Abstract
Gaucher disease caused by hereditary deficiency of β-glucocerebrosidase is the most prevalent lysosomal storage disease. The incidence of the 5 commonest mutations was estimated in the Polish Gaucher disease population. A trial to establish genotype/phenotype correlations was performed. A relatively high frequency of type III disease can be stated in the studied Polish Gaucher patients. The most frequent mutation was L444P, followed by the N370S mutation. A distinct correlation between genotype and phenotype was observed in the studied group of Polish patients with Gaucher disease.
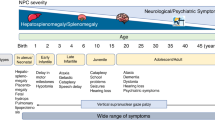
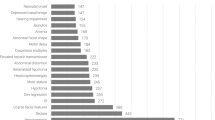
Similar content being viewed by others
Introduction
Gaucher disease, caused by hereditary deficiency of β-glucocerebrosidase, is the most prevalent lysosomal storage disease. The disorder presents a wide spectrum of clinical symptoms and is divided into three clinical forms: type I, non-neuronopathic (adult); type II, acute neuronopathic (infantile), and type III, subacute neuronopathic (juvenile) [1]. More than 50 mutations of the glucocerebrosidase gene have been reported [2]. Some of these mutations are more common, but their relative frequencies vary widely among ethnic groups [3–7]. Several authors have tried to establish genotype-phenotype correlations [2, 5–10]. These correlations have not proven to be unequivocal, but have permitted some useful generalizations [2].
Prior to this study, no mutation analysis had been performed in the Polish Gaucher disease population. We tested six of the most common mutations [3, 4]: 84 insG and 5 missense mutations. Missense mutation N370S and R463C are always found isolated; missense mutations D409H and L444P can be either isolated or a part of recombinant alleles between the gene and the pseudogene: RecNcil (it includes mutations L444P, A456P and V460V) and RecTL (which includes mutations D409H, L444P, A456P and V460V).
Materials and Methods
Genomic DNA of patients with type I or III Gaucher disease was extracted from blood samples by standard methods and tested for mutations.
Mutation 84 insG was studied by mismatched polymerase chain reaction (PCR) as described by Beutler et al. [11].
Mutations N370S, D409H, L444P, A456P and R463C: a 1,036-kb fragment of DNA extending from intron 8 to exon 11 was amplified by PCR using the primers: 5 AACCATGATTCCCTATCTTC3′ (sense primer) and 5′CTCCTCTAAGGATGTGCCTC3′ (antisense primer). The PCR product was specific for the gene since the sense primer was only partially homologous to the pseudogene. For each mutation, the PCR product was dotted on a membrane and hybridized with a pair of allele-specific oligonucleotides (ASO):
-
ASON370N: 5′ACCCTAGAACCTCCTGT3′
-
ASON370S: 5′ACCCTAGAGCCTCCTGT3′
-
ASOD409D: 5′ATCACCAAGGACACGTTTT3′
-
ASOD409H: 5′ATCACCAAGCACACGTTTT3′
-
ASOL444L: 5′CTGCGTCCAGGTCGTT3′
-
ASOL444P: 5′CTGCGTCCGGGTCGTT3′
-
ASOA456A: 5′GATGGCTCTGCTGTTGTGG3′
-
ASOA456P: 5′GATGGCTCTCCTGTTGTGG3′
-
ASOR463R: 5′GTGCTAAACCGGTGAGGGC3′
-
ASOR463P: 5′GTGCT AAACTGGTGAGGGC3′
Results and Discussion
Enzymatic diagnosis of Gaucher disease using leucocytes and fibroblasts has been possible in Poland since 1975 [12] and 34 patients have been diagnosed during the last 20 years: 18 with type I and 14 with types II and III. Among these patients, 22 are still alive: 8 have developed type III and 14 (from 11 families) have type I Gaucher disease (3 patients from the same family and 2 from another). Table 1 presents the patients’ clinical course and genotypes. The clinical examinations were performed by the same physician (A.T.-S.); the degree of clinical severity was established on the basis of the scoring index proposed by Zimran et al. [8]. There was no consanguinity among the parents. The majority of patients were from southern Poland. The frequency of the particular mutations was found to be: N370S, 26%; L444P, 37%; Rec-Ncil, 15%; 84 insG, 2%; unknown, 21%.
A relatively high frequency of type III disease can be stated in the studied Polish Gaucher disease population that derives from 19 families (8 families with type III, while there were only 11 families with type I).
Seven among the 8 patients with type III are homogenous for the L444P mutation. Interestingly, all of them are from southern Poland where the Polish population has not undergone the resettlement that affected other regions of the country. This situation is also observed in the case of other lysosomal storage diseases [12].
All of the patients with type III (L444P/L444P) exhibited marked bone involvement and hepatosplenomegaly. The IQ of two of these patients tested at the ages of 18 and 19 years was borderline normal/slightly deficient, while the IQ of 5 children with type III Gaucher disease tested at age 5–7 years was in the middle of the average range or above average. A retrospective comparison of the clinical pictures at age 5–7 years (early childhood) of 7 patients with type III and the L444P/L444P genotype showed an impressive similarity. In 3 patients with type III disease, severe bone deformation (very pronounced thoracic kyphosis) and progressive osteoporosis were found at the age of 16–19 years.
No homozygote for the N370S mutation was found among the patients with type I Gaucher disease. The reason for this may be the low frequency of identification of type I Gaucher disease, which often presents with very few or no symptoms at all. None of the studied persons declared Jewish ancestry, although we found one 84 insG mutation, which Horowitz and Zimran [3] believe to occur only among Ashkenazi Jews.
