Abstract
The rapidly changing field of gene therapy promises a number of innovative treatments for cancer patients. Advances in genetic modification of cancer and immune cells and the use of oncolytic viruses and bacteria have led to numerous clinical trials for cancer therapy, with several progressing to late-stage product development. At the time of this writing, no gene therapy product has been approved by the United States Food and Drug Administration (FDA). Some of the key scientific and regulatory issues include understanding of gene transfer vector biology, safety of vectors in vitro and in animal models, optimum gene transfer, long-term persistence or integration in the host, shedding of a virus and ability to maintain transgene expression in vivo for a desired period of time. Because of the biological complexity of these products, the FDA encourages a flexible, data-driven approach for preclinical safety testing programs. The clinical trial design should be based on the unique features of gene therapy products, and should ensure the safety of enrolled subjects. This article focuses on regulatory considerations for gene therapy product development and also discusses guidance documents that have been published by the FDA.
Similar content being viewed by others
Introduction
Initially, scientists pursued gene therapy for the administration of genetic material to treat genetic diseases, and it was soon adapted for cancer therapy. Approximately two-thirds of the clinical trials in gene therapy have been aimed at the treatment of various types of cancers.1 Past and current scientific advances have facilitated development of selectively targeted vectors that are efficient in gene transfer and reduce off-target effects. Several different strategies for targeting tumors are being pursued, including gene delivery of tumor antigens and growth factors, gene-modified antigen-presenting cells, gene editing in vivo, gene interference by vectored RNA interference, suicide gene therapy, and native oncolytic viruses and bacteria, with or without genetic modifications.
Antisense oligonucleotides have also been used for silencing the genes involved in development of cancer.2 Recently, short double-stranded RNA molecules termed small-interfering RNAs (siRNAs) and micro-interfering RNAs (miRNA), emerged as interesting molecules with potential therapeutic value.3, 4 siRNAs have multiple types of off-target effects, but there are several methods to help mitigate them. MicroRNA-like off-target effects can be mitigated by siRNA redundancy, siRNA pooling or chemical modification.5 In addition, Zinc-finger nucleases (ZFNs), transcription activator-like effector nucleases (TALENs) and clustered, regularly interspaced, short palindromic repeat (CRISPR)/CRISPR-associated (Cas)-9 systems comprise a powerful class of genome-editing techniques. ZFNs and TALENs enable a broad range of genetic modifications by inducing DNA double-strand breaks that gives rise to permanent gene disruptions and insertions.6
Recently, researchers have also focused on targeting the immune system using chimeric antigen receptor modified T cells and TCR modified T cells for cancer therapy.
In the United States, gene therapies are subject to oversight by two federal agencies within the Department of Health and Human Services: (i) the Food and Drug Administration (FDA), and (ii) the Office of Biotechnology Activities (OBA) at the National Institutes of Health. Gene therapy protocols are reviewed by the Recombinant DNA Advisory Committee (RAC), organized by OBA. The FDA and RAC have overlapping review roles, but with distinct responsibilities—both FDA and RAC consider preclinical and clinical issues. However, RAC serves as an open forum to publicly examine gene therapy concerns that extend beyond safety and efficacy to the consideration of ethical, legal and social implications.7 In contrast, FDA’s reviews and deliberations are confidential, unless scientific issues are discussed publicly at an FDA Advisory Committee meeting. RAC's recommendations are non-binding, while the FDA has the legal authority to regulate gene and cell therapy products under the Investigational New Drug (IND) application, the Biologics License Application (BLA) and the Investigational Device Exemption (IDE). These regulations are found in 21 CFR 312, 21 CFR 600 and 21 CFR 800, respectively. Cancer gene therapy (CGT) products are evaluated by the Office of Cellular, Tissue and Gene Therapies (OCTGT) in the Center for Biologics Evaluation and Research (CBER). Because CGT research poses novel scientific and regulatory challenges, the FDA has published several guidance documents for sponsors and investigators, which we describe in more detail in this article. In addition, the FDA has held numerous advisory committee discussions to seek advice on scientific issues involved with this class of product.
This article discusses the different types of CGT cancer products that OCTGT regulates, as well as key chemistry, manufacturing and controls (CMC) considerations, preclinical testing considerations, and clinical trial design and monitoring issues.
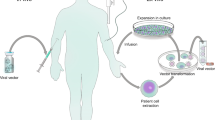
Table 1 summarizes the types of CGT products regulated by the OCTGT. For in vivo gene transfer, vectors are used to deliver the desired genes to cells in the patient’s body. In some circumstances, gene therapy vectors are mixed with liposomes and are delivered using a specialized catheter or a gene gun. For ex vivo gene transfer, cells are transduced with a vector, cultured or expanded and infused into the patient. Thus, a vector is a key component for CGT products, and a vehicle for delivering the therapeutic gene component. We describe different types of vectors and gene-modified cells in the following sections.
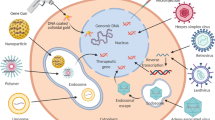
Gene transfer vectors are generally classified into two types: viral and nonviral. Viral vectors by nature offer high levels of transduction efficiency. The most common viral vectors used in clinical trials include, retrovirus, lentivirus, adenovirus, adeno-associated virus (AAV), herpes simplex virus, poxvirus and others (Table 1). These vectors generally are designed to deliver genes for tumor-associated antigens and growth factors. Each of the vector systems has its own unique advantages and limitations for gene therapy applications, and may require further modification for therapeutic use. Replication-competent retrovirus can permanently integrate into the genome of infected cells and requires cell division for transduction.8 Lentiviruses transduce not only proliferating cells but also non-proliferating cells, and lead to prolonged gene expression. Adenoviral vectors can deliver genes to dividing and non-dividing cells with very high transduction efficiency, but often stimulate an immune response to the infected cells, resulting in a loss of therapeutic gene expression after injection.9 Similar to adenoviruses, AAV can infect dividing and non-dividing cell types, but can transfect only a limited size of DNA (<5 kb).10 AAV vectors pose little toxicity, since this virus does not cause any pathologic effects in humans.11 Herpes simplex virus vectors have the advantage of being able to infect non-dividing cells, and have the capacity to carry large exogenous DNA (~40 kb); but cytotoxicity and maintenance of transgene expression can limit their therapeutic applications.8
Attenuated bacterial vectors derived from Listeria or Salmonella species have been used as cancer vaccines delivering foreign genes to elicit sustained and therapeutic immune responses. Some bacteria naturally target antigen-presenting cells, which provide a strong adjuvant effect due to their microbial origin.12 These bacterial vaccines are being used alone or in combination with chemotherapy and radiotherapy or immune modulators (for example, anti-cytotoxic T-lymphocyte antigen-4, anti-PD-1 antibody, imiquimod, GVAX (granulocyte–macrophage colony-stimulating factor gene-transfected tumor cell vaccine)).
