypertension64 and heart failure,65, 66 which is attenuated by treatment with a diuretic.66 Preliminary studies by Schmieder et al.67 have shown that dapagliflozin treatment caused a significant decrease in the skin tissue content of sodium in type 2 diabetic patients. Therefore, it can be hypothesized that SGLT2 inhibition has the potential to decrease sodium levels in the extracellular space, which contributes to the improvement in the dipping pattern of BP and the associated cardiovascular mortality.
Arterial stiffness
The non-dipping type of BP is associated with increases in the index of arterial stiffness,68 greater intima-media thickness in the carotid bifurcation and average intima-media thickness,69 all of which are related to the risk of CVD.70, 71 Interestingly, empagliflozin significantly decreased carotid-radial/femoral pulse wave velocity in patients with type 1 diabetes, suggesting an improvement in arterial stiffness.72 Furthermore, empagliflozin reduced the pulse and mean arterial pressures and caused a greater reduction in double product while inducing a trend of reduced ambulatory arterial stiffness index values in patients with type 2 diabetes.73 These data suggest that SGLT2 inhibitors improve arterial stiffness and vascular resistance in patients with type 2 diabetes. However, no studies have investigated a possible contribution of arterial stiffness improvement to the normalization of BP circadian rhythm during treatment with an SGLT2 inhibitor.
Other mechanisms
It has been shown that non-dipping nocturnal BP is associated with urinary albumin excretion in patients with type 2 diabetes.74 In the EMPA-REG OUTCOME trial, patients with type 2 diabetes who were treated with empagliflozin had a significantly lower risk of progression of microalbuminuria to macroalbuminuria.75 Moreover, Cherney et al.76 showed that, regardless of microalbuminuria or macroalbuminuria, empagliflozin caused a clinically meaningful reduction in the urinary albumin/creatinine ratio in patients with type 2 diabetes. A post hoc analysis of phase III clinical trials has shown that dapagliflozin effectively reduced albuminuria in hypertensive patients with type 2 diabetes who were treated with renin–angiotensin system inhibitors.77 In diabetic Akita mice, empagliflozin reduced both albuminuria and glomerular hyperfiltration.78 High levels of plasma triglycerides and low levels of high-density lipoprotein-cholesterol were also associated with non-dipper hypertension in subjects with metabolic abnormalities.43 Several clinical studies have shown that SGLT2 inhibitors slightly but significantly decrease triglycerides.3, 79 Serum uric acid levels have also independently been associated with type 2 diabetes,80 CVD81 and non-dipper hypertension.82 Recent clinical trials have demonstrated that SGLT2 inhibitors with either monotherapy3, 83 or add on therapy79 reduced the levels of serum uric acid (~10–15%) in patients with type 2 diabetes. However, the specific contributions of reductions in urinary albumin excretion, triglycerides and serum uric acid to the normalization of BP circadian rhythm have not yet been investigated during treatment with an SGLT2 inhibitor.
Conclusions
Recent clinical trials have indicated that treatment with an SGLT2 inhibitor elicits beneficial outcomes in terms of CV events in patients with type 2 diabetes. Emerging data have also shown that SGLT2 inhibitors not only decrease BP but also improve a disrupted circadian rhythm of BP. Thus it can be postulated that the beneficial effects of SGLT2 inhibitors on CV events are associated with the improvement in BP circadian rhythm. However, further investigation should be undertaken to determine the precise mechanism involved (Figure 1).
References
Fox CS, Pencina MJ, Wilson PW, Paynter NP, Vasan RS, D'Agostino RB Sr . Lifetime risk of cardiovascular disease among individuals with and without diabetes stratified by obesity status in the Framingham heart study. Diabetes Care 2008; 31: 1582–1584.
Kabakov E, Norymberg C, Osher E, Koffler M, Tordjman K, Greenman Y, Stern N . Prevalence of hypertension in type 2 diabetes mellitus: impact of the tightening definition of high blood pressure and association with confounding risk factors. J Cardiometab Syndr 2006; 1: 95–101.
Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, Mattheus M, Devins T, Johansen OE, Woerle HJ, Broedl UC, Inzucchi SE, Investigators E-RO. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 2015; 373: 2117–2128.
Mogi M, Horiuchi M . To overcome two diseases with one pill. Hypertens Res 2016; 39: 399–400.
Laakso M, Kuusisto J . Insulin resistance and hyperglycaemia in cardiovascular disease development. Nat Rev Endocrinol 2014; 10: 293–302.
Filippatos TD, Tsimihodimos V, Elisaf MS . Mechanisms of blood pressure reduction with sodium-glucose co-transporter 2 (SGLT2) inhibitors. Expert Opin Pharmacother 2016; 17: 1581–1583.
White WB . Ambulatory blood pressure monitoring: dippers compared with non-dippers. Blood Press Monit 2000; 5 (Suppl 1): S17–S23.
Ohkubo T, Hozawa A, Yamaguchi J, Kikuya M, Ohmori K, Michimata M, Matsubara M, Hashimoto J, Hoshi H, Araki T, Tsuji I, Satoh H, Hisamichi S, Imai Y . Prognostic significance of the nocturnal decline in blood pressure in individuals with and without high 24-h blood pressure: the Ohasama study. J Hypertens 2002; 20: 2183–2189.
Ohkubo T, Imai Y, Tsuji I, Nagai K, Watanabe N, Minami N, Kato J, Kikuchi N, Nishiyama A, Aihara A, Sekino M, Satoh H, Hisamichi S . Relation between nocturnal decline in blood pressure and mortality. The Ohasama Study. Am J Hypertens 1997; 10: 1201–1207.
Tikkanen I, Narko K, Zeller C, Green A, Salsali A, Broedl UC, Woerle HJ . Investigators E-RB. Empagliflozin reduces blood pressure in patients with type 2 diabetes and hypertension. Diabetes Care 2015; 38: 420–428.
Mori H, Okada Y, Kawaguchi M, Tanaka Y . A case of type 2 diabetes with a change from a non-dipper to a dipper blood pressure pattern by dapagliflozin. J UOEH 2016; 38: 149–153.
Hassler C, Burnier M . Circadian variations in blood pressure: implications for chronotherapeutics. Am J Cardiovasc Drugs 2005; 5: 7–15.
Hermida RC, Ayala DE, Portaluppi F . Circadian variation of blood pressure: the basis for the chronotherapy of hypertension. Adv Drug Deliv Rev 2007; 59: 904–922.
Della Mea P, Lupia M, Bandolin V, Guzzon S, Sonino N, Vettor R, Fallo F . Adiponectin, insulin resistance, and left ventricular structure in dipper and nondipper essential hypertensive patients. Am J Hypertens 2005; 18: 30–35.
Cuspidi C, Meani S, Salerno M, Valerio C, Fusi V, Severgnini B, Lonati L, Magrini F, Zanchetti A . Cardiovascular target organ damage in essential hypertensives with or without reproducible nocturnal fall in blood pressure. J Hypertens 2004; 22: 273–280.
Fogari R, Zoppi A, Malamani GD, Lazzari P, Destro M, Corradi L . Ambulatory blood pressure monitoring in normotensive and hypertensive type 2 diabetes. Prevalence of impaired diurnal blood pressure patterns. Am J Hypertens 1993; 6: 1–7.
Pierdomenico SD, Pierdomenico AM, Coccina F, Lapenna D, Porreca E . Circadian blood pressure changes and cardiovascular risk in elderly-treated hypertensive patients. Hypertens Res 2016; 39: 805–811.
Fagard RH, Thijs L, Staessen JA, Clement DL, De Buyzere ML, De Bacquer DA . Night-day blood pressure ratio and dipping pattern as predictors of death and cardiovascular events in hypertension. J Hum Hypertens 2009; 23: 645–653.
