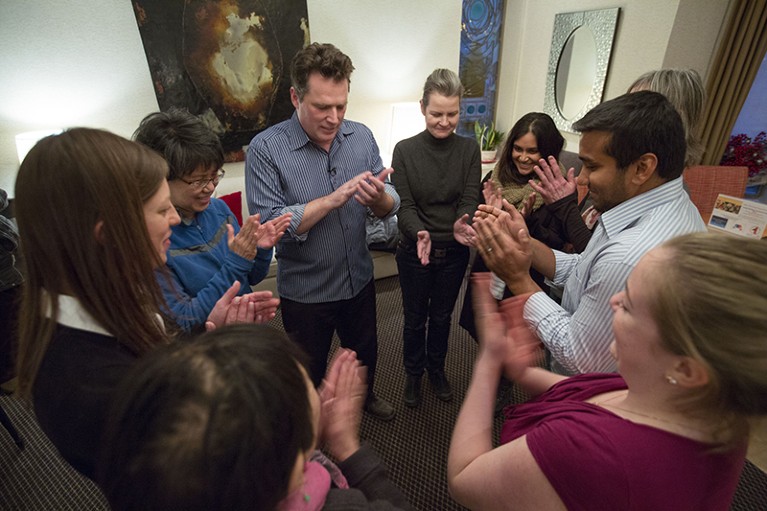
As more and more people survive cancer, researchers would do well to study these groups to gain insight into long-term effects of the treatments.Credit: Chris So/Toronto Star/Getty
When Gregory Aune was 16, he wasn’t particularly concerned about the lasting effects of the drugs and radiation that he was given to treat his lymphoma. “I saw kids around me die, so I felt pretty fortunate,” he says. Nearly 30 years later, Aune has a slightly different perspective. He’s still deeply grateful to have survived. But he has also dealt with hypothyroidism, diabetes and secondary skin cancer, and has had open-heart surgery and a stroke — all thought to have been brought on by the treatment that saved his life.
This experience has influenced Aune’s research. Now an oncologist and cancer researcher at the University of Texas Greehey Children’s Cancer Research Institute in San Antonio, he studies how cancer treatments can affect health in the long term.
It’s a topic that needs more attention. Dramatic improvements in cancer treatment are helping more people to survive once-deadly diseases. In the United States, the number of cancer survivors is projected to increase from nearly 17 million to 26 million by 2040. And the percentage of US cancer survivors living at least 5 years after diagnosis is expected to increase by 35% between 2017 and 2027.
But studies of survivors have lagged behind. There is understandably an intense focus on finding new ways to fight tumours, but significantly less effort has gone into finding ways to identify, understand and mitigate any long-term effects of cancer therapies. The issue was discussed on 31 March at the annual meeting of the American Association for Cancer Research in Atlanta, Georgia.
An analysis published in January examining how the US National Institutes of Health has supported survivorship research reveals where there is room for improvement (J. H. Rowland et al. J. Natl Cancer Inst. 111, 109–117; 2019). For one thing, the literature is small — just 215 studies were funded in 2016. Nearly half of those were in breast cancer, suggesting that survivors of other cancers deserve more attention. Only 14% specifically addressed the influence of ethnicity or sexual orientation on the topic of study, despite the key influence of these factors on cancer survival. And more than half were observational, although some researchers want to see more emphasis put on preventing and treating problems as well.
It is an area ripe for further discovery. Clinical research is needed to capture the long-term effects of treatments, including a host of new drugs that target the immune system. And more studies are needed of people aged 65 or older, a fast-growing segment of the survivor population. Such work would enable physicians and survivors to control therapy dosing, manage symptoms and detect early signs of complications more effectively.
A survey by the American Society of Clinical Oncology found that many survivorship studies focus on emotional well-being or physical health, but that few delved into the biological details or the influence of genetics (P. B. Jacobsen et al. J. Oncol. Pract. 12, 190–193; 2016). Yet such studies are important if we are to unravel why some treatments have long-term effects.
Advances in cancer research have extended and saved lives. But if their full benefits are to be realized, we must look beyond the point at which people are discharged from care. Researchers and funders should seize the chance to understand and treat the person, not just the tumour, and to make a real difference to the lives of millions of cancer survivors.

 Biological sex shapes tumour evolution across cancer types
Biological sex shapes tumour evolution across cancer types
 The cost of surviving cancer
The cost of surviving cancer
 Demand cancer drugs that truly help patients
Demand cancer drugs that truly help patients