Abstract
Combined dopamine D2 receptor antagonism and serotonin (5-HT)1A receptor agonism may improve efficacy and alleviate some side effects associated with classical antipsychotics. The present study describes the in vitro and in vivo characterization of 1-(2,3-dihydro-benzo[1,4]dioxin-5-yl)-4-[5-(4-fluoro-phenyl)-pyridin-3-ylmethyl]-piperazine monohydrochloride (SLV313), a D2/3 antagonist and 5-HT1A agonist. SLV313 possessed high affinity at human recombinant D2, D3, D4, 5-HT2B, and 5-HT1A receptors, moderate affinity at 5-HT7 and weak affinity at 5-HT2A receptors, with little-no affinity at 5-HT4, 5-HT6, α1, and α2 (rat), H1 (guinea pig), M1, M4, 5-HT3 receptors, and the 5-HT transporter. SLV313 had full agonist activity at cloned h5-HT1A receptors (pEC50=9.0) and full antagonist activity at hD2 (pA2=9.3) and hD3 (pA2=8.9) receptors. In vivo, SLV313 antagonized apomorphine-induced climbing and induced 5-HT1A syndrome behaviors and hypothermia, the latter behaviors being antagonized by the 5-HT1A antagonist WAY100635. In a drug discrimination procedure SLV313 induced full generalization to the training drug flesinoxan and was also antagonized by WAY100635. In the nucleus accumbens SLV313 reduced extracellular 5-HT and increased dopamine levels in the same dose range. Acetylcholine and dopamine were elevated in the hippocampus and mPFCx, the latter antagonized by WAY100635, suggesting possible 5-HT1A-dependent efficacy for the treatment of cognitive and attentional processes. SLV313 did not possess cataleptogenic potential (up to 60 mg/kg p.o.). The number of spontaneously active dopamine cells in the ventral tegmental area was reduced by SLV313 and clozapine, while no such changes were seen in the substantia nigra zona compacta following chronic administration. These results suggest that SLV313 is a full 5-HT1A receptor agonist and full D2/3 receptor antagonist possessing characteristics of an atypical antipsychotic, representing a potential novel treatment for schizophrenia.
Similar content being viewed by others
INTRODUCTION
Schizophrenia is characterized by the expression of a variety of symptomatologies such as negative symptoms (affective flattening, social withdrawal, anhedonia, and poverty of thought and content of speech), positive symptoms (delusions, hallucinations, and conceptual disorganization), disruptions of cognitive processing and mood disorders (eg Meltzer, 1999). For many years, the typical antipsychotic agents, for example haloperidol and chlorpromazine, were the most widely used drugs for the treatment of schizophrenia. However, the development of neurological side effects (dystonia, muscle rigidity, tremor and akathisia, and tardive dyskinesia) or extrapyramidal side effects (EPS) are often treatment limiting (Casey, 1996; Seeman et al, 1976). Atypical antipsychotics, such as clozapine, olanzapine, ziprasidone, quetiapine, and more recently aripiprazole have been developed for the combination of reduced EPS liability and the ability to treat, for example, negative symptoms.
Many atypical antipsychotics have interactions with serotonergic receptors and it has been suggested that serotonergic actions are important not only in increasing treatment efficacy but also in reducing EPS. While the serotonin 5-HT2A receptor may play a role in mediating the reduction in EPS observed with atypical antipsychotics (Meltzer, 1999) efficacy at 5-HT1A receptors might also be beneficial (for reviews see Millan, 2000; Meltzer et al, 2003). Interestingly, in the schizophrenic brain 5-HT1A receptor binding is altered in the hippocampus, cortex, and amygdala (Burnet et al, 1996; Gurevich and Joyce, 1997; Bantick et al, 2001; Yasuno et al, 2004). Atypical antipsychotics such as clozapine, ziprasidone, aripiprazole, and quetiapine are all 5-HT1A (partial) agonists; which may be very relevant for their actions in treating schizophrenia (Newman-Tancredi et al, 1996, 2001; Sprouse et al, 1999; Rollema et al, 2000; Jordan et al, 2002). For example, in the conditioned avoidance response (CAR) model of schizophrenia the nonselective 5-HT1A agonist (±)-8-hydroxy(di-n-aminopropylamino) tetralin (8-OH-DPAT) not only induced CAR disruption but enhanced the effects of the dopamine D2 receptor antagonists haloperidol and raclopride (Wadenberg and Ahlenius, 1991; Prinssen et al, 1996). Rather than increasing EPS the 5-HT1A agonists 8-OHDPAT and ipsapirone reduced EPS-like symptoms in rodents and non-human primates (Prinssen et al, 1999, 2000; Wadenberg and Ahlenius, 1991; Wadenberg, 1996; Wadenberg et al, 1999; Christoffersen and Meltzer, 1998). These preclinical studies are supported by the finding that buspirone and tandospirone attenuated Parkinsonian-like signs and tardive dyskinesia seen in schizophrenics (Goff et al, 1991; Yoshida et al, 1998). Together these data support the concept that mixed 5-HT1A agonistic/dopamine D2-like receptor antagonistic effects could be beneficial for the treatment of schizophrenia.
Additional evidence suggests that a variety of atypical antipsychotics produce a 5-HT1A-dependent and preferential increase of dopamine levels in the medial prefrontal cortex (mPFCx; an area thought to have reduced dopaminergic tone in schizophrenics (Weinberger and Lipska, 1995)) vs dorsal striatum (Moghaddam and Bunney, 1990; Nomikos et al, 1994; Pehek et al, 1993; Hertel et al, 1996; Ichikawa et al, 2001; Rollema et al, 1997, 2000). In addition, atypical antipsychotics, also via 5-HT1A receptor-dependent mechanisms, augment acetylcholine (ACh) neurotransmission in the mPFCx which should enhance cognitive function (Ichikawa et al, 2002a, 2002b). Furthermore, actions on both dopamine and ACh at the level of the hippocampus (important for declarative (storage) memory and pivotally affected in schizophrenia (Eichenbaum et al, 1999; Fernandez et al, 2002; Seidman et al, 2002)) were both augmented by clozapine, olanzapine, risperidone, and ziprasidone (Shirazi-Southall et al, 2002; Chung et al, 2004). These effects were sensitive to manipulation with 5-HT1A receptor antagonists (eg Li et al, 2004). Clinical effects of the atypical antipsychotics to improve long-term memory deficits in schizophrenic patients have been demonstrated (Meltzer and McGurk, 1999; Harvey and Keefe, 2001). As such, if the preclinical work can be extrapolated to the human, the effects seen in microdialysis studies suggest, at least in part, that cognitive enhancement with atypical antipsychotics could be due to increases in hippocampal dopamine and ACh. Interestingly, the (partial) 5-HT1A agonist tandospirone improved cognition in schizophrenic patients (Sumiyoshi et al, 2001a, 2001b). It is therefore relevant to further test the hypothesis that novel putative antipsychotics increase mPFCx and hippocampal dopamine and ACh. Compounds that have mixed D2 and 5-HT1A receptor moieties are of special interest.
In summary, it appears that the therapeutic window, side-effect profile and therapeutic efficacy of antipsychotic agents could be improved by the combination of a dopamine D2 receptor antagonist with 5-HT1A receptor agonist properties. Combination approaches with different medications are possible, but not desirable for reasons including issues relating to pharmacokinetics and patient compliance. The obvious choice is to synthesize and develop a single chemical entity. In the present study, we describe the pharmacological characterization of the novel putative antipsychotic agent 1-(2,3-dihydro-benzo[1,4]dioxin-5-yl)-4-[5-(4-fluoro-phenyl)-pyridin-3-ylmethyl]-piperazine monohydrochloride (SLV313; Figure 1), using in vitro and in vivo assays.
METHODS
Receptor Binding
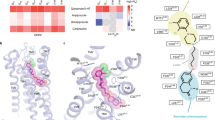
SLV313 was tested for the ability to bind to recombinant receptors expressed in cell systems or receptors sourced from native tissue (rat and guinea pig). The receptor-binding assays were performed at CEREP (Celle l'Evescault, France) using the conditions outlined in Table 1. Following incubation, the receptor preparations were rapidly filtered under vacuum through glass fiber filters which were washed with ice-cold buffer using a harvester. Bound radioactivity was measured by scintillation counting using a liquid scintillation cocktail. Compounds were tested at three logarithm unit concentrations; all determinations were performed as triplicates. IC50 values were determined by nonlinear regression analysis using Hill equation curve fitting and inhibition constants (Ki) calculated using the Cheng–Preushoff equation Ki=IC50/(1+L/Kd), where L is the concentration of radioligand in the assay and Kd the affinity of the radioligand for the receptor. Results are expressed as mean pKi±SD of at least three separate experiments. The expression of no significant inhibition of radioligand binding at concentrations of 1 μM and higher were concluded to be inactive.
In Vitro Functional Activity
Experiments assessing the D2,L and 5-HT1A receptor functional activity in vitro were performed in CHO-K1 cells transfected with either the human D2,L receptor (obtained from Dr D Grandy, Vollum Institute Oregon, USA; Bunzow et al, 1988) or the human 5-HT1A receptor (Allelix Biopharmaceuticals, Mississauga, ON, Canada; Fargin et al, 1989). Confluent cultures were grown in 24 well plates in DMEM medium supplemented with 10% heat-inactivated fetal calf serum, 2 mM glutamine, 1 mM pyruvate, 5000 U/ml penicillin, 5000 μg/ml streptomycin, and 200 μg/ml G418 at 37°C in a 93% air/7% CO2 mixture. Cells were loaded with 1 μCi [3H] adenine in 0.5 ml/well for 120 min and washed with 0.5 ml phosphate-buffered saline (PBS) containing 1 mM IBMX and incubated for 20 min with 0.5 ml PBS containing 1 mM IBMX and forskolin with or without test compound. After aspiration, the reaction was stopped with 1 ml trichloracetic acid. The [3H]ATP and [3H]cAMP formed in the cellular extract was assayed as previously reported (Salomon et al, 1974; Weiss et al, 1985). Briefly, 0.8 ml of extract was passed over Dowex (50WX-4 200–400 mesh) and aluminium oxide columns eluted with water and 0.1 M imidazole (pH=7.5). Eluates were mixed with 7 ml insta-gel and radioactivity counted with a liquid scintillation counter. The conversion of [3H]ATP to [3H]cAMP was expressed as the ratio of percentage radioactivity in the cAMP and ATP fractions. Basal activity was subtracted to correct for spontaneous activity. Dopamine D2,L-transfected cells were incubated in the presence of quinpirole (10−6 M) with the addition of SLV313. Similarly, CHO cells transfected with the 5-HT1A receptor were incubated in the presence of SLV313. In addition, the 5-HT1A agonist 8-OHDPAT was tested for comparative purposes. All studies were performed in quadruplicate.
