Abstract
Berberine is identified to lower the serum cholesterol level in human and hamster through the induction of low density lipoproteins (LDL) receptor in hepatic cells. To evaluate its potential in preventing atherosclerosis, the effect of berberine on atherosclerosis development in apolipoprotein E-deficient (apoE−/−) mice was investigated. In apoE−/− mice, berberine induced in vivo foam cell formation and promoted atherosclerosis development. The foam cell formation induced by berberine was also observed in mouse RAW264.7 cells, as well as in mouse and human primary macrophages. By inducing scavenger receptor A (SR-A) expression in macrophages, berberine increased the uptake of modified LDL (DiO-Ac-LDL). Berberine-induced SR-A expression was also observed in macrophage foam cells in vivo and in the cells at atherosclerotic lesion. Analysis in RAW264.7 cells indicated that berberine induced SR-A expression by suppressing PTEN expression, which led to sustained Akt activation. Our results suggest that to evaluate the potential of a cholesterol-reducing compound in alleviating atherosclerosis, its effect on the cells involved in atherosclerosis development, such as macrophages, should also be considered. Promotion of foam cell formation could counter-balance the beneficial effect of lowering serum cholesterol.
Similar content being viewed by others
Introduction
Reduction of serum cholesterol level has been proven as an effective way to prevent atherosclerosis development 1. The success of statin drugs and ezetimibe in preventing atherosclerosis by reducing serum low density lipoproteins (LDL) cholesterol level has instigated the search for cholesterol-controlling products 1, 2, 3, 4. Recently, berberine, a natural alkaloid isolated from Huanglian (Coptis chinensis), is reported to lower serum cholesterol level in human and hamster 5. The effect of berberine on lowering serum LDL cholesterol is mediated by stabilizing LDL receptor mRNA in the liver cells 5, 6. This represents a different mechanism from statins, which induce LDL receptor expression through inactivating 3-hydroxy-3-methylglutaryl coenzyme A reductase 2.
Berberine has been used as a non-prescription drug to treat diarrhea and gastroenteritis in China since 1950s. It is reported to have anti-diabetic effects in insulin-responsive cells and animal models 7. In 3T3-L1 adipocytes and L6 myotubes, berberine activates AMP-activated protein kinase and induces GLUT4 translocation 7. During 3T3-L1 adipocyte differentiation induction, berberine reduces the lipid accumulation in 3T3-L1 cells by inactivating PPARγ 7, 8. These beneficial metabolic effects of berberine and its history as a non-prescription drug in China suggest that berberine has the potential to be a drug for treating hyperlipidemia, hyperglycemia and obesity.
Atherosclerosis is a chronic inflammation condition resulting from the interaction between lipoproteins, monocyte-derived macrophages, T lymphocytes and other cellular elements in the arterial wall 9, 10, 11. During atherosclerosis development, the attraction of circulating monocytes by modified LDL into subendothelial arterial space and their differentiation into macrophages are the initial events 12, 13, 14, 15. In the subendothelial arterial space, the uptake of modified LDL by macrophages leads to the formation of foam cells in which a large amount of cholesteryl ester droplets are accumulated 9, 15, 16, 17. The release of cholesteryl lipids from apoptotic foam cell forms the initial plaques in subendothelial arterial space. The role of foam cells as the major culprit in atherosclerosis has been further demonstrated by the resistance to atherosclerosis in mice that lack macrophages 18, 19.
In macrophage, the uptake of modified LDL by scavenger receptors induces the formation of foam cell 20, 21, 22, 23. Besides hypercholesterolemia, other factors such as LDL oxidation and increased scavenger receptors can also disrupt the cholesterol homeostasis in macrophage, induce foam cell formation and cause atherosclerosis. As berberine targets multiple types of cells such as hepatocytes, adipocytes and muscle cells 5, 6, 7, 8, it is important to ascertain whether berberine has any effect on monocytes/macrophages, especially on foam cell formation. In order to evaluate the potential of berberine as a cholesterol-controlling drug for preventing atherosclerosis, its effect on atherosclerosis development needs to be more carefully investigated. In this report, we show that in apolipoprotein E-deficient (apoE−/−) mice, berberine promotes atherosclerosis development. The promotion of atherosclerosis resulted from berberine-induced in vivo foam cell formation. Using RAW264.7 cells, which can be induced by oxidized LDL (oxLDL) to form foam cells 24, we have identified that berberine induces the expression of scavenger receptor A (SR-A) through modulating the PI3-kinase signaling pathway. Specifically, by inactivating PPARγ, berberine inhibits PTEN expression and thus enhances PI3-kinase signaling.
Results
Berberine promotes atherosclerosis development in apoE−/− mice by inducing in vivo foam cell formation
ApoE−/− mouse is a well-established animal model for studying atherosclerosis 25, 26, 27. Because berberine is poorly absorbed if taken orally 28, we administrated berberine to mice by intraperitoneal injection. On average, berberine-treated mice took less food and gained less weight than the control mice (Figure 1A). After a 15-week berberine treatment, there was no significant change in the total serum triglycerides, LDL cholesterol or HDL cholesterol levels (Figure 1B). However, more atherosclerotic lesions were developed in berberine-treated mice (Figure 1C). The average size of atherosclerotic lesions in berberine-treated mice was about 50% larger than that in control mice (Figure 1D).