In addition, various oncolytic viruses with or without genetic modification are also being tested. Oncolytic viruses may be replication competent or attenuated viruses, for example, adenoviruses, vaccinia, herpes simplex viruses, measles virus, reovirus, vesicular stomatitis virus, Newcastle disease virus and others.
The other common in vivo gene delivery nonviral vector includes naked plasmid DNA that is administered systemically or into tumor or non-tumor tissues. Plasmid vectors are episomal, meaning they do not integrate in the host genome, and thus are lost when cells divide. Plasmid vectors have advantages over viral vectors, which may pose problems such as endogenous virus recombination, oncogenic effects and unexpected immune response. Further, plasmid vectors are simple to use, easy to produce on a large scale and generate a less severe immune response than does virus-mediated delivery.
Several new techniques are being developed for naked DNA delivery using physical methods to overcome safety issues and improve gene expression in vivo. Plasmid vectors are often incorporated in liposomes13 or nanoparticles14 for in vivo gene delivery. Liposomes made of cationic lipids, such as quaternary ammonium detergents and cationic cholesterol are frequently used. DNA can also be delivered using a gene gun; it is adsorbed on to microscopic gold particles and ‘shot’ into cells with a helium-pressured gun. Other physical methods to introduce a gene into nuclei include electroporation, ultrasound, and hydrodynamic delivery.15 The FDA has not yet issued a specific guidance for products containing nanoscale materials. However, it has recently issued guidance for the products involving application of nanotechnology.16 The relevant guidance documents are listed in Table 3.
Vectors expressing immunostimulatory molecules such as tumor-associated antigen, TCR ligands, costimulatory molecules, growth factors, antibody fragments, ligands and others are being used to transfect cancer cells, dendritic cells and other types of cells to be administered as cancer vaccines. Dendritic cells may also be pulsed with proteins or RNA from tumor cells to be used as a cancer vaccine.
To further enhance targeting, T-cell populations are being genetically modified using vectors encoding TCR genes. Adoptive transfer of these lymphocytes transduced with HLA-restricted TCR chains (α and β) are being tested in clinical trials. However, the TCR recognition is dependent on presentation of peptide in context of an appropriate HLA molecule, this limits the scope of these TCR-based products to patients with the correct HLA type. Therefore the use of chimeric antigen receptor modified T cells, which recognize target antigens directly without a requirement for presentation in the context of HLA has spurred great attention. Currently, ∼100 clinical studies are ongoing worldwide with genetically modified T-cell therapy products for various cancer indications. Among these clinical studies, 61 trials are in the United States (https://clinicaltrials.gov).
Chemistry, manufacturing and controls considerations
The following section discusses regulatory considerations for CMC of CGT products.
CGT product components
The FDA's primary objectives when reviewing an IND are, in all phases of the investigation, to assure the safety and rights of subjects; and, in phases 2 and 3, to assure that the quality of the scientific evaluation of drugs is adequate to permit an evaluation of the drug's effectiveness and safety (21 CFR 312.22(a)). Detailed information on CMC considerations can be found in an FDA document entitled, ‘Guidance for FDA Reviewers and Sponsors: Content and Review of Chemistry, Manufacturing, and Control (CMC) Information for Human Gene Therapy Investigational New Drug Applications (INDs)’17 (Table 3).
The sponsor is required to provide complete information on all components and materials used during the manufacture of a gene therapy product. These components may include vector, cells, plasmid, and other materials and reagents. In addition, the sponsor is required to provide information on both the manufacturing process and facility.
The most commonly used vectors in CGT clinical trials are listed in Table 1. Sponsors should provide in regulatory submissions detailed information about the vector used in the CGT product. This includes type of vector and vector construction, vector diagram and sequence analysis. Sponsors should also provide a description of the history and detailed derivation of the CGT vector and its sources. In addition, an IND submission should include the following: a diagram of the vector construct used for generation of the CGT product, with relevant restriction sites, gene insert, regulatory elements such as promoter, enhancer, and polyadenylation signal and selection markers.17 In general, for vectors that are <40 kb in size, the entire vector should be fully sequenced and analyzed. The sponsor should also include a summary of the sequence analysis, with promoters, coding sequences, polyadenylation signals, origins of replication and restriction sites. For vectors sized⩾40 kb, the entire vector sequencing may not be necessary. However, sequence analysis should be performed to analyze important components of the vector, such as the gene insert and its flanking regions, along with any regions of the vector that were modified during product development.17
For cells and cell substrates used in the production of CGT products, the FDA requires information about vector-transfected cells, whether autologous or allogeneic, including cell source and history, and general characteristics of the cells. For autologous or allogeneic cells used to make ex vivo gene-modified cell products, the FDA requires information about the source of cells, mobilization protocol and collection or recovery method used to obtain cells.18 If cells are obtained from a donor, donor screening and testing should be performed to determine donor eligibility as described in the FDA guidance, ‘Guidance for Industry: Eligibility Determination for Donors of Human Cells, Tissues, and Cellular and Tissue-Based Products (HCT/Ps)’.18 The cell bank system includes master cell bank and working cell bank used in the product manufacture. The IND submission should include: a description of the history, source, derivation and characterization of each cell bank, including master cell bank and working cell bank, used in the product manufacture. For the viral banks, including both the master viral bank and the working viral bank, submissions should also include issues such as culture conditions during scale up, testing of media and other reagents used during production. For further information on cell banks, sponsors are referred to ‘Points to Consider in the Characterization of Cell Lines Used to Produce Biologicals’,19 and International Conference on Harmonization (ICH) document Q5D, ‘Derivation and Characterization of Cell Substrates Used for Production of Biotechnological/Biological Products’.20
Reagents are defined as those materials that are used for cell growth, differentiation, selection, purification or other critical manufacturing steps, but that are not intended to be part of the final product. Since these reagents can affect the safety, potency and purity of the final product, the quality of reagents should be tested prior to their introduction into the manufacturing process. The variability of reagents should be controlled, and vendor qualifications should be built into the quality assurance process. When available, FDA-approved or -cleared reagents, or clinical grade reagents, are highly recommended. Often research-grade reagents are being used in the manufacturing process; however, if these are used, the FDA recommends including a certificate of analysis. Furthermore, if the reagent is human-derived or animal-derived material, additional tests may be needed to verify safety. The FDA recommends establishing a qualification program for the reagents used in the manufacturing process to demonstrate the absence of potentially harmful substances.21
CGT product manufacturing procedure and testing
Manufacturing procedures include vector derivation, purification, preparation and testing of cell banks, and final formulation of the product. Sponsors should provide to the FDA descriptions of all procedures used during the manufacturing process. This information will be used to assess the identity, quality, purity, potency, safety, stability and comparability of the final CGT product. It is the sponsor’s responsibility to provide information on methods, facilities and manufacturing controls to ensure that the CGT product meets appropriate standards of safety, identity, potency, quality and purity. It is also the sponsor’s responsibility to consider how to best ensure the implementation of standards, practices and procedures that conform to current Good Manufacturing Practice for their product and manufacturing operation.21 The manufacturer should establish acceptance criteria for specified attributes of each material. The certificate of analysis for each lot of material should meet established acceptance criteria. For further information, refer to the FDA ‘Guidance for Industry: current Good Manufacturing Practice for Phase 1 Investigational Drugs’.21
Manufacturing procedure
The FDA oversees the manufacturing processes for CGT products to ensure product safety and quality. The evaluation of CGT products will involve assessing the components used in product manufacturing, which include all reagents, vectors and cells; all procedures and steps in the manufacturing process; final product formulation and characterization; and evaluation of manufacturing process controls. In terms of procedures and steps of the manufacturing process, if the procedures involve gene therapy vector products, vector production techniques and purification methods will be assessed. If the process involves ex vivo gene-modified cells, the FDA will evaluate the method of cell collection/processing/culture conditions, irradiation of the tumor cells and final harvest of the cells.
