Abstract
The peroxisome proliferator-activated receptor γ (PPAR γ), a member of the nuclear receptor superfamily, is expressed at highest levels in adipose tissue and functions as a central regulator in the process of adipocyte differentiation. In the present study, we showed that human leukemic cell lines, not only myeloid but also lymphoid, express PPAR γ and its activation by natural ligand (15-deoxy-Δ12,14 - prostaglandin J2) and synthetic ligand (troglitazone) profoundly inhibited their proliferation by induction of apoptosis preferentially in the serum-free culture. We pursued its mechanism using the representative cell lines, and found that induction of apoptosis was accompanied by caspase-3 activation and specifically blocked by its inhibitor. While status of several apoptosis-related molecules remained unchanged, the c-Myc expression was markedly down-regulated within 24 h after troglitazone treatment. The c-myc mRNA levels were dramatically reduced at 1 h and became undetectable at 12 h after troglitazone treatment, which proved to be accompanied by complete blockade of the Tcf-4 activity in the electrophoretic mobility shift assay. We succeeded in establishing HL-60 cell lines growing well in the presence of troglitazone in the long-term serum-free culture. They showed neither induction of apoptosis nor down-regulation of the c-Myc expression via blockade of the Tcf-4 activity after troglitazone treatment. This is the first identification of the linkage between PPAR γ-mediated apoptosis and down-regulation of the c-myc gene expression.
Similar content being viewed by others
Introduction
The peroxisome proliferator-activated receptor (PPAR) forms a group of ligand-activated transcription factors that belong to the nuclear receptor superfamily which is characterized by a structural organization in functional modules consisting of a N-terminal domain, a DNA-binding domain, a hinge region, and a ligand-binding domain.1 The family of PPAR is comprised of three gene products (α, β and γ), each of which has different and specific tissue distribution and functions. PPAR α is predominantly expressed in hepatocytes, cardiomyocytes, proximal tubule cells of the kidney, and enterocytes, while PPAR β is more widely and often more abundantly expressed.2,3,4,5 PPAR γ is expressed at highest levels in adipose tissues and functions as a central regulator in the process of adipocyte differentiation.6,7 Activated PPAR γ forms a heterodimer with retinoid X receptor (RXR) and binds to the peroxisome proliferator responsive element (PPRE), which consists of a hexameric nucleotide direct repeat of recognition motif (AGGTCA) spaced by one nucleotide (DR-1).8,9,10 Recently, new specific activators and ligands for the different PPAR subtypes are emerging. 15-deoxy-Δ12,14-prostaglandin J2 (15d-PGJ2) is identified as a natural ligand for PPAR γ,11 while thiazolidinediones (TZDs) such as troglitazone, pioglitazone, and BRL49653 are chemically synthesized ligands for PPAR γ and have been used as a new class of oral anti-diabetic agents for the treatment of hyperglycemia and insulin resistance in type II diabetes.12,13
Although adipose tissue has been recognized as a principal site of the PPAR γ expression, it is now known that PPAR γ is expressed in many other types of tissues and cells. PPAR γ is expressed in peripheral monocytes and peritoneal macrophages and ligand activation of this receptor leads to inhibition of phorbol ester-induced nitric oxide and cytokine production.14,15 PPAR γ is also expressed at high levels in the colon16 and its ligand activation is shown to be involved in promotion or regression of colon tumors.17,18,19,20 Thus, PPAR γ is implicated in many processes relating to different aspects of cellular development, differentiation, and physiology.21 Recently, it has been shown that PPAR γ is expressed in some myeloid leukemic cell lines22 and their proliferation is suppressed by PPAR γ agonists through induction of the cyclin-dependent kinase inhibitor p21.23 It is also shown that ligand activation of this receptor promotes monocyte/macrophage differentiation24 or even partially induces apoptosis at a higher concentration25 in the human promyelocytic leukemic cell line HL-60 in the culture condition fully supplemented with fetal calf serum (FCS). The activity of PPAR γ agonists capable of modestly inducing apoptosis has also been documented in a variety of tumor types other than hematologic malignancy.26,27,28 However, it remains to be clarified regarding mechanism(s) of apoptosis induced by PPAR γ agonists.
In the present study, we show that triggering of PPAR γ induces apoptosis in a variety of human leukemic cell lines by activating caspase-3 preferentially in the serum-free culture, in the process of which marked down-regulation of the c-myc gene expression via complete blockade of the Tcf-4 activity is implicated.
Results
PPAR γ is constitutively expressed in leukemia cells
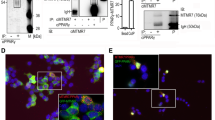
We first examined the PPAR γ expression on Western blot using 10 leukemic cell lines (lanes 1–5; myeloid; lane 6; T-lymphoid; lanes 7–10: B-lymphoid). As shown in Figure 1A, all cell lines constitutively expressed PPAR γ at a variety of levels; relatively lower expression in three B-lymphoid cell lines (lanes 7, 8 and 10). It is known that the preadipocyte cell line 3T3-L1 expresses two splicing-generated isoforms of PPAR γ (γ 1 and γ 2),29,30 and the γ 2 form is phosphorylated in differentiated 3T3-L1 cells.16,31,32 We compared the PPAR γ expression between the promyelocytic leukemic cell line HL-60 and positive (3T3-L1) and negative (fibroblast) controls. As shown in Figure 1B, HL-60 cells expressed PPAR γ 2, but not γ 1, at lower levels (lane 4) compared with undifferentiated (lane 2) and differentiated (lane 3) 3T3-L1 cells. The upper band of doublets, sometimes visualized in HL-60 cells on Western blot, might be the partially phosphorylated γ 2 form.
Expression of PPAR γ. (A) Expression of PPAR γ in human leukemic cell lines. The expression of PPAR γ in non-lymphoid cell lines (KOPM-28, KOPM-30, HL-60, ML-1, U937; lanes 1–5) and lymphoid cell lines (KOPT-K1, KOPN-30bi, KOPN-55bi, KOPN-46, KOCL-69; lanes 6–10) was examined on Western blot using anti-PPAR γ antibody. Anti-α-tubulin antibody was used for positive control. (B) Comparison of PPAR γ expression between HL-60 and 3T3-L1. The expression of PPAR γ in fibroblast (lane 1; negative control), undifferentiated (lane 2) and differentiated (lane 3) 3T3-L1 (positive controls), and HL-60 (lane 4) was examined on Western blot using anti-PPAR γ antibody
PPAR γ activation markedly inhibits DNA synthesis of leukemia cells
To assess the effect of PPAR γ agonists, we tested leukemic cell lines for their kinetics of [3H]-thymidine uptake in the absence or presence of different concentrations (2, 4, 6 μg/ml) of troglitazone in FCS-free D-MEM/F12 medium. As representatively shown in Figure 2 (myeloid one, B-lymphoid two, T-lymphoid one), [3H]-thymidine uptake in all of the cell lines examined was inhibited by troglitazone in a dose-dependent manner, showing a greater than 98% inhibition at a concentration of 6 μg/ml. The inhibition was observed from the first day and reached maximal levels between 3 and 5 days after initiation of culture. As depicted in HL-60 cells, an addition of 15d-PGJ2 also showed a similar inhibition of [3H]-thymidine uptake in a dose-dependent manner (0.25–1 μM), showing a greater than 98% inhibition at a concentration of 0.5 or 1 μM (Figure 3A). Of note, an addition of FCS to D-MEM/F12 medium dose-dependently suppressed the inhibition by troglitazone (Figure 3B). The troglitazone-induced inhibition was not suppressed by an addition of cycloheximide (CHX) even at a concentration of 1 μg/ml that inhibits the cellular growth by itself (Figure 3C), suggesting no requirement of protein synthesis for the inhibitory effect of troglitazone on [3H]-thymidine uptake. These results suggest that PPAR γ agonists exert a profound inhibitory effect on the proliferation of leukemia cells preferentially in the serum-free culture system.
