- OUTLOOK
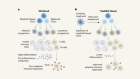
Miniature medical robots step out from sci-fi

Illustration: Jan Kallwejt
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
doi: https://doi.org/10.1038/d41586-022-00859-0
This article is part of Nature Outlook: Robotics and artificial intelligence, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Ghosh, A. & Fischer, P. Nano Lett. 9, 2243–2245 (2009).
Wu, Z. et al. Sci. Adv. 4, eaat4388 (2018).
Gao, C. et al. ACS Appl. Mater. Interfaces 11, 23392–23400 (2019).
Xu, H. et al. ACS Nano 12, 327–337 (2018).
Yan, X. et al. Sci. Robot. 2, eaaq1155 (2017).
Hortelao, A. C. et al. Sci. Robot. 6, eabd2823 (2021).
Gao, W. et al. ACS Nano 9, 117–123 (2015).
Felfoul, O. et al. Nature Nanotechnol. 11, 941–947 (2016).
Ye, Y. et al. Nano Lett. 21, 8086–8094 (2021).
Villa, K. et al. Cell Rep. Phys. Sci. 1, 100181 (2020).

 Breaking into the black box of artificial intelligence
Breaking into the black box of artificial intelligence
 Teaching robots to touch
Teaching robots to touch
 Learning over a lifetime
Learning over a lifetime
 Bioinspired robots walk, swim, slither and fly
Bioinspired robots walk, swim, slither and fly