Benjamin Thompson
Welcome to Coronapod.
Noah Baker
In this show, we’re going to bring you Nature’s take on the latest COVID-19 developments.
Benjamin Thompson
And we’ll be speaking to experts around the world about research during the pandemic.
Amy Maxmen
We’re entering a new era now. We have new COVID strategies, there’s some new unknowns and we’ve got a vaccine.
Benjamin Thompson
Hi, listeners. Welcome back to Coronapod. I’m Benjamin Thompson, once more in the South London basement. Noah Baker is out this week, but I’m joined on the line from Washington DC by Nidhi Subbaraman.
Nidhi Subbaraman
Hi, very nice to be here.
Benjamin Thompson
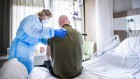
Today we’re going to talk about a topic that I’m sure has maybe played on the minds of a lot of listeners and certainly it has with friends of mine, and it’s not something that we’ve talked about on the podcast before, and that’s the effect that COVID-19 may be having during pregnancy, and that’s something that you’ve been looking at for Nature. Now, lots to discuss on this one, but I guess if we kind of head back maybe to the start of the pandemic, there was, as with so many other topics, a real scarcity of data on this issue.
Nidhi Subbaraman
Yeah, so if we rewind to February or March just about a year ago when, certainly in the US, people were beginning to pay attention to how this pandemic might be affecting their day-to-day lives here, one of the big questions that quickly arose was how does the disease affect pregnant people because at the time, some basics were still unknown and I think friends of mine certainly and doctors too were wondering what additional affects these additionally vulnerable groups should be aware of. The doctors who I spoke to remembered being a little bit worried at the time because respiratory viruses are known to be a little bit more concerning for pregnant people because of a few different things. One is that literally the biology of pregnancy pushes up your diaphragm and decreases your lung capacity, so when you have a respiratory infection that affects the lungs, you become additionally vulnerable there. And it’s known that influenza in the past, in the H1N1 pandemic in 2009, was putting pregnant people in the hospital and was leading to instances of fatalities. So, this was a big worry among maternal fetal doctors, OBGYNs, to figure out what was COVID going to look like.
Benjamin Thompson
Yeah, and maybe before we talk about how some of this data was collected, maybe let’s go straight to the headline then. What’s the sort of prevailing thoughts thus far from doctors and researchers on the effects that this virus may be having?
Nidhi Subbaraman
So, the good news is that this is not the worst case scenario as far as respiratory viruses are concerned. Babies are mostly spared the worst effects of the infection. Mostly, people are not seeing what is called vertical transmission, which is what happens when a mother who has SARS-CoV-2 passes it on to her baby. Those instances are very rare. They’re also not seeing high rates of stillbirths when babies don’t make it through because of the virus. Those are very rare. And although there is a higher risk of the baby being born early, pre-term births, mostly those are being seen in the third trimester, which is when the bad effects of an early delivery are – compared to the first two trimesters – minimised. So, pregnant women are a higher-risk group but there are some bright spots. Mothers aren’t dying. Rates of fatalities among pregnant people aren’t especially high although the risk is slightly higher, and they are weirdly less likely to show symptoms in the way that people who aren’t pregnant are. That’s something that came out of the biggest study of this group and it’s a little bit baffling still at this time, but it’s something that doctors and nurses who do see pregnant people should be aware of.
Benjamin Thompson
Some of the data that I saw from your feature suggested that good news that this isn’t potentially the worst sort of case scenario, but that people who are pregnant are ending up in hospital maybe at higher rates than those who aren’t.
Nidhi Subbaraman
So, the data is a little bit like weird on this question because the best data we have are from pregnant people who wound up in the hospital for any reason, so like they could have broken a foot and wound up in hospital and been tested that way. So, the biggest study that includes like 77 cohort studies from across the world only includes women who wound up in the hospital, so it’s not quite clear if somebody had a mild infection and never was tested because they never went near a doctor because they were advised, ‘Well, stay home and don’t come in unless it’s absolutely necessary.’ We don’t know what the situation is there for mild infection, so that’s a big question mark.
Benjamin Thompson
So, there’s little data then on things like community rates of transmission and are people who are pregnant maybe more vulnerable in general, we just don’t know that at the moment.
Nidhi Subbaraman
Yeah, the data is a little bit limited in that aspect, but a picture is coming together slowly.
Benjamin Thompson
And how are researchers then sort of putting the pieces together to get a better idea of what’s going on?
Nidhi Subbaraman
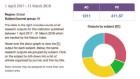
So, back in March again when maternal fetal researchers, OBGYNs, were worried about this, many of them who had been working on other questions to do with pregnancy or had been perhaps working with Zika, they sort of turned their work to COVID and they began plugging in with their hospital systems and gathering data from any of the patients who were coming in with COVID and tagging that they were pregnant, so there were these little cohorts that you saw collecting in California and Boston and Washington State and Switzerland, and the UK, of course, has this massive data collecting system in place already affiliated with the healthcare system, so the numbers started racking up and the results of those have begun making it into the literature. The CDC’s data also has begun showing up. In November, the agency published a big study that basically presented the data from over 400,000 women that included over 23,000 women who had been tagged as being pregnant.
Benjamin Thompson
But although data is now being collected and you’ve told us some of the results that have been found, there is a significant gap in the data and there’s one question in particular that I think you’ve been investigating and that obviously needs to be answered, and that’s about vaccinations. Because I know that most of the vaccine trials that happened sort of last year didn’t include pregnant women and we know that in general most if not all drug studies don’t include people who are pregnant, right?