Sturrock ND, George E, Pound N, Stevenson J, Peck GM, Sowter H . Non-dipping circadian blood pressure and renal impairment are associated with increased mortality in diabetes mellitus. Diabet Med 2000; 17: 360–364.
Ayala DE, Moya A, Crespo JJ, Castineira C, Dominguez-Sardina M, Gomara S, Sineiro E, Mojon A, Fontao MJ, Hermida RC, Hygia Project I. Circadian pattern of ambulatory blood pressure in hypertensive patients with and without type 2 diabetes. Chronobiol Int 2013; 30: 99–115.
Haffner SM, Lehto S, Ronnemaa T, Pyorala K, Laakso M . Mortality from coronary heart disease in subjects with type 2 diabetes and in nondiabetic subjects with and without prior myocardial infarction. N Engl J Med 1998; 339: 229–234.
Group AC, Patel A, MacMahon S, Chalmers J, Neal B, Billot L, Woodward M, Marre M, Cooper M, Glasziou P, Grobbee D, Hamet P, Harrap S, Heller S, Liu L, Mancia G, Mogensen CE, Pan C, Poulter N, Rodgers A, Williams B, Bompoint S, de Galan BE, Joshi R, Travert F . Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med 2008; 358: 2560–2572.
Duckworth W, Abraira C, Moritz T, Reda D, Emanuele N, Reaven PD, Zieve FJ, Marks J, Davis SN, Hayward R, Warren SR, Goldman S, McCarren M, Vitek ME, Henderson WG, Huang GD, Investigators V. Glucose control and vascular complications in veterans with type 2 diabetes. N Engl J Med 2009; 360: 129–139.
Salsali A, Kim G, Woerle HJ, Broedl UC, Hantel S . Cardiovascular safety of empagliflozin in patients with type 2 diabetes: a meta-analysis of data from randomized placebo-controlled trials. Diabetes Obes Metab 2016; 18: 1034–1040.
Sonesson C, Johansson PA, Johnsson E, Gause-Nilsson I . Cardiovascular effects of dapagliflozin in patients with type 2 diabetes and different risk categories: a meta-analysis. Cardiovasc Diabetol 2016; 15: 37.
Neal B, Perkovic V, de Zeeuw D, Mahaffey KW, Fulcher G, Stein P, Desai M, Shaw W, Jiang J, Vercruysse F, Meininger G, Matthews D . Rationale, design, and baseline characteristics of the Canagliflozin Cardiovascular Assessment Study (CANVAS)–a randomized placebo-controlled trial. Am Heart J 2013; 166: 217–223 e211.
Clinicaltrials.gov. Multicenter trial to evaluate the effect of dapagliflozin on the incidence of cardiovascular events (DECLARE-TIMI58). Accessed on 08 January 2016 https://clinicaltrials.gov/ct2/show/NCT01730534.
Singh JS, Fathi A, Vickneson K, Mordi I, Mohan M, Houston JG, Pearson ER, Struthers AD, Lang CC . Research into the effect Of SGLT2 inhibition on left ventricular remodelling in patients with heart failure and diabetes mellitus (REFORM) trial rationale and design. Cardiovasc Diabetol 2016; 15: 97.
Clinicaltrials.gov. Cardiovascular outcomes following ertugliflozin treatment in type 2 diabetes mellitus participants with vascular disease, the VERTIS CV Study (MK-8835-004). Accessed on 09 September 2016 https://clinicaltrials.gov/ct2/show/NCT01986881.
Lin B, Koibuchi N, Hasegawa Y, Sueta D, Toyama K, Uekawa K, Ma M, Nakagawa T, Kusaka H, Kim-Mitsuyama S . Glycemic control with empagliflozin, a novel selective SGLT2 inhibitor, ameliorates cardiovascular injury and cognitive dysfunction in obese and type 2 diabetic mice. Cardiovasc Diabetol 2014; 13: 148.
