Abstract
Background
To evaluate vision 3 months after SmartSight lenticule extraction treatments.
Design
Case series.
Methods
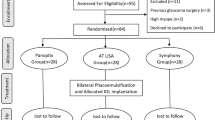
This case series of patients were treated at Specialty Eye Hospital Svjetlost in Zagreb, Croatia. Sixty eyes of 31 patients consecutively treated with SmartSight lenticule extraction were assessed. The mean age of the patients was 33 ± 6 years (range 23–45 years) at the time of treatment with a mean spherical equivalent refraction of −5.10 ± 1.35 D and mean astigmatism of 0.46 ± 0.36 D. Monocular corrected distance visual acuity (CDVA), uncorrected distance visual acuity (UDVA) were assessed pre- and post-operatively. Ocular and corneal wavefront aberrations have been postoperatively compared to the preoperative baseline values. Changes in ocular wavefront refraction, as well as changes in keratometric readings are reported.
Results
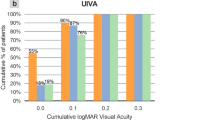
At 3 months post-operatively, mean UDVA was 20/20 ± 2. Spherical equivalent showed a low myopic residual refraction of −0.37 ± 0.58 D with refractive astigmatism of 0.46 ± 0.26 D postoperatively. There was a slight improvement of 0.1 Snellen lines at 3-months follow-up. Compared to the preoperative status, ocular aberrations (at 6 mm diameter) did not change at 3 months follow-up; whereas corneal aberrations increased (+0.22 ± 0.21 µm for coma; +0.17 ± 0.19 µm for spherical aberration; and +0.32 ± 0.26 µm for HOA-RMS). The same correction was determined using changes in ocular wavefront refraction, as well as changes in keratometric readings.
Conclusion
Lenticule extraction after SmartSight is safe and efficacious in the first 3 months postoperatively. The post-operative outcomes indicate improvements in vision.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
Data are available upon request.
References
Bohac M, Koncarevic M, Dukic A, Biscevic A, Cerovic V, Merlak M, et al. Unwanted astigmatism and high-order aberrations one year after excimer and femtosecond corneal surgery. Optom Vis Sci. 2018;95:1064–76. https://doi.org/10.1097/OPX.0000000000001298
Reinstein DZ, Archer TJ, Gobbe M. Small incision lenticule extraction (SMILE) history, fundamentals of a new refractive surgery technique and clinical outcomes. Eye Vis. 2014;1:3. https://doi.org/10.1186/s40662-014-0003-1
Izquierdo L Jr, Sossa D, Ben-Shaul O, Henriquez MA. Corneal lenticule extraction assisted by a low-energy femtosecond laser. J Cataract Refract Surg. 2020;46:1217–21. https://doi.org/10.1097/j.jcrs.0000000000000236
Pradhan KR, Arba-Mosquera S. Three-month outcomes of myopic astigmatism correction with small incision guided human cornea treatment. J Refract Surg. 2021;37:304–11. https://doi.org/10.3928/1081597X-20210210-02. Epub 2021 May 1
Tsai PS, Blinder P, Migliori BJ, Neev J, Jin Y, Squier JA, et al. Plasma-mediated ablation: an optical tool for submicrometer surgery on neuronal and vascular systems. Curr Opin Biotechnol. 2009;20:90–99. https://doi.org/10.1016/j.copbio.2009.02.003. Epub 2009 Mar 5
Noack J, Vogel A. Laser-induced plasma formation in water at nanosecond to femtosecond time scales: calculation of thresholds, absorption coefficients, and energy density. IEEE J Quantum Electron. 1999;35:1156–67.