Nidhi Subbaraman
Yes, this vaccine question has certainly been on our minds in the last months as the vaccines have rolled out in various countries as they have been approved. Two things were colliding here. One, it was still quite murky how and if pregnant women were a high-risk group and what the risks were. And secondly, as you just said, most drugs and vaccine trials, per protocol, they don’t include pregnant women and so doctors who were seeing patients were faced with this question, ‘Well, do I tell them to get the vaccine because they are slightly at higher risk or not?’ And so far, we’ve seen most of the major agencies also a little bit equivocating and not issuing a blanket recommendation because pregnant people, pregnant women, weren’t included in these trials. That said, the first surveys of the vaccine in the wild are gathering this data, so the CDC and the FDA in the US, are tracking pregnant women who have taken the vaccine to see if it has any effects, and as of February, 20,000 people had been included in that dataset and Anthony Fauci said there were no red flags. There are of course surveys that are being run by researchers themselves, for instance at the University of Washington where they’ve put out the word that pregnant women who’ve taken a vaccine out of their own choice can log in their information and be tracked as a research study to gather this information retroactively, and some of the vaccine makers are beginning their trials now that the first phases are done. It’s later than many researchers who study the ethics and study the space would like, and in some sense researchers and agency leaders who run programmes like this are making a fresh push and making a fresh call to the research community at large to rethink when and how pregnant women are included in these trials but also trials broadly.
Benjamin Thompson
And what do the doctors you spoke to have to say about all of this?
Nidhi Subbaraman
Most doctors that I spoke to were hopping mad that there weren’t instructions from agencies and all of them said that they would recommend that pregnant women strongly consider the vaccine and take it in consultation with their doctor. They said they were on board with it, in part – and when I was doing these interviews it was with the mRNA vaccines that were first online – they said no aspect of that vaccine biology is known to be concerning. And when the WHO also put out its recommendations for the mRNA vaccines, they added language that said there is no known point of concern. It’s just the absence of safety data that makes it concerning. So, yeah, I would not like to be in that position. Where agencies and doctors seem to have landed is that if you are in a higher-risk group because of your existing conditions or because you work in a job that puts you at high risk of exposure then you should probably think about getting the vaccine rather than if you’re at home and you’re not at high risk because of those reasons. So, that’s where people have landed among the people I’ve spoken to.
Benjamin Thompson
And if that’s one of the really big questions, certainly as vaccines are getting rolled out, what are some of the other things that aren’t really well understood that researchers really want to get a handle on in terms of COVID-19 and how it affects pregnancy?
Nidhi Subbaraman
One question was how a mother’s immunity transfers to babies and this is if a mother is infected with the virus and goes through the course of the disease, the antibodies in her blood, do they transfer over to the fetus and is the baby then protected? That is a question that we have a little bit of data on that we still need to understand a little better based on the interviews I’ve had with researchers. They say that antibodies do collect in the cord blood – this is the connection between the fetus and the mother – but it’s not known yet if the levels at which they’re found are sufficient to confer the protection that the baby would need against this particular virus. The levels that they found are lower than some other respiratory viruses, but perhaps that’s sufficient, perhaps that’s not. The other question that came up a little bit is how this status of infection during pregnancy, if it has any longer-term effect on a baby in its first years or even beyond that. There is a little bit of data that infections in a mother generally may put the baby at higher risk of certain neurodevelopmental conditions later on in their life based on a couple of studies. This has not been shown to be this case for SARS-CoV-2 by any means – it’s too early for that – but some groups are tracking in the first year of birth are babies meeting their usual neural goals. And then there’s a question of how this may have longer-term effects because of this general status of inflammation and infection being linked to this higher risk later on in life.
Benjamin Thompson
Which I guess, of course, it is impossible to know right now because here we are, what, a year and a little bit into the pandemic, but as you said earlier on, in the short term, babies seem to fare pretty well in terms of their immediate outcomes.
Nidhi Subbaraman
Yes, babies are at slightly higher risk for landing up in the NICU, the neonatal intensive care unit, but by and large, babies are born healthy, they don’t have respiratory infections and tracked through the first couple of weeks, they’re doing well.
Benjamin Thompson
Well, finally then, Nidhi, on this one, obviously a super important topic, but do you think things, lessons, will have been learnt in terms of data gathering, in terms of testing vaccines or what have you, that will be learnt in future research studies or in future disease outbreaks maybe?
Nidhi Subbaraman
So, I’m really curious if the tensions around when pregnant women are included in trials might see a renewed push and if the pace of how fast vaccines developed this time and the way that science has changed around this pandemic translates to the question of when pregnant women are included in research trials.
Benjamin Thompson
Well, let’s call it there then. I will put a link to your feature article in the show notes to this week’s podcast. Nidhi Subbaraman, thank you so much for joining me.
Nidhi Subbaraman
Thanks so much for having me.

 The latest COVID research updates
The latest COVID research updates
 ‘Major stones unturned’: COVID origin search must continue after WHO report, say scientists
‘Major stones unturned’: COVID origin search must continue after WHO report, say scientists
 Where did COVID come from? Five mysteries that remain
Where did COVID come from? Five mysteries that remain
 Can COVID spread from frozen wildlife? Scientists probe pandemic origins
Can COVID spread from frozen wildlife? Scientists probe pandemic origins