Abstract
Background
We hypothesized a pro-inflammatory diet would be associated with higher prostate cancer (PC) risk.
Methods
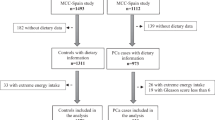
We prospectively recruited incident PC cases (n = 254) and controls (n = 328) at the Durham Veteran Affairs, from 2007 to 2018. From a self-completed 61-item Food Frequency Questionnaire, we calculated dietary inflammatory index (DII®) scores with and without supplements. We examined the association between DII scores with and without supplements and overall PC risk using logistic regression and risk of low-grade PC (grade group 1) and high-grade PC (grade group 2–5) with multinomial logistic regression.
Results
Cases were more likely to be Black (58 vs. 42%), had higher PSA (6.4 vs. 0.8 ng/ml), lower BMI (29.1 vs. 30.6 kg/m2) and were older (64 vs. 62 years) versus controls (all p < 0.01). Both black controls and cases had higher DII scores with and without supplements, though the DII scores with supplements in controls was not significant. On multivariable analysis, there were no associations between DII with or without supplements and overall PC risk (p-trend = 0.14, p-trend = 0.09, respectively) or low-grade PC (p-trend = 0.72, p-trend = 0.47, respectively). Higher DII scores with (p-trend = 0.04) and without supplements (p = 0.08) were associated with high-grade PC, though the association for DII without supplements was not significant.
Conclusions
A pro-inflammatory diet was more common among Black men and associated with high-grade PC in our case–control study. The degree to which a pro-inflammatory diet contributes to PC race disparities warrants further study. If confirmed, studies should test whether a low-inflammatory diet can prevent high-grade PC, particularly among Black men.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Global Burden of Disease Cancer Collaboration, Fitzmaurice C, Akinyemiju TF, Al Lami FH, Alam T, Alizadeh-Navaei R, Allen C, et al. Global, regional, and national cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life-years for 29 cancer groups, 1990 to 2016: a systematic analysis for the global burden of disease study. JAMA Oncol 2018; 4:1553–68.
Siegel RL, Miller KD, Jemal A. Cancer Stat. 2018;68:7–30.
Lin PH, Aronson W, Freedland SJ. Nutrition, dietary interventions and prostate cancer: the latest evidence. BMC Med. 2015;13:3.
Masko EM, Allott EH, Freedland SJ. The relationship between nutrition and prostate cancer: is more always better? Eur Urol. 2013;63:810–20.
Asghari G, Mirmiran P, Yuzbashian E, Azizi F. A systematic review of diet quality indices in relation to obesity. Br J Nutr. 2017;117:1055–65.
Prentice RL, Anderson GL. The women’s health initiative: lessons learned. Annu Rev Public Health. 2008;29:131–50.
Fowler ME, Akinyemiju TF. Meta-analysis of the association between dietary inflammatory index (DII) and cancer outcomes. Int J Cancer. 2017;141:2215–27.
Kim JH, Kim J. Index-based dietary patterns and the risk of prostate cancer. Clin Nutr Res. 2017;6:229–46.
Mengus C, Le Magnen C, Trella E, Yousef K, Bubendorf L, Provenzano M, et al. Elevated levels of circulating IL-7 and IL-15 in patients with early stage prostate cancer. J Transl Med. 2011;9:162.
Wallace TA, Prueitt RL, Yi M, Howe TM, Gillespie JW, Yfantis HG, et al. Tumor immunobiological differences in prostate cancer between African-American and European-American men. Cancer Res. 2008;68:927–36.
Gurel B, Lucia MS, Thompson IM Jr, Goodman PJ, Tangen CM, Kristal AR, et al. Chronic inflammation in benign prostate tissue is associated with high-grade prostate cancer in the placebo arm of the prostate cancer prevention trial. Cancer Epidemiol Biomark Prev. 2014;23:847–56.
Esmaillzadeh A, Kimiagar M, Mehrabi Y, Azadbakht L, Hu FB, Willett WC. Dietary patterns and markers of systemic inflammation among Iranian women. J Nutr. 2007;137:992–8.
Esposito K, Marfella R, Ciotola M, Di Palo C, Giugliano F, Giugliano G, et al. Effect of a Mediterranean-style diet on endothelial dysfunction and markers of vascular inflammation in the metabolic syndrome: a randomized trial. J Am Med Assoc. 2004;292:1440–6.
Shivappa N, Steck SE, Hurley TG, Hussey JR, Hebert JR. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014;17:1689–96.