CGT product testing
It is important to identify quality parameters and critical product attributes to ensure lot-to-lot consistency in the manufacturing process, and the desired clinical effect of the final product. CGT product testing should include microbiological testing (including sterility, mycoplasma and adventitious viral agents) to ensure safety and assessments of other product characteristics such as identity, purity (including endotoxin) and potency. The FDA recommends performing these tests throughout the manufacturing process, including on the manufacture of cell banks, to evaluate the manufacturing process itself and to ensure the quality and consistency of the CGT product. The specifications used for intermediate acceptance criteria and final product release criteria should be described. Specifications are the quality standards (that is, tests, analytical procedures and acceptance criteria) that confirm the quality of products, product components and other materials used in the production of a product. Specifications should be appropriate to the stage of product development, because release criteria should be refined and tightened as product development progresses toward licensure.
Adventitious agent testing
As appropriate, the sponsor should perform and describe adventitious agent testing as discussed in ‘Points to Consider in the Characterization of Cell Lines Used to Produce Biological Products’19 and ICH guidance Q5A: ‘Guidance on Viral Safety Evaluation of Biotechnology Products Derived From Cell Lines of Human or Animal Origin’.22 Both in vitro and in vivo viral testing are recommended, to ensure that the product is free from adventitious agents. In vitro viral testing should be performed on all cell banks, viral banks and final vector product. A number of assays have been developed to detect many known viruses in the CGT final product and the gene-modified cell product, such as PCR, quantitative PCR, antibody detection and so on, and next generation sequencing technology. If human cell lines are used in the therapeutic product, donor testing for human pathogens and human viral agents should be performed, as described in the FDA guidance.18
Identity
The final CGT product must be verified by assays that will identify the product for proper labeling and distinguish it from other products being processed in the same facility. Testing may include an assay measuring the presence of a vector (that is, expression assay, restriction enzyme digest) and an assay specific to the cellular component of the final product (that is, cell surface markers and so on). PCR-based methods and transgene expression-based immunoassays are also commonly used to confirm identity in the final product lot-release testing as well. For the final product, identity testing is important to ensure that the contents of the vial are labeled appropriately. Additional information on labeling is described in 21 CFR 312.6(a).
Purity
Testing for purity reflects the safety risks associated with the impurities and the ability of the process to remove those impurities. Impurities can be either product-related or process-related components that can be carried through to the final product. Purity testing should include assays for pyrogenicity/endotoxin, residual proteins, DNA, RNA or any reagents/components used during CGT product manufacturing. The purity testing should also include assays for solvents used during production and purification, and reagents used during manufacture. If the product is a genetically modified ex vivo cell therapy product, then purity testing should include a measurement of contaminating cell types or cell debris. The purity testing and specifications for release should be established at an early stage of the manufacturing process. For further information, refer to ICH Q3 on ‘Impurities’.23, 24, 25
Safety
Microbiological testing should be performed on cell banks, in-process intermediates and the final product, as appropriate. Microbiological testing includes sterility testing for bacterial and fungal contamination and mycoplasma testing discussed in 21 CFR 610.12 and in the United States Pharmacopoeia (USP) <71>.26, 27 Note that under 21 CFR 610.9, prior to product licensing, the alternative method must be shown to provide assurances of the safety, purity, potency and effectiveness of the biological product equal to or greater than the assurances provided in the 21 CFR 610.12. Sterility testing should be performed on both the in-process and the final product. In-process sterility testing should be performed at critical points during manufacturing, such as during purification, or after ex vivo gene modification or extended culture periods. A ‘negative’ or ‘no growth’ is an accepted criterion of the sterility test used for lot release of CGT products.
Mycoplasma testing should be performed on the product at the manufacturing stage when the test is most likely to detect contamination; such as after pooling of cultures for harvest, but prior to cell washing. Testing should be conducted on both cells and supernatant. Due to the limited dating period of many ex vivo genetically modified cellular products, it is frequently not feasible for a sponsor to perform the recommended culture-based assay for release testing. In those cases, we recommend the use of PCR-based mycoplasma assays or another rapid detection assay during product development. However, it is the sponsor’s responsibility to provide data to demonstrate that the PCR or other rapid detection test results have adequate sensitivity and specificity compared with the culture-based mycoplasma testing method.19
Other tests in addition to microbiological and adventitious agent testing, identity testing and purity testing mentioned above may also be required. General safety testing is required for licensure of all gene therapy vector products described in 21 CFR 610.11. However, cellular therapy products are exempt from general safety testing (21 CFR 610.11(g)).
