Abstract
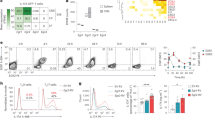
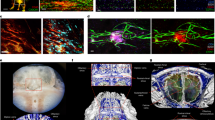
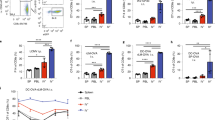
Interleukin 17–producing T helper cells (TH-17 cells) are important in experimental autoimmune encephalomyelitis, but their route of entry into the central nervous system (CNS) and their contribution relative to that of other effector T cells remain to be determined. Here we found that mice lacking CCR6, a chemokine receptor characteristic of TH-17 cells, developed TH-17 responses but were highly resistant to the induction of experimental autoimmune encephalomyelitis. Disease susceptibility was reconstituted by transfer of wild-type T cells that entered into the CNS before disease onset and triggered massive CCR6-independent recruitment of effector T cells across activated parenchymal vessels. The CCR6 ligand CCL20 was constitutively expressed in epithelial cells of choroid plexus in mice and humans. Our results identify distinct molecular requirements and ports of lymphocyte entry into uninflamed versus inflamed CNS and suggest that the CCR6-CCL20 axis in the choroid plexus controls immune surveillance of the CNS.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
McGeachy, M.J. & Cua, D.J. Th17 cell differentiation: the long and winding road. Immunity 28, 445–453 (2008).
Bettelli, E., Korn, T., Oukka, M. & Kuchroo, V.K. Induction and effector functions of TH17 cells. Nature 453, 1051–1057 (2008).
Dong, C. TH17 cells in development: an updated view of their molecular identity and genetic programming. Nat. Rev. Immunol. 8, 337–348 (2008).
Weaver, C.T., Hatton, R.D., Mangan, P.R. & Harrington, L.E. IL-17 family cytokines and the expanding diversity of effector T cell lineages. Annu. Rev. Immunol. 25, 821–852 (2007).
Gaffen, S.L. An overview of IL-17 function and signaling. Cytokine 43, 402–407 (2008).
Steinman, L. A brief history of TH17, the first major revision in the TH1/TH2 hypothesis of T cell-mediated tissue damage. Nat. Med. 13, 139–145 (2007).
Ivanov, I.I. et al. The orphan nuclear receptor RORγt directs the differentiation program of proinflammatory IL-17+ T helper cells. Cell 126, 1121–1133 (2006).
Komiyama, Y. et al. IL-17 plays an important role in the development of experimental autoimmune encephalomyelitis. J. Immunol. 177, 566–573 (2006).
Hofstetter, H.H. et al. Therapeutic efficacy of IL-17 neutralization in murine experimental autoimmune encephalomyelitis. Cell. Immunol. 237, 123–130 (2005).
Langrish, C.L. et al. IL-23 drives a pathogenic T cell population that induces autoimmune inflammation. J. Exp. Med. 201, 233–240 (2005).
Tzartos, J.S. et al. Interleukin-17 production in central nervous system-infiltrating T cells and glial cells is associated with active disease in multiple sclerosis. Am. J. Pathol. 172, 146–155 (2008).
Bettelli, E. et al. Loss of T-bet, but not STAT1, prevents the development of experimental autoimmune encephalomyelitis. J. Exp. Med. 200, 79–87 (2004).
Luger, D. et al. Either a Th17 or a Th1 effector response can drive autoimmunity: conditions of disease induction affect dominant effector category. J. Exp. Med. 205, 799–810 (2008).
Kroenke, M.A., Carlson, T.J., Andjelkovic, A.V. & Segal, B.M. IL-12- and IL-23-modulated T cells induce distinct types of EAE based on histology, CNS chemokine profile, and response to cytokine inhibition. J. Exp. Med. 205, 1535–1541 (2008).
Stromnes, I.M., Cerretti, L.M., Liggitt, D., Harris, R.A. & Goverman, J.M. Differential regulation of central nervous system autoimmunity by TH1 and TH17 cells. Nat. Med. 14, 337–342 (2008).
