Abstract
Objective:
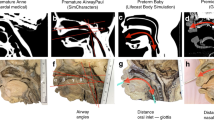
Proficiency in airway management is critical for neonatal health-care professionals. Simulation is a proven method to improve airway management skills. Skills transfer from simulation to the real life requires simulators with appropriate physical and functional fidelity.
Study design:
A cohort of neonatal health-care professionals evaluated eight different neonatal airway simulators for physical and functional fidelity.
Result:
Twenty-seven subjects completed 151 simulator evaluations. Significant differences were found between the simulators evaluated (P<0.001). The manikins with the highest fidelity scores were the SimNewB, Newborn Anne and Premature Anne (Laerdal Medical). The task trainers with the highest fidelity scores were the Neonatal Intubation Trainer (Laerdal Medical) and the Newborn Airway Trainer (Syndaver Labs).
Conclusion:
Simulator fidelity is an important aspect of simulation training, but is rarely evaluated. The results of this study can aid in choosing the best simulators for training and research, and provide feedback to the industry to guide future simulator development.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Program Requirements for Graduate Medical Education in Pediatrics. Accreditation Council for Graduate Medical Education (ACGME). Available at https://www.acgme.org/acgmeweb/Portals/0/PFAssets/2013-PR-FAQ-PIF/320_pediatrics_07012013.pdf (accesssed 1 July 2013).
Program Requirements for Graduate Medical Education in Neonatal-Perinatal Medicine. Accreditation Council for Graduate Medical Education (ACGME). Available at https://www.acgme.org/acgmeweb/portals/0/pfassets/2013-pr-faq-pif/329_neonatal_perinatal_peds_07012013.pdf (accessed 1 July 2013).
Leone TA, Rich W, Finer. NN . Neonatal intubation: success of pediatric trainees. J Pediatr 2005; 146 (5): 638–641.
Downes K, Narendran V, Meinzen-Derr J, McClanahan S, Akinbi H . The lost art of intubation: assessing opportunities for residents to perform neonatal intubation. J Perinatol 2012; 32: 927–932.
DeLaroche A, Riggs T, Maisels MJ . Impact of the new 16- hour duty period on pediatric interns' neonatal education. Clin Pediatr (Phila) 2014; 53 (1): 51–59.
Lopreiato J, Sawyer T . Simulation-based medical education in pediatrics. Acad Pediatr 2015; 15 (2): 134–142.
Kennedy CC, Cannon EK, Warner DO, Cook DA . Advanced airway management simulation training in medical education: a systematic review and meta-analysis. Crit Care Med 2014; 42 (1): 169–178.
Passiment M, Sacks H, Huang G . Medical Simulation in Medical Education: Results of an AAMC Survey. Association of American Medical Colleges: Washington, DC, 2011.
Johnson L, Mu T, Sawyer T . Use of medical simulation in neonatal-perinatal fellowship training programs. J Neonatal Perinatal Med 2012; 5 (4): 339–345.
Hamstra SJ, Brydges R, Hatala R, Zendejas B, Cook DA . Reconsidering fidelity in simulation-based training. Acad Med 2014; 89 (3): 387–392.
Maran NJ, Glavin RJ . Low-to high-fidelity simulation—a continuum of medical education? Med Educ 2003; 37 (Suppl 1): 22–28.
Curtis M, DiazGranados D, Feldman M . Judicious use of simulation technology in continuing medical education. J Contin Educ Health Prof 2012; 32 (4): 255–260.
Gagné RM . Training devices and simulators: some research issues. Am Psychol 1954; 9 (7): 95–107.
Schebesta K, Hüpfl M, Rössler B, Ringl H, Müller MP, Kimberger O . Degrees of reality: airway anatomy of high-fidelity human patient simulators and airway trainers. Anesthesiology 2012; 116 (6): 1204–1209.
