Abstract
Background:
The objectives of this phase I study were to assess the safety and tolerability of E7080 in patients with advanced, refractory solid tumours; to determine the maximum tolerated dose (MTD) and pharmacokinetics profile of E7080; and to explore preliminary evidence of its anti-tumour efficacy.
Methods:
E7080 was administered orally in escalating doses on a once-daily continuous schedule in 28-day cycles to eligible patients. Samples for pharmacokinetic analyses were collected on days 1, 8, 15 and 22 of cycle 1 and day 1 of cycle 2. Anti-tumour efficacy was assessed every two cycles.
Results:
Eighty-two patients received E7080 in dose cohorts from 0.2 to 32 mg. Dose-limiting toxicities were grade 3 proteinuria (two patients) at 32 mg, and the MTD was defined as 25 mg. The most frequently observed cumulative toxicities (all grades) were hypertension (40% of patients), diarrhoea (45%), nausea (37%), stomatitis (32%) and vomiting (23%). Seven patients (9%) had a partial response and 38 patients (46%) had stable disease as best response. E7080 has dose-linear kinetics with no drug accumulation after 4 weeks’ administration.
Conclusion:
E7080 is well tolerated at doses up to 25 mg per day. Encouraging anti-tumour efficacy was observed in patients with melanoma and renal cell carcinoma.
Similar content being viewed by others
Main
Aberrant angiogenesis is important in many disease states including cancer (Dvorak, 2005), and is critical for tumour cell survival, local invasion and metastasis (Verheul et al, 2004). Numerous extracellular cell surface and intracellular molecules that can modulate angiogenesis have been identified (Senger et al, 1990; Roy et al, 2006), including growth factors, adhesion molecules, proteinases, extracellular matrix proteins, transcription factors and signalling molecules (Ivy et al, 2009). Vascular endothelial growth factor (VEGF), fibroblast growth factor (FGF) and platelet-derived growth factor (PDGF) have been implicated among the many angiogenic stimulators that promote tumour angiogenesis. Vascular endothelial growth factor has been identified as a crucial regulator of physiological and pathological angiogenesis, primarily via activation of VEGF receptor-2 (VEGFR2; kinase insert domain receptor (KDR); Ferrara et al, 2003).
The concept of targeting angiogenesis for anti-tumour therapy was initially proposed in the 1970s (Folkman, 1972). A number of angiogenesis inhibitors have been approved for use in clinical oncology practice, including bevacizumab (colorectal, breast, non-small-cell lung and renal cell cancers), a monoclonal antibody directed against VEGF-A (Hurwitz et al, 2004; Reck et al, 2009), and sorafenib (renal cancer and hepatocellular carcinoma) and sunitinib (renal cell cancer, and gastrointestinal stromal and pancreatic neuroendocrine tumours), which are orally available multi-kinase inhibitors with activity against VEGF and PDGF receptors (Escudier et al, 2007; Motzer et al, 2007). E7080 is an orally active inhibitor of multiple receptor tyrosine kinases (RTKs), including KDR (VEGFR-2), Flt-1 (VEGFR-1), FGFR1, PDGFR-β and c-kit (Matsui et al, 2008b). E7080 potently inhibits VEGF-driven KDR phosphorylation in human umbilical vein endothelial cells (HUVECs) and inhibits VEGF-driven HUVEC proliferation and tube formation (Matsui et al, 2008b). It has potent anti-tumour activity against a number of human cancer cell lines in mouse xenograft models, mediated via inhibition of angiogenesis (Matsui et al, 2008a, 2008b). The strong potency against FGF-R1 differentiates E7080 from other currently approved tyrosine kinase inhibitors with antiangiogenesis properties (Karaman et al, 2008; Matsui et al, 2008b)
The objectives of this phase I study were to assess the safety and tolerability of E7080 in patients with advanced, refractory solid tumours; to determine the maximum tolerated dose (MTD) and pharmacokinetic (PK) profile of E7080; and to explore preliminary evidence of its anti-tumour efficacy.
Patients and methods
Patients and eligibility criteria
This was a non-randomised, open-label, phase I, dose-escalation study conducted in accordance with the International Conference on Harmonisation Good Clinical Practice with the ethical principles of the current Declaration of Helsinki and approved by the Research Ethics Committee at each of the two participating institutions (clinicaltrials.gov identifier NCT00121719). All patients provided written informed consent before any study-related procedures were performed.
