- NEWS
How common is long COVID? Why studies give different answers
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 606, 852-853 (2022)
doi: https://doi.org/10.1038/d41586-022-01702-2
References
Xie, Y., Xu, E., Bowe, B. & Al-Aly, Z. Nature Med. 28, 583–590 (2022).
Xie, Y. & Al-Aly, Z. Lancet Diabetes Endocrinol. https://doi.org/10.1016/S2213-8587(22)00044-4 (2022).
Al-Aly, Z., Bowe, B. & Xie, Y. Nature Med. https://doi.org/10.1038/s41591-022-01840-0 (2022).
Antonelli, M. et al. Lancet Infect. Dis. 22, 43–55 (2022).
Antonelli, M., Pujol, J.C., Spector, T. D., Ourselin, S. & Steves, C. J. Lancet 399, 2263–2264 (2022).

 Can drugs reduce the risk of long COVID? What scientists know so far
Can drugs reduce the risk of long COVID? What scientists know so far
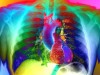 Heart-disease risk soars after COVID — even with a mild case
Heart-disease risk soars after COVID — even with a mild case
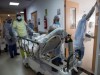 Diabetes risk rises after COVID, massive study finds
Diabetes risk rises after COVID, massive study finds
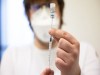 Long-COVID symptoms less likely in vaccinated people, Israeli data say
Long-COVID symptoms less likely in vaccinated people, Israeli data say






