Abstract
Two recruitment strategies for research were compared to prospectively identify patients with breathlessness who are awaiting a diagnosis in primary care. The first method utilised searches of the electronic patient record (EPR), the second method involved an electronic template triggered during a consultation. Using an electronic template triggered at the point of consultation increased recruitment to prospective research approximately nine-fold compared with searching for symptom codes and study mailouts.
Similar content being viewed by others
Patients living with breathlessness often seek help for the first time in primary care; around 4% of general practitioner (GP) consultations are due to breathlessness, and much of their management is undertaken in primary care1. This population commonly have underlying cardiorespiratory disease2, but there are significant delays in diagnosis and variation in clinical practice3,4,5. Successful recruitment to research trials in primary care is key to improving outcomes for adults presenting with breathlessness, but there are significant challenges, particularly with intervention trials6. A review of effective research recruitment in primary care indicates that the key elements include practitioner involvement, simple eligibility criteria, participant incentives and minimal impact on practitioner workload7.
We aimed to compare two prospective recruitment strategies for adults presenting with breathlessness for the first time in primary care using similar GP practices.
Methods
Recruitment strategies and participants
Two different strategies were applied to prospectively identify and recruit patients presenting with breathlessness to GP practices in Leicestershire, UK. The first method (Strategy 1) for a primary care breathlessness cohort study used weekly searches for new breathlessness Read codes in the electronic patient record (EPR), followed by a mail out of study information to identified patients at 14 GP practices. The second method (Strategy 2) implemented an opportunist approach using an electronic template on the EPR, triggered at the point of consultation by either breathlessness-free text or Read codes at 10 GP practices8. The template (Fig. 1) summarised the study and eligibility criteria, prompting GPs to ask patients’ permission to be contacted by the study team. The wording for the electronic template to aid recruitment was developed by members of the patient and public involvement (PPI) group. The electronic template was designed to maximise identification of patients with specific eligibility; first or second presentation with breathlessness, over the age of 40 years old and without a pre-existing diagnosis (e.g. Chronic Obstructive Pulmonary Disease [COPD] and heart failure). The pop-up, therefore, did not trigger in certain patient records to avoid the unnecessary burden and filtering out by the clinician. The protocol for the electronic template is included in the supplementary information. Weekly reports of the patients identified were sent securely via nhs.net to the study team.
The electronic template was developed in partnership with Keele Clinical Trials Unit who supported the implementation of the electronic patient record system (SystmOne and Egton Medical Information Systems [EMIS]) for each practice. In addition to enhancing opportunistic recruitment, the template was embedded in the clinical care template for GP practices in the intervention with links to the next steps needed for the trial and links to best practice guidelines for the usual care GP practices.
Research studies design
The studies using the different recruitment strategies were distinct in their purpose; one a cohort study and the second a feasibility cluster randomised controlled trial (cRCT). However, the participant eligibility and involvement were similar, requiring research visits of the same frequency, to the same location, and completion of the same outcome measures. The same Read codes were used for both strategies and are available in the supplementary information. The GP practices in both studies were a similar size from the same three clinical commissioning groups within the same county. The recruitment rate was compared at six months from each of the trial start dates.
Semi-structured interviews with patients and GP practice staff were performed, including experiences with the electronic template method, breathlessness and healthcare interactions. Interviews were audio-recorded, transcribed, coded and reviewed by the study team using thematic analysis9. Written informed consent was obtained from all participants recruited in both Strategy one and two. The study described in Strategy 2 was registered with ISRCTN (ID:14483247, date registered: 06/11/2019).
Ethical approval
Research Ethics approval was provided by Wales Research Ethics Committee (REC) 7 (REC Reference 18/WA/0022) for Strategy 1 and Nottingham REC 1 (REC Reference: 19/EM/0201) for Strategy 2.
