Abstract
Vascular calcification powerfully predicts mortality and morbidity from cardiovascular disease. Men have a greater risk of cardiovascular disease, compared to women of a similar age. These gender disparities suggest an influence of sex hormones. Testosterone is the primary and most well-recognised androgen in men. Therefore, we addressed the hypothesis that exogenous androgen treatment induces vascular calcification. Immunohistochemical analysis revealed expression of androgen receptor (AR) in the calcified media of human femoral artery tissue and calcified human valves. Furthermore, in vitro studies revealed increased phosphate (Pi)-induced mouse vascular smooth muscle cell (VSMC) calcification following either testosterone or dihydrotestosterone (DHT) treatment for 9 days. Testosterone and DHT treatment increased tissue non-specific alkaline phosphatase (Alpl) mRNA expression. Testosterone-induced calcification was blunted in VSMC-specific AR-ablated (SM-ARKO) VSMCs compared to WT. Consistent with these data, SM-ARKO VSMCs showed a reduction in Osterix mRNA expression. However, intriguingly, a counter-intuitive increase in Alpl was observed. These novel data demonstrate that androgens play a role in inducing vascular calcification through the AR. Androgen signalling may represent a novel potential therapeutic target for clinical intervention.
Similar content being viewed by others
Introduction
Being male is associated with an increased risk of cardiovascular disease1, suggesting that androgens may negatively impact the cardiovascular system. However, recent studies have suggested that testosterone may in fact exert protective effects on the cardiovascular system, as low plasma testosterone levels are associated with advanced atherosclerosis and independently related to cardiovascular disease and mortality2,3,4,5,6. Understanding this apparent discrepancy is of paramount importance, given the dramatic increase in the use of Androgen Replacement Therapy (ART) in men over the last decade7,8. Furthermore, the continued abuse of anabolic androgens in sport9 induces long term adverse medical effects including cardiovascular toxicity along with manic behavioural symptoms10.
Testosterone is the primary androgen in men. The biological actions of testosterone and particularly of nonaromatizable dihydrotestosterone (DHT), are predominantly mediated by the androgen receptor (AR)11. The AR modulates transcription by binding to androgen-response elements (AREs) in the promoter and enhancer regions of target genes in the nucleus12. The AR is expressed throughout the arterial wall13,14 and has been reported to play a notable role in vascular disease15,16. Additionally, testosterone can be converted to estradiol by aromatase expressed in the vessel wall17. The induction of rapid, non-genomic actions through interactions with additional signalling pathways may further refine the cellular effects of testosterone12,18.
Vascular calcification is a life-threatening complication of cardiovascular disease, affecting tissues including arteries, heart valves and cardiac muscle19,20,21,22. Whilst the mechanisms underpinning the pathogenesis of calcified aortic valve disease (CAVD) are still unclear, it has been shown to share many features with the predominantly studied arterial calcification22. Both CAVD and arterial calcification are recognised as active, tightly regulated processes, sharing many similarities with physiological bone formation23 and involves the deposition of hydroxyapatite crystals in arteries. Indeed VSMCs, the predominant cell type involved in vascular calcification, can undergo transdifferentiation to a chondrocytic, osteoblastic and osteocytic phenotype in a calcified environment24,25. Furthermore, it has been demonstrated that phosphate (Pi) accelerates this phenotypic trans-differentiation, evident in the loss of characteristic smooth muscle markers and the development of osteoblastic features, such as the expression of tissue-nonspecific alkaline phosphatase (TNAP), sodium-dependent phosphate co-transporter (PiT-1), osteocalcin and osteopontin and osteocyte markers including sclerostin and podoplanin (Pdpn/E11)25,26. Vascular calcification also involves the reciprocal loss of recognised calcification suppressors, such as inorganic pyrophosphate (PPi), matrix Gla protein (MGP) and fetuin A27,28.
The prevalence of vascular calcification is sexually dimorphic, showing a relative increase in men compared to women, which suggests possible hormonal influence29. Androgens have been reported to play a major regulatory role in bone formation, having significant effects on both osteoblast and osteoclast function30. The pro-calcificatory effects of androgens on established atherosclerotic lesions have recently been demonstrated in the Apolipoprotein E-null mouse model31. However, subsequent in vitro studies have suggested an inhibitory effect of testosterone on vascular calcification32. Given these inconsistent findings, there is a clear need for additional studies to firmly establish the role of androgens in vascular calcification. We have therefore undertaken analysis of clinical tissues in conjunction with in vitro calcification studies in C57BL/6 and SM-ARKO mice to address the hypothesis that testosterone induces vascular calcification through stimulation of AR.