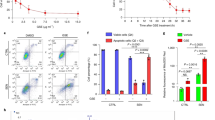
Berberine promotes atherosclerosis development by inducing in vivo foam cell formation in apoE−/− mice. (A) Food intake and body weight of mice (n = 10 per group). The daily food intake was measured every other week. The results are the average of eight measurements. The body weight is the average weight of 10 mice at the beginning on Western diet (W0) and after 15-week experiment (W15). C, mice with vehicle treatment; B, mice with berberine treatment (5 mg/kg/day). (B) Serum lipids. The labels are the same as in panel A. The results are the average of 10 mice. (C) Atherosclerotic lesions in the aortic root after 15-week experiment. Cryosection of aortic sinus was stained with Oil-red-O. Representative photographs are shown. (D) The average lesion size. For each mouse, the Oil-red-O-stained areas were measured in four sections of the aortic sinus and these were averaged to obtain the lesion size of one mouse. For each group, 10 mice were averaged. *P < 0.05. (E) In vivo foam cell formation in berberine-treated mice (n=6 per group). Oil-red-O staining of peritoneal macrophages isolated from mice treated with berberine for 2 weeks (2.5 mg/kg/day BBR and 5 mg/kg/day BBR) or not (Control). Representative photographs are shown. (F) Cholesterol content of peritoneal macrophages. The results are the average of six mice. B2.5, 2.5 mg/kg/day berberine; B5, 5 mg/kg/day berberine. *P < 0.05, **P < 0.01.
Because there was no change in serum cholesterol in berberine-treated mice, the berberine-promoted atherosclerosis would likely have resulted from other factors than serum cholesterol (Figure 1B). As foam cell is the major culprit in atherosclerosis 18, 19, peritoneal macrophages were collected from berberine-treated apoE−/− mice and analyzed for foam cell formation. The peritoneal macrophages collected from control apoE−/− mice exhibited the typical macrophage morphology and contained little amount of lipid droplets (Figure 1E). In contrast, most macrophages collected from berberine-treated apoE−/− mice contained massive amount of lipid droplets and the cellular cholesterol content was increased by several folds (Figure 1E and 1F).
The promotion of in vivo foam cell formation by berberine was confirmed by in vitro experiments with mouse primary macrophages. In normal culture medium with 10% fetal bovine serum (FBS), no foam cell was induced from the cultured mouse peritoneal macrophages (Figure 2A and 2B). When the cultured primary macrophages were treated with berberine, foam cell formation was induced and cellular cholesterol level was also increased (Figure 2A and 2B). The induction of foam cell formation by berberine in human primary macrophages was also observed (Figure 2C). Although the effect of berberine on serum cholesterol level in apoE−/− mouse was different from its reported effect in human (Figure 1B) 5, the promotion of foam cell formation was similar in cultured primary macrophages of both mouse and human (Figure 2).
Berberine induces in vitro foam cell formation. Bar = 10 μm. (A) Berberine induced foam cell formation in cultured mouse peritoneal macrophage (macrophage) and RAW264.7 cell (RAW264.7). +10 μM BBR, +20 μM BBR and +40 μM BBR indicate berberine concentration. Control, no berberine treatment. (B) Cholesterol of mouse peritoneal macrophage and RAW264.7 cell. The results are the average of three independent experiments. *P < 0.05, **P < 0.01. 5 μM B, 10 μM B and 20 μM B indicate berberine concentration. (C) Berberine induced foam cell formation in human primary macrophage.
Berberine promotes foam cell formation by inducing SR-A
In comparison to primary cells, the in vitro cultured cell line is usually more feasible for performing mechanistic studies. Mouse RAW264.7 cells are a macrophage-like cell line and can be induced to form foam cells in the presence of oxLDL (Supplementary information, Figure S1) 24. It could also be induced to form foam cells by berberine without the addition of oxLDL (Figure 2A). The foam cell formation and cholesterol accumulation induced by berberine in RAW264.7 cells were very similar to that in mouse primary macrophages (Figure 2A and 2B). Thus RAW264.7 cells appear to be a good model for studying the mechanism of berberine induction of foam cell formation (Supplementary information, Figure S1).
SR-A and CD36 are two most important scavenger receptors for the uptake of modified LDL, which promotes foam cell formation in macrophages 22. Berberine treatment increased the levels of SR-A on RAW264.7 cell surface, but not of CD36 (Figure 3A and 3B). It also induced DiO-Ac-LDL uptake in RAW264.7 cells (Figure 3C). This berberine-induced DiO-Ac-LDL uptake clearly resulted from SR-A increase, as it was specifically inhibited by antibody against SR-A (Figure 3D). In addition, berberine did not affect the cholesterol efflux from RAW264.7 cells (Figure 3E). These observations suggest that berberine-induced SR-A is the primary cause for the increased foam cell formation.