Functional activity at the D3 receptor was assessed using a GTPγS assay (Newman-Tancredi et al, 1999) at MDS-PS Laboratories (Taipei, Taiwan). Human recombinant dopamine D3 receptors were expressed in CHO-K1 cells. SLV313 (dissolved in DMSO) was preincubated in triplicates with the 40 μg/ml receptors and 1 μM GDP in HEPES buffer (20 mM HEPES, pH 7.4, 100 mM NaCl, 10 mM MgCl2, 1 mM DTT, 1 mM EDTA) for 20 min at 30°C, scintillation proximity assay beads were then added for another 60 min. Ligand displacement was initiated by 0.3 nM [35S]GTPγS for an additional 30 min incubation period. Agonistic effects were expressed as percentage of that of control of dopamine (0.3 μM) was used as the positive control; antagonistic effects of SLV313 were determined by assessing inhibition of 0.3 μM dopamine-induced [35S]GTPγS binding and the pA2 was calculated according to Cheng–Preushoff equation (above). Three independent experiments were performed.
In Vivo Activity
All animals used in the present studies were housed in a temperature (20±2°C) and humidity-controlled environment under a 12-h light-dark cycle (lights on 0700–1900 h). The a priori significance levels was set at p<0.05 for all experiments to assess significant differences from control.
All experimental procedures conformed to local animal care and use committee stipulations.
Antagonism of Apomorphine-Induced Climbing
Male NMRI mice (25–30 g; Charles River, Sulzfeld, Germany n=10) were habituated to a wire-mesh cage 60 min prior to apomorphine (1 mg/kg s.c.; Sigma, St Louis, MO, USA) administration. Vehicle (1% methylcellulose 10 ml/kg; Sigma), SLV313 (0, 0.1, 0.3, 0.6, 1, or 3 mg/kg p.o.), or haloperidol (0.03, 0.1, 0.3, or 1 mg/kg p.o.; Siegfried, Zofingen, Switzerland) were administered 60 min prior to apomorphine (s.c.). In addition, SLV313 (0.3, 1, and 3 mg/kg p.o.) was given 4 h prior to the administration of apomorphine to assess the longevity of the effect. At 10 and 20 min after apomorphine administration the climbing behavior of the mice was scored using an arbitrary rating scale (0: no climbing, 1: standing on hind-paws, and 2: climbing).
Behavioral scores were summed and ED50 values were calculated from the percentage inhibition of climbing intensity of vehicle-treated mice by logistic regression analysis of the resulting dose–response curve. Fieller's method was used to determine 95% confidence intervals of the ED50 in comparison to the control. The mean response for each dose is expressed as percentage relative to control together with a 95% confidence interval. A dose was defined to differ significantly from control when the 95% confidence interval did not cover the 100% level of the control group. The lowest dose of a compound that was statistically significant was defined as the minimal effective dose (MED). SAS was used for statistical analyses.
5-HT1A Receptor-Mediated Syndrome Behavior
Male Wistar rats (180–230 g; Harlan, Zeist, the Netherlands, n=8 per group) were used in these studies. Vehicle (1% methylcellulose vehicle; 2 ml/kg p.o.), SLV313 (1, 3, and 10 mg/kg p.o.), aripiprazole (Solvay Pharmaceuticals, the Netherlands; 3, 10, and 30 mg/kg p.o.), clozapine (10 mg/kg p.o.), and ziprasidone (Solvay Pharmaceuticals; 10 mg/kg p.o.) were administered and the intensity of flat body posture (FBP), hind limb abduction (HLA), forepaw treading (FPT), and lower lip retraction (LLR) were scored every 10 min 10–60 min after the administration of compound (0=absent, 1=present, and 2=intense) and the intensities were summed across each of the six time epochs (see Berendsen et al, 1989; Tricklebank et al, 1984). In addition, the ability of SLV313 to induce hypothermia (cf. Bill et al, 1991) was assessed by measuring the oral temperature prior to and at the end of the period of behavioral observation. In order to verify that the effects of SLV313 was caused by putative agonist actions at the 5-HT1A receptor, the selective 5-HT1A receptor antagonist N-(2-(4-(2-methoxyphenyl)-1-piperzinyl)ethyl)-N-(2-pyridinyl)cyclohexanecarboxamide; WAY100635; 0.03, 0.1, and 0.3 mg/kg s.c.; Solvay Pharmaceuticals) or vehicle were administered 30 min prior to SLV313 (6 mg/kg p.o.) and behavior and hypothermia were assessed as described above.
Temperature data were analyzed by a one-way analysis of variance (1-way ANOVA) with post hoc Dunnett's test as appropriate and serotonergic syndrome behaviors were analysed using the nonparametric Kruskall–Wallis with post hoc Mann–Whitney test using JMP software (SAS Institute, USA).
Flesinoxan-Induced Drug Discrimination
Pigeons (Utrecht University, Department of Veterinary Sciences, the Netherlands, n=12) were maintained at approximately 85% free feeding weights by postsessional feeding with standard pigeon grain with water and grit available ad libitum, except during behavioral testing.
The apparatus and procedure have been described in detail elsewhere (see Mos et al, 1997, for full description). Briefly, experiments were conducted in eight standard Le High Valley three-key pigeon chambers, with only the left and the right key being used. Subjects were trained to discriminate flesinoxan from vehicle on a standard fixed ratio (FR) 30 food reinforced schedule of reinforcement. During training sessions, flesinoxan (Solvay Pharmaceuticals; 0.25 mg/kg p.o., (A)) or vehicle (B) were administered 45 min prior to behavioral sessions. Daily session followed a 10-day repeating (ABAABBABBA) schedule.
Test sessions
Test sessions were interspersed between training sessions. The key receiving the first 30 pecks was designated as the ‘to-be-rewarded-key’ for each individual subject for the rest of that particular test session. A 5 s time out was presented for each peck on the nonselected key after the presentation of the first reinforcement. Test sessions ended after 20 min or 40 reinforcements or if the subject did not respond at all after 5 min, whichever came first. Test sessions were given on Wednesday and Friday, but only if the subject's response to first reinforcement (FRF-value) on three immediately preceding training sessions did not exceed 39. In the latter case, the test session was postponed until accuracy was achieved. Each test dose was given once, unless the FRF-value during the test session exceeded 39.
Generalization and antagonist tests
SLV313 (0.01, 0.03, 0.1, and 0.3 mg/kg p.o.) and haloperidol (0.1, 0.3, and 1.0 mg/kg p.o.) were tested for their ability to generalize for the flesinoxan appropriate key. The ability of WAY100635 (0.1, 0.3, and 1 mg/kg p.o.) to attenuate SLV313-induced substitution was also tested. In addition, in an antagonist test the effects of haloperidol on the training dose of flesinoxan were assessed. Flesinoxan (0.25 mg/kg) and compounds used in generalization studies were administered 45 min prior to the experimental session. In antagonism studies, the test drug was administered 15 min prior to administration of the ‘agonist,’ or 60 min prior to the session. All doses were tested in random order. Drugs were suspended in methylcellulose (1% w/v) and injected orally into the crop in a volume of 1 ml/kg.
Data analyses
The percentage of subjects selecting the flesinoxan-appropriate key was taken as a measure of generalization and full generalization was defined as at least 80% of all subjects selected the flesinoxan-associated key, conversely antagonism was defined when <20% of the pigeons failed to respond on the flesinoxan-appropriate key. ED50 values with 95% confidence limits were calculated using logistic analysis. Response rates were calculated to be the number of keypecks per second until the delivery of the first reinforcement. Control measures were taken from the last three training sessions when flesinoxan was administered. Differences between control values and response rates on test sessions were analyzed using Student's t-test (two tailed) using the previous training session as the control.
The Effect of SLV313 on Catalepsy
Male Wistar rats (180–230 g; Harlan, Zeist, the Netherlands, n=8 per group) were individually housed and habituated to the test room. The rats were treated with vehicle (1% tragacanth; 2 ml/kg p.o.), SLV313 (20 and 60 mg/kg p.o.), or haloperidol (1, 2, 4, or 8 mg/kg p.o.) 4 h before placing their front paws on a 15 cm high bar. The latency to remove their paws was recorded. In addition, an arbitrary definition was used which defined the animals as cataleptic if they maintained their positions for longer than 30 s without the loss of the righting reflex.
Data analyses
Latency and incidence (n/N) data were compared using the nonparametric Kruskall–Wallis test with a post hoc Wilcoxon test, using JMP statistical software.
In Vivo Microdialysis Studies
Effect of SLV313 in the nucleus accumbens
Male Wistar rats (275–350 g; Harlan, Zeist, the Netherlands; n=3–6 per dose) were anesthetized with halothane (1.5% halothane in NO2/O2 2 : 1). Baytril (150 μl/rat s.c.; Bayer) and Temgesic (50 μl/rat i.m.; Reckitt and Colman) were injected to prevent infection and induce postoperative analgesia, respectively. Rats were mounted in a stereotaxic instrument (David Kopf Instruments, CA, USA), the scalp incised and a hole was drilled over the anterior part of the nucleus accumbens and guide cannulae (CMA 12, Carnegie Medicine, Sweden) implanted: A: +10.3 (relative to the interaural line); M (relative to midline): −1.4; V (relative to the skull surface): 4.5 mm, (Paxinos and Watson, 1998).