Results
Expression of AR in human calcified cardiovascular tissue
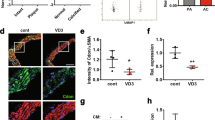
To investigate the role of the AR in vascular calcification, a critical and advanced phenotype of atherosclerosis, localisation studies were undertaken. Calcification of human femoral artery and aortic valve tissues was confirmed by alizarin red and von kossa staining (Fig. 1a I-IV,c I-IV). Immunohistochemistry established AR expression in calcified areas of human femoral artery and arterial valve tissues (Fig. 1b I-II,d I-II). Additionally, higher expression of AR was observed in calcified human aortic valve compared to control valve tissue (Fig. 1d I-II). These data are the first to show that AR is expressed alongside calcification in human calcified cardiovascular tissue.
Androgen receptor (AR) expression in calcified human cardiovascular tissue and primary murine VSMCs.
(a) Calcified human femoral artery was confirmed by alizarin red (I & III, arrows indicate positive alizarin red staining) and von kossa staining (II & IV, arrows indicate positive von kossa staining). (b) AR expression was observed in the calcified tunica media region of human femoral artery tissue (I & II, arrows indicate positive AR staining). (c) Calcified aortic valve was confirmed by alizarin red (I & II, arrows indicate positive alizarin red staining) and von kossa staining (III & IV, arrows indicate positive von kossa staining). (d) Higher AR expression was observed in calcified aortic valve compared to control (I & II, arrows indicate positive AR staining). (e) Immunofluorescence staining showed nucleus staining of AR in murine VSMCs (SMA-red, AR-green, DAPI-blue, arrows indicate colocalisation of AR and DAPI staining). (f) Representative image of western blotting for AR following 100 nM testosterone treatment in VSMCs (Images were cropped from original scans and gels were performed under the same experimental conditions. Unprocessed original scans are shown in Suppl Fig. 1) and (g) densitometry quantification (n = 3) showed increased expression of AR in VSMCs following treatment with testosterone. (h) Aromatase expression was absent from murine VSMCs (Images were cropped from original scans and gels were performed under the same experimental conditions. Unprocessed original scans are shown in Suppl Fig. 1). NC=Negative Control. Scale bar = 100 μm. *P < 0.05.
Isolated VSMCs were positively stained with alpha smooth muscle actin (SMA) antibody (Fig. 1e, red). AR expression was confirmed in cultured murine VSMCs (the predominant cell type responsible for blood vessel calcification) by immunofluorescence staining (Fig. 1e, green) and was shown to increase following incubation with testosterone (100 nM) (Fig. 1e, green) for 48 hrs. Additionally, AR is expressed in the nucleus of VSMCs, as evidenced by DAPI counterstaining (Fig. 1e, blue, white arrow). Increased expression of AR following treatment with testosterone was also confirmed by western blotting (Fig. 1f,g). RT-PCR analysis revealed aromatase was expressed by mouse ovary and testis, but not in VSMCs (Fig. 1h).
Androgens induce high Pi-dependent VSMC calcification
To investigate the role of the AR in VSMCs, we examined the effects of androgens on VSMC calcification. Initial studies examined whether androgens directly regulate the osteogenic differentiation and calcification of VSMCs. Since arterial calcification is highly correlated with elevated serum Pi levels, VSMCs were cultured in growth medium containing high Pi (3 mM) as previously described33,34. Cells were treated with 1–100 nM testosterone or DHT in the presence or absence of high Pi medium for up to 9 days. A minimum concentration of 10 nM testosterone treatment significantly increased calcium deposition of VSMCs at 9 days, as evaluated by HCl leaching (1.8 fold, P < 0.01, Fig. 2a). A minimum concentration of 100 nM DHT treatment significantly increased calcium deposition in VSMCs at 9 days (1.6 fold, P < 0.05, Fig. 2b). Testosterone and DHT (100 nM) induced a significant increase in the mRNA expression of Alpl a key mediator of mineralisation (1.14 fold, P < 0.01) (Fig. 2c). No change in the mRNA expression of the osteogenic marker Osterix or the mineralisation inhibitor Mgp was observed (Fig. 2d,e).
Androgens promote VSMC calcification and regulate osteogenic gene expression.
VSMCs were cultured with high phosphate (3 mM Pi; filled bar) or control (1 mM Pi; white bar) for up to 9 days. Calcium content (μg/mg protein) of cells treated with (a) testosterone (1–100 nM) (n = 4) or (b) DHT (1-100 nM) (n = 4). Fold change in the mRNA expression of (c) Alpl (d) Osterix and (e) Mgp following 48 hr treatment with testosterone (white bar) or DHT (filled bar) (n = 6). Results are presented as mean +/− S.E.M *P < 0.05; **P < 0.01; ***P < 0.001 compared with control.