Berberine specifically induces scavenger receptor A expression. *P < 0.05, **P < 0.01. (A) Cell surface SR-A. The flow cytometry graph is the fluorescence labeling by anti-SR-A antibody in RAW264.7 cells treated with (Red line) or without (Gray line) 10 μM berberine. The green line is the blank IgG. The bar graph is the average result of three experiments. C, control; B, berberine-treated cell. (B) Cell surface CD36. The labels are the same as in panel A. (C) DiO-Ac-LDL uptake. Gray line, control cell; Red line, berberine-treated cell; Green line, without adding DiO-Ac-LDL. (D) Inhibition of DiO-Ac-LDL uptake by anti-SR-A antibody. The gray bars are DiO-Ac-LDL uptake in control RAW264.7 cells blocked with blank IgG (IgG), anti-SR-A antibody (α-SRA) or anti-CD36 antibody (α-CD36). The red bars are DiO-Ac-LDL uptake in berberine-treated RAW264.7 cells blocked with antibody. (E) Cholesterol efflux. RAW264.7 cells were labeled with 3H-labeled cholesterol (Perkin-Elmer) and cholesterol efflux was measured in the presence or absence of 5 μM berberine as described by de la Llera Moya et al. 47. The results are the average of three experiments. (F) Time course of berberine induced SR-A expression. SR-A in RAW264.7 cell treated with or without (Control) 5 μM berberine (5 μM BBR) for the indicated times (0, 6, 12, 24, 48 and 96 h) was detected by western blot. (G) Real-time PCR of SR-A mRNA in RAW264.7 cell treated with or without (Ctrl) berberine for 48 h (2.5 μM BBR or 10 μM BBR). The results are the average of four experiments. (H) SR-A promoter activity. The luciferase analysis was carried out in 293T cells transfected with SR-A promoter-luciferase reporter plasmid and treated with berberine (5 μM BBR, 10 μM BBR and 20 μM BBR), LY294002 (10 μM LY and 20 μM LY) or both (10 B+10 LY and 10 B+20 LY) for 24 h. The results are the average of four experiments. (I) Inhibition of berberine-induced SR-A expression by LY294002. SR-A in RAW264.7 cell treated with berberine (5 μM BBR), LY294002 (5 μM LY or 20 μM LY) or both (5 B+5 LY and 5 B+20 LY) for 48 h was detected by western blot.
SR-A was expressed at a relatively constant level in RAW264.7 cells (Figure 3F). However, it was greatly induced by berberine treatment (Figure 3A and 3F). The analysis of SR-A mRNA and its gene promoter activity showed that berberine induced SR-A by increasing gene transcription (Figure 3G and 3H). To identify the signal molecules involved in berberine-induced SR-A transcription, the effect of PI3-kinase inhibitor (LY294002) or MEK inhibitors (PD98059 and U0126) on berberine-induced foam cell formation was analyzed. Only LY294002, but not PD98059 or U0126, inhibited berberine-induced foam cell formation (Supplementary information, Figure S2). Interestingly, LY294002 did not inhibit the basal SR-A expression, but inhibited berberine-induced SR-A expression (Figure 3H and 3I).
To ascertain whether berberine promotes atherosclerosis development in apoE−/− mouse by inducing SR-A, atherosclerotic lesions were analyzed for SR-A expression. As shown in Figure 4A, SR-A expression in the cells of atherosclerotic lesions was greatly enhanced in berberine-treated apoE−/− mice. Western blot of aorta samples also revealed the increased SR-A expression in berberine-treated apoE−/− mice (Figure 4B and 4C). In peritoneal macrophages obtained from berberine-treated apoE−/− mice, SR-A was increased in a dose-dependent manner (Figure 4D and 4E). Human primary macrophage samples from three of the four volunteers also exhibited berberine-induced SR-A expression (Figure 4F).
Berberine induces SR-A expression in vivo. (A) SR-A expression in cells at atherosclerotic lesion. Sections of aortic sinus were stained with anti-SR-A antibody (brown) and the nuclei were counter-stained with hematoxylin (blue). Representative photographs are shown. Control, control apoE−/− mice; BBR treated, apoE−/− mice treated with berberine for 15 weeks. (B) Western blot for SR-A in aorta samples. BBR5.0, apoE−/− mice treated with 5 mg/kg/day berberine for 4 weeks; M1, M2 and M3, individual mice. (C) Densitometer scanning of western blot in panel B. (D) Western blot for SR-A in peritoneal macrophages isolated from apoE−/− mice treated with or without (Ctrl) 2.5 mg/kg/day or 5 mg/kg/day berberine for 2 weeks (BBR2.5 and BBR5.0). (E) Densitometer scanning of western blot in panel D. (F) SR-A expression in human primary macrophages. Human primary macrophages of four volunteers (S1-4) were treated with 10 μmol/l berberine or not for 24 h. SR-A mRNA was determined by real-time RT-PCR. The ratio of berberine treatment to control was plotted.
Berberine induces SR-A expression by activating PI3-kinase signaling
LY294002, which inhibited berberine-induced SR-A expression and foam cell formation (Figure 3H, 3I and Supplementary information, Figure S2), is a widely used PI3-kinase inhibitor. The inhibitory effect of LY294002 on foam cell formation could be reversed by the addition of 3-phosphorylated phosphatidylinositol (dipalmitoyl-L-alpha-phosphatidylinositol-3, 4, 5-trisphosphate) (Figure 5A). The PI3-kinase signal cascade includes PI3-kinase that catalyzes the formation of 3-phosphorylated phosphatidylinositols and PTEN that dephosphorylates 3-phosphorylated phosphatidylinositol 29. By blocking PI3-kinase activity, LY294002 inhibited Akt-1 activation (Supplementary information, Figure S2) 30. Berberine treatment decreased PTEN expression without affecting PI3-kinase (p85 and p110 subunits) (Figure 5B and 5C). Decrease of PTEN could increase the stability of 3-phosphorylated phosphatidylinositols, which leads to sustained Akt-1 activation (Figure 5D).