At least 7 days after surgery microdialysis probes (CMA12, 2 mm) were inserted into the guide cannulae the evening before the experiment and perfused with an osmotically balanced Ringers solution containing: 147 mM NaCl, 4 mM KCl, 1.2 mM CaCl2, and 0.7 mM MgCl2 at a flow rate of 1.2 μl/min. On the day of the experiment, 20 min samples were collected into a vial containing 50 μl of formic acid/cysteine solution (0.02 M/0.2% w/v) was present in the collecting vial to prevent oxidation of dopamine. After the first five baseline samples, SLV313 (0.1, 0.3, 1, 3, and 10 mg/kg p.o.; 2 ml/kg p.o.) was administered and dialysate samples collected. Resulting samples were frozen on dry ice and stored at −80°C until later off-line analysis with high-performance liquid chromatography (HPLC) linked to electrochemical detection.
HPLC
Dialysis samples were analyzed with HPLC using electrochemical detection and employing a reversed phase column (Supelcosil LC-8DB, 25 × 4.6 mm2, dp=5 μm, Supelco), maintained at 45°C, a cooled Gilson autoinjector (model 232; 10°C) and diluter (model 401) and a Hewlett Packard (model 1050) pump operating at a flow rate of 1 ml/min. The mobile phase consisted of 50 mM acetic acid, sodium acetate (3 : 1), 1.46 mM HSA, 0.27 mM EDTA, and 16% (v/v) methanol. The final pH was adjusted to 4.9 with 1N NaOH. Dopamine, 3,4-dihydroxyphenyl acetic acid (DOPAC) and homovanilliuc acid (HVA), 5-HT, and 5-hyroxyindoleacetic acid (5-HIAA) were electrochemically detected with an EG&G (model 400, Princeton Applied Research) controller equipped with a glassy carbon working electrode (Antec cell, VT-03, Leiden, the Netherlands). The potential was set at 600 mV vs an Ag/AgCl reference electrode. The output was recorded on a Hewlett Packard (model 3396A) integrator. Calculations (pg/20 min) were made using peak height values of known concentrations of the components previously tested with the apparatus. All reagents used were high standard or HPLC grade.
Data analyses
Mean predrug baseline level were designated as 100% and evaluation of the area under the curve (AUC) for 120 min following drug administration, compared to basal dialysate levels (% AUC120) was performed to provide a readily visible index for the dose–response relationship. Statistical comparisons were performed with ANOVA and post hoc Bonferonni t-testing using SAS software.
Effect of SLV313 in the prefrontal cortex and hippocampus
Male Sprague–Dawley rats (250–350 g; Zivic-Miller Laboratories, Porterville, PA, USA) as described previously (Ichikawa et al, 2001, 2002b) were used in this study. Cannulae were implanted in the mPFCx and hippocampus (coordinates: A: +3.5, L: +1.2 (10° inclination), V: −5.5 mm, and A: +5.6, L: +5.0, V: −7.0 mm, respectively, relative to bregma; Paxinos and Watson, 1998) and 3–5 days after cannulation, microdialysis probes (polyacrylonitrile/sodium methalylsulfonate polymer, 310 μm o.d., 220 μm i.d., 40 kDa cutoff with 3 mm exposed membrane, AN69HF, Hospal; CGH Medical, Lakewood, CO) were inserted into the mPFCx or hippocampus following light isoflurane-induced anesthesia (induced by placement in an isoflurane-enriched environment and performed during a short 2 min sleep period). Experiments were conducted the following day after an overnight perfusion of Dulbecco's PBS solution (Sigma) including Ca2+: (138 mM NaCl, 8.1 mM Na2HPO4, 2.7 mM KCl, 1.5 mM KH2PO4, 0.5 mM MgCl, 1.2 mM CaCl2 at a pH of 7.4 using a flow rate of 0.4 μl/min). The flow rate was then increased to 1.5 μl/min for the experimental procedures. After stable baseline dialysates were obtained, vehicle or SLV313 (3, 10, and 20 mg/kg p.o.) was administered to the rats and 30 min dialysate samples collected for 210 min from either the hippocampus or mPFCx. In order to assess the role of 5-HT1A receptors, following basal dialysate sample collection, as described above, the rats were pretreated with vehicle or WAY100635 (0.2 mg/kg s.c.) and 30 min later with vehicle or SLV313 (10 mg/kg p.o.).
Determination of dopamine
Dialysate samples were directly applied onto an HPLC with electrochemical detection and analyzed with a Millennium chromatogram manager (Waters, Milford, MA, USA). Dopamine was separated (BDS Hypersil 3 μm C18, 1.0 × 100 mm2; Keystone Scientific, Bellefonte, PA, USA) at 35°C maintained by column heater (LC-22C Temperature Controller; BAS, West Lafayette, IN, USA). The mobile phase consisted of 48 mM anhydrous citric acid and 24 mM sodium acetate trihydrate containing 0.5 mM EDTA-Na2, 10 mM NaCl, 2 mM dodecyl sulfate sodium salt, and 17% (v/v) acetonitrile, adjusted to pH 4.8 with concentrated NaOH and the flow rate was 0.05 ml/min (LC-10AD; Shimadzu, Kyoto, Japan). A unijet working electrode (MF-1003, BAS) was set at +0.58 V (LC-4C, BAS) vs an Ag/AgCl reference electrode. Reagents used were analytical or HPLC grade.
Determination of ACh
The method has been described previously in detail (Ichikawa et al, 2002b). Briefly, dialysate samples were directly injected onto the liquid chromatography/electrochemistry system assisted by a chromatography manager (Millennium; Waters, Milford, MA, USA), and analyzed for ACh. ACh was separated on a coiled cation exchanger ACh column (analytical column; Sepstik 10 m ID 530°C 1.0 nm; BAS, West Lafayette, IN), followed by the postimmobilized enzyme reactor (IMER; BAS) which consisted of choline oxidase (ChO)/AChesterase. ACh is hydrolyzed by AChesterase to form acetate and choline in the post-IMER, and then choline is oxidized by ChO to produce betaine and hydrogen peroxide (H2O2). H2O2 was detected and reduced to H2O on an Unijet amperometric detector cell with a peroxidase-redox-coated glassy carbon electrode (MF-9080; BAS), set at +100 mV (LC–4C; BAS) vs Ag/AgCl reference electrode. This reduction was analyzed with the detector (LC–4C; BAS) indicating ACh in the chromatogram.
Data analyses
Mean predrug baseline levels were designated as 100% and AUC120 values were calculated. Following a significant overall repeated measures ANOVA (treatment × time), Fisher's-protected least significant difference post hoc pair-wise comparison and one-way ANOVA were used to determine group differences (StatView7 4.5. for the Macintosh).
The Effect of Chronic Administration of SLV313 on the Number of Spontaneously Active Ventral Tegmental Area (VTA) and Substantia Nigra Zona Compacta (SNC) Neurons
Male Sprague–Dawley rats (150–175 g at the start of the study, Taconic Farms, NY, USA) were treated with vehicle (1% methylcellulose, Sigma; 1 ml/kg), clozapine (20 mg/kg p.o., Tocris-Cookson, St Louis, MO, USA) or SLV313 (3 and 10 mg/kg p.o.). All compounds or vehicle were given once daily for 21 days with the experimenter blinded to treatment. The number of spontaneously active SNC and VTA dopamine neurons were determined 2 h after the final administration on day 21.
Animals were anesthetized with chloral hydrate (400 mg/kg i.p., Sigma), mounted in a stereotaxic instrument (David Kopf), placed on a heating pad (Finitronics, CT, USA) to maintain constant body temperature of 37–38°C and the lateral tail vein cannulated with a 25-gauge needle for the administration of supplemental anesthetic. The scalp was incised and a hole drilled over the SNC (anterior 3.0–3.5 mm to the lambda, lateral 1.8–2.5 mm to the midline and 6.0–8.5 mm ventral to the cortical surface) and VTA (anterior 3.0–3.5 mm, lateral 0.5–1.0 mm and ventral 6.0–8.5 mm; Paxinos and Watson, 1998).
Single barrel microelectrodes (glass borosilicate; WPI, FL, USA with a carbon filament and filled with 2 M NaCl and saturated 1% fast green (Sigma Chemical Co., USA)) pulled with an electrode puller (Narishige PE-2, Japan) and the tip broken back under a light microscope were used for recording single cellular dopamine activity. Impedances were in the range of 0.8–1.2 MΩ measured at 135 Hz in vitro and 1.5–2.0 MΩ in vivo.
The electrodes were passed through the SNC and VTA areas in a systematic manner 10 times using a hydraulic microdrive (David Kopf, Model 640). The electrode tracks were performed in a preset sequence kept constant from animal to animal. For half of the rats in each group, the order of recording was SNC–VTA and the order was reversed for the other rats. The number of spontaneously active dopamine neurons was determined in 10 stereotaxic electrode descents or tracks as previously described (White and Wang, 1983; Chiodo, 1988). Briefly, recordings from 10 electrode tracks (separated by 200 μm) with a constant sequence from animal to animal were performed. Each electrode descent was made in a slow, uniform speed (1–3 μm/s) using the microdrive. Only those cells whose electrophysiological profile matched those previously established for midbrain dopamine cells were counted. During the recording sessions, neurons encountered were considered dopaminergic if they had a wide action potential, with a distinct initial segment, late positive component and a characteristic low-pitch sound when monitored via an audioamplifier; a slow regular or bursting firing pattern and a spontaneous firing rate of 2–9 Hz (White and Wang, 1983). Data were analyzed using a one-way ANOVA and post hoc Student–Newman–Keuls test as necessary.
Histology
At the end of each experiments, a 25 μA cathodal current (Finitronics cathodal current source, Model VL-1200D) was passed through the recording electrode for 15 min, to deposit fast green dye in the brain. Animals were overdosed with chloral hydrate (i.v.) and perfused transcardially with 10% buffered formalin (VWR Scientific, Bridgeport, NJ, USA) for 10 min. The brains were removed and serial coronal sections (50 μm) were made using a cryostat at −20°C, stained with cresyl violet and counterstained with neutral red. The dye spot was viewed under a light microscope and served as a reference point for the location of each cell. Only data were used from animals with electrode placements in the SNC and VTA.