All patients who entered the study had a histologically or cytologically confirmed solid tumour, refractory to conventional therapies or for which there was no available effective therapy. Eligibility criteria included adequate performance status, haematological, renal and hepatic function (Supplementary Data, Appendix 1).
Primary and secondary outcome measures
The primary outcome measure for this clinical study was to determine the MTD for E7080 based on the observed dose-limiting toxicities (DLTs). Secondary outcome measures included the safety of E7080, its PK profile and efficacy measurements. A preliminary assessment of the effect of food on the PK profile was also performed after the MTD was determined.
Treatment administration
E7080 was administered orally on an empty stomach (after an overnight fast) on a continuous once-daily administration schedule, with one cycle of treatment consisting of 28 days. Only clear fluids were allowed within 2 h of drug administration. Treatment continued until progressive disease or unacceptable toxicity, despite dose modification.
The starting dose (0.2 mg per day) was based upon the Toxic Dose Low that caused only reversible testicular changes in 4-week toxicology studies in dogs. Dose escalation was performed with an accelerated design (Supplementary Data, Appendix 2) and continued until the MTD was determined.
Once the MTD had been established, a food-effect investigation was initiated. Patients were randomly assigned to receive the cycle 1, day 15 dose of E7080 in a fed (following a high-fat meal) or fasted (overnight fast of ⩾10 h) state, with each patient then receiving the cycle 1, day 22 dose in the reverse state. In both cases, no food was allowed for 4 h following administration of E7080.
Evaluation of toxicity
Toxicity was graded using the National Cancer Institute (Washington, DC, USA) Common Toxicity Criteria, version 3.0. Physical examination, measurement of blood pressure, full blood count, biochemical profile and urinalysis were performed weekly during cycle 1, during which DLT was defined. Electrocardiograms were performed on days 1 and 8 of cycle 1. A DLT was defined as any of the following drug-related toxicities: grade ⩾3 haematological or non-haematological toxicity; repeated grade 2 haematological or non-haematological toxicity requiring dose reduction; and failure to administer ⩾75% of the planned dosage of E7080 during cycle 1 as a result of treatment-related toxicity.
If one out of three patients experienced a DLT, up to three patients were treated at that dose level. The MTD was defined as the highest dose level at which one or fewer of six patients experienced a DLT. An additional cohort of 12 patients was treated at the MTD.
Criteria for dose interruptions and dose modifications, and the methods for disease evaluation and objective response assessments using Response Evaluation Criteria in Solid Tumours (Therasse et al, 2000), are included in the Supplementary Data.
Pharmacokinetic studies
Blood and urine samples for PK analyses were collected as described in the Supplementary Data, Appendix 3. E7080 concentrations were measured using a liquid chromatography-tandem mass spectrometry method. Pharmacokinetic parameters for plasma and urine included time to maximal plasma concentration (tmax), maximal plasma concentration (Cmax), area under the plasma concentration-time curve from zero to 24 h (AUC0-24), AUC from zero to infinity (AUC0-∞), AUC over the dosing interval (AUC0-τ), plasma half-life (t½), apparent clearance (CL/F) and volume of distribution (V/F) were calculated using WinNonlin (Pharsight Corporation, Mountain View, CA, USA), version 6.0. In the food-effect investigation, the 90% confidence intervals (CIs) for the log-transformed Cmax and AUC0-24 (fed/fasted) were calculated using analysis of variance. If a range within 80–125% was found, then the concomitant intake of food was considered not to modify the bioavailability of E7080.
Results
Patient characteristics
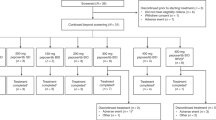
Eighty-two patients were enroled between July 2005 and July 2008 at The Netherlands Cancer Institute, Amsterdam, The Netherlands, and at the Beatson West of Scotland Cancer Centre, Glasgow, UK. Median age was 54 years (range 25–84 years). There were roughly equal numbers of men and women in the study. Almost half (46%) of patients had a Karnofsky performance status of >90. Most patients had undergone prior surgery and chemotherapy (Table 1). Specifically, most patients had received more than one prior systemic therapy regimen, including 25 patients (30%) who had received two regimens, 15 (18%) with three regimens and 10 (12%) with four or more regimens.