Berberine reduces PTEN expression. (A) Oil-red-O staining of RAW264.7 cells treated with 10 μM LY294002 (+LY), 5 μM dipalmitoyl-L-alpha-phosphatidylinositol-3, 4, 5-trisphosphate (+PIP3), or both (+LY & PIP3) for 4 days. Bar = 10 μm. Control, RAW264.7 cells 4 days after cell-cell contact. Cells were replated and then stained. (B) p85 subunit and p110 subunit of PI3-kinase in RAW264.7 cells treated with 5 μM berberine (B) for the indicated times (6 h, 24 h and 48 h) or not (C). (C) PTEN in RAW264.7 cells treated with berberine. The labels are the same as in panel B. (D) Akt-1 phosphorylation in berberine-treated RAW264.7 cell. (E) PTEN mRNA in RAW264.7 cells treated with or without (Ctrl) berberine for 48 h (2.5 μM BBR and 10 μM BBR) was measured by real-time RT-PCR. The results are the average of three experiments. *P < 0.05, **P < 0.01
Berberine reduced PTEN mRNA levels (Figure 5E). The activation of Akt only after prolonged berberine treatment indicated a relatively slow effect on PTEN expression, likely through transcription regulation (Figure 5D and Supplementary information, Figure S2). It is reported that berberine inhibits PPARγ activity by increasing PPARγ phosphorylation 7, 8 and PTEN transcription is regulated by PPARγ 31, 32. The inhibition of PPARγ by berberine was clearly illustrated by berberine-mediated inhibition of 3T3-L1 adipocyte differentiation, as PPARγ is one of the most important transcription factors in adipocyte differentiation (Figure 6A) 7, 8, 33, 34. In RAW264.7 cells, berberine inhibited PTEN expression induced by troglitazone, an agonist of PPARγ (Figure 6B). The inhibition of PPARγ by berberine in RAW264.7 cells could also be confirmed by the suppression of other PPARγ target genes, such as adipose fatty acid-binding protein (aP2) and lipoprotein lipase (LPL) (Figure 6C). The expression of these two genes was greatly inhibited in berberine-treated RAW264.7 cells (Figure 6C). Consistently, berberine increased PPARγ phosphorylation in these cells (Figure 6D).
Berberine inhibits PPARγ activity in RAW264.7 cell. (A) 3T3-L1 adipocyte differentiation inhibited by berberine. 3T3-L1 adipocyte differentiation was induced with the standard protocol 45, 46. Berberine (+10 μM BBR and +100 μM BBR), troglitazone (+10 μM Tro) or both (T+10 μM B and T+100 μM B) was added from day 0. Oil-Red-O staining was carried out on day 10. (B) Berberine inhibits troglitazone-induced PTEN expression in RAW264.7 cell. RAW264.7 cells were treated with berberine, troglitazone or both for the indicated times. PTEN was detected by western blot. (C) Real-time RT-PCR analysis for PPARγ target genes in berberine-treated RAW264.7 cell. The mRNA of target genes in RAW264.7 cells treated with or without (C) 10 μM berberine for 48 h (B) was determined by real-time RT-PCR. aP2, adipose fatty acid-binding protein; LPL, lipoprotein lipase. The results represent three independent experiments. **P < 0.01. (D) Berberine induces PPARγ phosphorylation in RAW264.7 cell. Cells were treated with berberine for 2 h at indicated concentration. Phosphorylated PPARγ (pPPARγ) and PPARγ protein (PPARγ) were detected by western blot.
Discussion
By screening herb compounds for induction of LDL receptor expression in HepG2 cells, berberine was identified to stabilize LDL receptor mRNA 5, 6. Subsequently, it was found to reduce serum cholesterol in human and hamster 5. However, whether berberine treatment reduces the risk of atherosclerosis in human, as other cholesterol-reducing drugs do, requires further investigation. As a model for human atherosclerosis, apoE−/− mice were used to evaluate the effect of berberine on atherosclerosis development. In this mouse model, berberine aggravated the development of atherosclerosis by promoting in vivo foam cell formation (Figure 1). This was confirmed by in vitro studies in mouse and human primary macrophages, as well as in mouse RAW264.7 cells (Figure 2). Thus, the induction of foam cells by berberine may counter-balance its beneficial effects of cholesterol reduction. For example, lovastatin, a statin drug for lowering serum cholesterol and reducing the risk of atherosclerosis, does not promote macrophage foam cell formation (Supplementary information, Figure S3). Our results suggest that to evaluate the effect of a cholesterol-reducing compound on atherosclerosis, its effect on the cells involved in atherosclerosis development, such as macrophages, should also be considered.
Atherosclerosis is a chronic inflammation condition resulting from the interaction between lipoproteins, monocyte-derived macrophages, T lymphocytes and other cellular elements in the arterial wall 9, 10, 11. Many cytokines, such as interleukins and macrophage-associated cytokines, are locally expressed in the atherosclerotic lesions and critically involved in the pathogenesis of this disease. They are mediators of the immuno-inflammatory response and could coordinate the cell interactions 11, 35. Berberine is also reported to have anti-inflammatory effects in vitro and in vivo 36, 37, 38. The administration of neutral sulfate berberine significantly reduced plasma tumor necrosis factor-α, interferon-γ and nitric oxide levels in mice challenged with lipopolysaccharide 38. It is well known that anti-inflammation favors the protection from atherosclerosis. The anti-inflammation effect of berberine could have beneficial impact on preventing atherosclerosis. However, our study showed that berberine promoted atherosclerosis development in apoE−/− mice. It is possible that the induction of foam cells by berberine overrides its beneficial effects of anti-inflammation in this mouse model for atherosclerosis.