RESULTS
Receptor Binding Profile
SLV313 binds with high affinity to the serotonin 5-HT1A receptor (pKi 9.1), the dopamine D2-like receptors (D2, D3, and D4 receptors (pKis of 8.4, 8.4, and 8.0, respectively) and serotonin 5-HT2B receptors (Table 2). Furthermore, SLV313 had moderate affinity for the serotonin 5-HT7 receptor (pKi 7.2), some affintity for serotonin 5-HT2A receptors (pKi 6.6) and adrenergic α1 receptors (pKi 6.3). SLV313 showed no appreciable affinity for a series of other monoamine sites (pKi <6), including serotonin 5-HT2C and 5-HT6, adrenergic α2 receptors, histamine H1 and the muscarinic M1 and M4 receptors. Table 2 shows the pKi's of SLV313 and a series of reference antipsychotics (clozapine, haloperidol, risperidone, ziprasidone, and olanzapine). In addition, a wider screen demonstrated that there was no receptor binding observed at a range of additional receptors including glutamate, imidazoline, NT1, benzodiazepine, H2, angiotensin, and neurokinin receptors (pKi <6; data not shown).
In Vitro Functional Activity
Quinpirole fully attenuated forskolin-induced accumulation of cAMP in CHO cells with a pEC50 of 6.8. The effect of 10−6 M quinpirole was concentration dependently antagonized by SLV313 (pA2 9.3±0.3, Figure 2 upper panel). Using similar methodologies, SLV313 was found to be a full and potent agonist at 5-HT1A receptors with a pEC50 of 9.0±0.2 (Figure 2, lower panel). In addition, the effects of SLV313 were measured using a GTPγS-binding system in CHO cells transfected with the human dopamine D3 receptor. SLV313 failed to stimulate the human D3 receptor at 10 μM, yet potently and fully (at 10 μM) inhibited dopamine (pA2=8.9±0.2, Figure 2, middle panel).
The effect of SLV313 on dopamine D2, D3 and 5-HT1A receptors. Upper panel: quinpirole alone (open circles) completely attenuated forskolin-induced accumulation of cAMP in CHO cells transfected with the D2 receptor with a pEC50 of 6.8. SLV313 (closed circles) concentration dependently antagonized quinpirole (1 μM) effects (pA2 of 9.3±0.3). Middle panel: in D3 receptor-transfected cells SLV313 possessed antagonist properties in the presence of dopamine (0.3 μM), using a GTPγS assay (filled circles; pA2 of 8.9±0.2; dopamine alone was also tested for control purposes open triangles). Lower panel: in CHO cells transfected with the 5-HT1A receptor SLV313 concentration dependently reduced forskolin-stimulated cAMP production in a concentration-dependent manner (filled circles; pEC50 of 9.0±0.2), similar to the 5-HT1A receptor agonist 8-OHDPAT (filled squares). All graphs demonstrate percentage difference from control and means±SEM from at least triplicate experiments, where SEM are not visible the symbols obscure the SEM.
Apomorphine-Induced Climbing Behavior
SLV313 dose dependently attenuated climbing induced by the dopamine receptor agonist apomorphine (1 mg/kg s.c.) with an ED50 (95% confidence limits) value of 0.41. (0.30–0.56) mg/kg p.o. (Figure 3, upper panel). Similarly, antagonism was observed with the D2 receptor antagonist and typical antipsyschotic haloperidol (ED50 0.10 (0.08–0.15) mg/kg p.o.; Figure 3, lower panel). MEDs were 0.3 and 0.1 mg/kg p.o., respectively. In addition, in a study designed to test the longevity of the effects of SLV313 after administration there was a dose-dependent reduction of apomorphine-induced climbing seen 4 h after administration (ED50=1.21 (<0.3 to ⩾3) and an MED of 1 mg/kg p.o., data not shown).
SLV313 and haloperidol dose dependently attenuated climbing behavior induced by the dopamine agonist apomorphine (1 mg/kg s.c.). The ED50 for SLV313 was 0.41 (0.30–056) mg/kg p.o. and for haloperidol 0.10 (0.08–0.15) mg/kg p.o. *p<0.05 cf. control data are expressed as percent control (100%). Data shown are means±SEM.
5-HT1A Receptor Syndrome
The characteristic behaviors associated with 5-HT1A receptor stimulation were observed after administration of SLV313. Nonparametric statistics confirmed the significant induction of FBP (MED=3 mg/kg p.o.), LLR (MED=1 mg/kg p.o.), and HLA (MED=10 mg/kg p.o.) but not FPT (Table 3). In addition, temperature measurements showed no difference recorded at the start of the experiment (p>0.05), but significant differences after the completion of the behavioral observations (F(3,28)=6.31, p<0.002) (Table 3). An experiment designed to assess the role of the 5-HT1A receptors on the effects of SLV313 demonstrated that WAY100635 antagonized SLV313-induced FBP, HLA, and LLR with MEDs of 0.1, 0.1, and 0.03 mg/kg s.c., respectively (Table 4); no significant effect on FPT was seen. No significant differences in the temperature between treatment groups at the beginning of the experiment (p>0.05), but significant treatment-induced differences in temperature were observed at the end of the experiment (F(4,35)=17.59, p<0.0001) (Table 4). The response in SLV313-treated animals was significantly different from vehicle-treated animals, and animals pretreated with WAY 100635 at 0.3 mg/kg were significantly different from vehicle+SLV313-treated animals. The partial 5-HT1A agonists aripiprazole (3, 10, and 30 mg/kg p.o.) failed to elicit any significant serotonergic syndrome behaviors, and no changes in temperature were seen at the start (F(3,28)=1.71, p<0.84) or at the end of the experiment (F(3,28)=2.45, p<0.08) (Table 3). Ziprasidone (10 mg/kg p.o.) and clozapine (30 mg/kg p.o.) demonstrated some limited ability to increase LLR and FBP together with a hypothermic effect (F(2,21)=17.45, p<0.001; post hoc, p<0.05 Table 3).
Flesinoxan Drug Discrimination Paradigm
The dose dependence of flesinoxan-induced generalization to the drug appropriate key has previously been demonstrated in the same subjects (Mos et al, 1997; Herremans et al, 1999). In the present study, SLV313 fully substituted for the training drug flesinoxan (ED50 of 0.03 (0.01–0.08)), with no effect on rates of responding (F(3,40)=1.93, p<0.13) (Figure 4, upper and lower panels). However, SLV313 (0.25 mg/kg p.o.) failed to attenuate the training dose of flesinoxan (0.25 mg/kg) in antagonism studies (100% of animals chose the drug key; 1.91±0.21 pecks/s) (data not shown). In antagonism tests, WAY100635 fully antagonized flesinoxan-appropriate responding induced by SLV313 (0.1 mg/kg) with an ED50 value of 0.32 (0.1–1) (Figure 4, upper panel), with no effect on rates of responding (F(2,30=0.76, p<0.47) (Figure 4, lower panel). In order to assess whether the dopamine D2 antagonist properties of SLV313 contributed to the observed generalization, the effects of haloperidol to substitute to flesinoxan were assessed. Haloperidol failed to generalize to the drug key tested at a dose range of 0.1–1 mg/kg and surprisingly failed to reduce rates of responding (F(2,31)=0.75, p<0.47) (Table 5). In an antagonist test haloperidol reduced the effects of flesinoxan, although this was only seen at doses that reduced response rates (F(2,30)=3.83, p<0.05) (Table 5).
The effect of SLV313 in a flesinoxan drug discrimination procedure. Upper panel: SLV313 (open circles) fully generalized to the flesinoxan-appropriate key in pigeons trained to discriminate flesinoxan from vehicle. In antagonist tests, WAY100635 antagonized the effects of SLV313 (filled circles). Lower panel: in either study the response rates were not affected.
The Effect of SLV313 on Catalepsy
While haloperidol dose dependently increased the proportion of rats defined as cataleptic and the latency to remove their fore-paws from the bar (MED=4 mg/kg p.o., for both parameters), SLV313 at a dose up to 60 mg/kg p.o. failed to elicit these effects (Table 6).
In Vivo Microdialysis Studies
Effect in the nucleus accumbens
SLV313 induced a dose- and time-dependent increase in extracellular levels of DA, DOPAC, and HVA, a reduction in 5-HT levels and no change in 5-HIAA levels (time course data for 10 mg/kg p.o. are displayed (Figure 5)). Evaluation of the AUC for 120 min following drug administration, compared to basal dialysate levels (% AUC120) revealed that SLV313 (0.1–10 mg/kg p.o.) induced a dose-dependent increase in extracellular levels of dopamine (F(4,27)=4.73, p<0.0001; Figure 5, left upper panel) with an MED of 3 mg/kg p.o. Similar increases in DOPAC (F(4,27)=21.90, p<0.001, Figure 5, lower left and right panels) and HVA (F(4,27)=21.41, p<0.0001, Figure 5, lower left and right panels) were also observed. While SLV313 dose dependently reduced extracellular 5-HT (F(4,13)=21.82, p<0.0001, Figure 5, upper right panel) no significant effects were observed on the serotonin metabolite 5-HIAA (F(4,27)=0.74, p<0.57, Figure 5, lower right and left panels).
The effect of SLV313 on dialysate DA, HVA, DOPAC, 5-HT, and 5-HIAA in the nucleus accumbens. SLV313 concomitantly increased extracellular dopamine and decreased extracellular levels of 5-HT in the nucleus accumbens of freely moving rats. No effect was seen on extracellular 5-HIAA, but DOPAC and HVA levels were elevated. Data are expressed as percent of baseline for the time course following treatment with 10 mg/kg p.o. of SLV313 (indicated by the arrow) or with the expression of AUC120 data. *p<0.05 for all parameters shown but not for 5-HIAA.