Vogel A, Busch S, Jungnickel K, Birngruber R. Mechanisms of intraocular photodisruption with picosecond and nanosecond laser pulses. Lasers Surg Med. 1994;15:32–43. https://doi.org/10.1002/lsm.1900150106
Arba-Mosquera S, Verma S. Analytical optimization of the ablation efficiency at normal and non-normal incidence for generic super Gaussian beam profiles. Biomed Opt Express. 2013;4:1422–33. https://doi.org/10.1364/BOE.4.001422
Chernyak DA. From wavefront device to laser: an alignment method for complete registration of the ablation to the cornea. J Refract Surg. 2005;21:463–8. https://doi.org/10.3928/1081-597X-20050901-07
Gobbi PG, Carones F, Brancato R, Carena M, Fortini A, Scagliotti F, et al. Automatic eye tracker for excimer laser photorefractive keratectomy. J Refract Surg. 1995;11:S337–342. https://doi.org/10.3928/1081-597X-19950502-31
Dausch D, Klein R, Schröder E, Dausch B. Excimer laser photorefractive keratectomy with tapered transition zone for high myopia. A preliminary report of six cases. J Cataract Refract Surg. 1993;19:590–4. https://doi.org/10.1016/s0886-3350(13)80005-3
Bohac M, Biscevic A, Koncarevic M, Anticic M, Gabric N, Patel S. Comparison of wavelight allegretto eye-Q and Schwind Amaris 750 S excimer laser in treatment of high astigmatism. Graefes Arch Clin Exp Ophthalmol. 2014;252:1679–86. https://doi.org/10.1007/s00417-014-2776-2. Epub 2014 Aug 23
Siedlecki J, Luft N, Keidel L, Mayer WJ, Kreutzer T, Priglinger SG, et al. Variation of lenticule thickness for SMILE in low myopia. J Refract Surg. 2018;34:453–9. https://doi.org/10.3928/1081597X-20180516-01
Giri P, Azar DT. Risk profiles of ectasia after keratorefractive surgery. Curr Opin Ophthalmol. 2017;28:337–42. https://doi.org/10.1097/ICU.0000000000000383
Genc SL, Ma H, Venugopalan V. Low-density plasma formation in aqueous biological media using sub-nanosecond laser pulses. Appl Phys Lett. 2014;105:063701 https://doi.org/10.1063/1.4892665
Wang J, Schuele G, Palanker D. Finesse of transparent tissue cutting by ultrafast lasers at various wavelengths. J Biomed Opt. 2015;20:125004 https://doi.org/10.1117/1.JBO.20.12.125004
Vogel A, Capon MR, Asiyo-Vogel MN, Birngruber R. Intraocular photodisruption with picosecond and nanosecond laser pulses: tissue effects in cornea, lens, and retina. Investig Ophthalmol Vis Sci. 1994;35:3032–44.
de Ortueta D, Schreyger FD. Centration on the cornea vertex normal during hyperopic refractive photoablation using videokeratoscopy. J Refract Surg. 2007;23:198–200. https://doi.org/10.3928/1081-597X-20070201-13
Köse B.Detection of and compensation for static cyclotorsion with an image-guided system in SMILE. J Refract Surg.2020;36:142–9. https://doi.org/10.3928/1081597X-20200210-01.
Vinciguerra P, Roberts CJ, Albé E, Romano MR, Mahmoud A, Trazza S, et al. Corneal curvature gradient map: a new corneal topography map to predict the corneal healing process. J Refract Surg. 2014;30:202–7. https://doi.org/10.3928/1081597X-20140218-02
Gatinel D, Weyhausen A, Bischoff M. The percent volume altered in correction of myopia and myopic astigmatism with PRK, LASIK, and SMILE. J Refract Surg. 2020;36:844–50. https://doi.org/10.3928/1081597X-20200827-01
Kind R, Kiraly L, Taneri S, Troeber L, Wiltfang R, Bechmann M, et al. Flushing versus not flushing the interface during small-incision lenticule extraction. J Cataract Refract Surg. 2019;45:562–8. https://doi.org/10.1016/j.jcrs.2018.12.001. Epub 2019 Mar 4
Shetty R, Shroff R, Kaweri L, Jayadev C, Kummelil MK, Sinha Roy A. Intra-operative cap repositioning in Small Incision Lenticule Extraction (SMILE) for enhanced visual recovery. Curr Eye Res. 2016;41:1532–8. https://doi.org/10.3109/02713683.2016.1168848
Schiano-Lomoriello D, Bono V, Abicca I, Savini G. Repeatability of anterior segment measurements by optical coherence tomography combined with Placido disk corneal topography in eyes with keratoconus. Sci Rep. 2020;10:1124. https://doi.org/10.1038/s41598-020-57926-7
Plaza-Puche AB, Salerno LC, Versaci F, Romero D, Alio JL. Clinical evaluation of the repeatability of ocular aberrometry obtained with a new pyramid wavefront sensor. Eur J Ophthalmol. 2019;29:585–92. https://doi.org/10.1177/1120672118816060. Epub 2018 Dec 5
Taneri S, Arba-Mosquera S, Rost A, Kießler S, Dick HB. Repeatability and reproducibility of manifest refraction. J Cataract Refract Surg. 2020;46:1659–66. https://doi.org/10.1097/j.jcrs.0000000000000343
Hamilton DR, Chen AC, Khorrami R, Nutkiewicz M, Nejad M. Comparison of early visual outcomes after low-energy SMILE, high-energy SMILE, and LASIK for myopia and myopic astigmatism in the United States. J Cataract Refract Surg. 2021;47:18–26. https://doi.org/10.1097/j.jcrs.0000000000000368
Rahaman A, Rahaman S, Fu H. Glass burn threshold: an innovative method to characterize refractive femtosecond laser performance. Invest Ophthalmol Vis Sci 2022;63:4364–A0301.