The cholesterol-reducing effect of berberine in human and hamster results from the increased LDL receptor level in the liver 5. However, in apoE−/− mouse, berberine treatment did not increase the LDL receptor mRNA or protein in the liver (Supplementary information, Figure S4). These results may explain why berberine does not alter the serum cholesterol and lipids in apoE−/− mouse (Figure 1B). Despite the difference in lowering serum cholesterol between mouse and human, the effect of berberine on promoting foam cell formation is similar in both mouse and human macrophages (Figure 2 and Figure 4). Because the serum cholesterol level is not altered in berberine-treated apoE−/− mouse, the aggravation of atherosclerosis appears to be related to the effect of berberine on SR-A expression in macrophages (Figure 4). As berberine targets multiple types of cells, such as hepatocytes, adipocytes, muscle cells and macrophages (Figure 2 and Figure 4) 5, 6, 7, 8, the animal study in apoE−/− mouse is essential for understanding its potential effect in human atherosclerosis.
The mechanism of berberine-induced foam cell formation is examined using RAW264.7 cells and primary macrophages (Figure 3 4 5). SR-A increase appears to be the major effect through which berberine alters the cholesterol homeostasis in macrophages (Figure 3 and Supplementary information, Figure S5). In our current study, berberine induces SR-A expression through the activation of PI3-kinase signaling cascade (Figure 5 and Supplementary information, Figure S2). The involvement of PI3-kinase signaling cascade in SR-A expression is also found in human vascular smooth muscle cells 39. The temporal order of berberine's effects on PI3-kinase signaling cascade and PPARγ supports the fact that PPARγ is the target of berberine (Figure 5 and Figure 6) 7, 8. Berberine-induced PPARγ phosphorylation precedes the decrease of PTEN and the activation of Akt (Figure 5C, 5D, 6D and Supplementary information, Figure S2). Only after prolonged berberine treatment are berberine's effect on PTEN and Akt observed. As in adipocytes and myotubes 7, 8, PPARγ might also be the target of berberine in macrophages (Figure 6). The detailed mechanism of berberine-induced PPARγ phosphorylation is under investigation.
Materials and Methods
Materials
Anti-SR-A antibody was from Serotec. Anti-CD36 antibody was from Cascade Bioscience. Anti-p85α, anti-p110α, anti-PPARγ, anti-Akt-1 and anti-phospho-Akt (Ser473-phosphorylated form) antibodies were from Santa Cruz Biotechnology. Anti-phospho-PPARγ antibody was from Upstate Biotechnology. Anti-PTEN, horseradish peroxidase-conjugated and fluorescein isothiocyanate (FITC)-conjugated secondary antibodies and berberine were from Sigma. Lipoprotein-deficient FBS and 3, 3′-dioctadecyloxacarbocyanine perchlorate-labeled acetylated LDL (DiO-Ac-LDL) were from Biomedical Technologies. LY294002 and dipalmitoyl-L-alpha-phosphatidylinositol-3, 4, 5-trisphosphate were from Calbiochem.
Animal experiments
ApoE−/− mice (C57BL/6J) from the Jackson Laboratory (Bar Harbor, ME, USA) were housed at 22 ± 2 °C, 55% ± 5% relative humidity, with a 12-h light/dark cycle. 8-week-old male mice (n = 10 per group) were placed on a Western diet (21% fat, 0.21% cholesterol; D12079B; Research Diets Inc.) and received daily intraperitoneal injection of either vehicle or berberine (5 mg/kg/day) for 15 weeks. After an overnight fasting period, 100 μl blood was drawn by tail bleeding. The serum lipids were determined by enzymatic procedures (Wako Chemicals).
For histological and immunohistochemical analyses, mice were sacrificed and hearts were perfused with 20 ml saline and 10 ml 3.7% buffered formalin. Serial cryosections of 10-μm thickness were taken from the region of the proximal aorta through the aortic sinuses and stained with Oil-red-O. The lesion size was quantified by measuring Oil-red-O stained area. The mean lesion size for each individual mouse was calculated from four sections, starting at the appearance of the tricuspid valves 40. SR-A in cells at atherosclerotic lesion was stained with anti-SR-A antibody. 3, 3′-diaminobenzidine (Sigma) was used to reveal SR-A by brown colorization. Cell nuclei were counterstained with hematoxylin.
For western blot of SR-A in aorta sample, apoE−/− mice (n = 6 per group) fed on Western diet and treated with berberine (5 mg/kg/day) for 4 weeks were sacrificed and perfused with 20 ml saline; the aorta were immediately excised and frozen in liquid nitrogen. After tissue homogenization, protein extract was subjected to western blot for SR-A.
All animal experiments were carried out in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals and were approved by the Biological Research Ethics Committee of Shanghai Institutes for Biological Sciences.
In vivo and in vitro foam cell formation
8-week-old male apoE−/− mice (n = 6 per group) were treated by berberine (2.5 mg/kg/day or 5 mg/kg/day) or vehicle control for 2 weeks and the peritoneal macrophages were collected as described by Takahashi et al. 41. 3 days after peritoneal injection of 1 ml 3% thioglycolate broth, macrophages were obtained by peritoneal lavage with Dulbecco's modified Eagle's medium (DMEM) containing 10% FBS. Cells were plated at 1.0 × 106 per ml of DMEM with 10% FBS. After incubation for 3 h at 37 oC, the non-adherent cells were washed away and the adherent cells were collected for western blot, cholesterol measurement or Oil-red-O staining.
Mouse peritoneal macrophages collected from 8-week-old male C57BL/6 mice were cultured in DMEM with 10% FBS for 24 h and treated with berberine for additional 48 h. Mouse RAW264.7 cells were plated (5 × 105 cells per 35-mm dish), cultured in DMEM with 10% FBS for 48 h and treated with berberine for additional 48 h. The cells were harvested or fixed for Oil-red-O staining.