Kinetics of [3H]-thymidine uptake. HL-60, KOCL-69, KOPN-55bi, and KOPT-K1 were cultured in D-MEM/F12 medium with or without different concentrations (0 μg/ml, open squares; 2 μg/ml, filled squares; 4 μg/ml, open circles; 6 μg/ml, filled circles) of troglitazone, and their [3H]-thymidine uptakes were measured at different days. Results are expressed as the mean c.p.m of triplicate samples and the S.E. was always less than 10%. Data shown are representatives of three separate experiments
The effect of PPAR γ agonists on HL-60 cells. Results are expressed as the mean c.p.m of triplicate samples and the S.E. was always less than 10%. Data shown are representatives of three separate experiments. (A) Kinetics of [3H]-thymidine uptake after 15d-PGJ2 treatment. HL-60 was cultured in D-MEM/F12 with or without different concentrations (0 μM, open squares; 0.25 μM, filled squares; 0.5 μM, open circles; 1 μM, filled circles) of 15d-PGJ2, and their [3H]-thymidine uptakes were measured at different days. (B) The effect of FCS on [3H]-thymidine uptake after troglitazone treatment. HL-60 was cultured in D-MEM/F12 for 3 days with or without different concentrations (0–10 μg/ml) of troglitazone in the presence or absence of different concentrations (0%, open squares; 1%, filled squares; 4%, open circles; 7%, filled circles; 10%, filled triangles) of FCS, and their [3H]-thymidine uptakes were measured. (C) The effect of cycloheximide (CHX) on [3H]-thymidine uptake after troglitazone treatment. HL-60 was cultured in D-MEM/F12 for 3 days with or without different concentrations (0 μg/ml, open squares; 2 μg/ml, filled squares; 4 μg/ml, open circles; 6 μg/ml, filled circles) of troglitazone in the presence or absence of different concentrations (0, 0.01, 0.1, and 1 μg/ml) of CHX, and their [3H]-thymidine uptakes were measured. (D) Kinetics of cell numbers after troglitazone treatment. HL-60 was cultured in D-MEM/F12 with or without different concentrations (0 μg/ml, open squares; 4 μg/ml, open circles; 6 μg/ml, filled circles) of troglitazone, and numbers of living cells were counted at different exposure times (6, 12, 24, 36 and 48 h). Results are expressed as the mean cell number of triplicate samples and the S.E. shown as vertical bars was always less than 10%
PPAR γ activation strongly induces apoptosis of leukemia cells
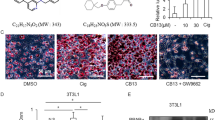
To address an inhibitory effect of troglitazone, we examined changes in the cell number of leukemia cells in the serum-free culture after troglitazone treatment by dye exclusion test. As representatively shown in HL-60 cells (Figure 3D), living cells were gradually decreased from 12 h after troglitazone treatment, and a few living cells were detectable after 48 h-culture with 6 μg/ml of troglitazone. We next examined the morphological changes of HL-60 and KOPT-K1 cells on smears, and found that a large population of cells showed features characteristic of apoptosis (cell shrinkage, condensed chromatin, and fragmented nuclei) 24 h after treatment with 6 μg/ml of troglitazone (Figure 4). The cell cycle analysis also showed that 24 h-treatment of HL-60 with troglitazone dose-dependently increased the populations in hypodiploid region (M1) corresponding to the apoptotic cells (Figure 5, left). The M1 populations were apparently detected at 12 h (62.9%) and reached 75.9% at 24 h after treatment with 6 μg/ml of troglitazone (Figure 5, right). A lower concentration (4 μg/ml) of troglitazone partially induced apoptosis with a concomitant inhibition of cell cycle progression. These results suggest that full-scaled ligand activation of PPAR γ strongly induces apoptosis of leukemia cells in the serum-free culture.
Cell cycle analysis after troglitazone treatment. Left: HL-60 was cultured in D-MEM/F12 for 24 h with or without different concentrations (0, 2, 4 and 6 μg/ml) of troglitazone. Right: HL-60 was cultured in D-MEM/F12 for different exposure times (6, 12 and 24 h) with troglitazone (6 μg/ml). Cell cycle analysis was performed as described in Materials and methods. Horizontal and vertical axes represent DNA content and cell number, respectively. Hypodiploid cells (M1 region) were considered as apoptotic cells. The data were representatives from three separate experiments
PPAR γ activation induces cleavage of caspase-3
It is currently indicated that cysteine proteases, called caspases, could be central components of cell death machinery in various forms of apoptosis. Of the 10 members of caspases identified, caspase-3 (CPP32/Apopain) is one of the strongest mammalian cell-death-inducing proteases.33 We therefore investigated whether induction of apoptosis by troglitazone depends on activation of caspase-3. Since caspase-3 is cleaved from its 32 kDa inactive precursor form to the 17 and 12 kDa subunits with strong protease activity through the 19 and 20 kDa intermediate cleavage products, this cleavage process was pursued on Western blot using anti-caspase-3 antibody which is known to react with the 32, 20, 19 and 17 kDa forms. As shown in Figure 6A, the 32 kDa inactive form in HL-60 and KOPT-K1 cells was started to be cleaved into the 17 kDa active form after 12 h-treatment with troglitazone (6 μg/ml). This activation process was specifically blocked by an addition of a selective inhibitor Z-DEVD-FMK at 50 μM or higher concentrations in HL-60 cells, which was visualized as disappearance of the 17 kDa active form (Figure 6B). Moreover, an addition of Z-DEVD-FMK (50 μM) partially inhibited apoptosis induced by troglitazone (data not shown). These results indicate that the troglitazone-induced apoptosis is at least elicited by activation of caspase-3.
Cleavage of caspase-3 after troglitazone treatment. (A) Activation of caspase-3, HL-60 and KOPT-K1 cell lines were cultured in D-MEM/F12 with troglitazone (6 μg/ml) and harvested at indicated times; (lanes 1–5: 0, 3, 6, 12 and 24 h for HL-60, lanes 6–9: 0, 12, 24 and 48 h for KOPT-K1), and the total cell lysates were subjected to Western blotting and stained with anti-caspase-3 antibody. The 32 kDa uncleaved, the 19 kDa partially cleaved, and the 17 kDa cleaved products of caspase-3 were indicated by arrows. (B) Inhibition of caspase-3 cleavage by Z-DEVD-FMK. HL-60 was cultured in D-MEM/F12 with troglitazone (6 μg/ml) for 24 h with or without different concentrations of Z-DEVD-FMK (lanes 1–4: 0, 25, 50 and 100 μM), and the total cell lysates were subjected to Western blotting and stained with anti-caspase-3 antibody. The 32 kDa uncleaved, 20/19 kDa partially cleaved, and 17 kDa cleaved products of caspase-3 were indicated by arrows
PPAR γ activation does not induce changes in the expression or tyrosine phosphorylation of several apoptosis-related molecules
The susceptibility of normal and cancer cells to induction of apoptosis is regulated by the balance of expression between apoptosis-inducing genes/proteins and apoptosis-suppressing genes/proteins. The anti-apoptotic proteins Bcl-2 and Bcl-XL, which reside mainly in the outer mitochondrial membranes, inhibit activation of caspase-3 by preventing release of cytochrome c,34 whereas apoptosis-inducing proteins such as Bax and Bad induce its release by counteracting anti-apoptotic proteins. The interaction of Fas, a member of TNF receptor family, with its ligand (FasL) activates caspase-8, which induces apoptosis by cleaving and activating downstream caspases such as caspase-3.35 To identify mechanism of the troglitazone-induced apoptosis, we investigated changes in the expression of several apoptosis-related molecules. Given the information that promoter-enhancer regions of FasL gene (AGGTCT C AGGTAA from −2160 to −2148) and Bax gene (AGTTCA G AGACCA from −794 to −806) have similar sites to DR-1,36,37 we first examined the expression of FasL on flow cytometry and Bax on Western blot in HL-60 cells, but the expression of both molecules was not changed up to 24 h after troglitazone treatment (data not shown). In addition, no changes in the expression of Bcl-2, Bcl-XL, and Fas in HL-60 cells were demonstrated (data not shown).