Depending on the type of CGT products, if the final product is a genetically modified cell therapy, the minimum release criterion for viability is generally set at 70%. For administration of a gene vector, the dose should be described as the concentration of plasmid DNA, viral particle number or titer.17
Stability
The shelf lives of CGT products may vary widely, depending on the nature of the product and its storage conditions. CGT products should be assessed for stability to support the dating period. Stability testing should be designed on the basis of a comprehensive understanding of the final product and its intended use. Stability testing must be designed during early phases of the clinical trial to verify the storage conditions, and performed in all phases of clinical trials to demonstrate that the product or components are sufficiently stable for the time period of the clinical trial (21 CFR 312.23(a)(7)(ii)). Stability testing should be based on real-time, real-temperature studies and should include a measure of product integrity, sterility, identity, purity, quality and other applicable assays. Potency assays in stability testing, similar to lot release testing, should measure a relevant biological functionality either in vitro or in vivo. Stability testing must demonstrate that the product is within acceptable chemical and physical limits. The stability profile will be provided by a combination of product-specific assays. For further information, refer to the FDA guidance for gene therapy product,17 ICH Q1A(R): ‘Stability Testing of New Drugs and Products’28 and the guideline, ICH Q1E: ‘Evaluation of Stability Data’.29
Potency
Potency is defined as ‘the specific ability or capacity of the product, as indicated by appropriate laboratory tests or by adequately controlled clinical data obtained through the administration of the product in the manner intended, to effect a given result’ (21 CFR 600.3(s)). Potency tests consist of either in vitro or in vivo tests, or both, which have been specifically designed for the product, based on individual product attributes. Potency measurements may include either direct measurement of biological activity, such as biological assays based on product-specific attributes, or indirect measurement of biological activity, such as surrogate markers substantiated by correlation to a relevant biological activity. The potency assay often has a high degree of variability. Measuring and calculating the CGT product activity may require multiple and frequent sampling intervals over a designated time period. It also requires analysis of multiple lots of products to compensate for the variability of assays. In general, the potency test is not required during early stages of clinical trials. However, before initiating a phase 3 study, the potency assay will need to be developed and validated during the phase 3 studies. For further information, refer to the FDA guidance entitled ‘Guidance for Industry: Potency Tests for Cellular and Gene Therapy Products, 2011’.30
Comparability
Product manufacturing may need to be scaled up as development of a CGT product progresses to later-phase clinical trials and toward marketing. Changes in manufacturing methods of a CGT product may necessitate an assessment of comparability to ensure that these changes have not affected the safety, identity, purity or efficacy of the product. The most frequently encountered issues with CGT product scale up are, (i) changes of manufacturing facilities; (ii) changes of manufacturing processes; and (iii) changes of reagents and equipment. Comparability studies are needed to bridge the early-phase product to the later-phase product and to support later-phase development or licensure.31 It is important that product characterization should be performed early in product development. Without full product characterization, it will be difficult to determine the impact of the manufacturing process or manufacturing change on the product itself.32 A comparability protocol should be well-defined for assessing the effect of specific CMC changes on the identity, purity, stability and potency of a CGT product. A comparability protocol specifies the tests and studies performed, including the analytical procedures used, and acceptance criteria to demonstrate that specified CMC changes do not adversely affect the product (ICH Guidance for Industry: Q5E, 2005).33 In general, such comparability studies should be conducted prior to phase 3 clinical trials. Consultation with OCTGT throughout the CGT product development program is recommended to ensure that the design of any additional preclinical studies is adequate to allow for seamless product development.34
Final product release criteria testing
The final product is the final formulated product used in clinical trials. Final product testing for CGT products is a challenge. Because there is considerable variability in the product manufacturing process and the active ingredient is not always well-defined, the final product testing for CGT products focuses on product characterization and lot-to-lot consistency. Final product release criteria testing should be performed on each lot of product that is manufactured. Manufacturer should establish acceptance criteria of release test methods for the final product during the early stage of the product’s development. The results and all of the proposed specifications (that is, safety, purity, potency, identity, test methods and acceptance criteria) should be satisfied for the final product. Before the product may be licensed, these parameters must be validated (21 CFR 211.165(e)). A qualification program should be established, including safety testing (sterility, endotoxin, mycoplasma and adventitious agents), functional analysis, purity testing and assays to demonstrate absence of potentially harmful substances (for example, residual solvent testing). If any component is intended to be part of the final product, such as human serum albumin or dimethyl sulfoxide, it should be listed including the concentration and source ((21 CFR 312.23(a) (7) (iv) (b)), and (21 CFR 211.84(a)).
Environment assessment and shedding studies
The FDA has recently published a guidance entitled, ‘Guidance for Industry: Determining the Need for and Content of Environmental Assessments for Gene Therapies, Vectored Vaccines and Related Recombinant Viral or Microbial Products,’ dated March 2015.35 In general, an IND is excluded from the environmental assessment. INDs for clinical studies using gene therapy products will not significantly affect the quality of the environment; because these clinical trials are closely monitored, relatively small quantities of product are involved and only a limited number of patients in a designated study group are treated. For a BLA application of a gene therapy product, a full environmental assessment is usually required unless the FDA has granted categorical exclusion (21 CFR 25.15(a)). A sponsor wishing to claim a categorical exclusion must state that the action requested qualifies for a categorical exclusion and no extraordinary circumstances exist.35
CGT products present the possibility of viral or bacterial shedding, that is, excretion/secretion of viral particles or bacteria that could be transmitted to other individuals. Although product-based viruses and bacteria may not be as infectious or as virulent as the parent strain of a virus or bacterium, the possibility of transmission raises safety concerns. An analysis of data collected from patients in clinical gene therapy trials demonstrated that shedding of viral vectors occurs in practice, and is mainly determined by the type of vector and the route of vector administration.36 A qualitative model presented in the study can help to determine the risk of shedding occurring via the different excretion routes.37
To understand this risk, shedding studies should be conducted in the target patient population. Recently, the FDA has released a guidance document for shedding studies, entitled ‘Guidance for Industry: Design and Analysis of Shedding Studies for Virus or Bacteria-Based Gene Therapy and Oncolytic Products,’ August 2015.38 Shedding studies are only recommended for oncolytic and virus-based gene therapy products, not for genetically modified mammalian cells and other products. The purpose of the shedding study is to collect information about the likelihood of transmission to untreated individuals and measures to prevent such transmission. Shedding data collected during a clinical trial will provide a comprehensive understanding of the shedding profile of CGT products in the target patient population(s). Typically, clinical shedding studies are not stand-alone studies; sponsors should consult with OCTGT in the early stages of product development for specific recommendations on their products.38
Preclinical considerations
Preclinical testing of CGT products
The diverse range of investigational gene therapy products intended for the treatment of cancer may vary in biological complexity and purported mechanisms of action. Thus, a standardized preclinical testing program, applicable to all CGT products does not exist. Instead, the FDA has taken a flexible, data-driven approach to assess the safety of these therapies in the context of the product’s biology and the intended clinical indication. Nevertheless, there are general scientific and regulatory considerations common to all CGT products, which can help guide the design of the preclinical testing program.
According to federal regulation (21 CFR 312.23 (a) (8)), the submission of adequate pharmacological and toxicological information to support a proposed clinical investigation is required. This information supports a position of reasonable safety for administration of a specific investigational product to subjects participating in a specific clinical trial. To meet this requirement, preclinical studies are conducted to: (i) identify potential target organs/tissues of toxicity and the temporal profile (onset and possible resolution) of any observed toxicity; (ii) identify an appropriate clinical starting dose level and inform the clinical dose-escalation scheme and dosing regimen; and (iii) identify potentially relevant parameters that should be monitored in the subjects to assess safety and bioactivity.