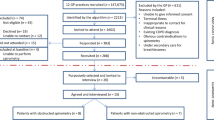
Over 6 months, more participants were identified and recruited using Strategy 2, 36/130 (28%) compared with Strategy 1, 4/146 (3%) participants (Fig. 2). The proportion of patients identified to the study team using Strategy 2 ranged from 6 to 14% of those where the template was triggered (our best estimate of the true denominator). In-depth review of the template activity in six of the GP practices showed the template was closed by clinicians without action for 33% (311/980) of patients and that there was no difference in frequency of triggering pre and post-March 2020 when the pandemic began.
Ten clinicians (nine GPs and one Respiratory Nurse) and seven administrative staff from each of the practices using the electronic template in Strategy 2 were interviewed to explore their views on the recruitment process, workload and study experience. Overall, GPs found the electronic template to be unobtrusive and helpful to have prompts, and patients were positive about receiving information about research from their GP (Table 1). One GP expressed finding the frequency of the template pop-up an annoyance during consultations.
Strategy 1 was limited by a lack of coding for breathlessness, and therefore searching for breathlessness-related Read codes did not yield enough eligible patients to contact, and once contacted were less likely to participate. GPs frequently code for diagnoses in primary care on the electronic patient record, previously using Read codes and more recently using SNOMED codes in the UK. GPs are less likely to code for symptoms such as breathlessness which are more commonly added as free text10, with the expectation that once a diagnosis is reached then the corresponding code will be added. The aim of coding is to provide a standardised vocabulary for clinicians to record patient findings11. However, clinical practice research datalink (CPRD) work has highlighted the challenges in using code lists in primary care to search for clinical features of interest, with inconsistent use of code labels5,10.
In contrast, the opportunistic use of an electronic ‘pop-up’ within a clinical consult in primary care has previously been used successfully to recruit to several trials for other symptom-based research and interventions, including musculoskeletal problems and back pain12,13 and appeared to increase recruitment of patients presenting with breathlessness in our data. During initial engagement and consultation with GPs and practice staff prior to the study set up some described ‘pop up fatigue’ for this kind of template, and the design was refined. However, our qualitative data demonstrate that the majority of practices found this to be an effective prompt with minimal disruption to the clinical consultation (Table 1). The careful consideration of the wording used at the point of template design, and consultation with our patient and public involvement (PPI) group, helped to ensure this was user-friendly and caused minimal disruption to the patient–clinician interaction.
The qualitative data from clinicians suggest that the impact of COVID-19 during the study period was perceived to increase the triggering of the electronic template, causing a problem for clinicians as more patients were presenting with breathlessness. This may have been perceived irritation during a time of high pressure, as review of the number of triggers at the GP practices demonstrated very little change in activity between March and August 2020. The way in which patients were accessing healthcare was significantly altered during this time, and the advantage of using the template was that it was always in use as a prompt whether consultations were face-to-face or by telephone.
There are limitations in our data as the two strategies were not compared within the same study design or period, and the GP practices taking part were not the same practices in the two studies. However, Strategy 2 was predominantly used during the COVID-19 pandemic in 2020, so our results may be underestimating recruitment in non-pandemic times. Coercion is an important ethical consideration when approaching patients for healthcare research via their usual health professional such as a GP14. To reduce this, the template used in Strategy 2 was only asking if patients could be contacted about a study for breathlessness, and not whether they were interested in taking part or consenting to take part in the research. Patients who gave permission were contacted by the study team with further information about the study and given time to make an informed decision. The key aspect of this work that made the electronic template an important asset was recruiting patients prospectively at the point of breathlessness presentation and in a primary care setting. There were no references in the interviews with patients to indicate they felt pressured to say yes when asked if they could be contacted regarding a research study.
An electronic template triggered at the point of consultation increased recruitment approximately nine-fold to prospective research compared with searching for symptom codes and study mailouts. Both healthcare professionals and patients were positive about the electronic template recruitment strategy. The electronic template is an effective method for researchers to consider maximising opportunistic patient recruitment and minimising the impact on clinician time in primary care.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
The datasets generated and analysed during the current study are available from the corresponding author on reasonable request via email that is related to this work on recruitment strategies. The data generated relevant to study specific outcomes for each respective study described in this paper are still in the analysis and writing up stage and will not be available prior to publication of the respective study results.