Patients received E7080 in dose cohorts: 0.2, 0.4, 0.8, 1.6, 3.2, 6.4, 12.5, 16, 20, 25 and 32 mg, with subsequent expansion of the MTD dose cohort (25 mg), which included 11 patients in the food-effect evaluation. A number of patients required dose reductions due to cumulative toxicity after the DLT assessment period at higher starting doses (>16 mg), which were below the MTD (Supplementary Data, Table 1) but higher than the lowest dose at which anti-tumour activity had been observed. Consequently, an additional cohort of patients was enroled at a dose of 12 mg to allow for further investigation of the tolerability and anti-tumour effect of E7080.
Toxicity
Dose-limiting toxicity
Dose-limiting toxicities occurred in five patients: at doses of 6.4 mg (n=1, grade 3 febrile neutropenia), 12.5 mg (n=1, grade 4 thrombocytopenia), 16 mg (n=1, grade 3 hypertension and grade 3 fatigue in the same patient) and 32 mg (n=2, both grade 3 proteinuria). A second patient developed a possible DLT of grade 3 proteinuria at 12.5 mg. The majority of patients treated at the 12.5-mg dose level experienced little toxicity, and given the uncertainty over the true degree of proteinuria in this patient (grade 1 proteinuria at screening and possible inaccuracy of the collection method), an additional three patients were included at this dose level with no further DLTs. Subsequently, dose-escalation proceeded as planned, with the conclusion that a starting dose of 32 mg was not tolerable and the MTD should be 25 mg. No patient had a DLT on the basis of receiving <75% of the planned cycle 1 dose.
Treatment-related cumulative toxicity
The most frequent drug-related toxicities (all grades) were hypertension (n=33, 40%), proteinuria (n=21, 26%) and gastrointestinal toxicities including nausea (n=30, 37%), diarrhoea (n=28, 45%), stomatitis (n=26, 32%) and vomiting (n=19, 23%) (Table 2). Most of these toxicities were grade ⩽2 (data not shown). Grade 3 hypertension occurred in nine patients (11%) and grade 3 proteinuria in six patients (7%), with a trend towards an increase in hypertension and proteinuria with increasing doses of E7080 (Table 3). In the expanded MTD cohort of 25 mg (n=24), grade 3 hypertension occurred in three (13%) patients and grade 3 proteinuria in two (8%) patients.
Haematological toxicities occurred in six patients (7%). There was one report of grade 3 thrombocytopenia (in a patient receiving 25 mg) and two reports of grade 4 thrombocytopenia (in patients receiving 12.5 and 25 mg doses). There was one report of grade 3 neutropenia (in a patient receiving 25 mg) and one patient with a starting dose of 6.4 mg reported grade 3 febrile neutropenia.
Dose modifications
Dose modifications were required in 40 patients (49%); at the MTD of 25 mg, dose modifications were required in 13 patients (54%). Most dose modifications occurred in patients treated with doses of E7080 ⩾12 mg per day, and the majority were required early in the course of their treatments (Supplementary Data, Table 1). The most common reasons for dose modifications were proteinuria (n=14, 17%) and hypertension (n=9, 11%). Stomatitis led to a dose reduction in two patients.
Anti-tumour activity
Confirmed partial responses (PRs) were observed in patients diagnosed with renal cell carcinoma, melanoma and soft tissue sarcoma (Table 4). Thirty-eight patients (46%) had stable disease (SD) as best response. Clinical benefit (defined as PR rate plus SD rate) occurred in 45 patients (55%). As of 1 June 2011, two patients remain on treatment. Objective responses and/or prolonged disease stabilisation were observed in particular in patients with renal cancer and malignant melanoma. Four of nine patients with renal cancer treated with E7080 had PRs. A waterfall plot showing the extent of tumour reduction in all patients with renal cancer shows decreases ranging from 5 to 55% (Figure 1A). The range for all patients with melanoma was larger, with one patient showing a decrease of approximately 85% in the sum of the longest tumour diameters (Figure 1B).
Waterfall plots displaying tumour responses to E7080, with individual doses received (mg per day), in patients with (A) renal cancer and (B) melanoma, and Kaplan–Meier plots representing progression-free survival for patients with (C) renal cancer and (D) melanoma. Measurements were recorded as per the Response Evaluation Criteria in Solid Tumours. Abbreviation: CI=confidence interval.
