Abstract
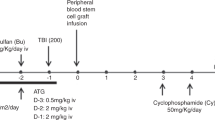
Inadequate T-cell chimerism following reduced-intensity conditioning transplantation may contribute to graft rejection and disease relapse. Anti-thymocyte globulin (ATG) enhances early donor T-cell chimerism, but may also deplete donor T cells, increasing risks of infection and relapse. We prospectively tested administration of rabbit ATG (rATG) ⩾14 days before the infusion of the graft, followed by in vivo decay of active rATG levels, to selectively deplete host T cells. Twenty-three patients received rATG total dose 4.5 mg/kg on days −16 and −15, fludarabine 30 mg/m2 per day on day −7 through −3, IV busulfan 130 mg/m2 per day on days −4 and −3 and cyclophosphamide 1500 mg/m2 on day −2. rATG levels were therapeutic in all patients on day −14, but were sub-therapeutic (<1 μg/mL) by day 0 in 82% of patients. Median donor T-cell chimerisms on days 30 and 180 were 100% (75–100%) and 100% (90–100%), respectively. Non-relapse mortality and relapse/progression at 48 months were 17 and 30%. Cumulative incidences of acute GvHD grades II–IV and III–IV were 39 and 9%. Median follow-up is 64 months (46–79 months). Survival and disease-free survival at 48 months were 70 and 52%. These data suggest that selective depletion of host T cells using this regimen is a feasible and effective strategy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bashey A, Owzar K, Johnson JL, Edwards PS, Kelly M, Baxter-Lowe LA et al. Reduced-intensity conditioning allogeneic hematopoietic cell transplantation for patients with hematologic malignancies who relapse following autologous transplantation: a multi-institutional prospective study from the Cancer and Leukemia Group B (CALGB trial 100002). Biol Blood Marrow Transplant 2011; 17: 558–565.
Niiya H, Kanda Y, Saito T, Ohnishi T, Kanai S, Kawano Y et al. Early full donor myeloid chimerism after reduced-intensity stem cell transplantation using a combination of fludarabine and busulfan. Haematologica 2001; 86: 1071–1074.
Valcarcel D, Martino R, Caballero D, Mateos MV, Perez-Simon JA, Canals C et al. Chimerism analysis following allogeneic peripheral blood stem cell transplantation with reduced-intensity conditioning. Bone Marrow Transplant 2003; 31: 387–392.
Baron F, Sandmaier BM . Chimerism and outcomes after allogeneic hematopoietic cell transplantation following nonmyeloablative conditioning. Leukemia 2006; 20: 1690–1700.
Keil F, Prinz E, Moser K, Mannhalter C, Kalhs P, Worel N et al. Rapid establishment of long-term culture-initiating cells of donor origin after nonmyeloablative allogeneic hematopoietic stem-cell transplantation, and significant prognostic impact of donor T-cell chimerism on stable engraftment and progression-free survival. Transplantation 2003; 76: 230–236.
Mohty M, Avinens O, Faucher C, Viens P, Blaise D, Eliaou JF . Predictive factors and impact of full donor T-cell chimerism after reduced intensity conditioning allogeneic stem cell transplantation. Haematologica 2007; 92: 1004–1006.
Saito B, Fukuda T, Yokoyama H, Kurosawa S, Takahashi T, Fuji S et al. Impact of T cell chimerism on clinical outcome in 117 patients who underwent allogeneic stem cell transplantation with a busulfan-containing reduced-intensity conditioning regimen. Biol Blood Marrow Transplant 2008; 14: 1148–1155.
Breuer S, Preuner S, Fritsch G, Daxberger H, Koenig M, Poetschger U et al. Early recipient chimerism testing in the T- and NK-cell lineages for risk assessment of graft rejection in pediatric patients undergoing allogeneic stem cell transplantation. Leukemia 2012; 26: 509–519.
