Abstract
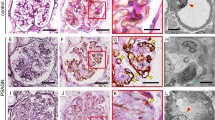
The mechanisms of hypertensive nephrosclerosis are not fully understood. In experimental models of the disease, inflammatory reactions such as macrophage infiltration play an important role. In human hypertensive nephrosclerosis, however, there have been few studies examining the role of inflammation histologically. We investigated whether the number of infiltrating macrophages was increased in human hypertensive nephrosclerosis, and evaluated the effects of a blockade of the renin-angiotensin system on clinical and histological findings. We examined macrophage infiltration using immunohistochemistry in renal biopsy specimens obtained from 16 patients with hypertensive nephrosclerosis, 5 patients with IgA nephropathy, 5 patients with membranous nephropathy, and 5 patients with minimal change nephrotic syndrome. The number of infiltrating macrophages in glomeruli was significantly larger in the patients with hypertensive nephrosclerosis than in those with minimal change nephrotic syndrome. The patients with hypertensive nephrosclerosis were divided into groups based on their use of antihypertensive agents at the time of renal biopsy. We investigated the effects of antihypertensive agents on clinical findings, macrophage infiltration, and monocyte chemoattractant protein-1 expression. There was no difference in clinical findings between the hypertensive groups. The numbers of infiltrating macrophages and monocyte chemoattractant protein-1−positive cells in glomeruli were significantly smaller in patients treated with an angiotensin-converting enzyme inhibitor or angiotensin II type 1 receptor blocker, whereas calcium channel blockers had no influence on histological findings. In conclusion, inflammation is involved in the progression of human hypertensive nephrosclerosis and the inflammatory process is inhibited by blocking the renin-angiotensin system.
Similar content being viewed by others
Article PDF
References
USRDS: United States Renal Data System 2002 Annual Data Report: incidence and prevalence. Am J Kidney Dis 2003; 41 ( Suppl 2): S41–S56.
Mann JFE, Hilgers KF, Veelken R, Geiger H, Schmieder RE, Luft FC : Effect of antihypertensive therapy on progression of non-diabetic renal disease. Clin Nephrol 1992; 38: S74–S77.
Ikee R, Kobayashi S, Saigusa T, et al: Impact of hypertension and hypertension-related vascular lesions in IgA nephropathy. Hypertens Res 2006; 29: 15–22.
Johnson RJ, Alpers CE, Yoshimura A, et al: Renal injury from angiotensin II–mediated hypertension. Hypertension 1992; 19: 464–474.
Hilgers KF, Hartner A, Porst M, et al: Monocyte chemoattractant protein-1 and macrophage infiltration in hypertensive kidney injury. Kidney Int 2000; 58: 2408–2419.
Mezzano S, Droguett A, Burgos ME, et al: Renin-angiotensin system activation and interstitial inflammation in human diabetic nephropathy. Kidney Int Suppl 2003; 86: S64–S70.
Hilgers KF, Hartner A, Porst M, Veelken R, Mann JFE : Angiotensin II type 1 receptor blockade prevents lethal malignant hypertension. Relation to kidney inflammation. Circulation 2001; 104: 1436–1440.
Lewis EJ, Hunsicker LG, Clarke WR, et al: Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001; 345: 851–860.
Ruggenenti P, Perna A, Gherardi G, et al: Renoprotective properties of ACE-inhibition in non-diabetic nephropathies with non-nephrotic proteinuria. Lancet 1999; 354: 359–364.
Hotta O, Yusa N, Ooyama M, Taguma Y : Urinary macrophage counts and ratio to T lymphocytes: possible use in differential diagnosis and management of glomerular disease. J Clin Lab Anal 1996; 10: 205–208.
Oda T, Hotta O, Taguma Y, et al: Clinicopathological significance of intratubular giant macrophages in progressive glomerulonephritis. Kidney Int 1998; 53: 1190–1200.
Furuta T, Saito T, Ootaka T, et al: The role of macrophages in diabetic glomerulosclerosis. Am J Kidney Dis 1993; 21: 480–485.