Patients with renal cancer (all dose cohorts; n=9) had a median progression-free survival (PFS) of 477 days (95% CI 279.0–559.0 days) and one patient remains on treatment after 59 weeks (Figure 1C). Patients (n=14) with melanoma had a median PFS of 217 days (95% CI 109.0–379.0 days) (Figure 1D). All but one patient with renal cancer treated with E7080 had received at least one prior therapy (Supplementary Data, Table 2, data not documented for one patient), although six of these had not received prior antiangiogenesis therapy. Examples of computed tomography responses in a patient with renal cancer and a patient with melanoma are shown in Figure 2.
CT scans showing tumour responses to E7080. (A) CT scans of thorax (upper panels) and abdomen (lower panels) from a patient with renal cancer at baseline (left panels) and after 24 weeks’ treatment with E7080 (right panels). Overall reduction in tumour size was 51%. (B) CT scans of thorax from a patient with melanoma at baseline (left) and after 32 weeks’ treatment with E7080 (right). Overall reduction in tumour size was 77%. Abbreviation: CT=computed tomography.
Pharmacokinetics
Blood samples for PK analyses were obtained from 81 patients after a single dose of E7080 (Supplementary Data, Table 3). E7080 was absorbed rapidly with maximum concentrations achieved within 3 h. Both exposure to E7080 and observed Cmax concentrations increased linearly with increasing dose (Supplementary Data, Figures 1 and 2), and the median t½ of E7080 varied between 5.3 and 8.3 h at the higher dose levels (⩾6.4 mg). The terminal elimination phase could not be estimated properly for several patients treated at the lower dose levels (up to 0.4 mg) due to insufficient data points in the terminal phase. Consequently, no t1/2, CL/F or V/F could be reported for these patients. At the higher doses, median clearance of E7080 ranged between 4.3 and 10.4 l h−1, while the drug had a moderate median V/F ranging between 50.5 and 92.0l. Comparable results were obtained following multiple doses of E7080 (Supplementary Data, Table 4). No accumulation was observed after multiple dosing (the Cmax values observed at steady state were equal to those observed after a single dose). Eleven patients were included in the food-effect study. No effect of food on exposure or maximum achieved plasma concentrations were observed (AUC ratio fed/fasted of 1.00 (90% CI 0.83–1.20); Cmax ratio fed/fasted of 0.98 (90% CI 0.73–1.31)). However, there was a significant effect on tmax, shifting from 2 h in the fasted group to 5 h in the fed group (median values 2.0 vs 5.0 h, respectively; P=0.015).
Discussion
E7080 is well tolerated when administered by a single, oral, daily continuous dosing schedule. The DLTs were grade 3 proteinuria, observed in two patients at 32 mg, as well as febrile neutropenia, proteinuria, thrombocytopenia and hypertension/fatigue observed in one patient each at 6.4, 12.5, 12.5 and 16 mg, respectively. The MTD was defined as 25 mg once daily, a total daily dose that is comparable to the maximum daily dose determined in another recently published clinical study of E7080 (Yamada et al, 2011), in which E7080 was administered twice daily (b.i.d.) in a 2-week-on/1-week-off schedule (MTD of 13 mg b.i.d.).
Treatment-related hypertension (all grades, all cycles) was reported in 40% of patients in this study, in keeping with the incidence of hypertension reported in the other phase I study with E7080, as well as in studies of other agents that target the VEGF-signalling pathway (Roodhart et al, 2008; Launay-Vacher and Deray, 2009; Yamada et al, 2011). The incidence of treatment-related proteinuria observed in this study (all grades, all cycles; 26% of patients) was much higher than with sorafenib or sunitinib (Faivre et al, 2006; Strumberg et al, 2006), but comparable to bevacizumab (Kamba and McDonald, 2007) and lower than that observed for b.i.d. dosing with E7080 (Yamada et al, 2011). Hypertension was manageable in this study with the introduction of antihypertensive agents at first occurrence of diastolic blood pressure ⩾100 mm Hg, although dose reductions for proteinuria were required in 17% of patients and for hypertension in 11% of patients. Significant proteinuria was managed by dose interruption and/or modification with no indication for renal support. Recently, a management model for hypertension and proteinuria following treatment with E7080 has been developed using PK, blood pressure and urinalysis data from the study described here (Keizer et al, 2010), and which can be applied to future studies. A clear relation between exposure and response was established, both for hypertension and for the probability of experiencing proteinuria (Keizer et al, 2010).
