- NEWS FEATURE
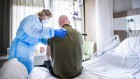
How months-long COVID infections could seed dangerous new variants
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 606, 452-455 (2022)
doi: https://doi.org/10.1038/d41586-022-01613-2
References
Sonnleitner, S. T. et al. Nature Commun. 13, 2560 (2022).
Martin, M. A. & Koelle, K. Sci. Transl. Med. 13, eabh1803 (2021).
Wilkinson, S. A. J. et al. Preprint at medRxiv https://doi.org/10.1101/2022.03.02.22271697 (2022).
Kemp, S. A. et al. Nature 592, 277–282 (2021).
Choi, B. et al. N. Engl. J. Med. 383, 2291–2293 (2020).
Tian, F. et al. eLife 10, e69091 (2021).
Hill, V. et al. Preprint at bioRxiv https://doi.org/10.1101/2022.03.08.481609 (2022).
Martin, D. P. et al. Mol. Biol. Evol. 39, msac061 (2022).
Meng, B. et al. Nature 603, 706–714 (2022).
Gonzalez-Reiche, A. S. Preprint at medRxiv https://doi.org/10.1101/2022.05.25.22275533 (2022).
Harari, S. et al. Preprint at medRxiv https://doi.org/10.1101/2022.02.17.22270829 (2022).
Graf, T. et al. Virus Evol. 7, veab091 (2021).
Gandhi, S. et al. Nature Commun. 13, 1547 (2022).
Huygens, S. et al. Preprint at medRxiv https://doi.org/10.1101/2022.04.06.22273503 (2022).
Rodionov, R. N. et al. Lancet Microbe 2, E138 (2021).
Bradley, R. E. et al. J. Clin. Immunol. 42, 32–35 (2022).

 Are COVID surges becoming more predictable? New Omicron variants offer a hint
Are COVID surges becoming more predictable? New Omicron variants offer a hint
 COVID is spreading in deer. What does that mean for the pandemic?
COVID is spreading in deer. What does that mean for the pandemic?
 Beyond Omicron: what’s next for COVID’s viral evolution
Beyond Omicron: what’s next for COVID’s viral evolution
 Where did Omicron come from? Three key theories
Where did Omicron come from? Three key theories
 The coronavirus is mutating — does it matter?
The coronavirus is mutating — does it matter?