Effect in the prefrontal cortex
SLV313 (3, 10, and 20 mg/kg p.o.) significantly increased dopamine release in the mPFC (F(1,9)=10.8, p<0.001; F(1,13)=17.61, p<0.001; F(1,13)=22.1, p<0.0001, respectively; n=7–8) (Figure 6, upper panel). AUC analyses confirmed that SLV313 (3, 10, and 20 mg/kg p.o.) significantly increased dopamine release in the mPFC (F(1,9)=10.26, p<0.01; F(1,13)=33.03, p<0.001; F(1,13)=35.26, p<0.001, respectively; Figure 8). The increase in cortical dopamine release produced by 10 mg/kg SLV313 was inhibited by WAY100635 (0.2 mg/kg s.c.) (F(1,10)=24.12, p<0.0001; n=4–8) (Figure 9, upper panel). In addition, SLV313 at 20 mg/kg (p.o.) also significantly increased ACh release in the mPFCx (F(1,11)=9.03, p<0.0032; n=6–7), but 3 and 10 mg/kg did not (F(1,8)=0.327, p<0.57; F(1,11)=0.147, p<0.7, respectively; n=4–6) (Figure 7, upper panel) which was confirmed by analyses of the AUC data (F(1,11)=0.3, p<0.58; F(1,8)=2.22, p<0.11; F(1,11)=9.0, p<0.033; 3, 10, and 20 mg/kg p.o., respectively; Figure 8). AUC analysis for the antagonism experiments was not performed (Figures 6, 7, 8 and 9).
Time course effects of SLV313 (3–20 mg/kg, p.o.) on extracellular dopamine levels in the medial prefrontal cortex (upper panel) and hippocampus (lower panel). Data are means±SEM of the dialysate dopamine levels, expressed as a percentage of each predrug baseline dopamine value. The arrow indicates drug injection. Upper panel: ***p<0.001 from time points 60–210 min for the groups of 10 and 20 mg/kg, compared to vehicle-treated rats. Lower panel: **p<0.01 from time points 60–210 min for the group of 10 mg/kg, compared to vehicle-treated rats. ***p<0.01 from time point 90–210 min for the group 20 mg/kg, compared to vehicle-treated rats.
The effect of WAY100635 (0.2 mg/kg, s.c.) on SLV313 (10 mg/kg, p.o.)-induced dopamine release in the medial prefrontal cortex (upper panel) and hippocampus (lower panel). Data are means±SEM of the dialysate dopamine levels, expressed as a percentage of each predrug baseline dopamine value. The arrows indicate drug injection times. Upper panel: ***p<0.001 from time points 60–210 min for the group of WAY100635 plus SLV313 following post hoc tests, compared to the WAY100635 group. Lower panel: ***p<0.001 from time points 60–120 and 210 min for the group of WAY100635 plus SLV313, compared to the WAY100635 group following post hoc tests.
Time-course effects of SLV313 (3–20 mg/kg, p.o.) on extracellular acetylcholine levels in the medial prefrontal cortex (upper panel) and hippocampus (lower panel). Data are means±SEM of the dialysate acetylcholine levels, expressed as a percentage of each predrug baseline acetylcholine value. The arrow indicates drug injection and **p<0.01 from time points 60–210 min for the group of 20 mg/kg, compared to vehicle-treated rats with post hoc analyses.
Effect in the hippocampus
Similar to the effect in the mPFC, SLV313 (3, 10, and 20 mg/kg p.o.), significantly increased dopamine release in the hippocampus (F(1,7)=7.22, p<0.0086; F(1,10)=18.89; p<0.0001; F(1,11)=7.99, p<0.006, respectively; n=5–8) (Figure 6, lower panel). Analyses of the AUC confirmed these effects (F(1,7)=9.56, p<0.001; F(1,10)=19.36; p<0.001; F(1,11)=13.06, p<0.001, respectively) (Figure 8, left panel). WAY100635 (0.2 mg/kg, s.c.) inhibited SLV313 (10 mg/kg, p.o.)-induced dopamine release in the hippocampus (F(1,10)=20.88, p<0.0001; n=4–8) (Figure 7, lower panel). However, SLV313, only at the high dose of 20 mg/kg, transiently increased ACh release in the hippocampus but in the time course analysis this was not confirmed following post hoc analysis (F(1,9)=8.61, p<0.004; n=5–6; AUC F(1,9)=13.26, p<0.05) whereas three did not (F(1,8)=0.77, p<0.38 (AUC F(1,8)=0.772, p<0.38); n=4–6) and a significant effect was only seen for the AUC determination at 10 mg/kg (F(1,10)=0.89, p<0.20 vs AUC F(1,10)=9.08, p<0.05; n=4–6) (Figure 7, lower panel and Figure 8). AUC analyses for the antagonism experiments was not performed.
The Effect of Chronic Administration of SLV313 on the Number of Spontaneously Active VTA and SNC Neurons
A significant effect of treatment on the number of spontaneously active VTA dopamine neurons (F(3,36)=30.6, p<0.001) but not SNC dopamine neurons (F(3,36)=0.12, p<0.95) was observed. Subsequent post hoc analyses of the VTA data indicated that the chronic administration of 3 or 10 mg/kg p.o. of SLV313 or 20 mg/kg p.o. of clozapine significantly decreased the number of spontaneously active VTA dopamine neurons compared to vehicle-treated animals (Figure 10). In addition, the chronic administration of 10 mg/kg of SLV313 produced a significantly greater decrease in the number of spontaneously active VTA dopamine neurons compared to 20 mg/kg of clozapine.
The effect of repeated (21 days) oral administration of vehicle, SLV313, or clozapine on the number of spontaneously active SNC and VTA dopamine neurons in anesthetized male Sprague–Dawley rats. Each value represents the mean number of spontaneously active dopamine neurons per stereotaxically defined electrode descent±SEM. A total of 10 animals were examined for each treatment group. Animals received one p.o. administration per day for 21 days. On the test day, animals were given the appropriate treatment and 2 h later, the number of spontaneously active dopamine neurons was determined. *p<0.05 vs vehicle and +p<0.05 vs clozapine group. Filled bars VTA, open bars SNC.
DISCUSSION
Data from the present studies demonstrate that SLV313 displayed dopamine D2/3 receptor antagonist and serotonin 5-HT1A receptor agonist properties in vitro and in vivo. Receptor-binding studies demonstrated that SLV313 had appreciable receptor binding to serotonin 5-HT2B receptors with moderate affinities at serotonin 5-HT7, serotonin 5-HT2A and adrenergic α1 receptors. In addition, SLV313, at 10−6 M, and displayed no affinity for a number of other receptors or transporters. In vivo SLV313 acted as a serotonin 5-HT1A receptor agonist and dopamine D2 receptor antagonist, did not induce catalepsy, was preferentially active in the meso(cortico)limbic pathway and induced dopamine and ACh increases in the hippocampus and mPFCx.
The pattern of receptor-binding affinity differed notably from that of the other antipsychotic agents tested in that moderate serotonin 5-HT2A and noradrenergic α1 binding was seen and SLV313 was devoid of serotonin 5-HT6, adrenergic α2, muscarinic, and H1 activity. Moreover, the dopamine D2 receptor affinity was greater than that of clozapine and olanzapine and serotonin 5-HT1A receptor affinity was similar to ziprasidone. The lack of both H1 and 5-HT2C receptor binding may be beneficial for the actions of SLV313 insofar as 5-HT2C, histamine H1 and muscarinic receptors have all been linked to weight gain induced by some of the novel antipsychotics (Reynolds et al, 2002; Hartfield et al, 2003).
While SLV313 showed potent serotonin 5-HT2B receptor binding, further studies demonstrated that these were fully antagonist in nature (data not shown). Cellular functional assays suggested that SLV313 reversed the effects of the dopamine agonist quinpirole on D2-mediated cAMP accumulation. In addition to dopamine D2 receptor antagonism, full serotonin 5-HT1A receptor agonism and dopamine D3 receptor antagonism was also observed in vitro. SLV313 is not unusual in possessing affinity for the dopamine D4 receptor as many antipsychotics have affinity for this receptor. However, both preclinical (Newman-Tancredi et al, 1997; Bristow et al, 1997a) and clinical data (Bristow et al, 1997b) suggest that dopamine D4 receptors are probably not a pharmacological target for the treatment of schizophrenia. Conversely, it has been suggested that dopamine D3 receptor antagonism, with or without dopamine D2 antagonism may represent a target for antipsychotic strategies (for review see Joyce and Millan, 2005). However, confirmation is needed as novel clinical candidates have not yet cleared Phase II clinical studies. Other antipsychotics demonstrate mixed dopamine D2 and serotonin 5-HT1A effects (at varying ratios), for example ziprasidone, clozapine, SSR181507, and aripiprazole are all serotonin 5-HT1A partial agonists (eg Newman-Tancredi et al, 1996, 2001; Jordan et al, 2002; and see earlier). In support of the present study SLV313 was shown to bind to rat striatal dopamine D2 and cortical serotonin 5-HT1A receptors where it elicits antagonist and agonist effects, respectively (Newman-Tancredi et al, 2004).
