Abstract
Background
Hyperglycemia can promote the development of prostate cancer (PCa). Differential expression levels of miRNAs between PCa patients and controls were also reported. Therefore, we examined the relationship between hyperglycemia and miRNA levels in PCa.
Methods
Relative expression of urinary miR-574-3p, miR-375, miR-205-5p, miR-200b-3p, miR-187-3p, miR-182-5p, and miR-100-5p were investigated in 105 PCa patients and 138 noncancer controls by Real-Time quantitative PCR. Fasting plasma glucose measurements were retrieved from clinical records. The differential miRNA expressions among groups were compared using non-parametric tests. Correlations with glucose and prostate-specific antigen (PSA) were tested using Pearson correlation coefficient.
Results
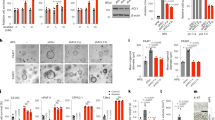
When we analyzed miRNA expression according to glycemic state, significant down-regulations were found for miR-200b-3p, miR-187-3p, miR-182-5p, and miR-100-5p in noncancer controls with high glucose. The lowest down-regulations were observed for miR-187-3p, miR-182-5p, and miR-100-5p. Subsequently, when hyperglycemia was considered in PCa, significant dysregulations of selected miRNAs were found in hyperglycemic PCa patients than in controls with high glucose. In particular, miR-375 and miR-182-5p showed a 3-FC in hyperglycemic PCa patients than controls who left hyperglycemia untreated. Conversely, only a down-regulation of miR-574-3p was observed in PCa patients regardless of glycemic status and only modest down-regulation of miR-574-3p, miR-200b-3p, miR-187-3p and miR-182-5p were found in normoglycemic PCa patients. Next, significant correlations between miRNAs and glucose (miR-200b-3p, miR-100-5p) and PSA (miR-205-5p and miR-187-3p) were detected in controls. Similarly, miR-205-5p and miR-187-3p were correlated with glucose in PCa patients, while miR-574-3p and miR-375 showed inverse relationships.
Conclusions
miRNA dysregulations can occur in hyperglycemic PCa patients as compared to noncancer controls who left hyperglycemia untreated. Hyperglycemia can consistently promote the expression of miR-375 and miR-182-5p. Uncontrolled hyperglycemic state could contribute to the creation of a suitable microenvironment for later PCa development by promoting gene expression.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The dataset used during the current study is available from the corresponding author upon reasonable request.
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68:394–424.
Auvinen A, Moss SM, Tammela TLJ, Taari K, Roobol MJ, Schrader FH, et al. Absolute effect of prostate cancer screening: balance of benefits and harms by center within the European randomized study of prostate cancer screening. Clin Cancer Res. 2015;22:243–9.
Ahdoot M, Wilbur AR, Reese SE, Lebastchi AH, Mehralivand S, Gomella PT, et al. MRI-targeted, systematic, and combined biopsy for prostate cancer diagnosis. N. Engl J Med. 2020;382:917–28.
Bartel DP. MicroRNAs: target recognition and regulatory functions. Cell. 2009;136:215–33.
Nair VS, Pritchard CC, Tewari M, Ioannidis JPA. Design and analysis for studying microRNAs in human disease: a primer on -omic technologies. Am J Epidemiol. 2014;180:140–52.
Volinia S, Calin GA, Liu C-G, Ambs S, Cimmino A, Petrocca F, et al. A microRNA expression signature of human solid tumors defines cancer gene targets. Proc Natl Acad Sci USA. 2006;103:2257–61.
Ardekani AM, Naeini MM. The role of MicroRNAs in human diseases. Avicenna J Med Biotechnol. 2010;2:161–79.
Fabris L, Ceder Y, Chinnaiyan AM, Jenster GW, Sorensen KD, Tomlins S, et al. The potential of MicroRNAs as prostate cancer biomarkers. Eur Urol. 2016;70:312–22.
Aveta A, Cilio S, Contieri R, Spena G, Napolitano L, Manfredi C, et al. Urinary MicroRNAs as biomarkers of urological cancers: a systematic review. Int J Mol Sci. 2023;24:10846.
Marrone MT, Selvin E, Barber JR, Platz EA, Joshu CE. Hyperglycemia, classified with multiple biomarkers simultaneously in men without diabetes, and risk of fatal prostate cancer. Cancer Prev Res. 2019;12:103.
Murtola TJ, Vihervuori VJY, Lahtela J, Talala K, Taari K, Tammela TLJ, et al. Fasting blood glucose, glycaemic control and prostate cancer risk in the Finnish Randomized Study of Screening for Prostate Cancer. Br J cancer. 2018;118:1248–54.
Murtola TJ, Salli SM, Talala K, Taari K, Tammela TLJ, Auvinen A. Blood glucose, glucose balance, and disease-specific survival after prostate cancer diagnosis in the Finnish Randomized Study of Screening for Prostate Cancer. Prostate Cancer Prostatic Dis. 2019;22:453–60.