Human primary monocytes were isolated from the blood of healthy normalipidermic volunteers of age between 25 and 30 years with a life-time non-smoking history, no acute or chronic illness, and no current medication 42, 43. Peripheral blood mononuclear cells isolated by Ficoll-Hypaque gradient centrifugation were suspended in DMEM with 10% heat-inactivated FBS and seeded into 60-mm dishes (8 × 105 cells/ml). After 2 h incubation, the non-adherent cells were washed away and the medium was replaced with macrophage-SFM medium (Gibco) supplemented with 500 U/ml of granulocyte-macrophage colony-stimulating factor (PetroTech) and penicillin (100 U/ml)-streptomycin (100 μg/ml). After 7 days, the adherent cells were used as human monocyte-derived macrophages. On day 7, cells were treated with berberine in DMEM with 10% FBS for 24 h and then harvested or fixed for Oil-red-O staining.
Cholesterol measurement
Cells were washed with phosphate-buffered saline (PBS). The cellular lipids were obtained by sonicating the cells in hexane/isopropanol (3/2, v/v) and extracting for 24 h. After removing cell debris by centrifuging at 12 000 g, the supernatant was dried under nitrogen flush and re-dissolved in isopropanol. Total cholesterol was determined with an Amplex Red Cholesterol Assay Kit (Invitrogen) 44. The protein was determined by Lowry assay.
Western blot
Cells were washed with ice-cold PBS, lysed directly in boiling 1× Laemmli SDS buffer containing 20 mmol/l dithiolthretol and heated at 100 oC for 5 min. Samples were subjected to western blot 45, 46.
Real-time RT-PCR
Total RNA was prepared from cells with TRIzolTM reagent (Invitrogen). Total RNA (2 μg) was reverse-transcribed with oligo-dT primer. The cDNA samples were then diluted to appropriate concentration for real-time PCR analysis (Rotor-Gene 3000, Corbett Research Pty Ltd). Hypoxanthine-guanine phosphoribosyl transferase (HPRT) was used as a constitutive gene control. The target mRNA was normalized with HPRT in the same sample. The PCR primers are: PTEN (forward: 5′-CGG AAC TTG CAA TCC TCA GT-3′; reverse: 5′-AGG TTT CCT CTG GTC CTG GT-3′), SR-A (forward: 5′-TGG TCC ACC TGG TGC TCC-3′; reverse: 5′-ACC TCC AGG GAA GCC AAT TT-3′), aP2 (forward: 5′-AAA GAC AGC TCC TCC TCG AAG GTT-3′; reverse: 5′-TGA CCA AAT CCC CAT TTA CGC-3′), LPL (forward: 5′-GGC TCT GCC TGA GTT GTA G-3′; reverse: 5′-AGA AAT TTC GAA GGC CTG GT-3′), HPRT (forward: 5′-CCT GCT GGA TTA CAT TAA AGC-3′; reverse: 5′-TTC AAC ACT TCG AGA GGT CCT-3′).
DiO-Ac-LDL Uptake
DiO-Ac-LDL uptake was performed as described by Cao et al. 39. RAW264.7 cells were treated with or without berberine for 48 h, incubated in DMEM with 2% lipoprotein-deficient FBS and 10 μg/ml DiO-Ac-LDL for 4 h at 37 °C, washed with PBS and analyzed by FACScan flow cytometer (BD Biosciences). For anti-SR-A or anti-CD36 antibody-blocking experiment, cells were pre-incubated with 10 μg/ml antibody in DMEM containing 2% lipoprotein-deficient FBS for 1 h at 37 °C. DiO-Ac-LDL was then added to the cells for uptake.
Cell surface receptor measurement
RAW264.7 cells were treated with 10 μM berberine or not for 48 h, washed with ice-cold PBS containing 0.5% bovine serum albumin, and incubated with anti-SR-A, anti-CD36 or isotype blank antibody for 1 h on ice. FITC-conjugated secondary antibody was used for flow cytometry analysis.
SR-A gene promoter analysis
Human SR-A promoter fragment (−696 to +46, was kindly provided by Dr Christopher Glass, University of California, San Diego) in a luciferase reporter vector (pGL3-basic, Promega) was transfected into HEK 293T cells by Lipofectamine 2000 (Invitrogen). 24 h after transfection, cells were treated with berberine, LY294002 or both for additional 24 h. Luciferase reporter assay was carried out using the Dual-Luciferase Reporter Assay System (Promega) and the transfection efficiencies were normalized to Renilla luciferase activity.
Statistical Analysis
Data were presented as mean ± SD. Differences were analyzed by Student's t-test. P < 0.05 was considered statistically significant.
( Supplementary information is linked to the online version of the paper on the Cell Research website.)
References
Grundy SM . Statin trials and goals of cholesterol-lowering therapy. Circulation 1998; 97:1436–1439.
McKenney JM . Lovastatin: a new cholesterol-lowering agent. Clin Pharm 1988; 7:21–36.
Miura S, Saku K . Ezetimibe, a selective inhibitor of the transport of cholesterol. Intern Med 2008; 47:1165–1170.
Grigore L, Norata GD, Catapano AL . Combination therapy in cholesterol reduction: focus on ezetimibe and statins. Vasc Health Risk Manag 2008; 4:267–278.