The frequency of N370S (23%) in the Polish population is comparable to that in other non-Jewish European populations [5, 7, 14]. Differing results were obtained only in Portugal, where a much higher frequency (60%) was reported [6].
We found very distinct similarities in the clinical picture among the affected siblings in the two type I Gaucher disease families.
Symptoms of Parkinson’s disease were found in one 47-year-old female patient in whom a mutation was not identified.
Patients with the N370 S/RecNcil genotype showed considerable similarities with each other in the clinical picture and course of the disease, with characteristic slight or lack of bone involvement and a generally more mild course of the disease.
A distinct correlation between genotype and phenotype was observed in the studied group of Polish patients with Gaucher disease. This was particularly evident in patients with type I disease and the N370 S/RecNcil genotype and in patients with type III disease and the L444P/L444P genotype. In the latter group, the course of the disease in the successive periods of life of these patients was strikingly similar. These observations differ from those of other authors, e.g. Rice et al. [15] or Sidansky et al. [10, 13], who did not find clear relationships between genotype and phenotype in non-Jewish populations. The Polish population may be more homogenous than the American population. The fact that significant differences were found between genotype and phenotype in comparisons of Japanese and non-Jewish patients with Gaucher disease may suggest the effect of ethnic or other than genetic factors on the clinical picture [7].
References
Beutler E, Grabowski GA: Gaucher disease; in Scriver CR, Beaudet AL, Sly WS, Valle D (eds): The Metabolic and Molecular Bases of Inherited Disease, ed 7. New York, McGraw-Hill, 1995, pp 2641–2670.
NIH Technology Assessment Panel on Gaucher disease: Gaucher Disease. JAMA 1996;275:548–553
Horowitz M, Zimran A: Mutations causing Gaucher disease. Hum Mut 1994;3:1–11
Beutler E, Gelbart T: Gaucher disease mutations in non-Jewish patients. Br J Haematol 1993;85:401–405
Walley A, Barth ML, Ellis I, Fensom A, Harris A: Gaucher’s disease in the United Kingdom: Screening non-Jewish patients for the two common mutations. J Med Genet 1993;30:280–283
Amaral O, Fortuna AM, Lacerda L, Pinto R, Sa Mirand AMC: Molecular characterisation of type 1 Gaucher disease families and patients: Intra-familial heterogeneity at the clinical level. J Med Genet 1994;31:401–404
Ida H, Iwasawa A, Kawame H, Rennert OM, Maekawa K, Eto Y: Characteristics of gene mutations among 32 unrelated Japanese Gaucher disease patients: Absence of the common Jewish 84GG and 1226G mutations. Hum Genet 1995;95:717–720
Zimran A, Gross E, West C, Sorge J, Kubitz M, Beutler E: Prediction of severity of Gaucher’s disease by identification of mutations at DNA level. Lancet 1989;ii:349–352
Strasberg P, Triggs-Raine B, Warren I, Skomorowski MA, McInnes B, Becker L, Callahan J, Clarke J: Genotype-phenotype pitfalls in Gaucher disease. J Clin Lab Analysis 1994;8:228–236
Sidransky E, Bottler A, Stubbelfield B, Ginns EJ: DNA mutational analysis of type 1 and type 3 Gaucher patients: How well do mutations predict phenotype? Hum Mut 1994;3:25–28
Beutler E, Gelbart T, Kuhl W, Sorge J, West C: Identification of the second common Jewish Gaucher disease mutation makes possible population-based screening for the heterozygous state. Proc Natl Acad Sci USA 1991;88:10544–10547
Czartoryska B, Tylki-Szymańska A, Górska D, Sawnor-Korszyńska D: Lipidoses detected in Poland through 1993. Pediatr Neurol 1994;11:295–297
Sidransky E, Tsuji S, Stubblefield BK, Currie J, FitzGibbon E, Gins E: Gaucher patients with oculomotor abnormalities do not have a unique genotype. Clin Genet 1992;41:1–5
Michelakakis H, Dimitriou E, Van Weely S, Boot RG, Mavridon I, Verhoek M, Aerts JMFG: Characterization of glucocerebrosidase in Greek Gaucher disease patients: Mutation analysis and biochemical studies. J Inher Metab Dis 1995;18:609–615
Rice EO, Hifflin TE, Sokallah S, Lee RE, Sansieri CA, Barranger JA: Gaucher disease: Studies of phenotype molecular diagnosis and treatment. Clin Genet 1996;49:111–118
Acknowledgements
This work was supported by grants 290/P05/95 from the Polish Committee for Scientific Research. Genzyme provided assistance in the determination of genotypes.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Tylki-Szymańska, A., Millat, G., Maire, I. et al. Types I and III Gaucher Disease in Poland: Incidence of the Most Common Mutations and Phenotypic Manifestations. Eur J Hum Genet 4, 334–337 (1996). https://doi.org/10.1159/000472228
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1159/000472228
Key Words
This article is cited by
-
‘Non-neuronopathic’ Gaucher disease reconsidered. Prevalence of neurological manifestations in a Dutch cohort of type I Gaucher disease patients and a systematic review of the literature
Journal of Inherited Metabolic Disease (2008)
-
Gaucher disease in Romanian patients: incidence of the most common mutations and phenotypic manifestations
European Journal of Human Genetics (2002)