Shivappa N, Steck SE, Hurley TG, Hussey JR, Ma Y, Ockene IS, et al. A population-based dietary inflammatory index predicts levels of C-reactive protein in the Seasonal Variation of Blood Cholesterol Study (SEASONS). Public Health Nutr. 2014;17:1825–33.
Cavicchia PP, Steck SE, Hurley TG, Hussey JR, Ma Y, Ockene IS, et al. A new dietary inflammatory index predicts interval changes in serum high-sensitivity C-reactive protein. J Nutr. 2009;139:2365–72.
Shivappa N, Bosetti C, Zucchetto A, Montella M, Serraino D, La Vecchia C, et al. Association between dietary inflammatory index and prostate cancer among Italian men. Br J Nutr. 2015;113:278–83.
Shivappa N, Hebert JR, Askari F, Kardoust Parizi M, Rashidkhani B. Increased inflammatory potential of diet is associated with increased risk of prostate cancer in Iranian men. Int J Vitam Nutr Res. 2016;86:161–8.
Shivappa N, Jackson MD, Bennett F, Hebert JR. Increased dietary inflammatory index (DII) is associated with increased risk of prostate cancer in Jamaican men. Nutr Cancer. 2015;67:941–8.
Shivappa N, Miao Q, Walker M, Hebert JR, Aronson KJ. Association between a dietary inflammatory index and prostate cancer risk in Ontario, Canada. Nutr Cancer. 2017;69:825–32.
Shivappa N, Niclis C, Coquet JB, Roman MD, Hebert JR, Diaz MDP. Increased inflammatory potential of diet is associated with increased odds of prostate cancer in Argentinian men. Cancer Causes Control. 2018;29:803–13.
Graffouillere L, Deschasaux M, Mariotti F, Neufcourt L, Shivappa N, Hébert JR, et al. The dietary inflammatory index is associated with prostate cancer risk in French middle-aged adults in a prospective study. J Nutr. 2016;146:785–91.
McMahon DM, Burch JB, Hebert JR, Hardin JW, Zhang J, Wirth MD. et al. Diet-related inflammation and risk of prostate cancer in the California Men’s Health Study. Ann Epidemiol. 2019;29:30–38.
Vazquez-Salas RA, Shivappa N, Galvan-Portillo M, Lopez-Carrillo L, Hebert JR, Torres-Sanchez L. Dietary inflammatory index and prostate cancer risk in a case-control study in Mexico. Br J Nutr. 2016;116:1945–53.
Antonelli JA, Jones LW, Banez LL, Thomas JA, Anderson K, Taylor LA, et al. Exercise and prostate cancer risk in a cohort of veterans undergoing prostate needle biopsy. J Urol. 2009;182:2226–31.
Williams CD, Whitley BM, Hoyo C, Grant DJ, Iraggi JD, Newman KA, et al. A high ratio of dietary n-6/n-3 polyunsaturated fatty acids is associated with increased risk of prostate cancer. Nutr Res. 2011;31:1–8.
Demark-Wahnefried W, Aziz NM, Rowland JH, Pinto BM. Riding the crest of the teachable moment: promoting long-term health after the diagnosis of cancer. J Clin Oncol. 2005;23:5814–30.
Pinto BM, Eakin E, Maruyama NC. Health behavior changes after a cancer diagnosis: what do we know and where do we go from here? Ann Behav Med. 2000;22:38–52.
Willett WC, Sampson L, Stampfer MJ, Rosner B, Bain C, Witschi J, et al. Reproducibility and validity of a semiquantitative food frequency questionnaire. Am J Epidemiol. 1985;122:51–65.
Tabung FK, Steck SE, Zhang J, Ma Y, Liese AD, Agalliu I, et al. Construct validation of the dietary inflammatory index among postmenopausal women. Ann Epidemiol. 2015;25:398–405.
Wirth MD, Shivappa N, Davis L, Hurley TG, Ortaglia A, Drayton R, et al. Construct validation of the Dietary Inflammatory Index among African Americans. J Nutr Health Aging. 2017;21:487–91.
Wirth MD, Burch J, Shivappa N, Violanti JM, Burchfiel CM, Fekedulegn D, et al. Association of a Dietary Inflammatory Index with inflammatory indices and metabolic syndrome among police officers. J Occup Environ Med. 2014;56:986–9.
