- NEWS AND VIEWS
Two types of fibroblast drive arthritis
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 570, 169-170 (2019)
doi: https://doi.org/10.1038/d41586-019-01594-9
References
Lynch, M. D. & Watt, F. M. J. Clin. Invest. 128, 26–35 (2018).
Malmström, V., Catrina, A. I. & Klareskog, L. Nature Rev. Immunol. 17, 60–75 (2017).
Croft, A. P. et al. Nature 570, 246–251 (2019).
Huelsken, J. & Hanahan, D. Cell 172, 643–644 (2018).
Roberts, E. W. et al. J. Exp. Med. 210, 1137–1151 (2013).
Vallejos, C. A., Risso, D., Scialdone, A., Dudoit, S. & Marioni, J. C. Nature Methods 14, 565–571 (2017).
Vannella, K. M. & Wynn, T. A. Annu. Rev. Physiol. 79, 593–617 (2017).
Loeser, R. F., Goldring, S. R., Scanzello, C. R. & Goldring, M. B. Arthritis Rheum. 64, 1697–1707 (2012).
Competing Interests
T.A.W.’s employer Pfizer has approved products for rheumatoid arthritis.

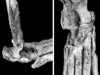 Read the paper: Distinct fibroblast subsets drive inflammation and damage in arthritis
Read the paper: Distinct fibroblast subsets drive inflammation and damage in arthritis
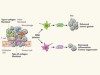 Fibroblasts for all seasons
Fibroblasts for all seasons
 The zinc link
The zinc link