Tyrosine phosphorylation of c-Jun N-terminal kinase 1 (JNK1) and p38 induced by environmental stresses such as osmolar change, ionizing radiation, anti-cancer drugs, and serum starvation is known to be associated with induction of apoptosis.38,39,40,41,42 Since apoptosis induced by PPAR γ activation is facilitated in the serum-free culture condition, we examined changes in their tyrosine phosphorylation. JNK1 and p38 were tyrosine phosphorylated before stimulation, but their up-regulation of phosphorylation was not observed in HL-60 cells after troglitazone treatment (data not shown).
PPAR γ activation markedly down-regulates the expression of c-Myc protein and c-myc mRNA
c-Myc (c-myc proto-oncogene product) is not only a transcriptional activator implicated in the control of cell proliferation, differentiation, and transformation, but also involved in the regulation of apoptosis.43 We investigated changes in the c-Myc expression in the serum-free culture after troglitazone treatment (6 μg/ml) on Western blot using HL-60, KOPT-K1, and KOPN-55bi cell lines. The c-Myc expression was started to be down-regulated between 3 and 6 h after treatment and became almost or completely undetectable at 24 h, although time course of c-Myc down-regulation slightly varied among cell lines and among experiments (Figure 7A). Down-regulation of c-Myc by troglitazone was observed in a dose-dependent manner (Figure 7B). To rule out the possibility that FCS starvation itself down-regulates the c-Myc expression, we examined changes in the c-Myc expression after incubation of HL-60 cells in FCS-free D-MEM/F12 medium for 24 h without an addition of troglitazone, and found that the C-Myc expression was not decreased, but rather up-regulated (Figure 7C). Since the troglitazone-mediated inhibition of [3H]-thymidine uptake was dose-dependently blocked by an addition of FCS into the medium (Figure 3B), we investigated the effect of FCS on the c-Myc expression after 24 h-treatment with troglitazone using HL-60 and KOPT-K1. As shown in Figure 7D, down-regulation of the c-Myc expression was also suppressed by an addition of FCS in a dose-dependent fashion. Given the information that PPAR γ agonists promote monocyte/macrophage differentiation in the culture condition fully supplemented with FCS24 or even induces apoptosis at a higher concentration in HL-60 cells,25 we next investigated whether higher concentrations of 24 h-treatment with troglitazone are capable of suppressing c-Myc expression in 10% FCS-medium. As shown in Figure 7E, the c-Myc expression in HL-60 and KOPT-K1 was not changed by troglitazone up to a concentration of 10 μg/ml (lanes 1–5 and 7–11), but down-regulated at 12 μg/ml (lanes 6 and 12). In addition, marked inhibition of [3H]-thymidine uptake and induction of apoptosis was also observed in HL-60 and KOPT-K1 after 24 h-treatment with troglitazone greater than 12 μg/ml in the culture condition supplemented with 10% FCS (data not shown). These results suggest that inhibition of the c-Myc expression might play a key role in the troglitazone-induced apoptosis preferentially in the condition where anti-apoptotic signals are not delivered from FCS, although higher concentrations of troglitazone can induce apoptosis with c-Myc down-regulation even in the presence of high concentrations of FCS.
Changes in the expression of c-Myc protein and c-myc mRNA after troglitazone treatment. On Western blotting, the membranes were stained with anti-c-Myc or anti-α-tubulin antibody (positive control). (A) The c-Myc expression after treatment with troglitazone (6 μg/ml) in serum free culture. HL-60 (lanes 1–5), KOPT-K1 (lanes 6–10), and KOPN-55bi (lanes 11–15) cells were cultured in D-MEM/F12 with troglitazone (6 μg/ml) and harvested at the indicated times (lanes 1, 6 and 11, lanes 2, 7 and 12, lanes 3, 8 and 13, lanes 4, 9 and 14, and lanes 5, 10 and 15; 0, 3, 6, 12 and 24 h, respectively). (B) The c-Myc expression after treatment with different concentrations of troglitazone. HL-60 (lanes 1–4) and KOPT-K1 (lanes 5–8) were cultured in D-MEM/F12 for 24 h with or without different concentrations (lanes 1–4: 0, 2, 4 and 6 μg/ml; lanes 5–8: 0, 2, 4 and 6 μg/ml) of troglitazone. (C) The c-Myc expression after serum free culture without troglitazone. HL-60 was washed and cultured in D-MEM/F12 without an addition of troglitazone and harvested at the indicated times (lanes 1–3; 0, 12 and 24 h). (D) The c-Myc expression after troglitazone treatment in the presence of different concentrations of FCS. HL-60 (lanes 1–5) and KOPT-K1 (lanes 6–10) were cultured for 24 h in D-MEM/F12 medium with (lanes 2–5, lanes 7–10) or without (lanes 1, 6) troglitazone (6 μg/ml) in the absence (lanes 1, 2, 6 and 7) or presence of different concentration of FCS (lanes 3–5: 1, 4 and 7%, lanes 8–10: 1, 4 and 7%). (E) The c-Myc expression after treatment with different concentrations of troglitazone in the presence of 10% FCS. HL-60 (lanes 1–6) and KOPT-K1 (lanes 7–12) were cultured in 10% FCS-D-MEM/F12 medium for 24 h with or without different concentrations (lanes 1–6: 0, 4, 6, 8, 10 and 12 μg/ml; lanes 7–12: 0, 4, 6, 8, 10 and 12 μg/ml) of troglitazone. (F) The c-myc expression after troglitazone treatment. HL-60 was cultured in D-MEM/F12 with troglitazone (6 μg/ml) and RNA was isolated at the indicated times (lanes 1–5; 0, 1, 3, 6 and 12 h). Northern blot analysis was performed using a probe for c-myc. Each lane contains 25 μg of total RNA and equal loading was shown by amount of 28S ribosomal RNAs stained with ethidium bromide
To pursue mechanism of decrease in the c-Myc expression after troglitazone treatment (6 μg/ml), we examined changes in c-myc mRNA levels on Northern blot. As shown in Figure 7F, the c-myc mRNA levels (both 2.3 kb major and 3.1 kb minor transcripts) were dramatically reduced up to one-twentieth at 1 h, gradually tapered thereafter, and became undetectable at 12 h after treatment, indicating that reduction of c-myc mRNA levels might be responsible for down-regulation of the c-Myc expression after troglitazone treatment.
PPAR γ activation does not fully inhibit the DNA binding of NF-κB
Since it is known that the murine c-myc promoter contains the responsive element of NF-κB44,45 and that inhibition of DNA binding of NF-κB induces apoptosis of murine B-lymphoma cells with down-regulation of c-myc,44 we tried to investigate whether NF-κB activity could be repressed by PPAR γ activation in HL-60 cells. However, it was very difficult to evaluate an inhibitory effect of troglitazone in the electrophoretic mobility shift assay (EMSA) because the endogenous NF-κB activity was too low before troglitazone treatment. Therefore, HL-60 cells were pretreated with TNF-α (10 μg/ml) to enhance the NF-κB activity according to the previous reports.46,47 Preincubation of HL-60 cells with TNF-α efficiently up-regulated the NF-κB activity, which was only partially inhibited by 1-h treatment with 6 μg/ml of troglitazone (data not shown).
PPAR γ activation completely inhibits the DNA binding of Tcf-4
The c-myc oncogene is also known to be regulated by the adenomatous polyposis coli (APC)/β-catenin/Tcf-4 pathway. In normal colon cells, the c-myc expression is repressed by wild-type APC which negatively regulates β-catenin. β-catenin is a coactivator for the transcription factor, such as T cell factor (Tcf)/lymphoid enhancer factor (Lef) which is able to directly activate c-myc expression through the specific DNA binding in the c-myc promoter. In APC-deficient colon-carcinoma cell lines, the constitutive presence of transcriptionally active nuclear β-catenin/Tcf-4 complexes are observed and c-myc is active all the time.48 We therefore investigated whether the endogenous Tcf-4 activity could be repressed by PPAR γ activation. For this purpose, HL-60 cells were first cultured in the absence of troglitazone in D-MEM/F12 medium for 120 min, and the Tcf-4 activity was evaluated in EMSA. As shown in Figure 8, two bands of the Tcf-4 DNA complexes (lanes 1, 6 and 8) were demonstrated, and their specificity was proved by invisualization with an addition of unlabeled Tcf-4 consensus sequence (lane 7) and by supershift of the upper band with antibodies against Tcf-3/-4 (lane 2) and Tcf-4 (lane 3). The Tcf-4 DNA complexes were not supershifted with antibodies against β-catenin (lane 4) and PPAR γ (lane 5). HL-60 cells were next incubated in the presence of troglitazone (6 μg/ml) in D-MEM/F12 medium for various times (30, 60, 90 and 120 min), and then nuclear extracts were prepared for EMSA. Surprisingly, these complexes became undetectable at 30 min (lane 9) after troglitazone treatment and did not reappear at 60 (lane 10), 90 (lane 11) and 120 (lane 12) min. These results suggest that down-regulation of c-myc transcript after PPAR γ activation might be mediated by the complete blockade of the Tcf-4 activity.