Schebesta K, Hüpfl M, Ringl H, Machata AM, Chiari A, Kimberger O . A comparison of paediatric airway anatomy with the SimBaby high-fidelity patient simulator. Resuscitation 2011; 82 (4): 468–472.
Klotz JJ, Dooley-Hash SL, House JB, Andreatta PB . Pediatric and neonatal intubation training gap analysis: instruction, assessment, and technology. Simul Healthc 2014; 9 (6): 377–383.
Bajka M, Tuchschmid S, Streich M, Fink D, Székely G, Harders M . Evaluation of a new virtual-reality training simulator for hysteroscopy. Surg Endosc 2009; 23 (9): 2026–2033.
Barsness K, Rooney D, Davis L . Collaboration in simulation: the development and initial validation of a novel thoracoscopic neonatal simulator. J Pediatr Surg 2013; 48: 1232–1238.
Sullivan G, Artino A . Analyzing and interpreting data from likert-type scales. J Grad Med Educ 2013; 5 (4): 541–542.
Trevisanuto D, Parotto M, Doglioni N, Ori C, Zanardo V, Micaglio M . The supreme Laryngeal Mask Airway™ (LMA): a new neonatal supraglottic device: comparison with Classic and ProSeal LMA in a manikin. Resuscitation 2012; 83 (1): 97–100.
Micaglio M, Doglioni N, Parotto M, Zanardo V, Ori C, Trevisanuto D . Training for neonatal resuscitation with the laryngeal mask airway: a comparison of the LMA-ProSeal and the LMA-Classic in an airway management manikin. Paediatr Anaesth 2006; 16 (10): 1028–1031.
Micaglio M, Trevisanuto D, Doglioni N, Zanette G, Zanardo V, Ori C . The size 1 LMA-ProSeal: comparison with the LMA-Classic during pressure controlled ventilation in a neonatal intubation manikin. Resuscitation 2007; 72 (1): 124–127.
Saracoglu KT, Eti Z, Kavas AD, Umuroglu T . Straight video blades are advantageous than curved blades in simulated pediatric difficult intubation. Paediatr Anaesth 2014; 24 (3): 297–302.
Kalbhenn J, Boelke AK, Steinmann D . Prospective model-based comparison of different laryngoscopes for difficult intubation in infants. Paediatr Anaesth 2012; 22 (8): 776–780.
McGaghie WC . Simulation in professional competence assessment: basic considerations. In: Tekian A, McGuire CH, McGaghie WC (eds). Innovative Simulations for Assessing Professional Competence. Department of Medical Education, University of Illinois at Chicago: Chicago, USA, 1999, pp 7–22.
Acknowledgements
We thank the neonatal fellows, neonatal nurse practitioners and neonatologists in the University of Washington, Division of Neonatology for their participation in the study. The Premature Anne manikin used in this study was provided to the investigators on educational loan from Laerdal Medical before its commercial release. All other simulators used in this investigations were previously purchased and owned by the University of Washington Neonatal Education and Simulation-based Training (NEST) Program, or the University of Washington Institute for Simulation and Interprofessional Studies.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Sawyer, T., Strandjord, T., Johnson, K. et al. Neonatal airway simulators, how good are they? A comparative study of physical and functional fidelity. J Perinatol 36, 151–156 (2016). https://doi.org/10.1038/jp.2015.161
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2015.161
This article is cited by
-
Creation of a rating scale to teach Less Invasive Surfactant Administration (LISA) in simulation
BMC Medical Education (2024)
-
Anatomic accuracy, physiologic characteristics, and fidelity of very low birth weight infant airway simulators
Pediatric Research (2022)
-
Creating a Validated Simulation Training Curriculum in Otolaryngology
Current Otorhinolaryngology Reports (2020)
-
Accuracy of the nasal-tragus length measurement for correct endotracheal tube placement in a cohort of neonatal resuscitation simulators
Journal of Perinatology (2017)
-
Real vs simulated umbilical cords for emergency umbilical catheterization training: a randomized crossover study
Journal of Perinatology (2017)