Abstract
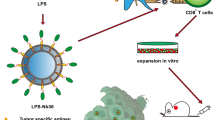
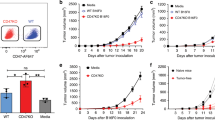
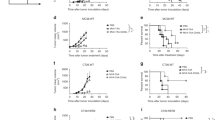
The present study uses an in vivo murine tumor model expressing the human HER-2/neu antigen to evaluate the potential vaccine using dendritic cells (DCs) infected with adenovirus AdVHER-2. We first investigated whether infected DCs (DCHER-2) engineered to express HER-2/neu could induce HER-2/neu-specific immune responses. Our data showed that (i) AdVHER2-infected DCHER-2 expressed HER-2/neu by Western blot and flow cytometric analysis, and (ii) vaccination of mice with DCHER-2 induced HER-2/neu-specific cytotoxic T-lymphocyte (CTL) responses, but protected only 25% of vaccinated mice from challenge of 3×105 MCA26/HER-2 tumor cells. Further, to enhance the efficacy of DCHER-2 vaccine, we coinfected DCs with both AdVHER-2 and AdVTNF-α. The infected DCs (DCHER-2/TNF-α) displayed the expression of both HER-2/neu and TNF-α by flow cytometric and ELISA analysis. We next investigated whether DCHER-2/TNF-α could induce stronger HER-2/neu-specific immune responses. We found that DCHER-2/TNF-α displayed up-regulation of immunologically important CD40, CD86, and ICAM-I molecules compared with DCHER-2, indicating that the former ones are more mature forms of DCs. Vaccination of DCHER-2/TNF-α induced stronger allogeneic T-cell proliferation and 36% enhanced HER-2/neu-specific T-cell responses in vitro than DCHER-2 cells. More importantly, it stimulated the significant anti–HER-2/neu immunity in vivo, which protected 8/8 mice from challenge of 3×105 MCA26/HER-2 tumor cells. Therefore, DCs genetically engineered to express both the tumor antigen and cytokines such as TNF-α as an immunoadjuvant are likely to represent a new direction in DC vaccine of cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Coussens L, Yang-Feng TL, Liao YC et al. Tyrosine kinase receptor with extensive homology to EGF receptor shares chromosomal location with neu oncogene Science 1985 230: 1132–1139
Slamon DJ, Godolphin W, Jones LA et al. Studies of the HER-2/neu proto-oncogene in human breast and ovarian cancer Science 1989 244: 707–712
Ishikawa T, Kobayashi M, Mai M et al. Amplification of the c-erbB-2 (HER-2/neu) gene in gastric cancer cells Am J Pathol 1997 151: 761–768
Paterson MC, Dietrich KD, Danyluk J et al. Correlation between c-erbB-2 amplification and risk of recurrent disease in node-negative breast cancer Cancer Res 1991 51: 556–567
Andrulis IL, Bull SB, Blackstein ME et al. neu/erbB-2 amplification identifies a poor-prognosis group of women with node-negative breast cancer. Toronto Breast Cancer Study Group J Clin Oncol 1998 16: 1340–1349
Ioannides CG, Whiteside TL . T cell recognition of human tumors: implications for molecular immunotherapy of cancer Clin Immunol Immunopathol 1993 66: 91–106
Disis ML, Pupa SM, Gralow JR et al. High titer HER-2/neu protein-specific antibody can be detected in patients with early-stage breast cancer J Clin Oncol 1997 15: 3363–3367
Disis ML, Grabstein KH, Sleath PR et al. Generation of immunity to the HER-2/neu oncogenic protein in patients with breast and ovarian cancer using a peptide-based vaccine Clin Cancer Res 1999 5: 1289–1297
Zaks TZ, Rosenberg SA . Immunization with a peptide epitope (p369–377) from HER-2/neu leads to peptide-specific cytotoxic T lymphocytes that fail to recognize HER-2/neu+ tumors Cancer Res 1998 58: 4902–4908
Nagata Y, Furugen R, Hiasa A et al. Peptides derived from a wild-type murine protooncogene c-erbB-2/HER2/neu can induce CTL and tumor suppression in syngeneic hosts J Immunol 1997 159: 1336–1343