The in vitro efficacy at D2 and 5-HT1A receptors of SLV313 was mirrored using in vivo behavioral models insofar as SLV313 attenuated apomorphine-induced climbing, like haloperidol, and attenuated amphetamine- and methylphenidate-stimulated locomotor activity (Kleven et al, 2003). Such effects are indicative of putative D2 receptor antagonism. SLV313 also increased extracellular dopamine levels in the nucleus accumbens of conscious rats, an action consistent with dopamine D2 receptor antagonism in vivo. Consistent with 5-HT1A agonist effects SLV313-induced serotonin 5-HT1A syndrome behaviors and hypothermia, which was antagonized by pretreatment with the 5-HT1A receptor antagonist WAY100635. Unlike the nonselective serotonin 5-HT1A agonist 8-OHDPAT (Tricklebank et al, 1984; Depoortere et al, 2003) SLV313 did not induce fore-paw-treading behaviors. This inability to induce fore-paw-treading behavior was also demonstrated with SSR181507 (Depoortere et al, 2003) and the authors proposed that the lack of SSR181507 on fore-paw-treading may indicate a reduced propensity to induce the serotonin syndrome. However, the effects of SSR181507 have not been reported on other serotonergic syndrome behaviors (Depoortere et al, 2003) so such a conclusion might prove preliminary. It is unlikely that mixed D2 antagonists and 5-HT1A agonists, like SLV313, will induce the serotonin syndrome in humans to any great extent in a clinical schizophrenia treatment setting, as chronic administration of 8-OH-DPAT results in tolerance to syndrome behaviors (Prinssen et al, 2000), but interestingly not in the ability to reduce haloperidol-induced catalepsy (Prinssen et al, 2000). Whether such a direct comparison across preclinical and clinical studies can yet be made is unclear for such mixed D2/3 antagonists with 5-HT1A agonist compounds. No components of the serotonergic syndrome were observed following treatment with either ziprasidone or aripiprazole (Wolff et al, 2003). This lack of effect of aripiprazole was confirmed in the present study and although ziprasidone and clozapine did show some efficacy the effects were very weak compared to SLV313. Furthermore, neither aripiprazole nor ziprasidone antagonized the actions of 8-OHDPAT (Wolff et al, 2003) and aripiprazole failed to reduce hippocampal serotonin 5-HT dialysate levels (Assie et al, 2005). Thus, aripiprazole appears devoid of intrinsic agonist actions at serotonin 5-HT1A receptors in vivo using the paradigms described here. Interestingly, in vivo electrophysiological studies have demonstrated that ziprasidone and SSR181507 act as agonists at serotonin 5-HT1A receptors and reduce dorsal raphe nucleus serotonergic cell firing (Sprouse et al, 1999; Claustre et al, 2003). Clozapine and olanzapine, however, appear to mediate this effect via α1 noradrenergic receptors (Sprouse et al, 1999; Lejeune et al, 1994). Consistent with such an action in vivo microdialysis studies demonstrated that SLV313 reduced extracellular levels of serotonin in the nucleus accumbens suggesting an agonist action at the somatodendritic (5-HT1A) autoreceptor (or via feedback inhibition). Similarly SLV313 reduced hippocampal serotonin dialysate levels (Assie et al, 2005), which were dependent on stimulation of the 5-HT1A receptor. SLV313 fully (>80%) substituted for the serotonin 5-HT1A agonist flesinoxan in pigeons trained to discriminate flesinoxan from vehicle and was antagonized by WAY100635 consistent with a serotonin 5-HT1A agonist profile (Mos et al, 1997). Dopamine D2 receptor antagonism is not involved in the flesinoxan cue as haloperidol did not substitute for flesinoxan and only slightly attenuated the flesinoxan response, but only when response rates were reduced. Taken together, these data convincingly suggest that SLV313 has serotonin 5-HT1A agonist and D2/3 antagonist effects in vivo and in vitro.
A combination of serotonin 5-HT1A agonism and D2 antagonism may confer positive benefits for the treatment of schizophrenia (see for reviews Millan, 2000; Meltzer et al, 2003). One such mechanism would be by the reduction of neurological or EPS side effects seen in preclinical (Prinssen et al, 1999, 2000; Wadenberg and Ahlenius, 1991; Wadenberg, 1996; Wadenberg et al, 1999; Christoffersen and Meltzer, 1998; and see Depoortere et al, 2003) and clinical studies (Goff et al, 1991; Yoshida et al, 1998). In the rat, the reduction of the cataleptic effect was only evident with moderate to high intrinsic activity 5-HT1A receptor agonists (Prinssen et al, 1999). At doses up to 60 mg/kg p.o. SLV313 did not induce catalepsy (ie at doses >20 the CAR activity; McCreary et al, 2002) in contrast to haloperidol. Further, SLV313, like clozapine, significantly reduced the number of spontaneously active cells in the VTA, but not the SNC commensurate with a putative mesolimbic activity and atypical antipsychotic action (Chiodo, 1988; White and Wang, 1983; Chiodo and Bunney, 1983; Freeman and Bunney, 1987). Thus, based on its electrophysiological profile, SLV313 may be classified as an atypical antipsychotic preclinically. It is possible that SLV313-induced agonistic action at serotonin 5-HT1A receptors may be important in producing its VTA-selective effects since the in vivo electrophysiological results obtained with SLV313 are similar to those reported following the chronic administration of the mixed D2 antagonist/5-HT1A receptor agonists 1192U90 and SSR181507 (Jones-Humble et al, 1996; Claustre et al, 2003). A role for the D2 receptor in assisting in this action cannot be excluded (Nakamura et al, 2006). Thus, data from the present electrophysiological and catalepsy studies, coupled with the results with 1192U90 and SSR181517 (Jones-Humble et al, 1996; Claustre et al, 2003), support the hypothesis of limbic selectivity with mixed serotonin 5-HT1A agonists and D2 antagonists in the same molecule.
Besides a potential reduction in EPS liability, combined serotonin 5-HT1A agonism and D2 receptor antagonism could confer additional benefits over typical antipsychotic agents. For example, the potentiation of antipsychotic-like effects in the CAR paradigm (Wadenberg and Ahlenius, 1991; Prinssen et al, 1996) at doses far lower than the ‘normal’ cataleptic dose and the effects seen with SLV313 in the CAR paradigm (McCreary et al, 2002) support potential efficacy against the positive symptoms of schizophrenia, but positive symptoms are not the only symptom set in schizophrenia. One of the hypotheses of the abnormalities underlying schizophrenia has been the hypofrontality model which proposes hypoactive mPFCx circuitry in schizophrenia (Weinberger and Lipska, 1995). The mPFCx may have a role in decision making, working memory, and attentional processing (Goldman-Rakic, 1998) and may have an additional role in the treatment of the negative symptoms of schizophrenia (Weinberger and Lipska, 1995). It has also been suggested that ACh may also be of pivotal importance for the cognitive symptoms of schizophrenia at the level of both the mPFCx and hippocampus and that atypical antipsychotics increase dopamine and ACh in both of these brain areas (Eichenbaum et al, 1999; Seidman et al, 2002; Moghaddam and Bunney, 1990; Kuroki et al, 1999; Ichikawa et al, 2002a, 2002b; Shirazi-Southall et al, 2002; Li et al, 2004; Chung et al, 2004) via serotonin 5-HT1A receptor-dependent mechanisms (Rollema et al, 1997; Ichikawa and Meltzer, 1999; Li et al, 2004). Recent studies with SSR181507 suggested that combined serotonin 5-HT1A and dopamine D2 antagonism, with the absence of serotonin 5-HT2A receptor antagonism, augments dopamine levels in the mPFCx (Claustre et al, 2003). This serotonin 5-HT1A-dependent increase in hippocampal dopamine was confirmed in the present study with SLV313. The SLV313-induced augmented dopamine efflux was antagonized by pretreatment with the 5-HT1A antagonist WAY100635 (see also Assie et al, 2005). Such effects have also been noted with other antipsychotics (Ichikawa et al, 2002a, 2002b). ACh was also elevated significantly following treatment with SLV313 in the mPFCx and hippocampus (transiently and modestly), consistent with other antipsychotics (see Li et al, 2004). Taken together, the present data, provided they can be extrapolated to humans, suggest that SLV313 may improve the negative symptoms of schizophrenia (Weinberger and Lipska, 1995) as well as cognitive and attentional processing (Goldman-Rakic, 1998; Kuroki et al, 1999; Meltzer, 1999; Meltzer and McGurk, 1999; Harvey and Keefe, 2001). Indeed, serotonin 5-HT1A receptor agonism in the mPFCx has been shown to improve attentional processing in the rat five-choice serial reaction time task (Winstanley et al, 2003) and the serotonin 5-HT1A (partial) receptor agonist tandospirone improved cognition in schizophrenic patients (Sumiyoshi et al, 2001a, 2001b).
In summary, SLV313 is a novel putative antipsychotic possessing 5-HT1A receptor agonist and dopamine D2/3 receptor antagonist properties both in vitro and in vivo. It is possible that SLV313 may be a broadly effective antipsychotic with low potential for EPS for the treatment of schizophrenia and other psychoses, for example bipolar disorder. However, verification of this hypothesis is needed in the clinic.
References
Assie MB, Ravailhe V, Faucillon V, Newman-Tancredi A (2005). Contrasting contribution of 5-HT1A receptor activation to neurochemical profile of novel antipsychotics: frontocortical dopamine and hippocampal serotonin release in rat brain. J Pharmacol Exp Ther 315: 265–272.
Bantick RA, Deakin JF, Grasby PM (2001). The 5-HT1A receptor in schizophrenia: a promising target for novel atypical neuroleptics? J Psychopharmacol 15: 37–46.
Berendsen HH, Jenck F, Broekkamp CL (1989). Selective activation of 5HT1A receptors induces lower lip retraction in the rat. Pharmacol Biochem Behav 33: 821–827.
Bill DJ, Knight M, Forster EA, Fletcher A (1991). Direct evidence for an important species difference in the mechanism of 8-OH-DPAT-induced hypothermia. Br J Pharmacol 103: 1857–1864.
Bonhaus DW, Bach C, DeSouza A, Salazar FH, Matsuoka BD, Zuppan P et al (1995). The pharmacology and distribution of human 5-hydroxytryptamine2B (5-HT2B) receptor gene products: comparison with 5-HT2A and 5-HT2C receptors. Br J Pharmacol 115: 622–628.
Bristow LJ, Collinson N, Cook GP, Curtis N, Freedman SB, Kulagowski JJ et al (1997a). L-745, 870, a subtype selective dopamine D4 receptor antagonist, does not exhibit a neuroleptic-like profile in rodent behavioral tests. J Pharmacol Exp Ther 283: 1256–1263.
Bristow LJ, Kramer MS, Kulagowski J, Patel S, Ragan CI, Seabrook GR (1997b). Scizophrenia and L-745, 870, a novel dopamine D4 receptor antagonist. TIPS 18: 186–188.
Bunzow JR, Van Tol HH, Grandy DK, Albert P, Salon J, Christie M et al (1988). Cloning and expression of a rat D2 dopamine receptor cDNA. Nature 336: 783–787.
Burnet PW, Eastwood SL, Harrison PJ (1996). 5-HT1A and 5-HT2A receptor mRNAs and binding site densities are differentially altered in schizophrenia. Neuropsychopharmacology 15: 442–555.
Casey DE (1996). Extrapyramidal syndromes and new antipsychotic drugs: findings in patients and non-human primate models. Br J Psychiatr 29: 32–39.
Chiodo LA (1988). Dopamine-containing neurons in the mammalian central nervous system: electrophysiology and pharmacology. Neurosci Biobehav 12: 49–91.