Arthur R, Muller H, Garmo H, Holmberg L, Stattin P, Malmstrom H, et al. Association between baseline serum glucose, triglycerides and total cholesterol, and prostate cancer risk categories. Cancer Med. 2016;5:1307–18.
Paiva RM, Zauli DAG, Neto BS, Brum IS. Urinary microRNAs expression in prostate cancer diagnosis: a systematic review. Clin Transl Oncol. 2020;22:2061–73.
Al-Mahayni S, Ali M, Khan M, Jamsheer F, Moin ASM, Butler AE. Glycemia-induced miRNA changes: a review. Int J Mol Sci. 2023;24:7488.
Hu Z, Dong J, Wang L-E, Ma H, Liu J, Zhao Y, et al. Serum microRNA profiling and breast cancer risk: the use of miR-484/191 as endogenous controls. Carcinogenesis. 2012;33:828–34.
Echouffo-Tcheugui JB, Selvin E. Prediabetes and what it means: the epidemiological evidence. Annu Rev Public Health. 2021;42:59–77.
Oger F, Gheeraert C, Mogilenko D, Benomar Y, Molendi-Coste O, Bouchaert E, et al. Cell-specific dysregulation of microrna expression in obese white adipose tissue. J Clin Endocrinol Metab. 2014;99:2821–33.
Weale CJ, Matshazi DM, Davids SFG, Raghubeer S, Erasmus RT, Kengne AP, et al. Circulating miR-30a-5p and miR-182-5p in prediabetes and screen-detected diabetes mellitus. Diabetes Metab Syndr Obes. 2020;13:5037–47.
Pek SLT, Sum CF, Lin MX, Cheng AKS, Wong MTK, Lim SC, et al. Circulating and visceral adipose miR-100 is down-regulated in patients with obesity and Type 2 diabetes. Mol Cell Endocrinol. 2016;427:112–23.
Li X, Li J, Cai Y, Peng S, Wang J, Xiao Z, et al. Hyperglycaemia-induced miR-301a promotes cell proliferation by repressing p21 and Smad4 in prostate cancer. Cancer Lett. 2018;418:211–20.
Gajeton J, Krukovets I, Muppala S, Verbovetskiy D, Zhang J, Stenina-Adognravi O. Hyperglycemia-induced miR-467 drives tumor inflammation and growth in breast cancer. Cancers. 2021;13:1346.
Hudson RS, Yi M, Esposito D, Watkins SK, Hurwitz AA, Yfantis HG, et al. MicroRNA-1 is a candidate tumor suppressor and prognostic marker in human prostate cancer. Nucleic Acids Res. 2012;40:3689–703.
Abramovic I, Vrhovec B, Skara L, Vrtaric A, Nikolac Gabaj N, Kulis T, et al. MiR-182-5p and miR-375-3p have higher performance than PSA in discriminating prostate cancer from Benign prostate hyperplasia. Cancers. 2021;13:2068.
Szczyrba J, Loprich E, Wach S, Jung V, Unteregger G, Barth S, et al. The MicroRNA profile of prostate carcinoma obtained by deep sequencing. Mol Cancer Res. 2010;8:529–38.
Konoshenko MY, Lekchnov EA, Bryzgunova OE, Zaporozhchenko IA, Yarmoschuk SV, Pashkovskaya OA, et al. The panel of 12 cell-free microRNAs as potential biomarkers in prostate neoplasms. Diagnostics. 2020;10:38.
Wang NL, Li Q, Cheng NH, Guan G, Wang ZL, Qin Y, et al. miR-205 is frequently downregulated in prostate cancer and acts as a tumor suppressor by inhibiting tumor growth. Asian J Androl. 2013;15:735–41.
Nayak B, Khan N, Garg H, Rustagi Y, Singh P, Seth A, et al. Role of miRNA-182 and miRNA-187 as potential biomarkers in prostate cancer and its correlation with the staging of prostate cancer. Int Braz J Urol. 2020;46:614–23.
Li Y, Li J, Yu H, Liu Y, Song H, Tian X, et al. HOXA5-miR-574-5p axis promotes adipogenesis and alleviates insulin resistance. Mol Ther Nucleic Acids. 2022;27:200–10.
Raza ST, Rizvi S, Afreen S, Srivastava S, Siddiqui Z, Fatima N, et al. Association of the circulating micro-RNAs with susceptible and newly diagnosed type 2 diabetes mellitus cases. Adv Biomark Sci Technol. 2022;5:57–67.
Lieb V, Weigelt K, Scheinost L, Fischer K, Greither T, Marcou M, et al. Serum levels of miR-320 family members are associated with clinical parameters and diagnosis in prostate cancer patients. Oncotarget. 2018;9:10402–10416.
Singh PK, Preus L, Hu Q, Yan L, Long MD, Morrison CD, et al. Serum microRNA expression patterns that predict early treatment failure in prostate cancer patients. Oncotarget. 2014;5:824–40.
