Abstract
Objective:
To assess whether women having preconceptional health care utilization were more likely to have early initiation of prenatal care than were women not having preconceptional health care utilization.
Study Design:
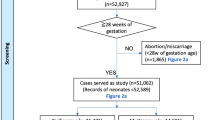
In this cohort study, data were collected prospectively from a population-based Perinatal Health Care Surveillance System in China. The analysis included 195?796 women who delivered single live births in 13 cities/counties during 1997 to 2000. Mantel–Haenszel test was employed to calculate risk ratios and 95% confidence intervals (CI). Multivariate logistic regression was conducted to assess the association between preconceptional health care utilization and early initiation of prenatal care after controlling for maternal residence, age at delivery, educational attainment, occupation, parity, preconceptional medical disorders, and high-risk medical experiences during the first trimester. SPSS 11.5 (SPSS Inc.) was employed for data analysis.
Results:
Women having preconceptional health care utilization were 2.6 times (95%CI: 2.5 to 2.6) more likely to have early initiation of prenatal care compared with women not having preconceptional health care utilization. When stratified by maternal residence, age at delivery, educational attainment, occupation, parity, preconceptional medical disorder, high-risk medical experiences during the first trimester, and preconceptional medical disorders, this association still existed. After controlling for stratification factors mentioned above and the interaction of maternal age, educational attainment, and parity, women having preconceptional health care utilization were 2.7 times (95%CI: 2.6 to 2.8) more likely to have early initiation of prenatal care than were women not having preconceptional health care utilization.
Conclusion:
Women who had preconceptional health care utilization were more likely to have early prenatal care than were women not having preconceptional health care utilization.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Centers for Disease Control and Prevention. Entry into prenatal care – United States, 1989–1997. MMWR 2000; 49 (18): 393–398.
Johnson AA, Ei-khorazaty MN, Hatcher BJ, Wingrove BK, Milligan R, Harris C et al. Determinants of late prenatal care initiation by African American women in Washington, DC. Matern Child Health J 2003; 7: 103–114.
Nothnagle M, Marchi K, Egerter S, Braveman P . Risk factors for late or no prenatal care following Medicaid expansions in California. Matern Child Health J 2000; 4: 251–259.
Elam-evans LD, Adams MM, Delaney KM, Wilson HG, Rochat RW, Mccarthy BJ . Patterns of prenatal care initiation in Georgia, 1980–1992. Obstet Gynecol 1997; 90: 71–77.
Tita ATN, Hollier LM, Waller K . Seasonality in conception of births and influence on late initiation of prenatal care. Obstet Gynecol 2001; 97: 976–981.
MaCaw-Binns A, La Grenade J, Ashley D . Under-user of antenatal care: a comparison of non-attenders and late attenders for antenatal care with early attenders. Soc Sci Med 1995; 40 (7): 1003–1012.
Wiemann CM, Berenson AB, Pino LG, McCombs SL . Factors associated with adolescents’ risk for late entry into prenatal care. Fam Plann Perspect 1997; 29: 273–276.
Petersen DJ, Alexander GR . Seasonal variation in adolescent conceptions, induced abortions, and late initiation of prenatal care. Public Health Rep 1992; 107: 701–706.
Chandler D . Late entry into prenatal care in a rural setting. J Midwifery Womens Health 2002; 47: 28–34.
Lia-Hoagberg B, Rode P, Skovholt CJ, Oberg CN, Berg C, Mullett S et al. Barriers and motivators to prenatal care among low-income women. Soc Sci Med 1990; 30: 487–495.
Kupek E, Petrou S, Vause S, Maresh M . Clinical, provider and sociodemograohic predictors of late initiation of antenatal care in England and Wales. BJOG 2002; 109: 265–273.
de Weerd S, Thomas CMG, Cikot RJLM, Steegers-Theunissen RPM, de Boo TM, Steegers EAP . Preconception counseling improves folate status of women planning pregnancy. Obstet Gynecol 2002; 99: 45–50.
Steel JM, Johnstone FD, Hepburn DA, Smith AF . Can prepregnancy care of diabetic women reduce the risk of abnormal babies? BMJ 1990; 301: 1070–1074.
Buekens P, Kotelchuck M, Blondel B, Kristensen FB, Chen J-H, Masuy-Stroobant G . A comparison of prenatal care use in the United States and Europe. Am J Public Health 1993; 83: 31–36.
Moos MK . Preconceptional health promotion: a health education opportunity for all women. Women Health 1989; 15 (3): 55–68.
Acknowledgements
We would like to gratefully acknowledge the work and supports of the leaders and health care professionals at all levels responsible for the operation of Perinatal Health Care Surveillance System in the surveyed areas.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on the Journal of Perinatology website (http://www.nature.com/jp)
Supplementary information
Rights and permissions
About this article
Cite this article
Liu, Y., Liu, J., Ye, R. et al. Association of preconceptional health care utilization and early initiation of prenatal care. J Perinatol 26, 409–413 (2006). https://doi.org/10.1038/sj.jp.7211537
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211537
Keywords
This article is cited by
-
The Association Between Preconception Care Receipt and the Timeliness and Adequacy of Prenatal Care: An Examination of Multistate Data from Pregnancy Risk Assessment Monitoring System (PRAMS) 2009–2011
Maternal and Child Health Journal (2018)
-
Prenatal Care Utilization in Mississippi: Racial Disparities and Implications for Unfavorable Birth Outcomes
Maternal and Child Health Journal (2011)
-
Impact of Pre-Conception Health Care: Evaluation of a Social Determinants Focused Intervention
Maternal and Child Health Journal (2010)