References
Frese, T., Sobeck, C., Herrmann, K. & Sandholzer, H. Dyspnea as the reason for encounter in general practice. J. Clin. Med. Res. 3, 239–246 (2011).
Sandberg, J. et al. Underlying contributing conditions to breathlessness among middle-aged individuals in the general population: a cross-sectional study. BMJ Open Respir. Res. https://doi.org/10.1136/bmjresp-2020-000643 (2020).
Jones, R. C. et al. Opportunities to diagnose chronic obstructive pulmonary disease in routine care in the UK: a retrospective study of a clinical cohort. Lancet Respir. Med. 2, 267–276 (2014).
Kim, D. et al. Route to heart failure diagnosis in English primary care: a retrospective cohort study of variation. Br. J. Gen. Pract. 69, e697–e705 (2019).
Chen, Y. et al. Prognostic value of first-recorded breathlessness for future chronic respiratory and heart disease: a cohort study using a UK national primary care database. Br. J. Gen. Pract. 70, e264–e273 (2020).
Foster, J. M., Sawyer, S. M., Smith, L., Reddel, H. K. & Usherwood, T. Barriers and facilitators to patient recruitment to a cluster randomized controlled trial in primary care: lessons for future trials. BMC Med. Res. Methodol. 15, 18 (2015).
Ngune, I., Jiwa, M., Dadich, A., Lotriet, J. & Sriram, D. Effective recruitment strategies in primary care research: a systematic review. Qual. Prim. care 20, 115–123 (2012).
Doe, G. et al. Feasibility study of a multicentre cluster randomised control trial to investigate the clinical and cost-effectiveness of a structured diagnostic pathway in primary care for chronic breathlessness: protocol paper. BMJ Open 11, e057362 (2021).
Clarke, V. & Braun, V. Thematic analysis. J. Posit. Psychol. 12, 297–298 (2017).
Hayward, R. A., Chen, Y., Croft, P. & Jordan, K. P. Presentation of respiratory symptoms prior to diagnosis in general practice: a case-control study examining free text and morbidity codes. BMJ Open 5, e007355 (2015).
NHSDigital. Read Codes, https://digital.nhs.uk/services/terminology-and-classifications/read-codes (2020).
Healey, E. L. et al. Integrating case-finding and initial management for osteoarthritis, anxiety, and depression into primary care long-term condition reviews: results from the ENHANCE pilot trial. Fam. Pract. https://doi.org/10.1093/fampra/cmab113 (2021).
Foster, N. et al. Effect of stratified care for low back pain in family practice (IMPaCT Back): a prospective population-based sequential comparison. Ann. Fam. Med. 12, 102–111 (2014).
Barton, C., Tam, C. W. M., Abbott, P. & Liaw, S.-T. Ethical considerations in recruiting primary care patients to research studies. Aust. Fam. Physician 45, 144–148 (2016).
Acknowledgements
We thank our patient participants for taking part in both studies described in this manuscript and the GP practices involved. We also acknowledge and thank our public and patient involvement (PPI) members and external trial steering committee members for their assistance in reviewing the study as a whole. This work was funded by a NIHR Clinician Scientist Fellowship (CS-2016-16-020) awarded to R.A.E. The work was supported by the NIHR Leicester Biomedical Research Centre—Respiratory. The views expressed are those of the authors and not necessarily those of the National Health Service, the NIHR, or the Department of Health.
Author information
Authors and Affiliations
Contributions
R.A.E. conceived the research idea for the wider projects relating to this recruitment strategy, and developed the theory and plan for this study alongside her co-authors. S.W. developed the electronic template with support from co-authors and input from the PPI members. G.D., J.C., S.E., and H.E. completed recruitment of the participants. G.D. drafted the initial manuscript. All authors reviewed, commented, and approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Doe, G., Wathall, S., Clanchy, J. et al. Comparing research recruitment strategies to prospectively identify patients presenting with breathlessness in primary care. npj Prim. Care Respir. Med. 32, 49 (2022). https://doi.org/10.1038/s41533-022-00308-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41533-022-00308-5