Gastrointestinal toxicities were observed frequently but were generally mild (grade ⩽2). Stomatitis was mainly observed at the higher dose levels, but led to a dose reduction in only two patients (2%). Stomatitis is commonly observed with other angiogenesis inhibitors, although the underlying mechanism remains unclear (Eskens and Verweij, 2006). Interestingly, stomatitis was not reported with b.i.d. dosing (Yamada et al, 2011). In our study, haematological toxicities were uncommon, occurring in 7% of patients (all grades). There was one occurrence of grade 3 neutropenia, one of grade 3 febrile neutropenia, and one of grade 3 and two of grade 4 thrombocytopenia.
Clinical benefit (PR or SD) was observed in 55% of patients treated with E7080, which compares favourably with other phase I studies (Horstmann et al, 2005). E7080 has antiangiogenic properties, so efficacy in patients with renal cell carcinoma could have been anticipated. Six of these nine patients had not previously received an angiogenesis inhibitor due to reimbursement issues at the study centres. Nevertheless, two patients who had previously been treated with angiogenesis inhibitors for renal cell carcinoma had evidence of clinical benefit (one with disease stabilisation lasting 10 cycles; one with a PR lasting 18 cycles).
The preliminary evidence for the efficacy of E7080 in patients with melanoma is of interest. Angiogenesis is required for melanoma progression and metastasis (Basu et al, 2009). Expression of VEGF and VEGFR1–3 is significantly higher in melanoma than in nevi, and VEGFR2 expression is higher in metastases than in primary melanomas (Mehnert et al, 2010). Basic FGF and its respective RTKs form an autocrine loop that affects human melanoma growth and metastasis, and basic FGF induces a transformed phenotype in normal human melanocytes (Nesbit et al, 1999). Expression of a dominant-negative FGF receptor (FGFR) inhibits proliferation and survival of melanoma cells in vitro (Ozen et al, 2004). Autocrine cell proliferation and tumourigenesis of human melanoma cells are also suppressed in vitro by a kinase-deficient FGFR1 (Yayon et al, 1997). Thus E7080, by targeting both FGFR1 and VEGFR2, may have efficacy in patients with metastatic melanoma. The preliminary evidence of efficacy in patients with melanoma is unexpected given the recent failure of sorafenib in this patient population (Ott et al, 2010). The observed efficacy of E7080 might be caused by more potent target inhibition or by its effects on additional targets (e.g., FGFR1) compared with sorafenib and sunitinib. Targeting of c-kit might also have contributed to this effect, as c-kit mutations and/or overexpression can be found in certain melanoma subtypes (Curtin et al, 2006). It was shown that imatinib, an inhibitor of c-kit, is active in patients with metastatic melanoma harbouring c-kit aberrations (Guo et al, 2011). Recently, this was also shown for sunitinib (Minor et al, 2012). E7080 can reduce the number of c-kit-positive circulating endothelial progenitor cells and circulating endothelial cells, but not c-kit-negative cells (Yamada et al, 2011). This suggests an effect of E7080 on c-kit expressing cells in vivo. However, mutation analyses (c-kit, B-Raf, N-ras) were not performed on tumour samples from patients with melanoma in our study, as these analyses were not routinely performed in patients with melanoma at the time of recruitment.
The MTD was 25 mg, but maintaining this dose for long-term administration may be challenging as dose reductions were required in 54% of patients who started treatment at this dose. However, clinical benefit was observed more frequently in patients in the higher dose cohorts. Patients with higher diastolic blood pressure levels (⩾90 mm Hg) during treatment with the angiogenesis inhibitor axitinib have responded better than patients with levels below 90 mm Hg (Rixe et al, 2009). Consequently, we propose a starting dose of 25 mg of E7080, and patients who develop hypertension should receive antihypertensive drugs and remain on the same dose of E7080, if possible. Pharmacokinetics analyses showed that the co-administration of food had no effect on the plasma peak levels for E7080, and that plasma concentrations exceeded the levels that appeared effective in vitro (Yamada et al, 2011).
