Abstract
Data sources Ovid Medline, Embase, EBM Review, Cochrane Central Register of Control Trials and the Cochrane Database of Systematic Reviews.
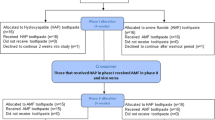
Study selection Randomised controlled trials or prospective cohort studies published in English with ≥10 patients and ≥6 months follow-up (the longest follow-up period was chosen in longitudinal studies which were published more than once). Experimental animal or in vitro studies were excluded.
Data extraction and synthesis Data on the primary outcome reduction in bleeding on probing (BOP) in implants treated surgically for peri-implantitis, and secondary outcomes pocket probing depth (PPD) and RBL (radiographic bone-loss) were extracted and meta-analysis conducted.
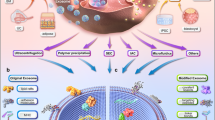
Results Sixteen papers met the inclusion criteria. Four treatment modalities to supplement mechanical debridement were identified: (1) apically repositioned flap, (2) chemical surface decontamination, (3) implantoplasty and (4) bone augmentation. Inconsistent results were evident which were dependent on several treatment-independent factors. No clinical benefits were identified for the additional use of surface decontamination, while limited evidence demonstrated improvement of clinical and radiographic outcomes after implantoplasty. The effect of bone augmentation appeared limited to 'filling' radiographic defects.
The meta-analysis was conducted using eight randomised clinical trials and two controlled prospective cohort studies. Meta-analysis demonstrated that implants treated with surface decontamination had SMD of -0.21 (95% CI: -1.70 to 1.27) for periodontal pocket reduction (PPD) reduction. Only one study reported the effect of implantoplasty on PPD, which shows a significant SMD of -3.33 (95% CI: -4.37 to -2.28 mm).
Bone augmentation with grafting materials and the additional use of membrane resulted in SMD of 0.15 mm (95% CI: -0.55 to 0.84 mm) and 0.30 mm (95% CI: -0.31 to 0.91 mm), respectively. In terms of RBL changes, the use of surface decontamination methods resulted in SMD of 0.54 mm (95% CI: -0.20 to 1.28 mm). Implants treated with implantoplasty had SMD of -3.38 (95% CI: -.43 to -2.33 mm). The SMD for RBL changes after the use of bone augmentation was -1.05 (95% CI: -1.80 to -0.31 mm). However, the additional use of membrane had SMD of -0.16 (95% CI: -0.56 to 0.24 mm.
Conclusions The outcomes of the currently available surgical interventions for peri-implantitis remain unpredictable. There is no reliable evidence to suggest which methods are the most effective. Further randomised controlled studies are needed to identify the best treatment methods.
Similar content being viewed by others
A commentary on
Al-Kadhim KAH, Pritchard MF, Farnell DJJ, Thomas DW, Adams R, Claydon N.
Surgical therapy for peri-implantitis management: a systematic review and meta-analysis. Oral Surg 2018; 11: 200-212.

GRADE rating
Commentary
Replacing edentulous spaces with implants is a viable option for patients to restore the form and function of the oral cavity. Although implants have a good success rate, there are failures due to peri-implantitis which is defined as loss of supporting marginal bone around the implant that, if left untreated, will lead to implant failure. The question for this article addresses the management of patients with peri-implantitis. The search strategy was comprehensive; the authors looked at relevant studies with follow-up reference lists. A limitations of the study was including English papers only.
The authors included randomised controlled trials and prospective studies that present different potential sources of bias. These studies need to be evaluated separately for potential sources of bias, and even though it is mentioned that they assess the quality of the included studies, the authors do not describe the final assessment of the quality of the studies. Hence, it is unclear the overall validity and quality of the included studies.
Even though the authors combine similar interventions such as decontamination methods, implantoplasty, bone augmentation or additional membrane, they should not combine the interventions since the treatments are so diverse by nature. Therefore any results from the present review, due to methodology and the unclear validity and relevance of the included studies, should be interpreted with extreme caution.
A previous systematic review published in 20121 included nine RCTs considered by the authors as high or unclear risk of bias. The authors evaluated: different non-surgical interventions (five trials); adjunctive treatments to non-surgical interventions (one trial); different surgical interventions (two trials); adjunctive therapy to surgical interventions (one trial). The follow-up for the studies ranged from three months to four years. Statistically significant differences were observed in two small trials. After four months adjunctive local antibiotics to manual debridement in patients who lost at least 50% of the bone around implants showed improved mean probing attachment levels (PAL) of 0.61 mm (95% confidence interval (CI) 0.40 to 0.82) and reduced probing pockets depths (PPD) of 0.59 mm (95% CI 0.39 to 0.79). After four years, patients with peri-implant infrabony defects > 3 mm treated with Bio-Oss and resorbable barriers gained 1.4 mm more PAL (95% CI 0.24 to 2.56) and 1.4 mm PPD (95% CI 0.81 to 1.99) than patients treated with a nanocrystalline hydroxyapatite.
Another systematic review with a similar topic concluded that adjunctive resective and/or augmentative measures are promising; however their beneficial effect on the clinical outcome of surgical treatments needs to be further investigated.2
We can all agree that further studies need to be conducted to evaluate the best surgical intervention to minimise peri-implant disease. Most of the interventions seem useful, however the true benefit remains unclear.
References
Esposito M, Grusovin MG, Worthington HV. Interventions for replacing missing teeth: treatment of peri-implantitis. Cochrane Database Syst Rev 2012; 1: CD004970
Schwarz F, Schmucker A, Becker J. Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis and peri-implantitis: a systematic review and meta-analysis. Int J Implant Dent 2015; 1: 22.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
De Bartolo, A., Veitz-Keenan, A. Inconclusive evidence of treatment modalities for peri-implantitis. Evid Based Dent 20, 24–25 (2019). https://doi.org/10.1038/s41432-019-0007-8
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41432-019-0007-8
This article is cited by
-
In vitro surgical and non-surgical air-polishing efficacy for implant surface decontamination in three different defect configurations
Clinical Oral Investigations (2021)
-
From Periodontitis to Periimplantitis—the Quest for the Missing Link
Current Oral Health Reports (2020)
-
Current Protocols for the Treatment of Peri-implantitis
Current Oral Health Reports (2019)