Inhibition of the DNA binding of Tcf-4 after PPAR γ activation. HL-60 cells were cultured in the absence of troglitazone in D-MEM/F12 medium for 120 min, and nuclear extracts were prepared (lanes 1–8) which were incubated without antibody (lane 1) or with antibody against Tcf-3/-4 (lane 2), Tcf-4 (lane 3), β-catenin (lane 4), or PPAR γ (lane 5), followed by an addition of 32P-labeled Tcf-4 oligonucleotide in the absence (lane 6) or presence of 100-fold excess of unlabeled mismatched (lanes 1–5) or consensus (lane 7) Tcf-4 oligonucleotide for EMSA. Nuclear extracts were also prepared from HL-60 after incubation with troglitazone (6 μg/ml) for 30 (lane 9), 60 (lane 10), 90 (lane 11), or 120 min (lane 12) in D-MEM/F12 medium, followed by an addition of 32P-labeled Tcf-4 oligonucleotide in the presence of 100-fold excess of unlabeled mismatched Tcf-4 oligonucleotide. The reaction mixture of nuclear extracts were run on polyacrylamide gels and analyzed by autoradiography. The bands specific for Tcf-4 and supershifted by anti-Tcf-4 or anti-Tcf-3/-4 antibody were indicated by closed and open arrows, respectively
c-Myc is not down-regulated after PPAR γ activation in the troglitazone-resistant HL-60 cells
To add evidence of a causative link between troglitazone-induced apoptosis and down-regulation of c-Myc, we established the mildly resistant (up to 2 μg/ml of troglitazone) and highly resistant (up to 4 μg/ml of troglitazone) HL-60 cell lines in the serum-free culture. No difference in the PPAR γ expression was observed on Western blot among original (sensitive) and two resistant cell lines (data not shown). As shown in Figure 9A, numbers of living cells were decreased markedly in the sensitive cell line, slightly in the mildly resistant cell line, but almost not in the highly resistant cell line after treatment with 4 μg/ml of troglitazone. Using these three cell lines, we investigated changes in the c-Myc expression on Western blot after 24 h-culture with or without 4 μg/ml of troglitazone (Figure 9B). Although the c-Myc expression was almost identical in the culture without troglitazone, its down-regulation was only modest in the mildly resistant cell line and was not observed in the highly resistant cell line in the culture with troglitazone in contrast to its disappearance in the sensitive cell line. The expression of α-tubulin used as control substantially remained unchanged. This result supports the notion that down-regulation of c-Myc might play a pivotal role in the apoptotic event of leukemia cells after PPAR γ activation.
Analysis of troglitazone-resistant HL-60 cells. (A) Kinetics of cell numbers after troglitazone treatment. The original (left), the mildly resistant (up to 2 μg/ml of troglitazone; middle), and the highly resistant cell lines (up to 4 μg/ml of troglitazone; right) were cultured in D-MEM/F12 in the absence (open squares) or presence of 4 μg/ml (filled circles) of troglitazone, and numbers of living cells were counted at 24 and 48 h after treatment. Results are expressed as the mean cell number of triplicate samples and the S.E. shown as vertical bars was always less than 10%. Data shown are representatives of three separate experiments. (B) Changes in the c-Myc expression with or without troglitazone treatment. Sensitive (lanes 1, 2), mildly resistant (lanes 3, 4), and highly resistant (lanes 5, 6) cell lines were cultured in D-MEM/F12 in the absence (lanes 1, 3 and 5) or presence (lanes 2, 4 and 6) of troglitazone (4 μg/ml) for 48 h. The total cell lysates were subjected to Western blotting and stained with anti-c-Myc or anti-α-tubulin antibody. (C) Comparison of Tcf-4 activity before troglitazone treatment among sensitive and resistant cell lines. Nuclear extracts were prepared from sensitive (lanes 1–4), mildly resistant (lanes 5–8), and highly resistant (lanes 9–12) HL-60 cell lines, and incubated for 30 min without (lanes 1–3, 5–7 and 9–11) or with anti-Tcf-4 antibody (lanes 4, 8 and 12) followed by an addition of 32P-labeled Tcf-4 oligonucleotide in the absence (lanes 1, 5 and 9) or presence of 100-fold excess of unlabeled mismatched (lanes 3, 4, 7, 8, 11 and 12) or consensus (lanes 2, 6 and 10) Tcf-4 oligonucleotide for EMSA. The reaction mixture of nuclear extracts were run on polyacrylamide gels and analyzed by autoradiography. The bands specific for Tcf-4 and supershifted by anti-Tcf-4 antibody were indicated by closed and open arrows, respectively. (D) Sensitive (lanes 1–6) and mildly resistant (lanes 7–15) HL-60 cell lines were cultured in the absence (lanes 1–3 and 7–9) or presence (lanes 4–6 and 10–15) of troglitazone (4 μg/ml) in D-MEM/F12 medium for 30 min (lanes 4, 5, 6, 10, 11 and 12), or 60 min (lanes 13, 14 and 15), and their nuclear extracts were incubated for 30 min without (lanes 1, 2, 4, 5, 7, 8, 10, 11, 13, and 14) or with anti-Tcf-4 antibody (lanes 3, 6, 9, 12 and 15) followed by an addition of 32P-labeled Tcf-4 oligonucleotide in the presence of 100-fold excess of unlabeled mismatched (lanes 2, 3, 5, 6, 8, 9, 11, 12, 14 and 15) or consensus (lanes 1, 4, 7, 10 and 13) Tcf-4 oligonucleotide for EMSA. The reaction mixture of nuclear extracts were run on polyacrylamide gels and analyzed by autoradiography. The bands specific for Tcf-4 and supershifted by anti-Tcf-4 antibody were indicated by closed and open arrows, respectively
PPAR γ activation does not inhibit the DNA binding of Tcf-4 in the troglitazone-resistant HL-60 cells
To further pursue mechanism of resistance to apoptosis with c-Myc down-regulation after PPAR γ activation, we investigated whether or not the endogenous Tcf-4 activity could be repressed by PPAR γ activation in the resistant HL-60 cell lines. For this purpose, we first evaluated the Tcf-4 activity before troglitazone treatment in the sensitive, mildly resistant, and highly resistant cell lines in EMSA, and found that the Tcf-4 activity was lowest in the sensitive cell line and highest in the highly resistant cell line (Figure 9C). We next examined changes in the Tcf-4 activity after treatment with 4 μg/ml of troglitazone in EMSA using the sensitive and mildly resistant cell lines (Figure 9D), and found that the complex band supershifted with anti-Tcf-4 antibody was only modestly down-regulated not only 30 but also 60 min after treatment in the mildly resistant cell line (lanes 12 and 15) in contrast to its disappearance 30 min after treatment in the sensitive cell line (lane 6). No down-regulation of the supershifted band was demonstrated in the highly resistant cell line which can grow well in the presence of 4 μg/ml of troglitazone before experiment (data not shown). These results suggest that resistance to apoptosis by PPAR γ activation is mediated by a gain of the Tcf-4 activity not fully influenced by ligand activation of PPAR γ.