Zaccardi F, Webb DR, Htike ZZ, Youssef D, Khunti K, Davies MJ . Efficacy and safety of sodium-glucose co-transporter-2 inhibitors in type 2 diabetes mellitus: systematic review and network meta-analysis. Diabetes Obes Metab 2016; 18: 783–794.
Ng CM, Yiu SF, Choi KL, Choi CH, Ng YW, Tiu SC . Prevalence and significance of white-coat hypertension and masked hypertension in type 2 diabetics. Hong Kong Med J 2008; 14: 437–443.
Eguchi K, Pickering TG, Hoshide S, Ishikawa J, Ishikawa S, Schwartz JE, Shimada K, Kario K . Ambulatory blood pressure is a better marker than clinic blood pressure in predicting cardiovascular events in patients with/without type 2 diabetes. Am J Hypertens 2008; 21: 443–450.
Tamura K, Wakui H, Azushima K, Uneda K, Umemura S . Circadian blood pressure rhythm as a possible key target of SGLT2 inhibitors used for the treatment of Type 2 diabetes. Hypertens Res 2016; 39: 396–398.
Lambers Heerspink HJ, de Zeeuw D, Wie L, Leslie B, List J . Dapagliflozin a glucose-regulating drug with diuretic properties in subjects with type 2 diabetes. Diabetes Obes Metab 2013; 15: 853–862.
Amin NB, Wang X, Mitchell JR, Lee DS, Nucci G, Rusnak JM . Blood pressure-lowering effect of the sodium glucose co-transporter-2 inhibitor ertugliflozin, assessed via ambulatory blood pressure monitoring in patients with type 2 diabetes and hypertension. Diabetes Obes Metab 2015; 17: 805–808.
Chilton R, Tikkanen I, Crowe S, Johansen OE, Broedl UC, Woerle HJ, Hach T . 4b.03: empagliflozin reduces systolic blood pressure in dipper and non-dipper patients with type 2 diabetes and hypertension. J Hypertens 2015; 33 (Suppl 1): e53.
Weber MA, Mansfield TA, Cain VA, Iqbal N, Parikh S, Ptaszynska A . Blood pressure and glycaemic effects of dapagliflozin vs. placebo in patients with type 2 diabetes on combination antihypertensive therapy: a randomised, double-blind, placebo-controlled, phase 3 study. Lancet Diabetes Endocrinol 2016; 4: 211–220.
Takeshige Y, Fujisawa Y, Rahman A, Kittikulsuth W, Nakano D, Mori H, Masaki T, Ohmori K, Kohno M, Ogata H, Nishiyama A . A sodium-glucose co-transporter 2 inhibitor empagliflozin prevents abnormality of circadian rhythm of blood pressure in salt-treated obese rats. Hypertens Res 2016; 39: 415–422.
Guidelines (JSH 2014). Chapter 7. Hypertension complicated by other diseases. Hypertens Res 2014; 37: 315–324.
Kotsis V, Stabouli S, Papakatsika S, Rizos Z, Parati G . Mechanisms of obesity-induced hypertension. Hypertens Res 2010; 33: 386–393.
Shimizu I, Yoshida Y, Minamino T . A role for circadian clock in metabolic disease. Hypertens Res 2016; 39: 483–491.
Ukkola O, Vasunta RL, Kesaniemi YA . Non-dipping pattern in ambulatory blood pressure monitoring is associated with metabolic abnormalities in a random sample of middle-aged subjects. Hypertens Res 2009; 32: 1022–1027.
Rahman A, Kittikulsuth W, Fujisawa Y, Sufiun A, Rafiq K, Hitomi H, Nakano D, Sohara E, Uchida S, Nishiyama A . Effects of diuretics on sodium-dependent glucose cotransporter 2 inhibitor-induced changes in blood pressure in obese rats suffering from the metabolic syndrome. J Hypertens 2016; 34: 893–906.