Chiodo LA, Bunney BS (1983). Typical and atypical neuroleptics: Differential effects of chronic administration on the activity of A9 and A10 dopamine neurons. J Neurosci 7: 1607–1619.
Christoffersen CL, Meltzer LT (1998). Reversal of haloperidol-induced extrapyramidal side effects in cebus monkeys by 8-hydroxy-2-(di-n-propylamino)tetralin and its enantiomers. Neuropsychopharmacology 18: 399–402.
Chung YC, Li Z, Dai J, Meltzer HY, Ichikawa J (2004). Clozapine increases both acetylcholine and dopamine release in rat ventral hippocampus: role of 5-HT(1A) receptor agonism. Brain Res 1023: 54–63.
Claustre Y, Peretti DD, Brun P, Gueudet C, Allouard N, Alonso R et al (2003). SSR181507, a dopamine D(2) receptor antagonist and 5-HT(1A) receptor agonist. I: Neurochemical and electrophysiological profile. Neuropsychopharmacology 28: 2064–2076.
Depoortere R, Boulay D, Perrault G, Bergis O, Decobert M, Francon D et al (2003). SSR181507, a dopamine D2 receptor antagonist and 5-HT1A receptor agonist. II: Behavioral profile predictive of an atypical antipsychotic activity. Neuropsychopharmacology 28: 1889–1902.
Dini S, Caselli GF, Ferrari MP, Giani R, Clavenna G (1991). Heterogeneity of [3H]-mepyramine binding sites in guinea pig cerebellum and lung. Agents Actions 33: 181–184.
Dorje F, Wess J, Lambrecht G, Tackle R, Mutschler E, Brann MR (1991). Antagonist binding profiles of five cloned human muscarinic receptor subtypes. J Pharmacol Exp Ther 256: 727–733.
Eichenbaum H, Dudchenko P, Wood E, Shapiro M, Tanila H (1999). The hippocampus, memory, and place cells: is it spatial memory or a memory space? Neuron 23: 209–226.
Fargin A, Raymond JR, Regan JW, Cotecchia S, Lefkowitz RJ, Caron MG (1989). Effector coupling mechanisms of the cloned 5-HT1A receptor. J Biol Chem 64: 14848–14852.
Fernandez G, Klaver P, Fell J, Grunwald T, Elger CE (2002). Human declarative memory formation: segregating rhinal and hippocampal contributions. Hippocampus 12: 514–519.
Freeman AS, Bunney BS (1987). Chronic neuroleptic effects on DA neuron activity: a model for predicting therapeutic efficacy and side effects? Psychopharmacol Ser 3: 225–235.
Goff DC, Midha KK, Brotman AW, McCormick S, Waites M, Amico ET (1991). An open trial of buspirone added to neuroleptics in schizophrenic patients. J Clin Psychopharmacol 11: 193–197.
Goldman-Rakic PS (1998). The cortical dopamine system: role in memory and cognition. Adv Pharmacol 42: 707–711.
Grandy DK, Marchionni MA, Makam H, Stofko RE, Alfano M, Frothingham L et al (1989). Cloning of the cDNA and gene for a human D2 DA receptor. Proc Natl Acad Sci USA 86: 9762–9766.
Greengrass P, Bremner R (1979). Binding characteristics of 3H-prazosin to rat brain alpha-adrenergic receptors. Eur J Pharmacol 55: 323–326.
Gurevich EV, Joyce JN (1997). Alterations in the cortical serotonergic system in schizophrenia: a postmortem study. Biol Psychiatr 42: 529–545.
Hartfield AW, Moore NA, Clifton PG (2003). Serotonergic and histaminergic mechanisms involved in intralipid drinking? Pharmacol Biochem Behav 76: 251–258.
Harvey PD, Keefe RS (2001). Studies of cognitive change in patients with schizophrenia following novel antipsychotic treatment. Am J Psychiatr 158: 176–184.
Herremans AHJ, van der Heyden JAM, van Drimmelen M, Olivier B (1999). The 5-HT1A agonist flesinoxan shares discriminative stimulus properties with some 5-HT2 receptor antagonists. Pharmacol Biochem Behav 64: 389–395.
Hertel P, Nomikos GG, Iurlo M, Svensson TH (1996). Risperidone: regional effects in vivo on release and metabolism of dopamine and serotonin in the rat brain. Psychopharmacology (Berlin) 124: 74–86.
Hope AG, Peters JA, Brown AM, Lambert JJ, Blackburn TP (1996). Characterization of a human 5-hydroxytryptamine3 receptor type A (h5-HT3R-AS) subunit stably expressed in HEK 293 cells. Br J Pharmacol 118: 1237–1245.
Ichikawa J, Dai J, Meltzer HY (2002a). 5-HT(1A) and 5-HT(2A) receptors minimally contribute to clozapine-induced acetylcholine release in rat medial prefrontal cortex. Brain Res 939: 34–42.
Ichikawa J, Dai J, O'Laughlin IA, Fowler WL, Meltzer HY (2002b). Atypical, but not typical, antipsychotic drugs increase cortical acetylcholine release without an effect in the nucleus accumbens or striatum. Neuropsychopharmacology 26: 325–339.
Ichikawa J, Ishii H, Bonaccorso S, Fowler WL, O'Laughlin IA, Meltzer HY (2001). 5-HT(2A) and D(2) receptor blockade increases cortical DA release via 5-HT(1A) receptor activation: a possible mechanism of atypical antipsychotic-induced cortical dopamine release. J Neurochem 76: 1521–1531.
Ichikawa J, Meltzer HY (1999). R(+)-8-OH-DPAT, a serotonin(1A) receptor agonist, potentiated S(-)-sulpiride-induced dopamine release in rat medial prefrontal cortex and nucleus accumbens but not striatum. J Pharmacol Exp Ther 291: 1227–1232.
Jones-Humble SA, Durcan MJ, Lyerly D, Norton MS, Tang FLM, Russell AV et al (1996). Preclinical neurochemical and electrophysiological profile of 1192U90, a potential antipsychotic. Neuropsychopharmacology 15: 217–229.
Jordan S, Koprivica V, Chen R, Tottori K, Kikuchi T, Altar CA (2002). The antipsychotic aripiprazole is a potent, partial agonist at the human 5-HT1A receptor. Eur J Pharmacol 441: 137–140.
Joyce JN, Millan MJ (2005). Dopamine D3 receptor antagonists as therapeutic agents. Drug Discovery Today 10: 917–925.
Kleven MS, Prinssen EPM, Koek W, Grevoz-Barret C, Newman-Tancredi A (2003). In vivo pharmacology of novel antipsychotics having mixed D2 antagonist/5HT1A agonist properties: evidence for lowered EPS liability. Soc Neurosci Abstr 33: 956.2.
Kuroki T, Meltzer HY, Ichikawa J (1999). Effects of antipsychotic drugs on extracellular dopamine levels in rat medial prefrontal cortex and nucleus accumbens. J Pharmacol Exp Ther 288: 774–781.
Lejeune F, Audinot V, Gobert A, Rivet JM, Spedding M, Millan MJ (1994). Clozapine inhibits serotoninergic transmission by an action at alpha 1-adrenoceptors not at 5-HT1A receptors. Eur J Pharmacol 260: 79–83.
Li Z, Ichikawa J, Dai J, Meltzer HY (2004). Aripiprazole, a novel antipsychotic drug, preferentially increases dopamine release in the prefrontal cortex and hippocampus in rat brain. Eur J Pharmacol 493: 75–83.
Mackenzie RG, Vanleeuven D, Pugsley TA, Shih Y-H, Demattos S, Tang L et al (1994). Characterization of the human dopamine D3 receptor expressed in transfected cell lines. Eur J Pharmacol 266: 79–85.
McCreary AC, Glennon JC, Tuinstra T, Herremans AHJ, Van der Heyden J, Long SK et al (2002). SLV313: a novel antipsychotic with additional antidepressant and anxiolytic-like acitons. Eur Neuropsychopharmacol 12: S274.
Meltzer HY (1999). The role of serotonin in antipsychotic drug action. Neuropsychopharmacology 2: 106–115.
Meltzer HY, Li Z, Kaneda Y, Ichikawa J (2003). Serotonin receptors: their key role in drugs to treat schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry 27: 1159–1172.
Meltzer HY, McGurk SR (1999). The effect of clozapine, risperidone and olanzapine on cognitive function in schizophrenia. Schizophrenia Bull 25: 233–255.
Mialet J, Berque-Bestel I, Sicsic S, Langlois M, Fischmeister R, Lezoualc'h F (2000). Pharmacological characterization of the human 5-HT(4(d)) receptor splice variant stably expressed in Chinese hamster ovary cells. Br J Pharmacol 131: 827–835.
Millan MJ (2000). Improving the treatment of schizophrenia: focus on serotonin (5-HT)1A receptors. J Pharmacol Exp Ther 295: 853–861.
Moghaddam B, Bunney BS (1990). Acute effects of typical and atypical antipsychotic drugs on the release of dopamine from prefrontal cortex, nucleus accumbens, and striatum of the rat: an in vivo microdialysis study. J Neurochem 54: 1755–1760.
Monsma FJ, Shen Y, Ward RP, Hamblin MW, Sibley DR (1993). Cloning and expression of a novel serotonin receptor with high affinity for tricyclic psychotropic drugs. Mol Pharmacol 43: 320–327.
Mos J, van Hest A, van Drimmelen M, Herremans AHJ, Olivier B (1997). The putative 5-HT1A receptor antagonist DU125530 blocks the discriminative stimulus properties of the 5-HT1A agonist flesinoxan in pigeons. Eur J Pharmacol 325: 145–153.
Mulheron JG, Casanas SJ, Arthur JM, Garnovskaya MN, Gettys TW, Raymond JR (1994). Human 5-HT1A receptor expressed in insect cells activates endogenous G(o)-like G protein(s). J Biol Chem 269: 12954–12962.
Nakamura K, Suzuki K, McCreary AC, Ashby Jr CR (2006). The acute and chronic administration of (±)-8-hydroxy-2-(di-n-propylamino)tetralin (8-OH-DPAT) significantly alters the activity of spontaneously active midbrain dopamine neurons in rats: an in vivo electrophysiological study. Synapse 59: 359–367.