Discussion
The c-myc proto-oncogene was initially identified as the cellular homolog of the viral oncogene v-myc, and its critical role in tumorigenesis has been well established.49 The c-myc gene product, c-Myc, is a member of the helix–loop–helix/leucine zipper transcription factor family whose function is achieved by heterodimerization with Max protein and subsequent activation of target genes via binding to the CAC (G/A) TG nucleotide motif.50 Its transcriptional activity is not only implicated in the control of cell proliferation, differentiation, and transformation, but also involved in the regulation of programmed cell death, apoptosis.43 The relationship between apoptosis and alteration in the c-Myc expression has been extensively studied in the past. Some investigators found that up-regulation of c-Myc expression caused apoptosis,51,52,53 while others provided a line of evidence that its down-regulation resulted in induction of apoptosis with caspase-3 activation.44,54 It is also reported that both down-regulation of c-myc expression by exposure to c-myc antisense oligodeoxynucleotide phosphorothioate and up-regulation after its withdrawal induces apoptosis of HL-60 cells.55
In the present study, we showed that ligand activation of PPAR γ strongly induced apoptosis of human myeloid and lymphoid leukemia cells preferentially in the serum-free culture system. We pursued mechanism of this event using several cell lines including HL-60 cells and found that down-regulation of the c-Myc expression by decrease in c-myc transcript might play a central role. In the glucocorticoid-induced apoptosis of leukemia cells which is known to accompany suppression of c-myc,55 the possibility has been raised that the glucocorticoid receptor is not always necessary to bind the DNA sequence because the mutant receptor lacking the DNA binding domain is as effective as the wild-type receptor in inhibition of the c-myc expression and induction of apoptosis.56 We thus postulated that the primary role of liganded PPAR γ is to associate with and then suppress (or activate) molecule(s) involved in up-regulation (or down-regulation) of the c-myc transcription, which supports our observations that induction of apoptosis by PPAR γ activation did not require protein synthesis and the c-myc promoter does not contain the DR-1 sequence to which PPAR γ can directly bind. It is reported that the murine and human c-myc promoter contains the responsive element of NF-κB,45,57,58 inhibition of DNA binding of NF-κB by blockade of rapid turnover of IκBα (inhibitor of NF-κB) with the specific serine/threonine protease inhibitor induces apoptosis of WEHI 231 murine B-lymphoma cells with down-regulation of c-Myc,44 and that activation of PPAR γ inhibits the transcriptional activity of the NF-κB p65 subunit in human monocyte-derived macrophages.57 Therefore, we first examined changes in the NF-κB activity after troglitazone treatment in HL-60 cells, but could not find evidence that the DNA binding of NF-κB was clearly suppressed.
There are four known members of the Tcf/Lef family in mammals: the lymphoid-specific factors Tcf-1 and Lef-1 and less well characterized Tcf-3 and Tcf-4.48,59 Recent evidence suggests that activation of c-myc gene is a key target for the APC/β-catenin/Tcf-4 pathway.48 Therefore, we next examined changes in the Tcf-4 activity after troglitazone treatment, and found that the DNA binding of Tcf-4 was completely inhibited, suggesting a pivotal role of suppression of the Tcf-4 activity in down-regulation of the c-myc gene expression.
We also showed that both induction of apoptosis and c-Myc down-regulation after PPAR γ activation were suppressed by an addition of FCS in a dose-dependent fashion although a higher concentration of troglitazone can induce apoptosis with down-regulation of c-Myc. It is reported that, in the culture condition fully supplemented with FCS, ligand activation of PPAR γ primarily induces monocyte/macrophage differentiation of HL-60 cells,6 suggesting that undetermined substance(s) included in FCS can transmit anti-apoptotic signal(s) implicating in the maintenance of the c-myc gene expression.
To address a causative link between induction of apoptosis and down-regulation of c-Myc after PPAR γ activation, we tried to generate HL-60 cells expressing exogenous c-myc cDNA by transfection of zinc-inducible expression plasmids, but failed because rapid induction of the c-Myc expression with ZnSO4 caused death of HL-60 cells irrespective of the presence or absence of troglitazone (data not shown). Therefore, we next tried to generate cell lines resistant to troglitazone in the serum free culture, and succeeded in establishing HL-60 cell lines growing well in the presence of troglitazone (2–4 μg/ml). We found that the c-Myc expression was only slightly or not down-regulated in the resistant cell lines after troglitazone treatment. To address this point, we examined the Tcf-4 activity in the sensitive and resistant cell lines in EMSA, and found the higher resistance to troglitazone was associated with the higher Tcf-4 activity. Moreover, the Tcf-4 activity was not getting down-regulated after PPAR γ activation as resistance to troglitazone was getting increased, strongly suggesting that the rescue from c-Myc down-regulation via complete blockade of the Tcf-4 activity might be mechanism of resistance to apoptosis by PPAR γ activation. Although it remains unclear at present how activation of PPAR γ inhibits the Tcf-4 activity, our preliminary data on coimmunoprecipitation experiments suggest the possibility that the liganded PPAR γ directly or indirectly recruits free Tcf-4 and thereby inhibits its DNA binding to the c-myc promotor (data not shown). In this regard, it might be possible that recruitment of free Tcf-4 by liganded PPAR γ is suppressed by an unknown mechanism in the resistant cell lines.
It is already shown that troglitazone reduces the growth rate of human colon and prostate tumors transplanted in mice.17,60 In addition, it is also shown that ligand activation of PPAR γ markedly inhibits angiogenesis in vitro and in vivo through reduction of mRNA levels of vascular endothelial cell growth factor receptors 1 and 2 and urokinase plasminogen activator.61 Thus, troglitazone might be applicable to the treatment of leukemia by itself or in combination with chemotherapeutic agents through the direct cytotoxic effect and/or inhibition of angiogenesis closely associated with tumor progression. The experiments using the mouse model are now under investigation.
Materials and Methods
Cells
Ten human leukemic cell lines; five myeloid (KOPM-28, KOPM-30, HL-60, ML-1, U937), one T-lymphoid (KOPT-K1), four B-lymphoid (KOPN-30bi, KOPN-55bi, KOPN-46, KOCL-69) were used. The human promyelocytic leukemic cell line HL-60 and T-lymphoid leukemic cell line KOPT-K1 were used throughout the study. Leukemia cells were maintained in suspension culture in RPMI-1640 medium supplemented with 10% FCS and were used for experiments after 3 h-culture in FCS-free D-MEM/F12 medium (GIBCO–BRL, Rockville, MD, USA). To establish HL-60 cell lines resistant to troglitazone, we first cultured HL-60 cells without troglitazone in the FCS-free D-MEM/F12 medium for 1 month, and next added troglitazone in the serum-free culture with stepwise increase in its concentration starting from 0.5 to 2 μg/ml. The mildly resistant cell line was established from cells growing well in the presence of 2 μg/ml of troglitazone. The mildly resistant cell lines was further cultured for more than 6 months with stepwise increase in troglitazone concentration, and the highly resistant cell line was finally established from cells growing well in the presence of 4 μg/ml of troglitazone. Fibroblasts and the preadepocyte cell line 3T3-L1 were also used for comparative analysis of the PPAR γ expression. Differentiated 3T3-L1 cells were obtained from undifferentiated 3T3-L1 cells after 3 day-culture in the presence of FCS, isobutylmethylxanthin, dexamethasone, and insulin as reported.62
Antibodies and reagents
Polyclonal antibodies against PPAR γ, caspase-3, Bax, Bcl-XL, and p38 were purchased from Santa Cruz (Santa Cruz, CA, USA), Pharmingen (San Diego, CA, USA), UBI (Lake Placid, NY, USA), Transduction Laboratories (Suite, Lexinton, KY, USA), and New England Biolabs (Beverely, MA, USA), respectively. Monoclonal antibodies against Fas (CD95; UB2) and Fas ligand (FasL; 4A5) were purchased from MBL (Nagoya, Aichi, Japan); Bcl-2 (124) and phosphotyrosine (4G10) from UBI; c-Myc (Ab-2), α-tubulin (TU-01), JNK1, and β-catenin from Calbiochem (LaJolla, CA, USA), Sanbio (Uden, Netherlands), Pharmingen, and Transduction Laboratories, respectively. Monoclonal antibodies against Tcf-4 (6H5) and Tcf-3/-4 (6F12) were produced and characterized by N Barker MD.63 Cycloheximide (CHX) and propidium iodide (PI) were purchased from Sigma (St. Louis, MO, USA). N-benzyloxycarbonyl-Asp-Glu-Val-Asp-fluoromethylketone (Z-DEVD-FMK) and 15d-PGJ2 were obtained from Kamiya Biomedical (Seattle, WA, USA) and Cayman Chemical (Ann Arbor, MI, USA), respectively. Troglitazone (CS-045) was kindly provided from Sankyo Co. (Tokyo, Japan).64
[3H]-thymidine uptake
Leukemia cells were cultured with or without various concentrations (0–6 μg/ml) of troglitazone in 200 μl of D-MEM/F12 medium in a flat-bottomed 96 well-culture plate (Costar, Cambridge) in triplicate (5×104 cells/well) at 37°C and 5% CO2. At different time points, cells were pulsed with [3H]-thymidine (1 μCi/well) for 4 h, and harvested onto glass-fiber filters. Radioactivity incorporated into DNA was measured using a scintillation counter.