Koreth J, Kim HT, Nikiforow S, Milford EL, Armand P, Cutler C et al. Donor chimerism early after reduced-intensity conditioning hematopoietic stem cell transplantation predicts relapse and survival. Biol Blood Marrow Transplant 2014; 20: 1516–1521.
Soiffer RJ, Lerademacher J, Ho V, Kan F, Artz A, Champlin RE et al. Impact of immune modulation with anti-T-cell antibodies on the outcome of reduced-intensity allogeneic hematopoietic stem cell transplantation for hematologic malignancies. Blood 2011; 117: 6963–6970.
Baron F, Labopin M, Blaise D, Lopez-Corral L, Vigouroux S, Craddock C et al. Impact of in vivo T-cell depletion on outcome of AML patients in first CR given peripheral blood stem cells and reduced-intensity conditioning allo-SCT from a HLA-identical sibling donor: a report from the Acute Leukemia Working Party of the European Group for Blood and Marrow Transplantation. Bone Marrow Transplant 2014; 49: 389–396.
Remberger M, Ringden O, Hagglund H, Svahn BM, Ljungman P, Uhlin M et al. A high antithymocyte globulin dose increases the risk of relapse after reduced intensity conditioning HSCT with unrelated donors. Clin Transplant 2013; 27: E368–E374.
Waller EK, Langston AA, Lonial S, Cherry J, Somani J, Allen AJ et al. Pharmacokinetics and pharmacodynamics of anti-thymocyte globulin in recipients of partially HLA-matched blood hematopoietic progenitor cell transplantation. Biol Blood Marrow Transplant 2003; 9: 460–471.
Buchler M, Longuet H, Lemoine R, Herr F, Gatault P, Thibault G et al. Pharmacokinetic and pharmacodynamic studies of two different rabbit antithymocyte globulin dosing regimens: results of a randomized trial. Transpl Immunol 2013; 28: 120–126.
Filipovich AH, Weisdorf D, Pavletic S, Socie G, Wingard JR, Lee SJ et al. National Institutes of Health consensus development project on criteria for clinical trials in chronic graft-versus-host disease: I. Diagnosis and staging working group report. Biol Blood Marrow Transplant 2005; 11: 945–956.
Lowsky R, Takahashi T, Liu YP, Dejbakhsh-Jones S, Grumet FC, Shizuru JA et al. Protective conditioning for acute graft-versus-host disease. N Engl J Med 2005; 353: 1321–1331.
Rupa-Matysek J, Lewandowski K, Nowak W, Sawinski K, Gil L, Komarnicki M . Correlation between the kinetics of CD3+ chimerism and t he incidence of graft-versus-host disease in patients undergoing allogeneic hematopoietic stem cell transplantation. Transplant Proc 2011; 43: 1915–1923.
Cutler C, Kim HT, Bindra B, Sarantopoulos S, Ho VT, Chen YB et al. Rituximab prophylaxis prevents corticosteroid-requiring chronic GVHD after allogeneic peripheral blood stem cell transplantation: results of a phase 2 trial. Blood 2013; 122: 1510–1517.
Koreth J, Stevenson KE, Kim HT, Garcia M, Ho VT, Armand P et al. Bortezomib, tacrolimus, and methotrexate for prophylaxis of graft-versus-host disease after reduced-intensity conditioning allogeneic stem cell transplantation from HLA-mismatched unrelated donors. Blood 2009; 114: 3956–3959.
Acknowledgements
This research was supported by a grant from Genzyme Corporation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
This research was supported by a grant from Genzyme Corporation to assist with data management. There are no other potential conflicts of interest to declare.
Rights and permissions
About this article
Cite this article
Sanacore, M., Zhang, X., Brown, S. et al. Preferential depletion of host over donor T cells through in vivo decay of active rabbit-anti-thymocyte globulin levels during reduced intensity conditioning. Bone Marrow Transplant 50, 829–833 (2015). https://doi.org/10.1038/bmt.2015.41
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2015.41