Kong W, Wei J, Abidi P, et al. Berberine is a novel cholesterol-lowering drug working through a unique mechanism distinct from statins. Nat Med 2004; 10:1344–1351.
Abidi P, Zhou Y, Jiang JD, Liu J . Extracellular signal-regulated kinase-dependent stabilization of hepatic low-density lipoprotein receptor mRNA by herbal medicine berberine. Arterioscle Thromb Vasc Biol 2005; 25:2170–2176.
Lee YS, Kim WS, Kim KH, et al. Berberine, a natural plant product, activates AMP-activated protein kinase with beneficial metabolic effects in diabetic and insulin-resistant states. Diabetes 2006; 55:2256–2264.
Huang C, Zhang Y, Gong Z, et al. Berberine inhibits 3T3-L1 adipocyte differentiation through the PPARgamma pathway. Biochem Biophys Res Commun 2006; 348:571–578.
Glass CK, Witztum JL . Atherosclerosis: the road ahead. Cell 2001; 104:503–516.
Ross R . The pathogenesis of atherosclerosis: a perspective for the 1990s. Nature 1993; 362:801–809.
Ross R . Atherosclerosis: an inflammatory disease. N Engl J Med 1999; 340:115–126.
Steinberg D, Parthasarathy S, Carew TE, Khoo JC, Witztum JL . Beyond cholesterol. Modifications of low-density lipoprotein that increase its atherogenicity. N Engl J Med 1989; 320:915–924.
Quinn MT, Parthasarathy S, Fong LG, Steinberg D . Oxidatively modified low density lipoproteins: a potential role in recruitment and retention of monocyte/macrophages during atherogenesis. Proc Natl Acad Sci USA 1987; 84:2995–2998.
Frostegard J, Nilsson J, Haegerstand A, Hamsten A, Wigzell H, Gidlund M . Oxidized low density lipoprotein induces differentiation and adhesion of human monocytes and the monocytic cell line U937. Proc Natl Acad Sci USA 1990; 87:904–908.
Bobryshev YV . Monocyte recruitment and foam cell formation in atherosclerosis. Micron 2006; 37:208–222.
Pataki M, Lusztig G, Robenek H . Endocytosis of oxidized LDL and reversibility of migration inhibition in macrophage-derived foam cells in vitro. A mechanism for atherosclerosis regression? Arterioscler Thromb 1992; 12:936–944.
de Villiers WJ, Smart EJ . Macrophage scavenger receptors and foam cell formation. J Leukoc Biol 1999; 66:740–746.
Qiao JH, Tripathi J, Mishra NK, et al. Role of macrophage colony-stimulating factor in atherosclerosis: studies of osteoporotic mice. Am J Path 1997; 150:1687–1699.
Smith JD, Trogan E, Ginsberg M, Grigaux C, Tian J, Miyata M . Decreased atherosclerosis in mice deficient in both macrophage colony stimulating factor (op) and apolipoprotein E. Proc Natl Acad Sci USA 1995; 92:8264–8268.
Goldstein JL, Ho YK, Basu SK, Brown MS . Binding site on macrophages that mediates uptake and degradation of acetylated low density lipoprotein, producing massive cholesterol deposition. Proc Natl Acad Sci USA 1979; 76:333–337.
van Berkel TJ, Out R, Hoekstra M, Kuiper J, Biessen E, van Eck M . Scavenger receptors: friend or foe in atherosclerosis? Curr Opin Lipidol 2005; 16:525–535.
Kunjathoor VV, Febbraio M . Podrez EA, et al. Scavenger receptors class A-I/II and CD36 are the principal receptors responsible for the uptake of modified low density lipoprotein leading to lipid loading in macrophages. J Biol Chem 2002; 277:49982–49988.
Takahashi K, Takeya M, Sakashita N . Multifunctional roles of macrophages in the development and progression of atherosclerosis in humans and experimental animals. Med Electron Microsc 2002; 35:179–203.
Han CY, Pak YK . Oxidation-dependent effects of oxidized LDL: proliferation or cell death. Exp Mol Med 1999; 31:165–173.
Piedrahita JA, Zhang SH, Hagaman JR, Oliver PM, Maeda N . Spontaneous hypercholesterolemia and arterial lesions in mice lacking apolipoprotein E. Proc Natl Acad Sci USA 1992; 89:4471–4475.
Plump AS, Smith JD, Hayek T, et al. Severe hypercholesterolemia and atherosclerosis in apolipoprotein E-deficient mice created by homologous recombination in ES cells. Cell 1992; 71:343–353.
Reddick RL, Zhang SH, Maeda N . Atherosclerosis in mice lacking Apo E: evaluation of lesional development and progression. Arterioscler Thromb 1994; 14:141–147.
Zeng X, Zeng X . Relationship between the clinical effects of berberine on severe congestive heart failure and its concentration in plasma studied by HPLC. Biomed Chromatogr 1999; 13:442–444.
Leslie NR, Downes CP . PTEN function: how normal cells control it and tumour cells lose it. Biochem J 2004; 382(Pt 1):1–11.
Vlahos CJ, Matter WF, Hui KY, Brown RF . A specific inhibitor of phosphatidylinositol3-kinase 2-(4-morpholinyl)-8-phenyl-4H-1-benzopyran-4-one (LY294002). J Biol Chem 1994; 269:5241–5248.
Patel L, Pass I, Coxon P, Downes CP, Smith SA, Macphee CH . Tumor suppressor and anti-inflammatory actions of PPARgamma agonists are mediated via upregulation of PTEN. Curr Biol 2001; 11:764–768.