Cell counts
Leukemia cells were cultured 2 days with or without various concentrations (0, 4 and 6 μg/ml) of troglitazone in 200 μl of D-MEM/F12 medium in a flat-bottomed 96-well culture plate in triplicate (5×104 cells/well) at 37°C and 5% CO2. At different hours after culture, numbers of living cells were counted by dye exclusion test.
Cell cycle analysis
Leukemia cells were cultured in D-MEM/F12 medium with or without different concentrations (0, 2, 4 and 6 μg/ml) of troglitazone. The cell cycle analysis was carried out at different exposure times (6, 12 and 24 h). After fixation in 70% ethanol on ice followed by washing with PBS, the cells were stained with 50 μg/ml PI for 20 min and used for analysis. Ten thousand events were analyzed on a FACScaliber flow cytometry (Beckton Dickinson, San Jose, CA, USA). Apoptotic cells were quantified by measuring signals in the hypodiploid region.
Cell morphology
Leukemia cells were cultured in a flat-bottomed 24 well-culture plate (1×105 cells/1 ml/well) in D-MEM/F12 medium in the presence or absence or troglitazone (6 μg/ml). The morphology of the cells was observed on cytospin smears after Wright–Giemsa staining. Apoptotic cells were identified by morphological features characteristic of apoptosis (i.e. cell shrinkage, nuclear condensation, formation of membrane blebs, and apoptotic bodies).
Flow cytometric analysis
Leukemia cells were cultured in D-MEM/F12 medium in the presence or absence of troglitazone (6 μg/ml) for 2 days. At different time points, the cells were washed with PBS three times, and stained with anti-Fas or anti-FasL antibody for 1 h on ice. The cells were then washed, stained with FITC-labeled second antibody, and analyzed on a FACScaliber.
Western blot analysis
Leukemia cells were cultured in D-MEM/F12 medium in the presence or absence of troglitazone (6 μg/ml) at 37°C and 5% CO2, and harvested at different time points. Western blot analysis was performed as described previously.65 Briefly, cells were solubilized in lysis buffer (50 mM Tris-HCl, pH 8.0, containing 1% Nonidet P-40, 150 mM NaCl, 0.05% NaN3, 5 mM EDTA, 1 mM PMSF, 0.2 TIU/ml aprotinin, 1 μg/ml pepstatin A, and 10 mM iodoacetamide) for 30 min on ice. Sodium dodecyl sulphate (SDS) was added to the lysis buffer at a final concentration of 0.1% for analysis of nuclear proteins (PPAR-γ, c-Myc). The cell lysates were separated on a 7.5–12.5% SDS-polyacrylamide gel under reducing conditions, and transferred to nitrocellulose membranes (Schleicher & Schuell, Keene, NH, USA), which were incubated with various primary antibodies overnight at 4°C followed by an incubation with horseradish peroxidase-conjugated second antibody for 1 h at room temperature. The detection of the bands was performed using an enhanced chemiluminescence (ECL) kit (Amersham Japan, Tokyo, Japan).
Analysis of tyrosine phosphorylation
Leukemia cells (1×107/well) were treated with troglitazone (6 μg/ml) in D-MEM/F12 medium and harvested at several time points. The JNK1 or p38 molecule was then immunoprecipitated using anti-JNK1 or p38 antibody and protein A-sepharose beads. The precipitates were eluted by SDS sample buffer, run on a 7.5% SDS-polyacrylamide gel, and transferred to a nitrocellulose membrane. The membrane was incubated with anti-phosphotyrosine antibody (1 μg/ml) overnight at room temperature, and then incubated with horseradish peroxidase-conjugated second antibody for 1 h. The bands were developed using an ECL kit.
Northern blot analysis
Leukemia cells were cultured in D-MEM/F12 medium in the presence or absence of troglitazone (6 μg/ml) in culture flasks at densities of 1×107 cells/ml, and harvested at different time points (1, 3, 6 and 12 h). Total RNA was extracted from cells using a commercial system (RNeasy total RNA kit) obtained from Qiagen (Hilden, Germany). Equal amount of RNA (20 μg) was electrophoresed through a 1% formaldehyde agarose gel and transferred to a nylon membrane (Hybond-N+; Amersham, Buckinghamshire, UK). Hybridization was performed overnight at 42°C with a α-32P-dCTP-labeled 1.4-kb HindIII/XbaI c-myc cDNA probe. After two times of high stringent washes with 0.1×SSC and 0.1% SDS at 42°C for 15 min, the membrane was exposed to a X-ray film (XAR-5 film; Eastman-Kodak, Rochester, NY, USA) with an intensifying screen at −80°C.
Electrophoretic mobility shift assay
Electrophoretic mobility shift assay (EMSA) was done according to the method previously described.66 Binding reactions in the EMSA were performed with a 32P-end-labeled DNA oligonucleotide probe containing the NF-κB consensus (5′-AGTTGAGGGGACTTTCCCAGGC-3′) and the Tcf consensus (5′-CCCTTTGATCTTACC-3′) binding site sequences (the consensus binding sites are underlined). In EMSA for NF-κB, cells were treated with TNF-α (10 ng/ml) for 1 h to activate endogenous NF-κB, and then nuclear extracts were prepared. In the competitive inhibition experiments, 100-fold molar excess of the unlabeled consensus or 1- or 2-bp mismatched oligonucleotide (NF-κB; 5′-AGTTGAGGCGACTTTCCCAGGC-3′, Tcf; 5′-CCCTTTGGCCTTACC-3′) was added to the reaction mixture of nuclear extracts from leukemia cells. The antibody was added to the nuclear extracts and incubated for 30 min prior to the DNA-binding reaction.