Senador D, Shewale S, Irigoyen MC, Elased KM, Morris M . Effects of restricted fructose access on body weight and blood pressure circadian rhythms. Exp Diabetes Res 2012; 2012: 459087.
Maury E, Ramsey KM, Bass J . Circadian rhythms and metabolic syndrome: from experimental genetics to human disease. Circ Res 2010; 106: 447–462.
Masaki T, Anan F, Yoshimatsu H . Visceral fat accumulation is associated with circadian blood pressure in Japanese patients with impaired glucose tolerance. Diabetes Care 2011; 34: e32.
Blonde L, Stenlof K, Fung A, Xie J, Canovatchel W, Meininger G . Effects of canagliflozin on body weight and body composition in patients with type 2 diabetes over 104 weeks. Postgrad Med 2016; 128: 371–380.
Seino Y, Sasaki T, Fukatsu A, Ubukata M, Sakai S, Samukawa Y . Efficacy and safety of luseogliflozin as monotherapy in Japanese patients with type 2 diabetes mellitus: a randomized, double-blind, placebo-controlled, phase 3 study. Curr Med Res Opin 2014; 30: 1245–1255.
Yokono M, Takasu T, Hayashizaki Y, Mitsuoka K, Kihara R, Muramatsu Y, Miyoshi S, Tahara A, Kurosaki E, Li Q, Tomiyama H, Sasamata M, Shibasaki M, Uchiyama Y . SGLT2 selective inhibitor ipragliflozin reduces body fat mass by increasing fatty acid oxidation in high-fat diet-induced obese rats. Eur J Pharmacol 2014; 727: 66–74.
Bolinder J, Ljunggren O, Kullberg J, Johansson L, Wilding J, Langkilde AM, Sugg J, Parikh S . Effects of dapagliflozin on body weight, total fat mass, and regional adipose tissue distribution in patients with type 2 diabetes mellitus with inadequate glycemic control on metformin. J Clin Endocrinol Metab 2012; 97: 1020–1031.
Oliva RV, Bakris GL . Blood pressure effects of sodium-glucose co-transport 2 (SGLT2) inhibitors. J Am Soc Hypertens 2014; 8: 330–339.
Li L, Soonthornpun S, Chongsuvivatwong V . Association between circadian rhythm of blood pressure and glucose tolerance status in normotensive, non-diabetic subjects. Diabetes Res Clin Pract 2008; 82: 359–363.
van Bruggen EF, Kremer J . Electron microscopy of bovine and human cervical mucus. Int J Fertil 1970; 15: 50–57.
Anan F, Takahashi N, Ooie T, Yufu K, Saikawa T, Yoshimatsu H . Role of insulin resistance in nondipper essential hypertensive patients. Hypertens Res 2003; 26: 669–676.
Ferrannini E, Muscelli E, Frascerra S, Baldi S, Mari A, Heise T, Broedl UC, Woerle HJ . Metabolic response to sodium-glucose cotransporter 2 inhibition in type 2 diabetic patients. J Clin Invest 2014; 124: 499–508.
Merovci A, Solis-Herrera C, Daniele G, Eldor R, Fiorentino TV, Tripathy D, Xiong J, Perez Z, Norton L, Abdul-Ghani MA, DeFronzo RA . Dapagliflozin improves muscle insulin sensitivity but enhances endogenous glucose production. J Clin Invest 2014; 124: 509–514.
Brands MW, Manhiani MM . Sodium-retaining effect of insulin in diabetes. Am J Physiol Regul Integr Comp Physiol 2012; 303: R1101–R1109.
