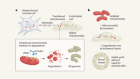
Illustration by Fabio Buonocore
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 573, 482-485 (2019)
doi: https://doi.org/10.1038/d41586-019-02847-3
Additional reporting by Brendan Maher.
Updates & Corrections
-
Correction 10 October 2019: An earlier version of this feature stated that an anonymous patient received a treatment called HeartSheet, developed by Yoshiki Sawa. The patient was told he was receiving a sheet of muscle cells from his thigh, which matches the description of HeartSheet, and was under the impression that Sawa was administering HeartSheet. Terumo, the company that produces HeartSheet, says that the patient did not receive HeartSheet but instead received an experimental treatment. Sawa has not returned Nature’s numerous requests for information or comment.
References
Daley, G. Q. et al. Stem Cell Rep. 6, 787–797 (2016).
Tsuji, K. et al. Eur. J. Heart Fail. 19, 1258–1269 (2017).
Miyamoto, S. Nature 569, 40 (2019).
Honmou, O. Jpn J. Neurosurg. 25, 979–984 (2016).
Sipp, D. & Sleeboom-Faulkner, M. Science 365, 644–646 (2019).

 A stem-cell race that no one wins
A stem-cell race that no one wins
 Japan’s approval of stem-cell treatment for spinal-cord injury concerns scientists
Japan’s approval of stem-cell treatment for spinal-cord injury concerns scientists
 Doubts over heart stem-cell therapy
Doubts over heart stem-cell therapy
 Japan poised to allow ‘reprogrammed’ stem-cell therapy for damaged corneas
Japan poised to allow ‘reprogrammed’ stem-cell therapy for damaged corneas
 Japan approves first human-animal embryo experiments
Japan approves first human-animal embryo experiments