Abbreviations
- PPAR:
-
peroxisome proliferator-activated receptor
- Tcf-4:
-
T cell factor-4
- APC:
-
adenomatous polyposis coli
- FCS:
-
fetal calf serum
- EMSA:
-
electrophoretic mobility shift assay
- ECL:
-
enhanced chemiluminescence
References
Mangelsdorf DJ, Thummel C, Beato M, Herrlich P, Schutz G, Umesono K, Blumberg B, Kastner P, Mark M, Chambon P, Evans RM . 1995 The nuclear receptor superfamily: the second decade Cell 83: 835–839
Braissant O, Foufelle F, Scotto C, Dauca M, Wahli W . 1996 Differential expression of peroxisome proliferator activated receptors (PPARs): tissue distribution of PPAR-α, -β, and -γ in adult rat Endocrinology 137: 354–366
Kliewer SA, Forman BM, Blumberg B, Ong ES, Borgmeyer U, Mangelsdorf DJ, Umesomo K, Evans RM . 1994 Differential expression and activation of a family of murine peroxisome proliferator activated receptors Proc. Natl. Acad. Sci. U.S.A. 91: 7355–7359
Lemberger T, Desvergne B, Wahli W . 1996 Peroxisome proliferator-activated receptors: a nuclear receptor signaling pathway in lipid physiology Annu. Rev. Cell Dev. Biol. 12: 335–363
Wahli W, Braissant O, Desvergne B . 1995 Peroxisome proliferator-activated receptors: transcriptional regulator of adipogenesis, lipid metabolism and more Chem. Biol. 2: 261–266
Spiegelman BM, Flier JS . 1996 Adipogenesis and obesity: rounding out the big picture Cell 87: 377–389
Kliewer SA, Lenhard JM, Willson TM, Patel I, Morris DC, Lehmann JM . 1995 A prostaglandin J2 metabolite binds peroxisome proliferator activated receptor and promotes adipocyte differentiation Cell 83: 813–819
Kliewer SA, Umesono K, Noonan DJ, Daniel J, Heyman RA, Evans RM . 1992 Convergence of 9-cis retinoic acid and peroxisome proliferator signalling pathways through heterodimer formation of their receptors Nature 358: 771–774
Dreyer C, Krey G, Keller H, Givel F, Helftenbein G, Wahli W . 1992 Control of the peroxisomal β-oxidation pathway by a novel family of nuclear hormone receptors Cell 68: 879–887
Ijpenberg A, Jeannin E, Wahli W, Desvergne B . 1997 Polarity and specific sequence requirements of peroxisome proliferator-activated receptor (PPAR)/retinoid X receptor heterodimer binding to DNA J. Biol. Chem. 272: 20108–20117
Forman BM, Tontonoz P, Chen J, Brun RP, Spiegelman BM, Evans RM . 1995 15-Deoxy-Δ12,14-prostaglandin J2 is a ligand for the adipocyte determination factor PPAR γ Cell 83: 803–812
Lehmann JM, Moore LB, Smith-Oliver TA, Willson WO, Wilson TM, Kliewer SA . 1995 An antidiabetic thiazolidinedione is a high affinity ligand for peroxisome-proliferated receptor γ (PPAR γ) J. Biol. Chem. 270: 12953–12956
Iwamoto Y, Kuzuya T, Matsuda A, Awata T, Kumakura S, Inooka G, Shiraishi I . 1991 Effect of new oral antidiabetic agent CS-045 on glucose tolerance and insulin secretion in patients with NIDDM Diabetes 14: 1083–1086
Jiang C, Ting AT, Seed B . 1998 PPAR γ agonists inhibit production of monocyte inflammatory cytokines Nature 391: 82–86
Ricote M, Li AC, Willson TM, Kelly CJ, Glass CK . 1998 The peroxisome proliferator-activated receptor-γ is a negative regulator of macrophage Nature 391: 79–82
Auboeuf D, Rieusset J, Fajas L, Vallier P, Frering V, Riou JP, Staels B, Auwerx J, Laville M, Vidal H . 1997 Tissue distribution and quantification of the expression of mRNAs of peroxisome proliferator-activated receptors and liver X receptor-alpha in humans: no alteration in adipose tissue of obese and NIDDM patients Diabetes 46: 1319–1327
Sarraf P, Mueller E, Jones D, King FJ, Deangelo DJ, Partridge JB, Holden SA, Chen LB, Singeer S, Fletcher C, Spiegelman BM . 1998 Differentiation and reversal of malignant changes in colon cancer through PPAR γ Nature Med. 4: 1046–1052
Brian S . 1998 PPAR γ and colorectal carcinoma: conflicts in a nuclear family Nature Med. 4: 1004–1005
Saez E, Tontonoz P, Nelson MC, Alvarez JG, Ming UT, Baird SM, Thomazy VA, Evans RM . 1998 Activators of the nuclear receptor PPAR γ enhance polyp formation Nature Med. 4: 1058–1061
Lefebvre AM, Chen I, Dereumaux P, Najib J, Fruchart JC, Geboes K, Briggs M, Heyman R, Auwerx J . 1998 Activation of the peroxisome proliferator-activated receptor γ promotes the development of colon tumors Nature Med. 4: 1053–1057
Spiegelman BM . 1998 PPAR γ in monocytes: less pain, any gain? Cell 93: 153–155
Green ME, Blumberg B, McBride OW, Yi HF, Kronquist K, Kwan K, Hsieh L, Green G, Nimer SD . 1995 Isolation of the human peroxisome proliferator-activated receptor gamma cDNA: expression in hematopoietic cells and chromosomal mapping Gene Expr. 4: 281–299
Sugiura A, Kiriyama Y, Nochi H, Tsuchiya H, Tamoto K, Sakurada Y, Ui M, Tokumitsu Y . 1999 Troglitazone suppresses cell growth of myeloid leukemia cell lines by induction of p21 WAF1/CIP1 cyclin-dependent kinase inhibitor Biochem. Biophys. Res. Commun. 261: 833–837
Tontonoz P, Nagy L, Alvarez JGA, Thomazy V, Evans RM . 1998 PPAR γ promotes monocyte/macrophage differentiation and uptake of oxidized LDL Cell 93: 241–252
Hirase N, Yanase T, Mu Y, Muta K, Umemura T, Takayanagi R, Nawata H . 1999 Thiazolidinedione induces apoptosis and monocytic differentiation in the promyelocytic leukemia cell line HL60 Oncology 57: 17–26
Chang T, Szabo E . 2000 Induction of differentiation and apoptosis by ligands of peroxisome proliferator-activated receptor γ in non-small cell lung cancer Cancer Res. 60: 1129–1138
Sato H, Ishihara S, Kawashima K, Moriyama N, Suetsugu H, Kazumori H, Okuyama T, Rumi MA, Fukuda R, Nagasue N, Kinoshita Y . 2000 Expression of peroxisome proliferator-activated receptor (PPAR γ) in gastric cancer and inhibitory effects of PPAR γ agonists Br. J. Cancer 83: 1394–1400
Jeffrey AK, Timothy AS, Keith WM, Janine LR, Stewart G, Murray DM . 1999 15-Deoxy-Δ12,14-prostaglandin J2, a ligand for peroxisome proliferator-activated receptor γ, induces apoptosis in JEG3 choriocarcinoma cells Biochem. Biophys. Res. Commun. 262: 579–585
Adams M, Montague CT, Prince JB, Holder JC, Smith SA, Sanders L, Digby JE, Sewter CP, Lazar MA, Chatterjee VK, O'Rahilly S . 1997 Activation of peroxisome proliferator-activated receptor γ have depot-specific effects on human preadipocyte differentiation J. Clin. Invest. 100: 3149–3153
Shao D, Lazar MA . 1997 Peroxisome proliferator activated receptor γ, CCAAT/enhancer-binding protein α, and cell cycle status regulate the commitment to adipocyte differentiation J. Biol. Chem. 272: 21473–21478
Ristow M, Muller-Wieland D, Pfeiffer A, Krone W, Kahn CR . 1998 Obesity associated with a mutation in a genetic regulator of adipocyte differentiation N. Engl. J. Med. 339: 953–959
Hu E, Kim JB, Sarraf P, Spiegelman BM . 1996 Inhibition of adipogenesis through MAP kinase-mediated phosphorylation of PPARγ Science 274: 2100–2103
Li P, Nijhawan D, Budihardjo I, Srinivasula SM, Ahmad M, Alnemri ES, Wang X . 1997 Cytochrome c and dATP-dependent formation of Apaf-1/Caspase-9 complex initiates an apoptotic protease cascade Cell 91: 479–489
Reed JC . 1997 Cytochrome c: Can't live with it- Can't live without it Cell 91: 559–562
Scaffidi C, Fulda S, Srinivasan A, Friesen C, Li F, Tomaselli KJ, Debatin KM, Krammer PH, Peter ME . 1998 Two CD95 (APO-1/Fas) signaling pathways EMBO J. 17: 1675–1687