Androgens induce calcification through the AR
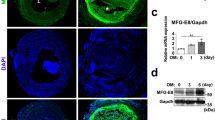
To examine whether testosterone-stimulated VSMC calcification is mediated through the AR, further studies were undertaken using cells derived from VSMC-specific AR-ablated (SM-ARKO) mice. Protein expression studies confirmed AR ablation in the VSMCs (Fig. 3a). Furthermore, testosterone exposure notably up-regulated AR protein expression in WT VSMCs, whereas AR expression remained absent in comparably-treated SM-ARKO cells (Fig. 3a). Additional studies revealed a marked reduction in Esr2 mRNA expression in SM-ARKO mice versus WT controls (0.4 fold; P < 0.05; Fig. 3b), whereas Esr1 expression remained unaltered (Fig. 3c). Consistent with our earlier observations (Fig. 2a), 100 nM testosterone significantly increased VSMC calcification in WT cells. However, testosterone-induced calcification was blunted in SM-ARKO cells (0.52 fold; P < 0.05; Fig. 3d). Consistent with these data, SM-ARKO VSMCs showed a significant reduction in Osterix mRNA expression (0.85 fold; P < 0.001; Fig. 4a). However, intriguingly, a counter-intuitive increase in Alpl was observed (3.3 fold; Fig. 4b, P < 0.001), with a concomitant decrease in the mineralisation inhibitor Mgp (0.5 fold; Fig. 4c, P < 0.001).
Androgens promote Pi-induced calcification via the AR.
(a) AR protein expression in SM-ARKO VSMCs versus WT control cells in the presence or absence of testosterone (100 nM) (Images were cropped from original scans and gels were performed under the same experimental conditions. Unprocessed original scans are shown in Suppl Fig. 1). Fold change in the mRNA expression of (b) Esr2 and (c) Esr1 in SM-ARKO VSMCs versus WT control cells (n = 5). (d) Calcium content (μg/mg protein) of SM-ARKO and WT VSMCs cultured with high phosphate (3 mM Pi) for 9 days and treated with testosterone (100 nM) (n = 6). Results are presented as mean + /− S.E.M *P < 0.05 compared with control.
Testosterone has no effect on apoptosis of VSMCs
Apoptosis plays an important role in vascular calcification, we therefore examined the effect of testosterone treatment on VSMC apoptosis. Alamar blue assay showed no effect of either testosterone or DHT on cell viability (Fig. 5a). DAPI staining revealed no effect of either testosterone or DHT on nuclei apoptosis (Fig. 5b).
Discussion
Whilst testosterone deficiency has been linked with cardiovascular disease in men1, the effects of ART on vascular health are currently highly controversial7,8. Given the increasing pharmacological use of androgens in society, a more complete understanding of the cardiovascular safety of exogenous androgens is essential. This investigation addressed the hypothesis that androgen-induced stimulation of the AR induces arterial calcification. Our work offers new insight into the role of androgens in disease and provides direct evidence to suggest that testosterone contributes to the pathological process of vascular calcification.
Our in vitro investigations revealed that exogenous testosterone and DHT treatment both had striking effects on the induction of VSMC calcification. A concomitant increase in expression of Alpl, a recognised regulator of osteoblastic differentiation and matrix mineralisation of VSMCs was observed. Indeed, there is a substantial body of evidence linking TNAP elevation with vascular calcification. TNAP upregulation has been observed in calcified coronary atherosclerotic plaques35, as well as in medial vascular calcification associated with diabetes36, in patients undergoing dialysis37,38 and has been proposed as a cause of the vessel calcification seen in uremia39. Consistent with these findings, an association between long-term anabolic steroid abuse in men and early vascular calcification has been previously reported40. Similarly, in women with polycystic ovary syndrome, elevated endogenous androgen levels are associated with increased vascular calcification41 and high dose testosterone administration in post-menopausal women has been associated with increased atherosclerosis as measured by detection of calcified deposits42. In addition, recent animal studies have employed the Apolipoprotein E mouse model to directly link testosterone and calcification in the vasculature31. However, in contrast to these data, a recent in vitro study has reported inhibitory effects of androgens on VSMC calcification32. This discrepancy may reflect key differences in the species, passage status and culture conditions of the cells investigated.