Newman-Tancredi A, Assie M-B, Leduc N, Ormiere A-M, Danty N, Cosi C (2004). Novel antipsychotics activate recombinant human and native rat serotinin 5-HT1A receptors: affinity, efficacy and potential implications for the treatment of scizophrenia. Int J Neuropsychopharmacol 8: 1–16.
Newman-Tancredi A, Audinot V, Chaput C, Verriele L, Millan MJ (1997). [35S]Guanosine-5′-O-(3-thio)triphosphate binding as a measure of efficacy at human recombinant dopamine D4.4 receptors: actions of antiparkinsonian and antipsychotic agents. J Pharmacol Exp Ther 282: 181–191.
Newman-Tancredi A, Chaput C, Verriele L, Millan MJ (1996). Clozapine is a partial agonist at cloned, human serotonin 5-HT1A receptors. Neuropharmacology 35: 119–121.
Newman-Tancredi A, Cussac D, Audinot V, Pasteau V, Gavaudan S, Millan MJ (1999). G protein activation by human dopamine D3 receptors in high-expressing Chinese hamster ovary cells: a guanosine-5′-O-(3-[35S]thio)-triphosphate binding and antibody study. Mol Pharmacol 55: 564–574.
Newman-Tancredi A, Verriele L, Touzard M, Millan MJ (2001). Efficacy of antipsychotic agents at human 5-HT(1A) receptors determined by [3H]WAY100, 635 binding affinity ratios: relationship to efficacy for G-protein activation. Eur J Pharmacol 428: 177–184.
Nomikos GG, Iurlo M, Andersson JL, Kimura K, Svensson TH (1994). Systemic administration of amperozide, a new atypical antipsychotic drug, preferentially increases dopamine release in the rat medial prefrontal cortex. Psychopharmacol (Berlin) 115: 147–156.
Paxinos G, Watson C (1998). The Rat Brain In Stereotaxic Coordinates. Academic Press: New York.
Pehek EA, Meltzer HY, Yamamoto BK (1993). The atypical antipsychotic drug amperozide enhances rat cortical and striatal dopamine efflux. Eur J Pharmacol 240: 107–109.
Prinssen EP, Kleven MS, Koek W (1996). Effects of dopamine antagonists in a two-way active avoidance procedure in rats: interactions with 8-OH-DPAT, ritanserin, and prazosin. Psychopharmacology 128: 191–197.
Prinssen EP, Kleven MS, Koek W (1999). Interactions between neuroleptics and 5-HT(1A) ligands in preclinical behavioral models for antipsychotic and extrapyramidal effects. Psychopharmacology 144: 20–29.
Prinssen EP, Koek W, Colpaert FC, Kleven MS (2000). Repeated treatment with 8-OH-DPAT induces tolerance to its ability to produce the 5-HT1A behavioural syndrome, but not to its ability to attenuate haloperidol-induced catalepsy. Behav Pharmacol 11: 299–305.
Reynolds GP, Zhang ZJ, Zhang XB (2002). Association of antipsychotic drug-induced weight gain with a 5-HT2C receptor gene polymorphism. Lancet 359: 2086–2087.
Rollema H, Lu Y, Schmidt AW, Sprouse JS, Zorn SH (2000). 5-HT(1A) receptor activation contributes to ziprasidone-induced dopamine release in the rat prefrontal cortex. Biol Psychiatr 48: 229–237.
Rollema H, Lu Y, Schmidt AW, Zorn SH (1997). Clozapine increases dopamine release in prefrontal cortex by 5-HT1A receptor activation. Eur J Pharmacol 338: R3–R5.
Salomon Y, Londos C, Rodbell M (1974). A highly selective adenylate cyclase assay. Analyt Biochem 58: 541–548.
Seeman P, Lee T, Chau-Wong M, Wong K (1976). Antipsychotic drug doses and neuroleptic/dopamine receptors. Nature 261: 717–719.
Seidman LG, Kremen WS, Koren D, Faraone SV, Goldstein JM, Tsuang MT (2002). A comparative profile analysis of neuropsychological functioning in patients with schizophrenia and bipolar psychoses. Schizophren Res 53: 31–44.
Shen Y, Monsma FJ, Metcalf MA, Jose PA, Hamblin MW, Sibley DR (1993). Molecular cloning and expression of a 5-hydroxytryptamine7 serotonin receptor subtype. J Biol Chem 268: 18200–18204.
Shirazi-Southall S, Rodriguez DE, Nomikos GG (2002). Effects of typical and atypical antipsychotics and receptor selective compounds on acetylcholine efflux in the hippocampus of the rat. Neuropsychopharmacology 26: 583–594.
Sprouse JS, Reynolds LS, Braselton JP, Rollema H, Zorn SH (1999). Comparison of the novel antipsychotic ziprasidone with clozapine and olanzapine: inhibition of dorsal raphe cell firing and the role of 5-HT1A receptor activation. Neuropsychopharmacology 21: 622–631.
Sumiyoshi T, Matsui M, Nohara S, Yamashita I, Kurachi M, Sumiyoshi C et al (2001a). Enhancement of cognitive performance in schizophrenia by addition of tandospirone to neuroleptic treatment. Am J Psychiatr 158: 1722–1725.
Sumiyoshi T, Matsui M, Yamashita I, Nohara S, Kurachi M, Uehara T et al (2001b). The effect of tandospirone, a serotonin(1A) agonist, on memory function in schizophrenia. Biol Psychiatr 15: 861–868.
Tatsumi M, Groshan K, Blakeley RD, Richelson E (1997). Pharmacological profile of antidepressants and related compounds at human monoamine transporters. Eur J Pharmacol 340: 249–258.
Tricklebank MD, Forler C, Fozard JR (1984). The involvement of subtypes of the 5-HT1 receptor and of catecholaminergic systems in the behavioral response to 8-hydroxy-2-(di-n-propylamino)tetralin in the rat. Eur J Pharmacol 106: 271–282.
Uhlen S, Wikberg JE (1991). Rat spinal cord alpha 2-adrenoceptors are of the alpha2A-subtype: comparison with alpha2A- and alpha2B-adrenoceptors in rat spleen, cerebral cortex and kidney using 3H-RX821002 ligand binding. Pharmacol Toxicol 69: 341–350.
Van Tol HH, Wu CM, Guan HC, Ohara K, Bunzow JR, Civelli O et al (1992). Multiple DA D4 receptor variants in the human population. Nature 358: 149–152.
Wadenberg ML (1996). Serotonergic mechanisms in neuroleptic-induced catalepsy in the rat. Neurosci Biobehav Rev 20: 325–339.
Wadenberg ML, Ahlenius S (1991). Antipsychotic-like profile of combined treatment with raclopride and 8-OH-DPAT in the rat: enhancement of antipsychotic-like effects without catalepsy. J Neural Transm 83: 43–53.
Wadenberg ML, Young KA, Richter JT, Hicks PB (1999). Effects of local application of 5-hydroxytryptamine into the dorsal or median raphe nuclei on haloperidol-induced catalepsy in the rat. Neuropharmacology 38: 151–156.
Weinberger DR, Lipska BK (1995). Cortical maldevelopment, anti-psychotic drugs, and schizophrenia: a search for common ground. Schizophren Res 16: 87–110.
Weiss S, Sebben M, Bockaert JJ (1985). Corticotropin-peptide regulation of intracellular cyclic AMP production in cortical neurons in primary culture. J Neurochem 45: 869–874.
White FJ, Wang RY (1983). Differential effects of classical and atypical antipsychotic drugs on A9 and A10 dopamine neurons. Science 221: 1054–1057.
Winstanley CA, Chudasama Y, Dalley JW, Theobald DE, Glennon JC, Robbins TW (2003). Intra-prefrontal 8-OH-DPAT and M100907 improve visuospatial attention and decrease impulsivity on the five-choice serial reaction time task in rats. Psychopharmacology (Berlin) 167: 304–314.
Wolff MC, Wainscott DB, Nelson DL, Moore NA, Overshiner CD, Leander JD et al (2003). An in vivo assessment of aripiprazole, ziprasidone, risperidone and olanzapine in rat assays indicative of 5-HT1A and D2 receptor activity Schizophren. Research 60 (S 1): 119.
Yasuno F, Suhara T, Ichimiya T, Takano A, Ando T, Okubo Y (2004). Decreased 5-HT1A receptor binding in amygdala of schizophrenia. Biol Psychiatr 55: 439–444.
Yoshida K, Sugita T, Higuchi H, Hishikawa Y (1998). Effects of tandospirone on tardive dyskinesia and parkinsonian symptoms. Eur Psychol 13: 421–422.
Acknowledgements
We acknowledge the technical assistance of the in vitro and in vivo pharmacology research groups of Solvay Pharmaceuticals Research and the suggestions of Dr Karen Marquis of Wyeth Research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McCreary, A., Glennon, J., Ashby, C. et al. SLV313 (1-(2,3-Dihydro-Benzo[1,4]Dioxin-5-yl)-4- [5-(4-Fluoro-Phenyl)-Pyridin-3-ylmethyl]-Piperazine Monohydrochloride): A Novel Dopamine D2 Receptor Antagonist and 5-HT1A Receptor Agonist Potential Antipsychotic Drug. Neuropsychopharmacol 32, 78–94 (2007). https://doi.org/10.1038/sj.npp.1301098
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1301098
Keywords
This article is cited by
-
Spontaneous object recognition and its relevance to schizophrenia: a review of findings from pharmacological, genetic, lesion and developmental rodent models
Psychopharmacology (2012)
-
The effects of PRX-07034, a novel 5-HT6 antagonist, on cognitive flexibility and working memory in rats
Psychopharmacology (2012)
-
Comparative pharmacology of antipsychotics possessing combined dopamine D2 and serotonin 5-HT1A receptor properties
Psychopharmacology (2011)
-
Serotonin1A receptors in the pathophysiology of schizophrenia: development of novel cognition-enhancing therapeutics
Advances in Therapy (2008)
-
Differential profile of typical, atypical and third generation antipsychotics at human 5-HT7a receptors coupled to adenylyl cyclase: detection of agonist and inverse agonist properties
Naunyn-Schmiedeberg's Archives of Pharmacology (2007)