In conclusion, this study demonstrates that E7080 is well tolerated when administered to patients with advanced solid tumours at doses up to 25 mg per day. Encouraging anti-tumour activity was observed in patients with melanoma and renal cell carcinoma. These results form the basis of phase II studies in several cancer types, including melanoma, most of which use a dosing regimen of 24 mg once daily. Preliminary results from one study in patients with advanced radioiodine-refractory differentiated thyroid cancer have demonstrated an objective response rate of 59% (Sherman et al, 2011) and a phase III study is ongoing (NCT01321554).
Change history
23 January 2013
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Basu B, Biswas S, Wrigley J, Sirohi B, Corrie P (2009) Angiogenesis in cutaneous malignant melanoma and potential therapeutic strategies. Expert Rev Anticancer Ther 9: 1583–1598
Curtin JA, Busam K, Pinkel D, Bastian BC (2006) Somatic activation of KIT in distinct subtypes of melanoma. J Clin Oncol 24: 4340–4346
Dvorak HF (2005) Angiogenesis: update 2005. J Thromb Haemost 3: 1835–1842
Escudier B, Eisen T, Stadler WM, Szczylik C, Oudard S, Siebels M, Negrier S, Chevreau C, Solska E, Desai AA, Rolland F, Demkow T, Hutson TE, Gore M, Freeman S, Schwartz B, Shan M, Simantov R, Bukowski RM (2007) Sorafenib in advanced clear-cell renal-cell carcinoma. N Engl J Med 356: 125–134
Eskens FA, Verweij J (2006) The clinical toxicity profile of vascular endothelial growth factor (VEGF) and vascular endothelial growth factor receptor (VEGFR) targeting angiogenesis inhibitors; a review. Eur J Cancer 42: 3127–3139
Faivre S, Delbaldo C, Vera K, Robert C, Lozahic S, Lassau N, Bello C, Deprimo S, Brega N, Massimini G, Armand JP, Scigalla P, Raymond E (2006) Safety, pharmacokinetic, and antitumor activity of SU11248, a novel oral multitarget tyrosine kinase inhibitor, in patients with cancer. J Clin Oncol 24: 25–35
Ferrara N, Gerber HP, LeCouter J (2003) The biology of VEGF and its receptors. Nat Med 9: 669–676
Folkman J (1972) Anti-angiogenesis: new concept for therapy of solid tumors. Ann Surg 175: 409–416
Glen H, Boss D, Evans TRJ, Roelvink M, Saro JM, Bezodis P, Copalu W, Das A, Crosswell G, Schellens JH (2007) A phase I dose finding study of E7080 in patients (pts) with advanced malignancies. J Clin Oncol 25(18S): 617s (abstract 14073)
Glen H, Boss DR, Morrison R, Roelvink M, Wanders A, Mazur A, Gupta A, Das A, Evans TRJ, Schellens JH (2008) A phase I study of E7080 in patients (pts) with advanced malignancies. J Clin Oncol 26(15S): 159s (abstract 3526)
Guo J, Si L, Kong Y, Flaherty KT, Xu X, Zhu Y, Corless CL, Li L, Li H, Sheng X, Cui C, Chi Z, Li S, Han M, Mao L, Lin X, Du N, Zhang X, Li J, Wang B, Qin S (2011) Phase II, open-label, single-arm trial of imatinib mesylate in patients with metastatic melanoma harboring c-Kit mutation or amplification. J Clin Oncol 29: 2904–2909
Horstmann E, McCabe MS, Grochow L, Yamamoto S, Rubinstein L, Budd T, Shoemaker D, Emanuel EJ, Grady C (2005) Risks and benefits of phase 1 oncology trials, 1991 through 2002. N Engl J Med 352: 895–904
Hurwitz H, Fehrenbacher L, Novotny W, Cartwright T, Hainsworth J, Heim W, Berlin J, Baron A, Griffing S, Holmgren E, Ferrara N, Fyfe G, Rogers B, Ross R, Kabbinavar F (2004) Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350: 2335–2342
Ivy SP, Wick JY, Kaufman BM (2009) An overview of small-molecule inhibitors of VEGFR signaling. Nat Rev Clin Oncol 6: 569–579
Kamba T, McDonald DM (2007) Mechanisms of adverse effects of anti-VEGF therapy for cancer. Br J Cancer 96: 1788–1795
Karaman MW, Herrgard S, Treiber DK, Gallant P, Atteridge CE, Campbell BT, Chan KW, Ciceri P, Davis MI, Edeen PT, Faraoni R, Floyd M, Hunt JP, Lockhart DJ, Milanov ZV, Morrison MJ, Pallares G, Patel HK, Pritchard S, Wodicka LM, Zarrinkar PP (2008) A quantitative analysis of kinase inhibitor selectivity. Nat Biotechnol 26: 127–132