Androgens act mainly through transcriptional control of target genes mediated by AR11. In the present study we confirmed that AR is expressed in VSMCs and identified for the first time the presence of AR expression in calcified human femoral artery and aortic valve tissue. These data are consistent with previous studies showing expression of AR in smooth muscle cells and endothelial cells in arteries14,43. Further studies are required to comprehensively establish AR expression levels throughout the different layers of arterial blood vessels. The ability of DHT to replicate the effects of testosterone, together with our data revealing a lack of aromatase expression, suggests that the pro-calcificatory androgenic effects are mediated directly through AR. Consistent with this hypothesis, our in vitro studies demonstrated that AR is up-regulated in VSMCs by androgen treatment. This is in agreement with reports of increased local AR expression in the innominate artery in response to testosterone and DHT-induced calcification in the ApoE mouse model31. However, in a recent clinical analysis, no association between coronary artery calcification in men and AR expression was observed13. Potentially the exclusion of patients with existing coronary artery disease may have resulted in an underestimation of any association between AR expression and calcification in this study.
The utilisation of a novel vascular selective ARKO mouse model was central to this investigation. The employment of a cell-specific mouse line with AR deleted from VSMCs44 emphatically highlights, for the first time, a functional role for AR in androgen-induced vascular calcification. Reduced Osterix expression was observed in SM-ARKO VSMCs, suggesting androgen receptor may regulate osteogenic differentiation of VSMCs. Unexpectedly, altered expression of the calcification regulator Mgp and Alpl was also noted in SM-ARKO cells. Further studies are required to investigate their roles in AR-mediated calcification.
This study reveals AR expression in diseased vascular tissue and highlights a potential link between pharmacological androgen use and vascular calcification. We note that this is achieved in a small sample and these data need to be extended with further samples in future investigations. However, the clear demonstration that androgens directly act through the AR to mediate pro-calcificatory effects in VSMCs may have important health ramifications for patients with elevated AR expression in their vascular tissues and for the use of ART. These data also have strong implications for the role of androgens in aortic valve calcification, which independently predicts mortality in aortic stenosis45,46.
Materials and Methods
Human tissues
Arterial samples were obtained with appropriate ethical approval from a patient undergoing amputation for critical limb ischaemia (Ethics Number: 13/ES/0126). Research ethics committee approval (National Health Service West of Scotland Research Ethics Committee: 12/WS/0227) and the written and informed consent of all participants were obtained. The sample was from an amputated leg from a man who had unsalvagable critical limb ischaemia secondary to in situ thrombosis of typical atherosclerotic femoro-popliteal peripheral arterial disease. He was an ex-smoker with no history of any endocrine disorder (including diabetes) and had an entirely normal masculine phenotype. He was on no hormonal treatment but was receiving standard therapy for atherosclerosis, namely aspirin and a HMG-CoA reductase inhibitor (statin). He had normal renal function and so the aetiology of the calcification in his femoral artery was associated with atherosclerosis. Serum testosterone levels were not measured. Human valve tissues were obtained with appropriate ethical approval from patients undergoing valve replacement surgery (Ethics No: 13/ES/0126). The control valve was from a 79 year old woman with aortic incompetence and generalised aortic dilatation with ascending aorta involvement. There was minor to moderate left ventricular impairment. The calcified valve was from a 67 year old woman with severe aortic stenosis detected by echocardiography. The aortic valve was removed at the time of aortic valve replacement operation and carefully preserved the integrity of the valve architecture. An informed consent was given for the use of the human tissue and this study was performed in conformation with the declaration of Helsinki.
Materials
The AR antibody (Catalog: SC-816-G) was from Santa Cruz Biotechnology (Paso Robles, US). Testosterone and DHT were obtained from Sigma (Poole, UK). The SMA antibody (Catalog: A2547) was from sigma. DAPI, Alexa Fluor@488 donkey-anti goat antibody (Catalog: A-11055) and Alexa Fluor@594 goat-anti mouse antibody (Catalog: A-11005) were from Invitrogen (Paisley, UK).
Mice
Mice with selective ablation of AR from VSMCs (SM-ARKO) were generated and genotyped as previously described14. All animal experiments were performed under UK Home Office licensed approval in accordance with Directive 2010/63/EU of the European Parliament and were maintained in accordance with Home Office guidelines for the care and use of laboratory animals. C57BL/6 mice were supplied by Charles River Laboratories (Harlow, Essex, UK).