The biology, mechanism of action and manufacturing process can vary significantly for each CGT product. As a consequence, the safety concerns associated with each product can also vary significantly and may be multi-faceted. These concerns may stem from the biology of the product itself, such as autoimmunity due to the expression of target/off-target antigen(s) in normal tissues; a cytokine storm from exuberant immune stimulation or unwanted viremia due to administration of a replication competent viral vector. The manufacturing process (for example, introduction of adventitious agents) or the delivery procedure (for example, local tissue toxicity from the use of an invasive route of administration or delivery modality (for example, electroporation)) can influence the safety profile of the administered gene therapy product. It is thus important to consider such factors when designing a preclinical testing program for this class of products. Therefore, a stepwise approach for the preclinical testing paradigm is recommended to enable the use of accumulated knowledge from early studies/existing data to inform definitive studies needed to address any remaining gaps or concerns related to product activity and safety.
Use of existing preclinical and clinical data from related products
In some cases, additional in vitro and in vivo preclinical studies may not be needed to support the clinical investigation of a new CGT product if a sufficient body of safety and activity data already exists with related products. The sponsor should provide sufficient scientific explanation for the relevance of existing data to support the safety of the investigational product. These data may come from publications in peer-reviewed journals, other regulatory files (with permission to access), public discussions/meetings, unpublished work of other colleagues and other sources. The determination of the adequacy of such data is on a case-by-case basis, thus early discussion with the FDA is recommended.
Proof-of-concept studies
The first step in the translation of a CGT product from bench to clinical investigation is the conduct of in vitro and in vivo studies that help define the pharmacological properties of the product. These studies are often termed proof-of-concept studies. They may range in scale and complexity from the use of an in vivo xenograft tumor model to in vitro studies showing lysis of tumor cells by the product. The goal of proof-of-concept studies is to meet several objectives: (1) establish a scientific basis for conducting the clinical trial; (2) determine a minimal pharmacologically effective dose level of the product; (3) characterize a potential dose–response relationship; (4) optimize the dosing regimen; (5) optimize the route of product administration; and (6) provide the basis for the animal species and/or animal disease model(s) used for further preclinical testing. Depending on the particular CGT product, it may be beneficial to evaluate the anti-tumor immune response generated by the product following administration in a tumor-bearing animal model. This helps identify whether a correlation exists between immune response and functional outcome, such as tumor growth inhibition or eradication. The information can contribute to understanding the product’s mechanism of action, as well as inform the development of activity biomarkers for possible application in the clinical trial.
Animal species selection
The selection of biologically relevant animal species for toxicology testing of CGT products is an important aspect of the preclinical development program. The use of biologically irrelevant animal species should be avoided, as the information obtained would not be informative and may even lead to incorrect conclusions regarding product safety. When biological and anatomical differences exist between humans and animals, these limitations should be recognized to allow for appropriate interpretation of the animal study results and translation of a potentially safe product dose level to humans. In some cases a biologically relevant animal species may not exist and the submission of in vitro data alone may be sufficient.
One key criterion to establish biological relevance is whether the gene therapy product is pharmacologically active in the selected animal species. For instance, some human cytokines exhibit biological activity in a species-specific manner; therefore, evaluation of the expressed human protein in certain animals would not yield informative data. In such cases, the use of a CGT product that encodes the animal analog transgene may be appropriate in preclinical testing. For CGT products intended to induce a cellular immune response via antigen presentation, the use of transgenic animals that express the relevant human HLA may be an acceptable approach. Additional factors to consider when establishing biological relevance of an animal species include: (1) tissue expression profile of the target in animals (for example, antigen, receptor and so on), (2) target binding profile in animals, (3) permissiveness to infection and replication of the viral vector in animals. This is not an exhaustive list of factors, as CGT products comprise a range of mechanisms of action which dictate the pharmacological activity of the product, and thus influence animal species selection.
Toxicology studies
Toxicology studies help to establish the safety profile of an investigational CGT product, thus, the conduct of these studies is an important step in the advancement of a product to initial clinical investigation. The primary objective of the toxicology studies is to identify, characterize and quantify potential local and systemic toxicities. If the investigational product exhibits toxicities, the temporal profile (that is, onset and possibility of resolution) and dose–response relationship should be investigated to provide a more comprehensive picture of the product safety. The data from these studies inform the design of the initial clinical trial by providing information on a potentially safe clinical starting dose level, dose-escalation scheme, dosing route and dosing schedule. Data from the toxicology studies may also help define subject eligibility criteria and appropriate clinical monitoring for potential local and systemic toxicities. Together with the proof-of-concept studies, toxicology studies contribute to determination of a reasonable benefit/risk profile of the CGT product for clinical investigation.
Preclinical study design
The design of the preclinical studies should mimic the planned clinical trial design to the extent possible, including dosing regimen and route of administration, because these parameters can influence the product’s safety and biological activity. Other basic design elements to enhance interpretability of the study results include: (1) appropriate randomization of study animals, (2) masked assessment of certain study parameters, (3) adequate numbers of animals, (4) appropriate control groups, (5) multiple dose levels that bracket the planned clinical dose levels, and (6) adequate study duration to allow for comprehensive assessment. For multi-component products (for example, CGT product administered with an adjuvant, two different gene therapy products administered using a prime-boost regimen and so on), evaluation of each component in addition to the final product combination is recommended to better understand the contribution of each component to the safety profile of the intended final clinical product.
Aspects of a toxicology study design for a CGT product might include traditional safety endpoints such as mortality, clinical observations, body weights, clinical pathology and histopathology. Other endpoints, including an immune response induced by the product to the target antigen, an immune response to the product itself and biodistribution of the vector to target and non-target tissues, as applicable, may also be assessed. For details on the biodistribution protocol designs refer to the ‘FDA Guidance for Industry: Gene Therapy Clinical Trials—Observing Subjects for Delayed Adverse Events’ 39 (Table 3).
CGT products comprise a diverse class of products with various purported mechanism(s) of action ranging from direct action of the product to lyse tumor cells to indirect action of the product to stimulate an anti-tumor immune response. Consequently, there is no one predefined conversion factor to enable translation of a potentially safe dose in animals to humans. The sponsor should justify with supporting scientific data on the extrapolation method used to determine the proposed clinical starting dose, dose-escalation scheme and dosing schedule.
Conduct of preclinical studies during clinical development
As an investigational CGT product advances in clinical development, the conduct of additional preclinical studies may be necessary in certain situations. If unexpected toxicities are identified during clinical development, it may be advantageous to conduct preclinical studies to better understand the mechanism of the observed toxicities and their association with the investigational product. If there are significant modifications to the manufacturing of the product such that uncertainty exists with product comparability, additional preclinical studies may be important to bridge the existing preclinical data with product manufactured using the ‘old’ process to product manufactured using the ‘new’ process. Depending on the product and target clinical population, the conduct of reproductive/developmental toxicity studies may need to be conducted in parallel with late-phase clinical trials. Considerations affecting the necessity for these studies include product biodistribution to reproductive tissues and the tissue expression profile of the target antigens in reproductive tissues.