Lee SY, Hur GY, Jung KH, et al. PPAR-gamma agonist increase gefitinib's antitumor activity through PTEN expression. Lung Cancer 2006; 51:297–301.
MacDougald OA, Lane MD . Transcriptional regulation of gene expression during adipocyte differentiation. Annu Rev Biochem 1995; 64:345–373.
Tontonoz P, Hu E, Spiegelman BM . Regulation of adipocyte gene expression and differentiation by peroxisome proliferator activated receptor gamma. Curr Opin Genet Dev 1995; 5:571–576.
Kleemann R, Zadelaar S, Kooistra T . Cytokines and atherosclerosis: a comprehensive review of studies in mice. Cardiovasc Res 2008; 79:360–376.
Lee CH, Chen JC, Hsiang CY, Wu SL, Wu HC, Ho TY . Berberine suppresses inflammatory agents-induced interleukin-1beta and tumor necrosis factor-alpha productions via the inhibition of IkappaB degradation in human lung cells. Pharmacol Res 2007; 56:193–201.
Zhou H, Mineshita S . The effect of berberine chloride on experimental colitis in rats in vivo and in vitro. J Pharmacol Exp Ther 2000; 294:822–829.
Li F, Wang HD, Lu DX, et al. Neutral sulfate berberine modulates cytokine secretion and increases survival in endotoxemic mice. Acta Pharmacol Sin 2006; 27:1199–1205.
Cao MW, Murao K, Imachi H, et al. Phosphatidylinositol 3-OH kinase-Akt/protein kinase B pathway mediates Gas6 induction of scavenger receptor a in immortalized human vascular smooth muscle cell line. Arterioscler Thromb Vasc Biol 2001; 21:1592–1597.
Van Eck M, De Winther MP, Herijgers N . et al. Effect of human scavenger receptor class A overexpression in bone marrow-derived cells on cholesterol levels and atherosclerosis in ApoE-deficient mice. Arterioscler Thromb Vasc Biol 2000; 20:2600–2606.
Takahashi N, Kawada T, Goto T, et al. Abietic acid activates peroxisome proliferator-activated receptor-gamma (PPARgamma) in RAW264.7 cells and 3T3-L1 adipocytes to regulate gene expression involved in inflammation and lipid metabolism. FEBS Lett 2003; 550:190–194.
Sarén P, Welgus HG, Kovanen PT . TNF-alpha and IL-1beta selectively induce expression of 92-kDa gelatinase by human macrophages. J Immunol 1996; 157:4159–4165.
Kaakinen R, Lindstedt KA, Sneck M, Kovanen PT, Orni K . Angiotensin II increases expression and secretion of cathepsin F in cultured human monocyte-derived macrophages: an angiotensin II type 2 receptor-mediated effect. Atherosclerosis 2007; 192:323–327.
Mizoguchi T, Edano T, Koshi T . A method of direct measurement for the enzymatic determination of cholesteryl esters. J Lipid Res 2004; 45:396–401.
Hong S, Huo H, Xu J, Liao K . Insulin-like growth factor-1 receptor signaling in 3T3-L1 adipocyte differentiation requires lipid rafts but not caveolae. Cell Death Differ 2004; 11:714–723.
Jin S, Zhai B, Qiu Z, Wu J, Lane MD, Liao K . c-Crk, a substrate of the insulin-like growth factor-1 receptor tyrosine kinase, functions as an early signal mediator in the adipocyte differentiation process. J Biol Chem 2000; 275:34344–34352.
de la Llera Moya M, Atger V, Paul JL, et al. A cell culture system for screening human serum for ability to promote cellular cholesterol efflux. Arterioscler Thromb 1994; 14:1056–1065.
Acknowledgements
We thank Dr Christopher Glass (University of California, San Diego) for kindly providing the SR-A promoter construct. This work was supported by grants 90208007, 30521005 and 30623002 from National Nature Sciences Foundation of China, 2002CB513000 and 2006CB910700 from Ministry of Sciences and Technology of China.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary information, Figure S1
Berberine induces foam cell formation and cholesterol accumulation in RAW264.7 cell. (PDF 151 kb)
Supplementary information, Figure S2
Berberine induced foam cell formation was blocked by PI3-kinase inhibitor, LY294002. (PDF 99 kb)
Supplementary information, Figure S3
Lovastatin does not induce foam cell formation in either mouse primary macrophage or RAW264.7 cell. (PDF 63 kb)
Supplementary information, Figure S4
LDL receptor expression in liver of berberine treated apoE−/− mice. (PDF 39 kb)
Rights and permissions
About this article
Cite this article
Li, K., Yao, W., Zheng, X. et al. Berberine promotes the development of atherosclerosis and foam cell formation by inducing scavenger receptor A expression in macrophage. Cell Res 19, 1006–1017 (2009). https://doi.org/10.1038/cr.2009.76
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cr.2009.76
Keywords
This article is cited by
-
MicroRNA-296: a promising target in the pathogenesis of atherosclerosis?
Molecular Medicine (2018)
-
Cholesterol-Lowering Nutraceuticals Affecting Vascular Function and Cardiovascular Disease Risk
Current Cardiology Reports (2018)
-
Therapeutic Potential and Mechanisms of Berberine in Cardiovascular Disease
Current Pharmacology Reports (2016)
-
AMPK activation—protean potential for boosting healthspan
AGE (2014)
-
Visfatin induces cholesterol accumulation in macrophages through up-regulation of scavenger receptor-A and CD36
Cell Stress and Chaperones (2013)