Weiner LM . Monoclonal antibody therapy of cancer Semin Oncol 1999 26: 43–51
Chen Y, Hu D, Eling DJ et al. DNA vaccines encoding full-length or truncated Neu induce protective immunity against Neu-expressing mammary tumors Cancer Res 1998 58: 1965–1971
Wei WZ, Shi WP, Galy A et al. Protection against mammary tumor growth by vaccination with full-length, modified human ErbB-2 DNA Int J Cancer 1999 81: 748–754
Foy TM, Bannink J, Sutherland RA et al. Vaccination with HER-2/neu DNA or protein subunits protects against growth of a HER-2/neu-expressing murine tumor Vaccine 2001 19: 2598–2606
Gabrilovich DI, Corak J, Ciernik IF et al. Decreased antigen presentation by dendritic cells in patients with breast cancer Clin Cancer Res 1997 3: 483–490
Troy AJ, Summers KL, Davidson PJ et al. Minimal recruitment and activation of dendritic cells within renal cell carcinoma Clin Cancer Res 1998 4: 585–593
Chaux P, Favre N, Martin M et al. Tumor-infiltrating dendritic cells are defective in their antigen-presenting function and inducible B7 expression in rats Int J Cancer 1997 72: 619–624
Nestle FO, Alijagic S, Gilliet M et al. Vaccination of melanoma patients with peptide or tumor lysate-pulsed dendritic cells Nat Med 1998 4: 328–332
Dhodapkar MV, Steinman RM, Sapp M et al. Rapid generation of broad T-cell immunity in humans after a single injection of mature dendritic cells J Clin Invest 1999 104: 173–180
Cella M, Sallusto F, Lanzavecchia A . Origin, maturation and antigen presenting function of dendritic cells Curr Opin Immunol 1997 9: 10–16
Pardoll D . Cancer vaccines Nat Med 1998 4: 525–530
Eggert A, Schreurs M, Boerman O et al. Biodistribution and vaccine efficiency of murine dendritic cells are dependent on the route of administration Cancer Res 1999 59: 3340–3345
Ribas A, Butterfield L, McBride W et al. Genetic immunization for the melanoma antigen MART-1/Melan-A using recombinant adenovirus-transduced murine dendritic cells Cancer Res 1997 57: 2865–2869
Butterfield L, Jilani S, Chakraborty N et al. Generation of melanoma-specific cytotoxic T lymphocytes by dendritic cells transduced with a MART-1 adenovirus J Immunol 1998 161: 5607–5613
Lapointe R, Royal R, Reeves M et al. Retrovirally transduced human dendritic cells can generate T cells recognizing multiple MHC class I and class II epitopes from the melanoma antigen glycoprotein 100 J Immunol 2001 167: 4758–4764
Labeur M, Roters B, Pers B et al. Generation of tumor immunity by bone marrow-derived dendritic cells correlates with dendritic cell maturation stage J Immunol 1999 162: 168–175
Zhang W, Chen Z, Li F et al. TNF-transgene-expressing dendritic cells undergo augmented cellular maturation and induce more robust T cell activation and antitumor immunity than dendritic cells generated in recombinant TNF Immunology 2002 In press
Wright P, Braun R, Babiuk L et al. Adenovirus-mediated TNF-α gene transfer induces significant tumor regression in mice Cancer Biother Radiopharm 1999 14: 49–57
Xiang J, Moyana T . Regression of engineered tumor cells secreting cytokines is related to a shift in host cytokine profile from type 2 to type 1 J Interferon Cytokine Res 2000 20: 349–354
Inaba K, Young J, Steiman R . Direct activation of CD8 cytotoxic T lymphocytes by dendritic cells J Exp Med 1987 166: 182–194
Andrechek E, Hardy W, Siegel P et al. Amplification of the neu/erbB-2 oncogene in a mouse model of mammary tumorigenesis Proc Natl Acad Sci USA 2000 97: 3444–3449
