- NEWS AND VIEWS
A new road to cancer-drug resistance
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 563, 478-480 (2018)
doi: https://doi.org/10.1038/d41586-018-07188-1
References
He, Y. J. et al. Nature https://doi.org/10.1038/s41586-018-0670-5 (2018).
Moynahan, M. E. & Jasin, M. Nature Rev. Mol. Cell Biol. 11, 196–207 (2010).
Schlacher, K. et al. Cell 145, 529–542 (2011).
Schlacher, K., Wu, H. & Jasin, M. Cancer Cell 22, 106–116 (2012).
Bryant, H. E. et al. Nature 434, 913–917 (2005).
Shalem, O. et al. Science 343, 84–87 (2014).
Sakai, W. et al. Cancer Res. 69, 6381–6386 (2009).
Goldstein, L. J. et al. J. Natl Cancer Inst. 81, 116–124 (1989).
Barbar, E. Biochemistry 47, 503–508 (2008).
Bunting, S. F. et al. Cell 141, 243–254 (2010).
Bouwman, P. et al. Nature Struct. Mol. Biol. 17, 688–695 (2010).
Lo, K. W. et al. J. Biol. Chem. 280, 8172–8179 (2005).
Rondinelli, B. et al. Nature Cell Biol. 19, 1371–1378 (2017).
Yamaguchi, H. et al. Oncogene 37, 208–217 (2018).
Ray Chaudhuri, A. et al. Nature 535, 382–387 (2016).
Sottoriva, A. et al. Nature Genet. 47, 209–216 (2015).

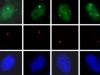 Read the paper: DYNLL1 binds to MRE11 to limit DNA end resection in BRCA1-deficient cells
Read the paper: DYNLL1 binds to MRE11 to limit DNA end resection in BRCA1-deficient cells
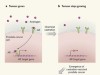 Resistance to prostate-cancer treatment is driven by immune cells
Resistance to prostate-cancer treatment is driven by immune cells
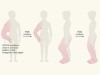 Lessons for cancer drug treatment from tackling a non-cancerous overgrowth syndrome
Lessons for cancer drug treatment from tackling a non-cancerous overgrowth syndrome