Ramteke P, Deb A, Shepal V, Bhat MK. Hyperglycemia associated metabolic and molecular alterations in cancer risk, progression, treatment, and mortality. Cancers. 2019;11:1402.
Yaribeygi H, Atkin SL, Sahebkar A. A review of the molecular mechanisms of hyperglycemia-induced free radical generation leading to oxidative stress. J Cell Physiol. 2018;234:1300–12.
He S, Shi J, Mao J, Luo X, Liu W, Liu R, et al. The expression of miR-375 in prostate cancer: a study based on GEO, TCGA data and bioinformatics analysis. Pathol Res Pract. 2019;215:152375.
Pickl JMA, Tichy D, Kuryshev VY, Tolstov Y, Falkenstein M, Schuler J, et al. Ago-RIP-Seq identifies Polycomb repressive complex I member CBX7 as a major target of miR-375 in prostate cancer progression. Oncotarget. 2016;7:59589–603.
Liu Y, Yang C, Chen S, Liu W, Liang J, He S, et al. Cancer-derived exosomal miR-375 targets DIP2C and promotes osteoblastic metastasis and prostate cancer progression by regulating the Wnt signaling pathway. Cancer Gene Ther. 2022;30:437–49.
Wang D, Lu G, Shao Y, Xu D. MiR-182 promotes prostate cancer progression through activating Wnt/β-catenin signal pathway. Biomed Pharmacother. 2018;99:334–9.
Stafford MYC, McKenna DJ. MiR-182 is upregulated in prostate cancer and contributes to tumor progression by targeting MITF. Int J Mol Sci. 2023;24:1824.
Ye X, Tam WL, Shibue T, Kaygusuz Y, Reinhardt F, Ng Eaton E, et al. Distinct EMT programs control normal mammary stem cells and tumour-initiating cells. Nature. 2015;525:256–60.
Gonzalez P, Lozano P, Ros G, Solano F. Hyperglycemia and oxidative stress: an integral, updated and critical overview of their metabolic interconnections. Int J Mol Sci. 2023;24:9352.
Pellacani D, Droop AP, Frame FM, Simms MS, Mann VM, Collins AT, et al. Phenotype-independent DNA methylation changes in prostate cancer. Br J Cancer. 2018;119:1133–43.
O’Hagan HeatherM, Wang W, Sen S, DeStefano Shields C, Lee Stella S, Zhang Yang W, et al. Oxidative damage targets complexes containing DNA methyltransferases, SIRT1, and polycomb members to promoter CpG islands. Cancer Cell. 2011;20:606–19.
Peluso M, Srivatanakul P, Jedpiyawongse A, Sangrajrang S, Munnia A, Piro S, et al. Aromatic DNA adducts and number of lung cancer risk alleles in Map-Ta-Phut Industrial Estate workers and nearby residents. Mutagenesis. 2013;28:57–63.
Kutwin P, Konecki T, Borkowska EM, Magdalena T-B, Jablonowski Z. Urine miRNA as a potential biomarker for bladder cancer detection - a meta-analysis. Cent Eur J Urol. 2018;71:177–85.
Abramovic I, Ulamec M, Katusic Bojanac A, Bulic-Jakus F, Jezek D, Sincic N. miRNA in prostate cancer: challenges toward translation. Epigenomics. 2020;12:543–58.
Li W, Zhang X, Sang H, Zhou Y, Shang C, Wang Y, et al. Effects of hyperglycemia on the progression of tumor diseases. J Exp Clin Cancer Res. 2019;38:327.
Brennan E, McClelland A, Hagiwara S, Godson C, Kantharidis P. miRNAs in the pathophysiology of diabetes and their value as biomarkers. In: Epigenetic biomarkers and diagnostics. Boston: Academic Press; 2016, p. 643–61.
Chen J-Y, Wang P-Y, Liu M-Z, Lyu F, Ma M-W, Ren X-Y, et al. Biomarkers for prostate cancer: from diagnosis to treatment. Diagnostics. 2023;13:3350.
Pang KH, Rosario DJ, Morgan SL, Catto JWF. Evaluation of a short RNA within prostate cancer gene 3 in the predictive role for future cancer using non-malignant prostate biopsies. PloS One. 2017;12:e0175070.
Funding
This work was partially supported by AIRC (Project Code: 17763) and Tuscany Region, Italy.
Author information
Authors and Affiliations
Contributions
Concept and design: [MZ, FC, EB, SS, MRR and MP]. Drafting of the manuscript: [MP]. Acquisition, analysis or interpretation of data, critical revisions to manuscript: [all authors]. Statistical analysis: [MP].
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Russo, V., Tamburrino, L., Morselli, S. et al. Hyperglycemia and microRNAs in prostate cancer. Prostate Cancer Prostatic Dis (2024). https://doi.org/10.1038/s41391-024-00809-z
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41391-024-00809-z