Keizer RJ, Gupta A, Mac Gillavry MR, Jansen M, Wanders J, Beijnen JH, Schellens JH, Karlsson MO, Huitema AD (2010) A model of hypertension and proteinuria in cancer patients treated with the anti-angiogenic drug E7080. J Pharmacokinet Pharmacodyn 37: 347–363
Launay-Vacher V, Deray G (2009) Hypertension and proteinuria: a class-effect of antiangiogenic therapies. Anticancer Drugs 20: 81–82
Matsui J, Funahashi Y, Uenaka T, Watanabe T, Tsuruoka A, Asada M (2008a) Multi-kinase inhibitor E7080 suppresses lymph node and lung metastases of human mammary breast tumor MDA-MB-231 via inhibition of vascular endothelial growth factor-receptor (VEGF-R) 2 and VEGF-R3 kinase. Clin Cancer Res 14: 5459–5465
Matsui J, Yamamoto Y, Funahashi Y, Tsuruoka A, Watanabe T, Wakabayashi T, Uenaka T, Asada M (2008b) E7080, a novel inhibitor that targets multiple kinases, has potent antitumor activities against stem cell factor producing human small cell lung cancer H146, based on angiogenesis inhibition. Int J Cancer 122: 664–671
Mehnert JM, McCarthy MM, Jilaveanu L, Flaherty KT, Aziz S, Camp RL, Rimm DL, Kluger HM (2010) Quantitative expression of VEGF, VEGF-R1, VEGF-R2, and VEGF-R3 in melanoma tissue microarrays. Hum Pathol 41: 375–384
Minor DR, Kashani-Sabet M, Garrido M, O'Day SJ, Hamid O, Bastian BC (2012) Sunitinib therapy for melanoma patients with KIT mutations. Clin Cancer Res 18: 1457–1463
Motzer RJ, Hutson TE, Tomczak P, Michaelson MD, Bukowski RM, Rixe O, Oudard S, Negrier S, Szczylik C, Kim ST, Chen I, Bycott PW, Baum CM, Figlin RA (2007) Sunitinib versus interferon alfa in metastatic renal-cell carcinoma. N Engl J Med 356: 115–124
Nesbit M, Nesbit HK, Bennett J, Andl T, Hsu MY, Dejesus E, McBrian M, Gupta AR, Eck SL, Herlyn M (1999) Basic fibroblast growth factor induces a transformed phenotype in normal human melanocytes. Oncogene 18: 6469–6476
Ott PA, Hamilton A, Min C, Safarzadeh-Amiri S, Goldberg L, Yoon J, Yee H, Buckley M, Christos PJ, Wright JJ, Polsky D, Osman I, Liebes L, Pavlick AC (2010) A phase II trial of sorafenib in metastatic melanoma with tissue correlates. PLoS One 5: e15588
Ozen M, Medrano EE, Ittmann M (2004) Inhibition of proliferation and survival of melanoma cells by adenoviral-mediated expression of dominant negative fibroblast growth factor receptor. Melanoma Res 14: 13–21
Reck M, von Pawel J, Zatloukal P, Ramlau R, Gorbounova V, Hirsh V, Leighl N, Mezger J, Archer V, Moore N, Manegold C (2009) Phase III trial of cisplatin plus gemcitabine with either placebo or bevacizumab as first-line therapy for nonsquamous non-small-cell lung cancer: AVAil. J Clin Oncol 27: 1227–1234
Rixe O, Dutcher K, Motzer RJ, Wilding G, Stadler WM, Garrett M, Pithavala Y, Kim S, Tarazi J, Rini BI (2009) Diastolic blood pressure (DBP) and pharmacokinetics (PK) as predictors of axitinib efficacy in metastatic renal cell cancer (mRCC). J Clin Oncol 2715(Suppl): Abstract 5045
Roodhart JM, Langenberg MH, Witteveen E, Voest EE (2008) The molecular basis of class side effects due to treatment with inhibitors of the VEGF/VEGFR pathway. Curr Clin Pharmacol 3: 132–143
Roy H, Bhardwaj S, Yla-Herttuala S (2006) Biology of vascular endothelial growth factors. FEBS Lett 580: 2879–2887
Senger DR, Connolly DT, Van de Water L, Feder J, Dvorak HF (1990) Purification and NH2-terminal amino acid sequence of guinea pig tumor-secreted vascular permeability factor. Cancer Res 50: 1774–1778
Sherman SI, Jarzab B, Cabanillas ME, Licitra LF, Pacini F, Martins R, Robinson B, Ball D, McCaffrey J, Shah MH, Bodenner D, Allison R, Newbold K, Elisei R, O'Brien JP, Schlumberger M (2011) A phase II trial of the multitargeted kinase inhibitor E7080 in advanced radioiodine (RAI)-refractory differentiated thyroid cancer (DTC). J Clin Oncol 2915(Suppl): Abstract 5503
