- NEWS
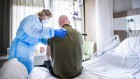
What the cruise-ship outbreaks reveal about COVID-19
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 580, 18 (2020)
doi: https://doi.org/10.1038/d41586-020-00885-w
References
Mizumoto, K., Kagaya, K., Zarebski, A. & Chowell, G. Euro Surveill. 25, 2000180 (2020).
Russell, T. W. et al. Preprint at medRxiv https://doi.org/10.1101/2020.03.05.20031773 (2020).
Mizumoto, K. & Chowell, G. Infect. Dis. Model. 5, 264–270 (2020).

 Coronavirus latest: China’s epicentre records no new cases
Coronavirus latest: China’s epicentre records no new cases
 Why does the coronavirus spread so easily between people?
Why does the coronavirus spread so easily between people?
 When will the coronavirus outbreak peak?
When will the coronavirus outbreak peak?
 Why snakes probably aren’t spreading the new China virus
Why snakes probably aren’t spreading the new China virus