Isolation of primary murine VSMCs
Mice were euthanized by cervical dislocation. Primary murine VSMCs were isolated as previously described25,33,34. After removal of adventitia, the aorta was cut open to expose the endothelial layer under a dissection microscope. Tissues from eight animals were pooled and incubated with 1 mg ml−1 trypsin (Invitrogen) for 10 min in order to remove any remaining adventitia and endothelium. After a further overnight incubation at 37 °C in a humidified atmosphere of 95% air/5% CO2 in α-MEM medium (Invitrogen) supplemented with 10% Fetal Bovine Serum (Invitrogen) and 1% gentamicin (Invitrogen), tissues were digested with 425 U/ml collagenase type II (Worthington Biochemical Corporation, Lakewood, USA) for 5 hrs. Medial cells were released and cell suspensions were centrifuged at 2000 g for 5 min. The cell pellet was washed and resuspended in the above mentioned culture medium. Isolated VSMCs were cultured with growth medium for two passages in T25 tissue culture flasks (Greiner Bio-one, GmbH, Frickenhausen, Baden-Wurttemberg, Germany) coated with 0.25 μg/cm2 laminin (Sigma) to promote maintenance of the contractile differentiation state47.
Induction of calcification
Primary VSMCs were seeded in growth medium at a density of 1.5 × 104/cm2 in multi-well plates. Calcification was induced as previously described25,33,34. In brief, cells were grown to confluence (day 0) and switched to calcification medium, which was prepared by adding 1 M inorganic phosphate (Pi) (a mixture of NaH2PO4 and Na2HPO4, pH 7.4) (Sigma), to reach a final concentration of 3 mM Pi. VSMCs were incubated for up to 9 days in 95% air/ 5% CO2 and the medium was changed every third/fourth day. Testosterone (1–100 nM) or DHT (1–100 nM) were added at day 0, according to previous publications14,32.
Determination of calcification
Calcium deposition was quantified as previously described34,48,49. Briefly, cells were rinsed twice with phosphate buffered saline (PBS) and decalcified with 0.6 N HCl at room temperature for 24 hrs. Free calcium was determined colorimetrically by a stable interaction with phenolsulphonethalein using a commercially available kit (Randox Laboratories Ltd., County Antrim, UK) and corrected for total protein concentration (Bio-Rad Laboratories Ltd, Hemel Hempstead, UK).
Analysis of gene expression
RNA was extracted using RNeasy total RNA (Qiagen, West Sussex, UK), according to the manufacturer’s instructions. RNA was reverse transcribed and specific cDNAs were semi-quantified by end point PCR or quantified by real-time PCR using the SYBR green detection method as previously reported33,34,48 Primers were obtained from Eurofins MWG Biotech (Ebersberg, Germany), Qiagen, Ambion (Cambridge UK) and Primer Design (Southampton, UK), with available sequences provided in the online Data Supplement (Suppl. Table S1).
Alamar blue staining
VSMCs were grown on 96-well plates at a density of 5,000 cells/ well. Alamar blue assay was performed as previously described49. Alamar blue reagent (Invitrogen) (10 μl/100 μl medium) was added to culture medium for the final 4 hrs of culture at 37 °C, 5% CO2. Optical density absorbance was analysed at wavelengths of 570 nm and 620 nm using a spectrophotometer (Multiskan Ascent; Thermo Electron Corporation,Vantaa, Finland).
Apoptosis
Apoptotic VSMCs were determined by manually counting pyknotic nuclei after staining with DAPI (Invitrogen) as previously described50.
Fluorescent immunocytochemical staining
VSMCs were seeded on glass coverslips in 12-well plates at a density of 50, 000 cells/well. Following confluence, VSMCs were serum-restricted for 24 hrs and treated with contro or 100 nM testosterone for 48 hrs. Cells were fixed with 4% paraformaldehyde and washed with PBS. The fixed cells were permeabilised with 0.3% Triton-X 100 (Sigma) and incubated with anti-AR antibody (Santa Cruz Biotechnology) and anti-SMA (Sigma) overnight at 4o C. After washing, cells were incubated with Alexa Fluor@488 donkey-anti goat antibody and Alexa Fluor@594 goat-anti mouse antibody (Invitrogen) for 1 hr in the dark. Glass coverslips were mounted onto slides with Prolong®Gold Anti-Fade Reagent contained DAPI (Invitrogen). Fluorescence signal was detected under a Leica fluorescence microscope (Milton Keynes, UK).
Western analysis
VSMCs were treated with 100 nM testosterone for 48 hrs. Cells were lysed in PhosphoSafe extraction buffer (Merck Biosciences Ltd, Nottingham, UK) containing “Complete” protease inhibitor cocktail (Roche, East Sussex, UK) according to manufacturer’s instructions. Western blotting was performed as previously described23,32,33. Nitrocellulose membranes were probed overnight at 4 °C with anti-AR antibody (Santa Cruz Biotechnology), washed in TBST and incubated with anti-goat IgG-peroxidase respectively (DAKO, Glostrup, Denmark) for 1 hr (1:1000 dilution in 5% milk). The immune complexes were visualised using enhanced chemiluminescence (ECL) (GE Healthcare, Buckinghamshire, UK). Membranes were then washed in ‘stripping buffer’ (Pierce, Rockford, Il, USA) and re-probed for 1 hr for β-actin expression (1:5000 dilution in 5% milk; anti β-actin clone AC15; Sigma-Aldrich).