Tuting T, Wilson CC, Martin DM et al. Autologous human monocyte-derived dendritic cells genetically modified to express melanoma antigens elicit primary cytotoxic T cell responses in vitro: enhancement by cotransfection of genes encoding the Th1-biasing cytokines IL-12 and IFN-α J Immunol 1998 160: 1139–1147
Nishioka Y, Hirao M, Robbins PD et al. Induction of systemic and therapeutic antitumor immunity using intratumoral injection of dendritic cells genetically modified to express interleukin 12 Cancer Res 1999 59: 4035–4041
Curiel-Lewandrowski C, Mahnke K, Labeur M et al. Transfection of immature murine bone marrow-derived dendritic cells with the granulocyte-macrophage colony-stimulating factor gene potently enhances their in vivo antigen-presenting capacity J Immunol 1999 163: 174–183
Chen Y, Emtage P, Zhu Q et al. Induction of ErbB-2/neu-specific protective and therapeutic antitumor immunity using genetically modified dendritic cells: enhanced efficacy by cotransduction of gene encoding IL-12 Gene Ther 2001 8: 316–323
Kass E, Panicali D, Mazzara G et al. Granulocyte/macrophage-colony stimulating factor produced by recombinant avian poxviruses enriches the regional lymph nodes with antigen-presenting cells and acts as an immunoadjuvant Cancer Res 2001 61: 206–214
Banchereau J, Steinman RM . Dendritic cells and the control of immunity Nature 1998 392: 245–252
Jonuleit H, Knop J, Enk AH . Cytokines and their effects on maturation, differentiation and migration of dendritic cells Arch Dermatol Res 1996 289: 1–8
Brunner C, Seiderer J, Schlamp A et al. Enhanced dendritic cell maturation by TNF-α or cytidine-phosphate-guanosine DNA drives T cell activation in vitro and therapeutic antitumor immune responses in vivo J Immunol 2000 165: 6278–6286
Cumberbatch M, Kimber I . Tumor necrosis factor-α is required for accumulation of dendritic cells in draining lymph nodes and for optimal contact sensitization Immunology 1995 84: 31–35
Kobayashi H, Wood M, Song Y et al. Defining promiscuous MHC class II helper T-cell epitopes for the HER-2/neu tumor antigen Cancer Res 2000 60: 5228–5236
Ben-Levy R, Paterson H, Marshall C . A single autophosphorylation site confers oncogenicity to the Neu/ErbB-2 receptor and enables coupling to the MAP kinase pathway EMBO J 1994 13: 3302–3311
Acknowledgements
This study was supported by a research grant (3-782) from Saskatchewan Cancer Agency.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, Z., Huang, H., Chang, T. et al. Enhanced HER-2/neu-specific antitumor immunity by cotransduction of mouse dendritic cells with two genes encoding HER-2/neu and alpha tumor necrosis factor. Cancer Gene Ther 9, 778–786 (2002). https://doi.org/10.1038/sj.cgt.7700498
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cgt.7700498
Keywords
This article is cited by
-
Exosomal pMHC-I complex targets T cell-based vaccine to directly stimulate CTL responses leading to antitumor immunity in transgenic FVBneuN and HLA-A2/HER2 mice and eradicating trastuzumab-resistant tumor in athymic nude mice
Breast Cancer Research and Treatment (2013)
-
Differential immune responses mediated by adenovirus- and lentivirus-transduced DCs in a HER-2/neu overexpressing tumor model
Gene Therapy (2011)
-
Anti-HER2 vaccines: new prospects for breast cancer therapy
Cancer Immunology, Immunotherapy (2010)
-
Vaccination of fiber-modified adenovirus-transfected dendritic cells to express HER-2/neu stimulates efficient HER-2/neu-specific humoral and CTL responses and reduces breast carcinogenesis in transgenic mice
Cancer Gene Therapy (2008)
-
Tumor Protection Following Vaccination With Low Doses of Lentivirally Transduced DCs Expressing the Self-antigen erbB2
Molecular Therapy (2008)