Rodrigues-Iturbe B, Vaziri ND, Herrera-Acosta J, Johnson RJ : Oxidative stress, renal infiltration of immune cells and salt-sensitive hypertension: all for one and one for all. Am J Physiol Renal Physiol 2004; 286: F606–F616.
Arima S, Kohagura K, Abe M, Ito S : Mechanisms that control glomerular hemodynamics. Clin Exp Nephrol 2001; 5: 55–61.
Gruden G, Setti G, Hayward A, et al: Mechanical stretch induces monocyte chemoattractant activity via an NF-κB–dependent monocyte chemoattractant protein-1−mediated pathway in human mesangial cells: inhibition by rosiglitazone. J Am Soc Nephrol 2005; 16: 688–696.
Ishimitsu T, Kameda T, Akashiba A, et al: Effects of valsartan on the progression of chronic renal insufficiency in patients with nondiabetic renal diseases. Hypertens Res 2005; 28: 865–870.
Agodoa LY, Appel L, Bakris GL, et al, for the African American Study of Kidney Disease and Hypertension (AASK) Group: Effect of ramipril vs amlodipine on renal outcomes in hypertensive nephrosclerosis: a randomized controlled trial. JAMA 2001; 285: 2719–2728.
Ruggenenti P, Fassi A, Ilieva AP, et al, for the Bergamo Nephrologic Diabetes Complications Trial (BENEDICT) Investigators : Preventing microalbuminuria in type 2 diabetes. N Engl J Med 2004; 351: 1941–1951.
Iino Y, Hayashi M, Kawamura T, et al: Renoprotective effect of losartan in comparison to amlodipine in patients with chronic kidney disease and hypertension—a report of the Japanese Losartan Therapy Intended for the Global Renal Protection in Hypertensive Patients (JLIGHT) study. Hypertens Res 2004; 27: 21–30.
Prodjosudjadi W, Gerritsma JS, van Es LA, Daha MR, Bruijn JA : Monocyte chemoattractant protein-1 in normal and diseased human kidneys: an immunohistochemical analysis. Clin Nephrol 1995; 44: 148–155.
Capers Q IV, Alexander RW, Lou P, et al: Monocyte chemoattractant protein-1 expression in aortic tissues of hypertensive rats. Hypertension 1997; 30: 1397–1402.
Chen XL, Tummala PE, Olbrych MT, Alexander RW, Medford RM : Angiotensin II induces monocyte chemoattractant protein-1 gene expression in rat vascular smooth muscle cells. Circ Res 1998; 83: 952–959.
Kim S, Ohta K, Hamaguchi A, et al: Contribution of renal angiotensin II type I receptor to gene expressions in hypertension-induced renal injury. Kidney Int 1994; 46: 1346–1358.
Kagami S, Border WA, Miller DE, et al: Angiotensin II stimulates extracellular matrix protein synthesis through induction of transforming growth factor-beta expression in rat glomerular mesangial cells. J Clin Invest 1994; 93: 2431–2437.
Rodrigues-Iturbe B, Johnson RJ : Role of inflammatory cells in the kidney in the induction and maintenance of hypertension. Nephrol Dial Transplant 2006; 21: 260–263.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Imakiire, T., Kikuchi, Y., Yamada, M. et al. Effects of Renin-Angiotensin System Blockade on Macrophage Infiltration in Patients with Hypertensive Nephrosclerosis. Hypertens Res 30, 635–642 (2007). https://doi.org/10.1291/hypres.30.635
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.30.635
Keywords
This article is cited by
-
Toll-like receptor-4 deficiency alleviates chronic intermittent hypoxia-induced renal injury, inflammation, and fibrosis
Sleep and Breathing (2019)
-
Toll-like Receptor 4 Deficiency Reduces Oxidative Stress and Macrophage Mediated Inflammation in Hypertensive Kidney
Scientific Reports (2017)
-
Prognostic value of morphologic and morphometric analyses in IgA nephropathy biopsies
Translational Medicine Communications (2016)
-
Subclinical nephrosclerosis is linked to left ventricular hypertrophy independent of classical atherogenic factors
Hypertension Research (2014)
-
Innate Immunity in Hypertension
Current Hypertension Reports (2014)