Abstract
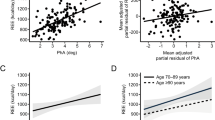
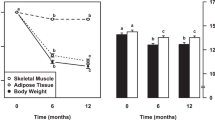
Under basal resting conditions muscle metabolism is reduced, whereas metabolism increases with physical activity. We wished to determine whether there was an association between resting energy expenditure (REE) and total energy expenditure (TEE) in peritoneal dialysis (PD) patients and lean body mass (LBM). We determined REE and TEE by recently validated equations, using doubly labelled isotopic water, and LBM by dual-energy X-ray absorptiometry (DXA) scanning. We studied 87 patients, 50 male (57.4%), 25 diabetic (28.7%), mean age 60.3±17.6 years, with a median PD treatment of 11.4 (4.7–29.5) months. The mean weight was 70.1±17.7 kg with a REE of 1509±245 kcal/day and TEE 1947±378 kcal/day. REE was associated with body size (weight r=0.78 and body mass index (BMI) r=0.72) and body composition (LBM r=0.77, lean body mass index (LBMI) r=0.76, r=0.62), all P<0.001). For TEE, there was an association with weight r=0.58, BMI r=0.49 and body composition (LBM r=0.64, LBMI (r=0.54), all P<0.001). We compared LBMI measured by DXA and that estimated by the Boer equation using anthropomorphic measurements, which overestimated and underestimated LBM for smaller patients and heavier patients, respectively. Muscle metabolism is reduced at rest and increases with physical activity. Whereas previous reports based on REE did not show any association with LBM, we found an association between both REE and TEE, using a recently validated equation derived from dialysis patients, and LBM measured by DXA scanning. Estimation of muscle mass from anthropomorphic measurements systematically overestimated LBM for small patients and conversely underestimated for heavier patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Paniagua R, Amato D, Vonesh E, Guo A, Mujais S, Mexican Nephrology Collaborative Study Group. Health-related quality of life predicts outcomes but is not affected by peritoneal clearance: The ADEMEX trial. Kidney Int 2005; 67: 1093–1104.
Daugirdas JT, Levin NW, Kotanko P, Depner TA, Kuhlmann MK, Chertow GM et al. Comparison of proposed alternative methods for rescaling dialysis dose: resting energy expenditure, high metabolic rate organ mass, liver size, and body surface area. Semin Dial 2008; 21: 377–384.
Bazanelli AP, Kamimura MA, da Silva CB, Avesani CM, Lopes MG, Manfredi SR et al. Resting energy expenditure in peritoneal dialysis patients. Perit Dial Int 2006; 26: 697–704.
Sridharan S, Wong J, Vilar E, Farrington K . Comparison of energy estimates in chronic kidney disease using doubly-labelled water. J Hum Nutr Diet 2016; 29: 59–66.
Fürstenberg A, Davenport A . Comparison of multifrequency bioelectrical impedance analysis and dual-energy X-ray absorptiometry assessments in outpatient haemodialysis patients. Am J Kidney Dis 2011; 57: 123–129.
Fürstenberg A, Davenport A . Assessment of body composition in peritoneal dialysis patients using bioelectrical impedance and dual-energy x-ray absorptiometry. Am J Nephrol 2011; 33: 150–156.
Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR Jr., Tudor-Locke C et al. 2011 Compendium of physical activities: a second update of codes and MET values. Med Sci Sports Exerc 2011; 43: 1575–1581.
Vilar E, Machado A, Garrett A, Kozarski R, Wellsted D, Farrington K . Disease-specific predictive formulas for energy expenditure in the dialysis population. J Ren Nutr 2014; 24: 243–251.
Wang AY, Sea MM, Tang N, Sanderson JE, Lui SF, Li PK et al. Resting energy expenditure and subsequent mortality risk in peritoneal dialysis patients. J Am Soc Nephrol 2004; 15: 3134–3143.
Zuo ML, Yue WS, Yip T, Ng F, Lam KF, Yiu KH et al. Prevalence of and associations with reduced exercise capacity in peritoneal dialysis patients. Am J Kidney Dis 2013; 62: 939–946.
Acknowledgements
This work was supported by a grant from British Renal Society. SE-K was awarded an International Society for Nephrology fellowship.
Disclaimer
None of the data contained in this report has been previously published in whole or part form.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Appendix
Appendix
Resting energy expenditure (REE) was estimated from a newer novel predictive equation which was derived and validated in a cohort of HD patients.4
REE=−2.497 × Age(years) × Factorage+0.011 × Height2.023(cm)+83.573 × Weight0.6291(kg)+68.171 × Factorsex
where Factor age is 0 if age <65 and 1 if ⩾65 and Factor sex is 0 if female and 1 if male.
Physical activity data—Each reported activity was assigned a metabolic equivalent of task (MET) value as per the Compendium of Physical Activities.4 Sleep time per day was assumed to be 8 h and any unreported time during the day was assumed as the time performing light activities at home. A Mean daily MET value was calculated.
Total energy expenditure (TEE) was estimated from the following equation.

Boer equation


Rights and permissions
About this article
Cite this article
El-Kateb, S., Sridharan, S., Farrington, K. et al. Comparison of resting and total energy expenditure in peritoneal dialysis patients and body composition measured by dual-energy X-ray absorptiometry. Eur J Clin Nutr 70, 1337–1339 (2016). https://doi.org/10.1038/ejcn.2016.120
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2016.120