Lees, J.R., Golumbek, P.T., Sim, J., Dorsey, D. & Russell, J.H. Regional CNS responses to IFN-γ determine lesion localization patterns during EAE pathogenesis. J. Exp. Med. 205, 2633–2642 (2008).
Engelhardt, B. & Ransohoff, R.M. The ins and outs of T-lymphocyte trafficking to the CNS: anatomical sites and molecular mechanisms. Trends Immunol. 26, 485–495 (2005).
Yednock, T.A. et al. Prevention of experimental autoimmune encephalomyelitis by antibodies against α4β1 integrin. Nature 356, 63–66 (1992).
Engelhardt, B., Vestweber, D., Hallmann, R. & Schulz, M. E- and P-selectin are not involved in the recruitment of inflammatory cells across the blood-brain barrier in experimental autoimmune encephalomyelitis. Blood 90, 4459–4472 (1997).
Carrithers, M.D., Visintin, I., Kang, S.J. & Janeway, C.A. Jr. Differential adhesion molecule requirements for immune surveillance and inflammatory recruitment. Brain 123, 1092–1101 (2000).
Piccio, L. et al. Molecular mechanisms involved in lymphocyte recruitment in inflamed brain microvessels: critical roles for P-selectin glycoprotein ligand-1 and heterotrimeric Gi-linked receptors. J. Immunol. 168, 1940–1949 (2002).
Vajkoczy, P., Laschinger, M. & Engelhardt, B. α4-integrin-VCAM-1 binding mediates G protein-independent capture of encephalitogenic T cell blasts to CNS white matter microvessels. J. Clin. Invest. 108, 557–565 (2001).
Engelhardt, B., Wolburg-Buchholz, K. & Wolburg, H. Involvement of the choroid plexus in central nervous system inflammation. Microsc. Res. Tech. 52, 112–129 (2001).
Ransohoff, R.M., Kivisakk, P. & Kidd, G. Three or more routes for leukocyte migration into the central nervous system. Nat. Rev. Immunol. 3, 569–581 (2003).
Giunti, D. et al. Phenotypic and functional analysis of T cells homing into the CSF of subjects with inflammatory diseases of the CNS. J. Leukoc. Biol. 73, 584–590 (2003).
Steffen, B.J., Breier, G., Butcher, E.C., Schulz, M. & Engelhardt, B. ICAM-1, VCAM-1, and MAdCAM-1 are expressed on choroid plexus epithelium but not endothelium and mediate binding of lymphocytes in vitro. Am. J. Pathol. 148, 1819–1838 (1996).
Pedemonte, E. et al. Mechanisms of the adaptive immune response inside the central nervous system during inflammatory and autoimmune diseases. Pharmacol. Ther. 111, 555–566 (2006).
Bromley, S.K., Mempel, T.R. & Luster, A.D. Orchestrating the orchestrators: chemokines in control of T cell traffic. Nat. Immunol. 9, 970–980 (2008).
Rossi, D.L., Vicari, A.P., Franz-Bacon, K., McClanahan, T.K. & Zlotnik, A. Identification through bioinformatics of two new macrophage proinflammatory human chemokines: MIP-3α and MIP-3β. J. Immunol. 158, 1033–1036 (1997).
Acosta-Rodriguez, E.V. et al. Surface phenotype and antigenic specificity of human interleukin 17–producing T helper memory cells. Nat. Immunol. 8, 639–646 (2007).
Cook, D.N. et al. CCR6 mediates dendritic cell localization, lymphocyte homeostasis, and immune responses in mucosal tissue. Immunity 12, 495–503 (2000).
Greaves, D.R. et al. CCR6, a CC chemokine receptor that interacts with macrophage inflammatory protein 3α and is highly expressed in human dendritic cells. J. Exp. Med. 186, 837–844 (1997).
Brown, D.A. & Sawchenko, P.E. Time course and distribution of inflammatory and neurodegenerative events suggest structural bases for the pathogenesis of experimental autoimmune encephalomyelitis. J. Comp. Neurol. 502, 236–260 (2007).