Holtz-Heppelmann CJ, Algeciras A, Badley AD, Paya CV . 1998 Transcriptional regulation of the human FasL promoter-enhancer region J. Biol. Chem. 273: 4416–4423
Miyasita T, Reed JC . 1995 Tumor suppressor p53 is a direct transcriptional activator of the human bax gene Cell 80: 293–299
Raingeaud J, Gupta S, Rogers JS, Dickens M, Han J, Ulevitch RJ, Davis RJ . 1998 Pro-inflammatory cytokines and environmental stress cause p38 mitogen-activated protein kinase activation by dual phosphorylation on tyrosine and threonine J. Biol. Chem. 273: 4416–4423
Davis RJ . 1994 MAPKs: new JNK expands the group Trends. Biochem. Sci. 19: 470–473
Xia Z, Dickens M, Raingeaud J, Davis RJ, Greenberg ME . 1995 Opposing effects of ERK and JNK-p38 MAP kinases on apoptosis Science 270: 1326–1331
Johnson NL, Gardner AM, Diener KM, Carol A, Carter L, Gleavy J, Jarpe MB, Minden A, Karin M, Zon LI, Johnson GL . 1996 Signal transduction pathways regulated by mitogen-activated/extracellular response kinase kinase kinase induce cell death J. Biol. Chem. 271: 3229–3237
Huang S, Jiang Y, Li Z, Nishida E, Mathias P, Lin S, Ulevitch RJ, Nemerow GR, Han J . 1997 Apoptosis signaling pathway in T cells is composed of ICE/Ced-3 family proteases and MAP kinase kinase 6b Immunity 6: 739–749
Kangas A, Nicholson DW, Holtta E . 1998 Involvement of CPP32/Caspase-3 in c-Myc-induced apoptosis Oncogene 16: 387–398
Wu M, Arsura M, Bellas RE, Fitzgerald MJ, Lee H, Schauer SL, Sherr DH, Sonenshein GE . 1996 Inhibition of c-myc expression induces apoptosis of WEHI 231 murine B cells Mol. Cell. Biol. 16: 5015–5025
Duyao MP, Buckler AJ, Sonenshein GE . 1990 Interaction of an NF-κB-like factor with a site upstream of the c-myc promoter Proc. Natl. Acad. Sci. U.S.A. 87: 4727–4731
Scheinman RI, Gualberto A, Jewell CM, Cidlowsi JA, Baldwin AS . 1995 Characterization of mechanisms involved in transrepression of NF-κB by activated glucocorticoid receptors Mol. Cell. Biol. 15: 943–953
Wang Y, Jhang JJ, Dai W, Lei KY, Pike JW . 1997 Dexamethasone potently enhances phorbol ester-induced IL-1β gene and nuclear factor NF-κB activation J. Immunol. 159: 534–537
He TC, Sparks AB, Rago C, Hermeking H, Zawel L, da Costa LT, Morin PJ, Vogelstein B, Kinzler KW . 1998 Identification of c-Myc as a target of the APC pathway Science 281: 1509–1512
Henriksson M, Luscher B . 1996 Proteins of the Myc network: essential regulators of cell growth and differentiation Adv. Cancer Res. 68: 109–182
Kretzner L, Blackwood EM, Eisenman RN . 1992 Myc and Max proteins possess distinct transcriptional activities Nature 359: 426–429
Askew DS, Ashmun RA, Simmons BC, Cleveland JL . 1991 Constitutive c-myc expression in an IL-3-dependent myeloid cell line suppressed cell cycle arrest and accelerates apoptosis Oncogene 6: 1915–1922
Evan GI, Wyllie AH, Gilbert CS, Littlewood TD, Land H, Brooks M, Waters CM, Penn LZ, Hancock DC . 1992 Induction of apoptosis in fibroblasts by c-myc protein Cell 69: 119–128
Shi Y, Glynn JM, Guilbert LJ, Cotter TG, Bissonnette RP, Green DR . 1992 Role of c-myc in activation-induced apoptotic cell death in T cell hybridomas Science 257: 212–214
Thulasi R, Harbour D, Thompson EB . 1993 Suppression of c-myc is a critical step in glucocorticoid-induced human leukemic cell lysis J. Biol. Chem. 268: 18306–18312
Kimura S, Maekawa T, Hirakawa K, Murakami A, Abe T . 1995 Alterations of c-myc expression by antisense oligodeoxynucleotides enhance the induction of apoptosis in HL-60 cells Cancer Res. 55: 1379–1384
Helmberg A, Auphan N, Caelles C, Karin M . 1995 Glucocorticoid-induced apoptosis of human leukemic cells is caused by the repressive function of the glucocorticoid receptor EMBO J. 14: 452–460
Chinetti G, Griglio S, Antonucci M, Torra IP, Delerive P, Majd Z, Fruchart JC, Chapman J, Najib J, Staels B . 1998 Activation of proliferator-activated receptors α and γ induces apoptosis of human monocyte-derived macrophages J. Biol. Chem. 273: 25573–25580
Zhang MY, Sun SC, Bell L, Miller BA . 1998 NF-κB transcription factors are involved in normal erythropoiesis Blood 91: 4136–4144
Korinek V, Barker N, Morin PJ, Wichen D, Weger R, Kinzler KW, Vogelstein B, Clevers H . 1996 Constitutive transcriptional activation by a β-catenin-Tcf complex in APC−/− colon carcinoma Science 275: 1784–1787
Kubota T, Koshizuka K, Williamson EA, Asou H, Said JW, Holden S, Miyoshi I, Koffler HP . 1998 Ligand for peroxisome proliferator-activated receptor γ (troglitazone) has potent antitumor effect against human prostate cancer both in vitro and in vivo Cancer Res. 58: 3344–3352
Xin X, Yang S, Kowalski J, Gerritsen ME . 1999 Peroxisome proliferator-activated receptor-γ ligands are potent inhibitors of angiogenesis in vitro and in vivo J. Biol. Chem. 274: 9116–9121
McGehee RE, Ron D, Brasier AR, Habener JF . 1993 Differentiation-specific element: a cis-acting developmental switch required for the sustained transcriptional expression of the angiotensinogen gene during hormonal-induced differentiation of 3T3-L1 fibroblasts to adipocytes Mol. Endocrinol. 7: 551–560
Barker N, Huls G, Korinek V, Clevers H . 1999 Restricted high level expression of Tcf-4 protein in intestinal and mammary gland epithelium Am. J. Pathol. 154: 29–35
Fujiwara T, Yoshioka S, Yoshioka T, Ushiyama I, Horikoshi H . 1988 Characterization of new oral antidiabetic agent CS-045. Studies in KK and ob/ob mice and zucker fatty rats Diabetes 37: 1549–1558
Kojika S, Sugita K, Inukai T, Saito M, Iijima K, Tezuka T, Goi K, Shiraishi K, Mori T, Okazaki T, Kagami K, Ohyama K, Nakazawa S . 1996 Mechanisms of glucocorticoid resistance in human leukemic cells; implication of abnormal 90 and 70 kDa heat shock proteins Leukemia 10: 994–999
Inukai T, Inaba T, Yoshihara T, Look AT . 1997 Cell transformation mediated by homodimeric E2A-HLF transcription factors Mol. Cell. Biol. 17: 1417–1424
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by M Naito
Rights and permissions
About this article
Cite this article
Yamakawa-Karakida, N., Sugita, K., Inukai, T. et al. Ligand activation of peroxisome proliferator-activated receptor γ induces apoptosis of leukemia cells by down-regulating the c-myc gene expression via blockade of the Tcf-4 activity. Cell Death Differ 9, 513–526 (2002). https://doi.org/10.1038/sj.cdd.4401000
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401000
Keywords
This article is cited by
-
Identifying Genetic Signatures Associated with Oncogene-Induced Replication Stress in Osteosarcoma and Screening for Potential Targeted Drugs
Biochemical Genetics (2023)
-
T cell factor-4 functions as a co-activator to promote NF-κB-dependent MMP-15 expression in lung carcinoma cells
Scientific Reports (2016)
-
Expression of Peroxisome Proliferator Activated Receptor-Gamma (PPAR-γ) in Human Non-small Cell Lung Carcinoma: Correlation with Clinicopathological Parameters, Proliferation and Apoptosis Related Molecules and Patients’ Survival
Pathology & Oncology Research (2012)
-
Transcription profiling of lung adenocarcinomas of c-myc-transgenic mice: Identification of the c-myc regulatory gene network
BMC Systems Biology (2008)
-
Ciglitazone Induces Caspase-Independent Apoptosis through Down-Regulation of XIAP and Survivin in Human Glioma Cells
Neurochemical Research (2008)