Strumberg D, Awada A, Hirte H, Clark JW, Seeber S, Piccart P, Hofstra E, Voliotis D, Christensen O, Brueckner A, Schwartz B (2006) Pooled safety analysis of BAY 43-9006 (sorafenib) monotherapy in patients with advanced solid tumours: Is rash associated with treatment outcome? Eur J Cancer 42: 548–556
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van GM, van Oosterom AT, Christian MC, Gwyther SG (2000) New guidelines to evaluate the response to treatment in solid tumors. European Organization for Research and Treatment of Cancer, National Cancer Institute of the United States, National Cancer Institute of Canada. J Natl Cancer Inst 92: 205–216
Verheul HM, Voest EE, Schlingemann RO (2004) Are tumours angiogenesis-dependent? J Pathol 202: 5–13
Yamada K, Yamamoto N, Yamada Y, Nokihara H, Fujiwara Y, Hirata T, Koizumi F, Nishio K, Koyama N, Tamura T (2011) Phase I dose-escalation study and biomarker analysis of E7080 in patients with advanced solid tumors. Clin Cancer Res 17: 2528–2537
Yayon A, Ma YS, Safran M, Klagsbrun M, Halaban R (1997) Suppression of autocrine cell proliferation and tumorigenesis of human melanoma cells and fibroblast growth factor transformed fibroblasts by a kinase-deficient FGF receptor 1: evidence for the involvement of Src-family kinases. Oncogene 14: 2999–3009
Acknowledgements
Editorial assistance was provided by Cath Bryant at Complete Medical Communications and was funded by Eisai Inc. We are grateful to the patients who participated in this study, their carers, and to the research teams at both participating study centres. This study was supported by Eisai Europe Limited. The Glasgow Experimental Cancer Medicine Centre at the Beatson West of Scotland Cancer Centre is supported by Cancer Research UK and by the Chief Scientist Office, Scotland.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
TRJE and HG received research funding from Eisai Inc. JB is a full-time employee of Eisai Inc. At the time of the study, JW, AM and WC were employees of Eisai Ltd. The other authors declare no conflict of interest.
Additional information
Preliminary results of this study were published in the ASCO Annual Meeting Proceedings 2007 (Glen et al, 2007). Updated results of this study were presented at the ASCO Annual Meeting 2008 (Glen et al, 2008).
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Supplementary Information accompanies the paper on British Journal of Cancer website
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Boss, D., Glen, H., Beijnen, J. et al. A phase I study of E7080, a multitargeted tyrosine kinase inhibitor, in patients with advanced solid tumours. Br J Cancer 106, 1598–1604 (2012). https://doi.org/10.1038/bjc.2012.154
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2012.154
Keywords
This article is cited by
-
A feasibility study of lenvatinib plus pembrolizumab in Japanese patients with advanced solid tumors
Cancer Chemotherapy and Pharmacology (2022)
-
Lenvatinib inhibits the growth of gastric cancer patient-derived xenografts generated from a heterogeneous population
Journal of Translational Medicine (2022)
-
Exploratory analysis of target concentration of lenvatinib in the treatment of hepatocellular carcinoma
Cancer Chemotherapy and Pharmacology (2021)
-
REFLECT—a phase 3 trial comparing efficacy and safety of lenvatinib to sorafenib for the treatment of unresectable hepatocellular carcinoma: an analysis of Japanese subset
Journal of Gastroenterology (2020)
-
Influences of ABC transporter and CYP3A4/5 genetic polymorphisms on the pharmacokinetics of lenvatinib in Chinese healthy subjects
European Journal of Clinical Pharmacology (2020)