Summary of preclinical assessment of CGT products
The preclinical assessment of a CGT product is an integral part of the overall product development from bench to bedside. It emphasizes a case-by-case approach for each investigational product, thus encouraging early discussion with the FDA. For a comprehensive summary of the preclinical assessment of CGT products, please refer to Table 3 and the ‘FDA Guidance for Industry: Preclinical Assessment of Investigational Cellular and Gene Therapy Products’ and to the ‘FDA Guidance for Industry: Clinical Considerations for Therapeutic Cancer Vaccines’ for preclinical recommendations for cancer vaccines.40, 41
Clinical considerations
Early-phase clinical trials
Early phase trials should be adequately designed to identify a safe, feasible dose and regimen to carry forward into a later-phase trial, unless toxicity issues become apparent and further development of the product is deemed unfavorable from a risk/benefit analysis. An IND protocol for a first-in-human CGT trial should contain the clinical information as outlined in Table 2. Further information may be found in the FDA guidance for industry (June 2015): Considerations for the Design of Early-Phase Clinical Trials of Cellular and Gene Therapy Products available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/default.htm.
Because of the complexity of gene therapy products, the classic paradigm of performing large oncology clinical trials, which enroll a diverse patient population to receive an off-the-shelf easily-manufactured product, may be infeasible or inefficient. Smaller and ‘smarter’ trials offer a possible conceptual path forward for clinical trial design for gene therapy products, which may be highly active in a specifically defined patient population.
Early phase trials, especially first-in-human trials, remain focused on the evaluation of safety, as in any early-phase cancer clinical trial. However, for the complex treatments of CGT, there should also be additional preliminary explorations:
-
Feasibility of administration
-
Dose exploration that may capture effective biologic activity rather than dose-limiting toxicity
-
Early evidence of potential efficacy, including specialized assessments of gene expression, immunologic changes and standard tumor responses
To streamline development of the product, knowledge of the product’s expected mechanism of action in a particular disease is essential to choose an appropriate study population, which might allow an early assessment of activity.
First-in-human oncology trials have often enrolled patients with advanced heavily pre-treated metastatic disease. Such a population may be appropriate for a product which is expected to have a rapid onset of action, independent of an intact immune system. In contrast, gene therapy products may have a more measured onset of action and/or require a functional immune system. Therefore, it may be uninformative to investigate some gene therapies in subjects with bulky or progressive metastatic disease who have ongoing immunosuppression from prior cytotoxic chemotherapies. It is essential to enroll a study population whose responses to a new treatment will provide interpretable safety and activity data.
In early-phase trials, there should be some dose and/or schedule exploration. For advanced cancer indications, significant treatment toxicities up to a predefined threshold are often expected and deemed acceptable. Unlike cytotoxic therapies, substantial toxicities that will permit identification of a maximum tolerate dose may not occur in the expected or feasible therapeutic range of CGT products. In this situation, the intent of dose/schedule exploration may be to determine the optimal biologically active dose and regimen. For some complex gene therapies, there may be substantial practical production limits on a quantity that can be produced or delivered. In this event, the trial objective may be to characterize the safety profile of the feasible dose and regimen, rather than finding the maximum tolerate dose.
A common secondary objective of early-phase clinical trials is to obtain preliminary data on product activity. In addition to standard oncology metrics to assess disease responses, specialized exploratory endpoints should be considered. For gene therapy products, these endpoints might include gene expression, cell engraftment or other immune function parameters.
Adverse event monitoring and reporting
Both acute and chronic gene therapy toxicities are often quite different than seen with cytotoxic agents. Dose-limiting toxicities may not occur during early-phase trials, and an maximum tolerate dose may not be defined. Yet, possible serious late-occurring toxicities can occur, which require appropriate planning and monitoring during development. Also, some products may be locally administered (for example, direct intratumoral injection or instillation into a specific space) and must have appropriate safety assessment for both localized and systemic toxicities. Because there may be prolonged biologic activity if there is integration of the therapeutic gene into the host genome, sponsors should consider an appropriate duration of safety assessments. An additional complicating factor is that the gene vector itself may result in toxicities that require specific vigilant monitoring. For further information, refer to FDA guidance for Industry (November 2006): Gene Therapy Clinical trials—Observing Subjects for Delayed Adverse Events available at http://www.fda.gov/cber/guidelines.htm.
Long-term follow-up
For CGT products, a broad variety of vectors have been developed. Because certain vectors, particularly retroviral, may cause insertional mutagenesis resulting in dysregulated gene expression and malignant transformation,42 or may have persistent biological activity, extended safety follow-up may be appropriate. Study subjects exposed to gene transfer technology may be at risk of developing delayed adverse events months or even years after administration. Specific testing for replication competent retrovirus, replication competent lentivirus, adenovirus and AAV are recommended.43 Thus depending on the vector type, its propensity to integrate and other factors (for example, replication competence), a long-term follow-up observation plan may be required. Considerable efforts have been undertaken to improve the safety of gene transfer, especially during the past decade. These efforts led to a public workshop, attended by industry, academic and regulatory representatives to discuss and formulate recommendations for long-term follow-up. Although some long periods (up to 15 years) of follow-up have been proposed, shorter period of observation may be suitable in individual trials. Pertinent previous preclinical and clinical experience with the product or similar products is highly relevant in the assessment of delayed adverse events. Experience with products in the same vector class, administered by a similar route, and given for the same clinical indication may contribute helpful information to determine the appropriate length of follow-up. Sponsors and investigators are referred to FDA’s guidance (Table 3) on observing subjects for delayed events.39
In selected instances in which long-term follow-up observations are generally required, it may be determined that the observations would have no clinical or scientific value based on the clinical trial population. For example, this may be true in patients with metastatic solid tumors enrolled in CGT studies. Long-term observations may be practically difficult and clinically irrelevant for the study subjects due to their short life expectancy.
Later-phase clinical trials
As costs for conduct of all phases of clinical research spiral upward, many investigators and pharmaceutical sponsors have attempted to abbreviate the drug development process by circumvention or significant abbreviation of phase 2 studies. However, a well-designed phase 2 trial can be an excellent screening discriminator to determine if further progress to phase 3 is warranted. Scant phase 2 programs may provide insufficient data on which to base the design of a phase 3 efficacy trial intended to support a license application. Importantly, an estimate of product activity can be determined in a well-conducted phase 2 trial. Inadequate phase 2 drug development can be one of the major factors accounting for failure in phase 3. Randomized phase 2 trials, due to their limited sample sizes, typically lack the statistical power for conclusive demonstration of the treatment effect of the investigational agent and provide a more limited patient experience for generalization of treatment effects to the general patient population. However, randomized phase 2 trials may provide more reliable data about treatment effect size than single-arm trial data compared with historical controls. These data may be useful when planning the design of the subsequent phase 3 trial. The quality and quantity of phase 2 development should be sufficient to provide adequate data to make a ‘go/no go’ decision about proceeding to phase 3.