El-Atat FA, Stas SN, McFarlane SI, Sowers JR . The relationship between hyperinsulinemia, hypertension and progressive renal disease. J Am Soc Nephrol 2004; 15: 2816–2827.
de la Sierra A, Redon J, Banegas JR, Segura J, Parati G, Gorostidi M, de la Cruz JJ, Sobrino J, Llisterri JL, Alonso J, Vinyoles E, Pallares V, Sarria A, Aranda P, Ruilope LM, Spanish Society of Hypertension Ambulatory Blood Pressure Monitoring Registry Investigators. Prevalence and factors associated with circadian blood pressure patterns in hypertensive patients. Hypertension 2009; 53: 466–472.
Uzu T, Ishikawa K, Fujii T, Nakamura S, Inenaga T, Kimura G . Sodium restriction shifts circadian rhythm of blood pressure from nondipper to dipper in essential hypertension. Circulation 1997; 96: 1859–1862.
Uzu T, Kimura G . Diuretics shift circadian rhythm of blood pressure from nondipper to dipper in essential hypertension. Circulation 1999; 100: 1635–1638.
Iijima H, Kifuji T, Maruyama N, Inagaki N . Pharmacokinetics, pharmacodynamics, and safety of canagliflozin in japanese patients with type 2 diabetes mellitus. Adv Ther 2015; 32: 768–782.
Kopp C, Linz P, Dahlmann A, Hammon M, Jantsch J, Muller DN, Schmieder RE, Cavallaro A, Eckardt KU, Uder M, Luft FC, Titze J . 23Na magnetic resonance imaging-determined tissue sodium in healthy subjects and hypertensive patients. Hypertension 2013; 61: 635–640.
Frohlich ED, Susic D . Sodium and its multiorgan targets. Circulation 2011; 124: 1882–1885.
Hammon M, Grossmann S, Linz P, Kopp C, Dahlmann A, Garlichs C, Janka R, Cavallaro A, Luft FC, Uder M, Titze J . 23Na magnetic resonance imaging of the lower leg of acute heart failure patients during diuretic treatment. PLoS ONE 2015; 10: e0141336.
Schmieder R, Ott C, Linz P, Jumar A, Friedrich S, Titze J, Hammon M, Uder M, Kistner I . Os 12-03 Sglt-2-inhibition with dapagliflozin reduces tissue sodium content. J Hypertens 2016; 34 (Suppl 1) ISH 2016 Abstract Book e76.
Lekakis JP, Zakopoulos NA, Protogerou AD, Papaioannou TG, Kotsis VT, Pitiriga V, Tsitsirikos MD, Stamatelopoulos KS, Papamichael CM, Mavrikakis ME . Arterial stiffness assessed by pulse wave analysis in essential hypertension: relation to 24-h blood pressure profile. Int J Cardiol 2005; 102: 391–395.
Salvetti M, Muiesan ML, Rizzoni D, Bettoni G, Monteduro C, Corbellini C, Viola S, Agabiti-Rosei E . Night time blood pressure and cardiovascular structure in a middle-aged general population in northern Italy: the Vobarno Study. J Hum Hypertens 2001; 15: 879–885.
Phillips RA, Butkevich A, Sheinart KF, Tuhrim S . Dipping is superior to cusums analysis in assessment of the risk of stroke in a case-control study. Am J Hypertens 2001; 14: 649–652.
Kikuya M, Ohkubo T, Asayama K, Metoki H, Obara T, Saito S, Hashimoto J, Totsune K, Hoshi H, Satoh H, Imai Y . Ambulatory blood pressure and 10-year risk of cardiovascular and noncardiovascular mortality: the Ohasama study. Hypertension 2005; 45: 240–245.
Cherney DZ, Perkins BA, Soleymanlou N, Har R, Fagan N, Johansen OE, Woerle HJ, von Eynatten M, Broedl UC . The effect of empagliflozin on arterial stiffness and heart rate variability in subjects with uncomplicated type 1 diabetes mellitus. Cardiovasc Diabetol 2014; 13: 28.
Chilton R, Tikkanen I, Cannon CP, Crowe S, Woerle HJ, Broedl UC, Johansen OE . Effects of empagliflozin on blood pressure and markers of arterial stiffness and vascular resistance in patients with type 2 diabetes. Diabetes Obes Metab 2015; 17: 1180–1193.