Kivisakk, P. et al. Localizing central nervous system immune surveillance: Meningeal antigen-presenting cells activate T cells during experimental autoimmune encephalomyelitis. Ann. Neurol. published online, doi:10.1002/ana.21379 (21 May 2008).
Hickey, W.F., Hsu, B.L. & Kimura, H. T-lymphocyte entry into the central nervous system. J. Neurosci. Res. 28, 254–260 (1991).
Flugel, A. et al. Migratory activity and functional changes of green fluorescent effector cells before and during experimental autoimmune encephalomyelitis. Immunity 14, 547–560 (2001).
Hirota, K. et al. Preferential recruitment of CCR6-expressing Th17 cells to inflamed joints via CCL20 in rheumatoid arthritis and its animal model. J. Exp. Med. 204, 2803–2812 (2007).
Khader, S.A. et al. IL-23 and IL-17 in the establishment of protective pulmonary CD4+ T cell responses after vaccination and during Mycobacterium tuberculosis challenge. Nat. Immunol. 8, 369–377 (2007).
Steinman, L. A few autoreactive cells in an autoimmune infiltrate control a vast population of nonspecific cells: a tale of smart bombs and the infantry. Proc. Natl. Acad. Sci. USA 93, 2253–2256 (1996).
O'Connor, R.A. et al. Cutting Edge: Th1 cells facilitate the entry of Th17 cells to the central nervous system during experimental autoimmune encephalomyelitis. J. Immunol. 181, 3750–3754 (2008).
Kebir, H. et al. Human TH17 lymphocytes promote blood-brain barrier disruption and central nervous system inflammation. Nat. Med. 13, 1173–1175 (2007).
Kreymborg, K. et al. IL-22 is expressed by Th17 cells in an IL-23-dependent fashion, but not required for the development of autoimmune encephalomyelitis. J. Immunol. 179, 8098–8104 (2007).
Haak, S. et al. IL-17A and IL-17F do not contribute vitally to autoimmune neuro-inflammation in mice. J. Clin. Invest. 119, 61–69 (2009).
Charo, I.F. & Ransohoff, R.M. The many roles of chemokines and chemokine receptors in inflammation. N. Engl. J. Med. 354, 610–621 (2006).
Balashov, K.E., Rottman, J.B., Weiner, H.L. & Hancock, W.W. CCR5+ and CXCR3+ T cells are increased in multiple sclerosis and their ligands MIP-1α and IP-10 are expressed in demyelinating brain lesions. Proc. Natl. Acad. Sci. USA 96, 6873–6878 (1999).
Ambrosini, E., Columba-Cabezas, S., Serafini, B., Muscella, A. & Aloisi, F. Astrocytes are the major intracerebral source of macrophage inflammatory protein-3α/CCL20 in relapsing experimental autoimmune encephalomyelitis and in vitro. Glia 41, 290–300 (2003).
Columba-Cabezas, S., Serafini, B., Ambrosini, E. & Aloisi, F. Lymphoid chemokines CCL19 and CCL21 are expressed in the central nervous system during experimental autoimmune encephalomyelitis: implications for the maintenance of chronic neuroinflammation. Brain Pathol. 13, 38–51 (2003).
Rottman, J.B. et al. Leukocyte recruitment during onset of experimental allergic encephalomyelitis is CCR1 dependent. Eur. J. Immunol. 30, 2372–2377 (2000).
Muller, M. et al. CXCR3 signaling reduces the severity of experimental autoimmune encephalomyelitis by controlling the parenchymal distribution of effector and regulatory T cells in the central nervous system. J. Immunol. 179, 2774–2786 (2007).
Liu, L. et al. Severe disease, unaltered leukocyte migration, and reduced IFN-γ production in CXCR3−/− mice with experimental autoimmune encephalomyelitis. J. Immunol. 176, 4399–4409 (2006).