Histology and immunohistochemistry
Tissues were fixed in 10% neutral buffered formalin (NBF) for 24 hrs before being dehydrated and embedded in paraffin wax and sectioning at 4 μm using standard procedures. Sections were de-waxed in xylene and stained with Von Kossa and alizarin red (Sigma) to visualise phosphate and calcium deposition, respectively. Immunohistochemistry was performed using the VECTASTAIN ABC Kit (Goat IgG) (Vector Labs, Peterborough, UK) according to manufacturer’s instructions. Sections were de-waxed in xylene and de-masked with citric acid based antigen unmasking solution (Vector Labs). Endogenous peroxidase and non-specific antibody binding were blocked before overnight incubation at 4 oC with 2 μg IgG/ml anti-AR antibody (Santa Cruz Biotechnology). The sections were then washed in PBS, incubated with diluted biotinylated secondary antibody (1:200 dilution) for 30 min. After washing in PBS for 5 min, the sections were incubated for 30 min with VECTASTAIN® ABC Reagent (Vector Labs). The sections were then incubated with DAB substrate reagent (0.06% DAB, 0.1% H2O2 in PBS) until the desired stain intensity developed. The sections were finally dehydrated, counterstained with haematoxylin and eosin and mounted in DePeX. Control sections were incubated with non-immune goat IgG (2 μg IgG/ml) in place of the primary AR antibody.
Statistical analysis
General Linear Model analysis and the Students t-test were used to assess the data. All data are expressed as the mean + /− S.E.M. Statistical analysis was performed using Minitab 16. P < 0.05 was considered to be significant.
Additional Information
How to cite this article: Zhu, D. et al. Ablation of the androgen receptor from vascular smooth muscle cells demonstrates a role for testosterone in vascular calcification. Sci. Rep. 6, 24807; doi: 10.1038/srep24807 (2016).
References
Sullivan, M. L., Martinez, C. M., Gennis, P. & Gallagher, E. J. The cardiac toxicity of anabolic steroids. Prog Cardiovasc Dis. 41, 1–15 (1998).
Jeppesen, L. L. et al. Decreased serum testosterone in men with acute ischemic stroke. Arterioscler Thromb Vasc Biol. 16, 749–754 (1996).
Simon, D. et al. Association between plasma total testosterone and cardiovascular risk factors in healthy adult men: The Telecom Study. J Clin Endocrinol Metab. 82, 682–685 (1997).
Stellato, R. K., Feldman, H. A., Hamdy, O., Horton, E. S. & McKinlay, J. B. Testosterone, sex hormone-binding globulin and the development of type 2 diabetes in middle-aged men: prospective results from the Massachusetts male aging study. Diabetes Care. 23, 490–494 (2000).
Fogari, R. et al. Serum testosterone levels and arterial blood pressure in the elderly. Hypertens Res. 28, 625–630 (2005).
Shores, M. M., Matsumoto, A. M., Sloan, K. L. & Kivlahan, D. R. Low serum testosterone and mortality in male veterans. Arch Intern Med. 166, 1660–1665 (2006).
Gan, E. H., Pattman, S., H. S. Pearce, S. & Quinton, R. A UK epidemic of testosterone prescribing, 2001–2010. Clin Endocrinol (Oxf). 79, 564–570 (2013).
Baillargeon, J. et al. Risk of Myocardial Infarction in Older Men Receiving Testosterone Therapy. Ann Pharmacother. 48, 1138–1144 (2014).
Handelsman, D. J. Testosterone: use, misuse and abuse. Med J Aust. 185, 436–439 (2006).
Kanayama, G., Hudson, J. I. & Pope, H. G. Jr. Illicit anabolic-androgenic steroid use. Horm Behav. 58, 111–121(2010).
Mangelsdorf, D. J. et al. The nuclear receptor superfamily: the second decade. Cell. 83, 835–839 (1995).
Heinlein, C. A. & Chang, C. Androgen receptor (AR) coregulators: an overview. Endocr Rev. 23, 175–200 (2002).
Liu, P. Y., Christian, R. C., Ruan, M., Miller, V. M. & Fitzpatrick, L. A. Correlating androgen and estrogen steroid receptor expression with coronary calcification and atherosclerosis in men without known coronary artery disease. J Clin Endocrinol Metab. 90, 1041–1046 (2005).