In certain circumstances, highly active drugs in specific populations may be investigated in single-arm trials. Many recent drug approvals for a well-defined population (for example, ALK-positive non-small cell lung cancer) have been founded on solid preclinical mechanisms of action, which have translated to substantial responses in clinical trials. Some of these efficacy trials have occasionally been single-arm trials, which may be appropriate in the setting of advanced disease when there is no standard of care therapy.
Because data from a phase 3 trial may support a marketing application, a sponsor may choose to submit a phase 3 protocol for special protocol assessment. The special protocol assessment is a means by which the sponsor reaches an agreement with FDA on the clinical design, endpoints and statistical analysis plan prior to commencement of the phase 3 trial. FDA will document such an agreement in writing. To learn more about special protocol assessment agreements, interested sponsors are advised to refer to FDA’s guidance on this topic at www.fda.gov/downloads/Drugs/Guidances/ucm080571.pdf.
Trial endpoints
Trial endpoints must be carefully chosen and may include measures of clinical and/or biological activity of the gene product. Immunological endpoints may be considered, when applicable, to support or correlate with clinical outcomes. Choice of endpoints for phase 3 trials can be challenging, both in terms of specific selection and in terms of their assessment. Sponsors are encouraged to refer to FDA’s guidance on appropriate clinical endpoints in cancer trials (Table 3). As with any cancer therapy, oncology endpoints typically demonstrate improvements in patient survival or function. Thus, CGT products which are administered locally and intended to demonstrate a local tumor response, must demonstrate a treatment effect on other meaningful endpoints, such as improved survival or decrease of tumor-related symptoms. Assessments of immune responses (for example, T-cell activation) may provide mechanistically useful data, especially when they can be correlated to clinical outcomes. However, at this time, immune response data are regarded as secondary or exploratory endpoints. Sponsors are strongly encouraged to discuss the choice of phase 3 endpoints with FDA.
Communication with FDA
Prior to initiating a phase 1 clinical trial, sponsors are encouraged to communicate with FDA before submitting an IND. A pre-IND meeting provides an opportunity for open communication between a sponsor and CBER/FDA to discuss planned IND content and to obtain CBER/FDA advice that may prevent a clinical hold. A typical pre-IND meeting will discuss the topics, including product manufacturing and safety issues, design of animal studies, design of initial clinical study, potential clinical hold issues and clarification of regulatory requirements.44 Pre-IND meetings can make a difference. The most common clinical hold issue found in INDs submitted to CBER/FDA was insufficient information to assess the risks to subjects of the proposed study. However, of all INDs that were preceded by a pre-IND meeting, only a small percentage of INDs were placed on hold.44
In addition, the FDA encourages both formal meetings and informal communications at different product development stages (for example, at the end of phase 1, end of phase 2, or pre-biologics license application). These meetings are not unscripted brainstorming sessions. Rather, they are highly structured planned events, conducted either via teleconference or face-to-face. Sponsors must submit a meeting package at least 30 days prior to the event. Submitted pre-read materials should contain meeting objectives, a list of questions and well-organized background information for each question to be discussed. Such communications are critical to ensure that product development addresses the good manufacturing practice requirements for a licensed product.45 For more detailed information, sponsors are encouraged to visit the FDA website.46
Conclusion
With the recent successes in multiple phases of clinical trials, it seems likely that CGT will soon be included in the treatment armamentarium for various neoplastic and other indications. As with any drug for cancer therapy, gene therapies must meet the approval standard of being safe and effective. However, there are unique features and challenges for sponsors of gene therapies, as outlined in this article. FDA remains actively involved with investigators and sponsors at all stages of product development.
References
Ginn SL, Alexander IE, Edelstein ML, Abedi MR, Wixon J . Gene therapy clinical trials worldwide to 2012 – an update. J Gene Med 2013; 15: 65–77.
Dias N, Stein CA . Antisense oligonucleotides: basic concepts and mechanisms. Mol Cancer Ther 2002; 1: 347–355.
Bartel DP . MicroRNAs: genomics, biogenesis, mechanism, and function. Cell 2004; 116: 281–297.
Rythe RCC, Flynt AS, Phillips JA III, Patton JG . siRNA therapeutics: big potential from small RNAs. Gene Ther 2005; 12: 5–11.
Jackson AL, Linsley PS . Recognizing and avoiding siRNA off-target effects for target identification and therapeutic application. Nat Rev Drug Discov 2010; 9: 57–67.
Wang H, Yang H, Shivalila CS, Dawlaty MM, Cheng AW, Zhang F et al. One-step generation of mice carrying mutations in multiple genes by CRISPR/Cas-mediated genome engineering. Cell 2013; 153: 910–918.
NIH Guideline for Research Involving Recombinant or Synthetic Nucleic Acid Molecules. Available at http://osp.od.nih.gov/office-biotechnology-activities/biosafety/nih-guidelines.
Ibraheem D, Elaissari A, Fessi H . Gene therapy and DNA delivery systems. Int J Pharm 2014; 459: 70–83.
Yang Y, Su Q, Wilson JM . Role of viral antigens in destructive cellular immune responses to adenovirus vector transduced cells in mouse lungs. J Virol 1996; 70: 7209–7212.
Hermonat PL, Quirk JG, Bishop BM, Han L . The packaging capacity of adeno-associated virus (AAV) and the potential for wild-type-plus AAV gene therapy vector. FEBS Lett 1997; 407: 78–84.
Samulski RJ, Zhu X, Xiao X, Brook JD, Housman DE, Epstein N et al. Targeted integration of adeno-associated virus (AAV) into human chromosome 19. EMBO J 1991; 10: 3941–3950.
Toussaint B, Chauchet X, Wang Y, Polac B, Le Gouellec A . Live-attenuated bacteria as a cancer vaccine vector. Exp Rev Vaccines 2013; 12: 1139–1145.
Gill DR, Southern KW, Mofford KA, Seddon T, Huang L, Sorgi F et al. A placebo-controlled study of liposome-mediated gene transfer to the nasal epithelium of patients with cystic fibrosis. Gene Ther 1997; 4: 199–209.
Konstan MW, Davis PB, Wagener JS, Hilliard KA, Stern R, Milgram LJ et al. Compacted DNA nanoparticles administered to the nasal mucosa of cystic fibrosis subjects are safe and demonstrate partial to complete cystic fibrosis transmembrane regulator reconstitution. Hum Gene Ther 2004; 15: 1255–1269.
Niidome T, Huang L . Gene therapy progress and prospects: nonviral vectors. Gene Ther 2002; 9: 1647–1652.
Considering Whether an FDA-Regulated Product Involves the Application of Nanotechnology, June 2014. Available at www.fda.gov/RegulatoryInformation/Guidances/ucm257698.htm.