Gaupp, S., Pitt, D., Kuziel, W.A., Cannella, B. & Raine, C.S. Experimental autoimmune encephalomyelitis (EAE) in CCR2−/− mice: susceptibility in multiple strains. Am. J. Pathol. 162, 139–150 (2003).
Eltayeb, S. et al. Temporal expression and cellular origin of CC chemokine receptors CCR1, CCR2 and CCR5 in the central nervous system: insight into mechanisms of MOG-induced EAE. J. Neuroinflammation 4, 14 (2007).
Matsui, M. et al. Treatment of experimental autoimmune encephalomyelitis with the chemokine receptor antagonist Met-RANTES. J. Neuroimmunol. 128, 16–22 (2002).
Kohler, R.E., Caon, A.C., Willenborg, D.O., Clark-Lewis, I. & McColl, S.R. A role for macrophage inflammatory protein-3α/CC chemokine ligand 20 in immune priming during T cell-mediated inflammation of the central nervous system. J. Immunol. 170, 6298–6306 (2003).
Franciotta, D., Salvetti, M., Lolli, F., Serafini, B. & Aloisi, F. B cells and multiple sclerosis. Lancet Neurol. 7, 852–858 (2008).
Kleinewietfeld, M. et al. CCR6 expression defines regulatory effector/memory-like cells within the CD25+CD4+ T-cell subset. Blood 105, 2877–2886 (2005).
Yamazaki, T. et al. CCR6 regulates the migration of inflammatory and regulatory T cells. J. Immunol. 181, 8391–8401 (2008).
Steinman, L. A rush to judgment on Th17. J. Exp. Med. 205, 1517–1522 (2008).
Sigmundsdottir, H. & Butcher, E.C. Environmental cues, dendritic cells and the programming of tissue-selective lymphocyte trafficking. Nat. Immunol. 9, 981–987 (2008).
Hickey, W.F. Basic principles of immunological surveillance of the normal central nervous system. Glia 36, 118–124 (2001).
Acknowledgements
We thank D. Jarrossay for cell sorting; T. Périnat and S. Minghelli for immunohistology analysis; E. Mira Catò and L. Perlini for technical assistance; B. Becher (University Hospital Zurich), C. Gerard (Harvard Medical School), J. Kirberg (Max-Plank Institute of Immunobiology) and M. Lipp (Max Delbruck Center) for mouse strains; L. Sallusto for discussions and support; and A. Almeida, A. Martín-Fontecha, G. Napolitani, U. Schenk and M. Uguccioni for discussions. Supported by the Swiss National Science Foundation (31-101962 to F.S.), the European Commission Sixth Framework Programme (LSB-CT-2005-518167 IINOCHEM and LSHG-CT-2005-005203 MUGEN), the US National Multiple Sclerosis Society (B.E. and C.C.), the Swiss Multiple Sclerosis Society, the Italian Foundation for Multiple Sclerosis (Stem Cell Project 2007-2009), the European Union-funded International Graduate Program in Molecular Medicine (A.R.), Boehringer Ingelheim Fonds (D.B.) and the Helmut Horten Foundation (to The Institute for Research in Biomedicine).
Author information
Authors and Affiliations
Contributions
A.R. did most of the experiments and contributed to experimental design; C.C., D. Baumjohann, F.B. and D. Bottinelli did experiments; S.L. generated the CCR6-knockout mice and provided intellectual input; B.E. and A.U. interpreted data, provided intellectual input and contributed to writing the manuscript; A.L. provided intellectual input and wrote the manuscript; and F.S. conceived the study, interpreted the data and wrote the manuscript.
Corresponding author
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–3 and Supplementary Methods (PDF 577 kb)
Rights and permissions
About this article
Cite this article
Reboldi, A., Coisne, C., Baumjohann, D. et al. C-C chemokine receptor 6–regulated entry of TH-17 cells into the CNS through the choroid plexus is required for the initiation of EAE. Nat Immunol 10, 514–523 (2009). https://doi.org/10.1038/ni.1716
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.1716