Wu, J. et al. Modulation of neointimal lesion formation by endogenous androgens is independent of vascular androgen receptor. Cardiovasc Res. 103, 281–290 (2014).
Hanke, H., Lenz, C., Hess, B., Spindler, K. D. & Weidemann, W. Effect of testosterone on plaque development and androgen receptor expression in the arterial vessel wall. Circulation. 103, 1382–1385 (2001).
Zitzmann, M. et al. The CAG repeat polymorphism in the androgen receptor gene affects bone density and bone metabolism in healthy males. Clin Endocrinol (Oxf). 55, 649–657 (2001).
Nathan, L. et al. Testosterone inhibits early atherogenesis by conversion to estradiol: critical role of aromatase. Proc Natl Acad Sci USA 98, 3589–3593 (2001).
Baron, S. et al. Androgen receptor mediates non-genomic activation of phosphatidylinositol 3-OH kinase in androgen-sensitive epithelial cells. J Biol Chem. 279, 14579–14586 (2004).
Margolis, J. R. et al. The diagnostic and prognostic significance of coronary artery calcification. A report of 800 cases. Radiology. 137, 609–616 (1980).
Schmermund, A. et al. Assessment of coronary calcification by electron-beam computed tomography in symptomatic patients with normal, abnormal or equivocal exercise stress test. Eur Heart J. 21, 1674–1682 (2000).
Wayhs, R., Zelinger, A. & Raggi, P. High coronary artery calcium scores pose an extremely elevated risk for hard events. J Am Coll Cardiol. 39, 225–230 (2002).
Dweck, M. R., Boon N. A. & Newby D. E. Calcific aortic stenosis: a disease of the valve and the myocardium. J Am Coll Cardiol. 60, 1854–63 (2012).
Zhu, D., Mackenzie, N. C., Farquharson, C. & Macrae, V. E. Mechanisms and clinical consequences of vascular calcification. Front Endocrinol (Lausanne). 3, 95 (2012).
Shroff, R. C. et al. Dialysis accelerates medial vascular calcification in part by triggering smooth muscle cell apoptosis. Circulation. 118, 1748–57 (2008).
Zhu, D., Mackenzie, N. C., Millan, J. L., Farquharson, C. & MacRae, V. E. The appearance and modulation of osteocyte marker expression during calcification of vascular smooth muscle cells. PLoS One. 6, e19595 (2011).
Speer, M. Y. et al. Smooth muscle cells give rise to osteochondrogenic precursors and chondrocytes in calcifying arteries. Circ Res. 104, 733–741 (2009).
Rutsch, F. et al. Mutations in ENPP1 are associated with ‘idiopathic’ infantile arterial calcification. Nat Genet. 34, 379–381 (2003).
Murshed, M., Harmey, D., Millan, J. L., McKee, M. D. & Karsenty, G. Unique coexpression in osteoblasts of broadly expressed genes accounts for the spatial restriction of ECM mineralization to bone. Genes Dev. 19, 1093–1104 (2005).
Allison, M. A. & Wright, C. M. Age and gender are the strongest clinical correlates of prevalent coronary calcification (R1). Int J Cardiol. 98, 325–330 (2005).
Vanderschueren, D. et al. Androgens and bone. Endocr Rev. 25, 389–425 (2004).
McRobb, L., Handelsman, D. J. & Heather, A. K. Androgen-induced progression of arterial calcification in apolipoprotein E-null mice is uncoupled from plaque growth and lipid levels. Endocrinology. 150, 841–848 (2009).
Son, B. K. et al. Androgen receptor-dependent transactivation of growth arrest-specific gene 6 mediates inhibitory effects of testosterone on vascular calcification. J Biol Chem. 285, 7537–7544 (2010).
Zhu, D., Mackenzie, N. C., Millan, J. L., Farquharson, C. & Macrae, V. E. Upregulation of IGF2 expression during vascular calcification. J Mol Endocrinol. 52, 77–85 (2014).
Zhu, D. et al. BMP-9 regulates the osteoblastic differentiation and calcification of vascular smooth muscle cells through an ALK1 mediated pathway. J Cell Mol Med. 19, 165–174 (2014).
Joshi, N. V. et al. 18 F-fluoride positron emission tomography for identification of ruptured and high-risk coronary atherosclerotic plaques: a prospective clinical trial. Lancet. 383, 705–713 (2014).
Shanahan, C. M. et al. Medial localization of mineralization-regulating proteins in association with Monckeberg’s sclerosis: evidence for smooth muscle cell-mediated vascular calcification. Circulation. 100, 2168–2176 (1999).