Guidance for FDA Reviewers and Sponsors: Content and Review of Chemistry, Manufacturing, and Control (CMC) Information for Human Gene Therapy Investigational New Drug Applications (INDs), April 2008. Available at http://www.fda.gov/cber/guidelines.htm.
Guidance for Industry: Eligibility Determination for Donors of Human Cells, Tissues, and Cellular and Tissue-Based Products (HCT/Ps), August 2007. Available at http://www.fda.gov/downloads/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/Tissue/UCM091345.pdf.
Point to Consider in the Characterization of Cell Lines Used to Produce Biologicals, July 1993. Available at http://www.fda.gov/cber/gdlns/ptccell.pdf.
ICH document Q5D: Derivation and Characterization of Cell Substrates Used for Production of Biotechnological/Biological Products (63 FR 50244, September 1998). Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/default.htm.
Guidance for Industry: cGMP for Phase 1 Investigational Drug, July 2008. Available at http://www.fda.gov/cber/guidelines.htm.
ICH Guidance on Viral Safety Evaluation of Biotechnology Products Derived from Cell Lines of Human or Animal Origin, (63 FR 51074, 24 September 1998). Available at http://www.ich.org/products/guidelines/quality/quality-single/article/viral-safety-evaluation-of-biotechnology-products-derived-from-cell-lines-of-human-or-animal-origin.html.
ICH Topic Q3 Impurities. Guidance for Industry: Q3A Impurities in New Drug Substances, February 2003. Available at http://www.fda.gov/downloads/drugs/guidancecomplianceregulatoryinformation/guidances/ucm073385.pdf.
Guidance for Industry: Q3B (R2) Impurities in New Drug Products, July 2006. Available at http://www.fda.gov/downloads/drugs/guidancecomplianceregulatoryinformation/guidances/ucm073389.pdf.
Guidance for Industry: Q3C Impurities: Residual Solvents, December 1997. Available at http://www.ich.org/products/guidelines/quality/quality-single/article/impurities-guideline-for-residual-solvents.html.
CFR: Code of Federal Regulations Title 21, 21 August 2015. Available at http://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfcfr/cfrsearch.cfm?fr=610.12.
United States Pharmacopoeia (USP), Chapter <71> Sterility Tests, 23rd edn, 1995. Available at http://www.usp.org.
Guidance for Industry: Q1A (R2): Stability Testing of New Drug Substances and Products (Revision 2), November 2003. Available at http://www.fda.gov/downloads/drugs/guidancecomplianceregulatoryinformation/guidances/ucm073369.pdf.
ICH Harmonized Tripartite Guidance Q1E: Evaluation of Stability Data, June, 2004. Available at http://www.ich.org/products/guidelines/quality/quality-single/article/evaluation-of-stability-data.html.
Guidance for Industry: Potency Tests for Cellular and Gene Therapy Products, January 2011. Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/default.htm.
Draft Guidance for Industry: Comparability Protocol – Protein Drug Products and Biological Products—Chemistry, Manufacturing, and Controls Information, September 2003. Available at http://www.fda.gov/cber/guidelines.htm.
Simek SL . Characterization of gene therapy products and the impact of manufacturing changes on product comparability. Dev Biol (Basel) 2005; 122: 139–144.
International Conference on Harmonization: Guidance for Industry: Q5E Comparability of Biotechnological/Biological Products Subject to Changes in Their Manufacturing Process, June 2005. Available at http://www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/ucm073476.pdf.
Guidance for Industry: Preclinical Assessment of Investigational Cellular and Gene Therapy Products, November 2013. Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/default.htm.
Guidance for Industry: Determining the Need for and Content of Environmental Assessments for Gene Therapies, Vectored Vaccines, and Related Recombinant Viral or Microbial Products, March 2015. Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/CellularandGeneTherapy/ucm401869.htm.
Shenk-Braat EA, van Mierlo MM, Wagemaker G, Bangma CH, Kaptein LC . An inventory of shedding data from clinical gene therapy trials. J Gene Med 2007; 9: 910–921.
Brandon EF, Hermsen HP, van Eijkeren JC, Tiesjema B . Effect of administration route on the biodistribution and shedding of replication-deficient AAV2: a qualitative modeling approach. Curr Gene Ther 2010; 10: 91–106.
Guidance for Industry: Design and Analysis of Shedding Studies for Virus or Bacteria-Based Gene Therapy and Oncolytic Products, August 2015. Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/default.htm.
Guidance for Industry: Gene Therapy Clinical Trials—Observing Subjects for Delayed Adverse Events, November 2006, Available at http://www.fda.gov/biologicsbloodvaccines/guidancecomplianceregulatoryinformation/guidances/cellularandgenetherapy/ucm072957.htm.
Guidance for Industry: Preclinical Assessment of Investigational Cellular and Gene Therapy Products, November 2013. Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/CellularandGeneTherapy/ucm388218.htm.
Guidance for Industry: Clinical Considerations for Therapeutic Cancer Vaccines, October 2011. Available at http://www.fda.gov/downloads/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/Vaccines/UCM278673.pdf.
Hacein-Bey-Abina S, von Kalle K, Schmidt M, Le Deist F, Wulffraat N, McIntyre E et al. A serious adverse event after successful gene therapy for X-linked severe combined immunodeficiency. N Engl J Med 2003; 348: 255–256.
Guidance for Industry: Supplemental Guidance on Testing for Replication Competent Retrovirus in Retroviral Vector Based Gene Therapy products and During Follow-up of Patients in Clinical Trials Using Retroviral Vectors, November 2006. Available at http://www.fda.gov/cber/guidelines.htm.
Miller DL, Ross JJ . Vaccine INDs: review of clinical holds. Vaccine 2005; 23: 1099–1101.
Takefman D, Bryan W . The state of gene therapies: the FDA perspective. Mol Therapy 2012; 20: 877–878.
CBER SOPP 8101.1, Scheduling and Conduct of Regulatory review Meetings with Sponsors and Applications, 15 October 2012. Available at http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/ProceduresSOPPs/ucm079448.htm.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Husain, S., Han, J., Au, P. et al. Gene therapy for cancer: regulatory considerations for approval. Cancer Gene Ther 22, 554–563 (2015). https://doi.org/10.1038/cgt.2015.58
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cgt.2015.58
This article is cited by
-
Semi-Implantable Bioelectronics
Nano-Micro Letters (2022)
-
Diethyldithiocarbamate-copper complex (CuET) inhibits colorectal cancer progression via miR-16-5p and 15b-5p/ALDH1A3/PKM2 axis-mediated aerobic glycolysis pathway
Oncogenesis (2021)
-
Interference chromatography: a novel approach to optimizing chromatographic selectivity and separation performance for virus purification
BMC Biotechnology (2020)
-
Decreased FBP1 expression rewires metabolic processes affecting aggressiveness of glioblastoma
Oncogene (2020)
-
Recent trends and advances in microbe-based drug delivery systems
DARU Journal of Pharmaceutical Sciences (2019)