Liu J, Wang Y. Influence of preoperative keratometry on refractive outcomes for myopia correction with small incision lenticule extraction. J Refract Surg. 2020;36:374–9. https://doi.org/10.3928/1081597X-20200513-01
Taneri S, Arba-Mosquera S, Rost A, Hansson C, Dick HB. Results of thin-cap small-incision lenticule extraction. J Cataract Refract Surg. 2021;47:439–44. https://doi.org/10.1097/j.jcrs.0000000000000470
Leccisotti A, Fields SV, De Bartolo G. Refractive corneal lenticule extraction with the CLEAR femtosecond laser application. Cornea. 2022. https://doi.org/10.1097/ICO.0000000000003123.
Kaluzny BJ, Verma S, Piotrowiak-Słupska I, Kaszuba-Modrzejewska M, Rzeszewska-Zamiara J, Stachura J, et al. Three-year outcomes of mixed astigmatism correction with single-step transepithelial photorefractive keratectomy with a large ablation zone. J Cataract Refract Surg. 2021;47:450–8. https://doi.org/10.1097/j.jcrs.0000000000000476
Munnerlyn CR, Koons SJ, Marshall J. Photorefractive keratectomy: a technique for laser refractive surgery. J Cataract Refract Surg. 1988;14:46–52. https://doi.org/10.1016/s0886-3350(88)80063-4
Qian Y, Liu Y, Zhou X, Naidu RK. Comparison of corneal power and astigmatism between simulated keratometry, true net power, and total corneal refractive power before and after SMILE surgery. J Ophthalmol. 2017;2017:9659481. https://doi.org/10.1155/2017/9659481.
Sideroudi H, Lazaridis A, Messerschmidt-Roth A, Labiris G, Kozobolis V, Sekundo W. Corneal irregular astigmatism and curvature changes after small incision lenticule extraction: three-year follow-up. Cornea. 2018;37:875–80. https://doi.org/10.1097/ICO.0000000000001532
Ganesh S, Patel U, Brar S. Posterior corneal curvature changes following refractive small incision lenticule extraction. Clin Ophthalmol. 2015;9:1359–64. https://doi.org/10.2147/OPTH.S84354. eCollection 2015
Lee H, Roberts CJ, Arba-Mosquera S, Kang DSY, Reinstein DZ, Kim TI. Relationship between decentration and induced corneal higher-order aberrations following small-incision lenticule extraction procedure. Investig Ophthalmol Vis Sci. 2018;59:2316–24. https://doi.org/10.1167/iovs.17-23451
Pradhan KR, Arba Mosquera S. Twelve-month outcomes of a new refractive lenticular extraction procedure. J Optom. 2023;16:30–41. https://doi.org/10.1016/j.optom.2021.11.001.
Funding
The study was self-financed.
Author information
Authors and Affiliations
Contributions
The authors confirm their contribution to the paper as follows: IG—study conception and design, data collection, analysis and interpretation of results, draft manuscript preparation. MB—study conception and design, data collection, analysis and interpretation of results, draft manuscript preparation. KG—study conception and design, data collection, analysis and interpretation of results. SAM—study conception and design, data collection, analysis and interpretation of results, draft manuscript preparation. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
SAM is an employee at and inventor in several patents owned by SCHWIND eye-tech-solutions. None of the other authors has financial or proprietary interests in materials or methods presented herein.
Ethical approval and consent to participate
The study was conducted according to the guidelines of the Declaration of Helsinki. The study was retrospective with anonymized data. Ethics approval was not required due to the retrospective nature of the review chart. The purpose of this clinical research does not represent a clinical investigation. The medical device was used within its intended purpose without any additional invasive or patient-burdensome procedures used. Informed consent was obtained from all subjects involved in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gabric, I., Bohac, M., Gabric, K. et al. First European results of a new refractive lenticular extraction procedure—SmartSight by SCHWIND eye-tech-solutions. Eye 37, 3768–3775 (2023). https://doi.org/10.1038/s41433-023-02601-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02601-0