Moe, S. M., Duan, D., Doehle, B. P., O’Neill, K. D. & Chen, N. X. Uremia induces the osteoblast differentiation factor Cbfa1 in human blood vessels. Kidney Int. 63, 1003–1011 (2003).
Shroff, R. C. et al. Dialysis accelerates medial vascular calcification in part by triggering smooth muscle cell apoptosis. Circulation. 118, 1748–1757 (2008).
Lomashvili, K. A., Garg, P., Narisawa, S., Millan, J. L. & O’Neill, W. C. Upregulation of alkaline phosphatase and pyrophosphate hydrolysis: potential mechanism for uremic vascular calcification. Kidney Int. 73, 1024–1030 (2008).
Santora, L. J. et al. Coronary calcification in body builders using anabolic steroids. Prev Cardiol. 9, 198–201 (2006).
Christian, R. C. et al. Prevalence and predictors of coronary artery calcification in women with polycystic ovary syndrome. J Clin Endocrinol Metab. 88, 2562–2568 (2003).
Hak, A. E., Westendorp, I. C., Pols, H. A., Hofman, A. & Witteman, J. C. High-dose testosterone is associated with atherosclerosis in postmenopausal women.Maturitas. 56, 153–160 (2007).
Kimura N. et al. Immunocytochemical localization of androgen receptor with polyclonal antibody in paraffin-embedded human tissues. J Histochem Cytochem. 41, 671–8 (1993).
Welsh, M. et al. Deletion of androgen receptor in the smooth muscle of the seminal vesicles impairs secretory function and alters its responsiveness to exogenous testosterone and estradiol. Endocrinology. 151, 3374–3385 (2010).
Clavel, M. A. et al. The complex nature of discordant severe calcified aortic valve disease grading: new insights from combined Doppler echocardiographic and computed tomographic study. J Am Coll Cardiol. 62, 2329–2338 (2013).
Clavel, M. A. et al. Impact of aortic valve calcification, as measured by MDCT, on survival in patients with aortic stenosis: results of an international registry study. J Am Coll Cardiol. 64, 1202–1213 (2014).
Johnson, K. A., Polewski, M. & Terkeltaub, R. A. Transglutaminase 2 is central to induction of the arterial calcification program by smooth muscle cells. Circ Res. 102, 529–537 (2008).
Mackenzie, N. C. et al. MOVAS-1 cell line: a new in vitro model of vascular calcification. Int J Mol Med. 27, 663–668 (2011).
Zhu, D., Mackenzie, N. C., Millan, J. L., Farquharson, C. & MacRae, V. E. A protective role for FGF-23 in local defence against disrupted arterial wall integrity? Molecular and Cellular Endocrinology. 372, 1–11 (2013).
Guicciardi, M. E. et al. Cellular inhibitor of apoptosis 1 (cIAP-1) degradation by caspase 8 during TNF-related apoptosis-inducing ligand (TRAIL)-induced apoptosis. Exp Cell Res. 317, 107–116 (2011).
Acknowledgements
This work was supported by an Institute Strategic Programme Grant (BB/J004316/1) and Institute Career Path Fellowship funding (BB/F023928/1) from the Biotechnology and Biological Sciences Research Council (BBSRC) and by a Bristish Heart Foundation Project Grant (PG/11/72/29334). The authors are grateful for support from the BHF Centre for Research Excellence.
Author information
Authors and Affiliations
Contributions
V.E.M. supervised the project, D.Z. and V.E.M. conceived and designed experiments and wrote the manuscript; D.Z. and J.W. performed experiments and analysed the data; P.W.F.H., J.W., A.T.V., D.A.L., M.R.D., D.E.N. and L.B.S. helped to prepare the manuscript. All authors read, discussed and edited the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zhu, D., Hadoke, P., Wu, J. et al. Ablation of the androgen receptor from vascular smooth muscle cells demonstrates a role for testosterone in vascular calcification. Sci Rep 6, 24807 (2016). https://doi.org/10.1038/srep24807
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep24807
This article is cited by
-
Stroke and thromboembolic events in men with prostate cancer treated with definitive radiation therapy with or without androgen deprivation therapy
Prostate Cancer and Prostatic Diseases (2019)
-
Protective effects of finasteride against testosterone-induced calcium oxalate crystallization and crystal-cell adhesion
JBIC Journal of Biological Inorganic Chemistry (2019)
-
Involvement Of Vascular Aldosterone Synthase In Phosphate-Induced Osteogenic Transformation Of Vascular Smooth Muscle Cells
Scientific Reports (2017)
-
Reduction of calprotectin and phosphate during testosterone therapy in aging men: a randomized controlled trial
Journal of Endocrinological Investigation (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.