Equiluz-Bruck S, Schnack C, Kopp HP, Schernthaner G . Nondipping of nocturnal blood pressure is related to urinary albumin excretion rate in patients with type 2 diabetes mellitus. Am J Hypertens 1996; 9: 1139–1143.
Wanner C, Inzucchi SE, Lachin JM, Fitchett D, von Eynatten M, Mattheus M, Johansen OE, Woerle HJ, Broedl UC, Zinman B, Investigators E-RO. Empagliflozin and progression of kidney disease in type 2 diabetes. N Engl J Med 2016; 375: 323–334.
Cherney D, Lund SS, Perkins BA, Groop PH, Cooper ME, Kaspers S, Pfarr E, Woerle HJ, von Eynatten M . The effect of sodium glucose cotransporter 2 inhibition with empagliflozin on microalbuminuria and macroalbuminuria in patients with type 2 diabetes. Diabetologia 2016; 59: 1860–1870.
Heerspink HJ, Johnsson E, Gause-Nilsson I, Cain VA, Sjostrom CD . Dapagliflozin reduces albuminuria in patients with diabetes and hypertension receiving renin-angiotensin blockers. Diabetes Obes Metab 2016; 18: 590–597.
Hagbarth KE, Vallbo AB . Afferent response to mechanical stimulation of muscle receptors in man. Acta Soc Med Ups 1967; 72: 102–104.
Bailey CJ, Gross JL, Pieters A, Bastien A, List JF . Effect of dapagliflozin in patients with type 2 diabetes who have inadequate glycaemic control with metformin: a randomised, double-blind, placebo-controlled trial. Lancet 2010; 375: 2223–2233.
Causevic A, Semiz S, Macic Dzankovic A, Cico B, Dujic T, Malenica M, Bego T . Relevance of uric Acid in progression of type 2 diabetes mellitus. Bosn J Basic Med Sci 2010; 10: 54–59.
Culleton BF, Larson MG, Kannel WB, Levy D . Serum uric acid and risk for cardiovascular disease and death: the Framingham Heart Study. Ann Intern Med 1999; 131: 7–13.
Turak O, Ozcan F, Tok D, Isleyen A, Sokmen E, Tasoglu I, Aydogdu S, Sen N, McFann K, Johnson RJ, Kanbay M . Serum uric acid, inflammation, and nondipping circadian pattern in essential hypertension. J Clin Hypertens (Greenwich) 2013; 15: 7–13.
Ferrannini E, Ramos SJ, Salsali A, Tang W, List JF . Dapagliflozin monotherapy in type 2 diabetic patients with inadequate glycemic control by diet and exercise: a randomized, double-blind, placebo-controlled, phase 3 trial. Diabetes Care 2010; 33: 2217–2224.
Acknowledgements
This work was supported by the Japan Society for the Promotion of Science (JSPS) Grants-in-Aid for Scientific Research (KAKENHI) (26460343 to Akira Nishiyama).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Rahman, A., Hitomi, H. & Nishiyama, A. Cardioprotective effects of SGLT2 inhibitors are possibly associated with normalization of the circadian rhythm of blood pressure. Hypertens Res 40, 535–540 (2017). https://doi.org/10.1038/hr.2016.193
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.193
Keywords
This article is cited by
-
Paradigm shift in heart failure treatment: are cardiologists ready to use gliflozins?
Heart Failure Reviews (2022)
-
Inverted circadian variation of arterial pressure in a geriatric patient: an indicator of autonomic dysfunction
BMC Geriatrics (2021)
-
Impaired nocturnal blood pressure dipping in patients with type 2 diabetes mellitus
Hypertension Research (2019)
-
Hypertension with diabetes mellitus complications
Hypertension Research (2018)
-
Clinical features and therapeutic perspectives on hypertension in diabetics
Hypertension Research (2018)