Ramallal R, Toledo E, Martinez-Gonzalez MA, Hernández-Hernández A, García-Arellano A, Shivappa N, et al. Dietary Inflammatory Index and incidence of cardiovascular disease in the SUN cohort. PLoS ONE. 2015;10:e0135221.
Shivappa N, Hebert JR, Rietzschel ER, De Buyzere ML, Langlois M, Debruyne E, et al. Associations between dietary inflammatory index and inflammatory markers in the Asklepios Study. Br J Nutr. 2015;113:665–71.
Willett WC, Howe GR, Kushi LH. Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr. 1997;65:1220S–1228S.
Nelson WG, DeWeese TL, DeMarzo AM. The diet, prostate inflammation, and the development of prostate cancer. Cancer Metastas Rev. 2002;21:3–16.
Nelson WG, Demarzo AM, Yegnasubramanian S. The diet as a cause of human prostate cancer. Cancer Treat Res. 2014;159:51–68.
Cross AJ, Peters U, Kirsh VA, Andriole GL, Reding D, Hayes RB, et al. A prospective study of meat and meat mutagens and prostate cancer risk. Cancer Res. 2005;65:11779–84.
Tabung FK, Smith-Warner SA, Chavarro JE, Fung TT, Hu FB, Willett WC, et al. An empirical dietary inflammatory pattern score enhances prediction of circulating inflammatory biomarkers in adults. J Nutr. 2017;147:1567–77.
Travis RC, Spencer EA, Allen NE, Appleby PN, Roddam AW, Overvad K, et al. Plasma phyto-oestrogens and prostate cancer in the European Prospective Investigation into Cancer and Nutrition. Br J Cancer. 2009;100:1817–23.
Jayedi A, Emadi A, Shab-Bidar S. Dietary Inflammatory Index and site-specific cancer risk: a systematic review and dose-response meta-analysis. Adv Nutr. 2018;9:388–403.
Kim Y, Jeon Y, Lee H, Lee D, Shim B. The prostate cancer patient had higher C-reactive protein than BPH patient. Korean J Urol. 2013;54:85–88.
Tindall EA, Severi G, Hoang HN, Southey MC, English DR, Hopper JL, et al. Interleukin-6 promoter variants, prostate cancer risk, and survival. Prostate. 2012;72:1701–7.
Vidal AC, Howard LE, Moreira DM, Castro-Santamaria R, Andriole GL, Freedland SJ. Aspirin, NSAIDs, and risk of prostate cancer: results from the REDUCE study. Clin Cancer Res. 2015;21:756–62.
Sourbeer KN, Howard LE, Andriole GL, Moreira DM, Castro-Santamaria R, Freedland SJ, et al. Metabolic syndrome-like components and prostate cancer risk: results from the Reduction by Dutasteride of Prostate Cancer Events (REDUCE) study. BJU Int. 2015;115:736–43.
Kato H, Sekine Y, Furuya Y, Miyazawa Y, Koike H, Suzuki K. Metformin inhibits the proliferation of human prostate cancer PC-3 cells via the downregulation of insulin-like growth factor 1 receptor. Biochem Biophys Res Commun. 2015;461:115–21.
Osei K, Schuster DP. Effects of race and ethnicity on insulin sensitivity, blood pressure, and heart rate in three ethnic populations: comparative studies in African-Americans, African immigrants (Ghanaians), and white Americans using ambulatory blood pressure monitoring. Am J Hypertens. 1996;9:1157–64.
Haffner SM, D’Agostino R, Saad MF, Rewers M, Mykkänen L, Selby J, et al. Increased insulin resistance and insulin secretion in nondiabetic African-Americans and Hispanics compared with non-Hispanic whites. The Insulin Resistance Atherosclerosis Study. Diabetes. 1996;45:742–8.
Kim HS, Moreira DM, Jayachandran J, Gerber L, Bañez LL, Vollmer RT, et al. Prostate biopsies from black men express higher levels of aggressive disease biomarkers than prostate biopsies from white men. Prostate Cancer Prostatic Dis. 2011;14:262–265.50.
Gaines AR, Turner EL, Moorman PG, Freedland SJ, Keto CJ, McPhail ME, et al. The association between race and prostate cancer risk on initial biopsy in an equal access, multiethnic cohort. Cancer Causes Control. 2014;25:1029–35.
Funding
This study was supported by the National Institutes of Health (grant number: K24 CA160653) and Department of Defense Award (DOD W81XWH-16-1-0750). ACV was supported by a Research Scholar Grant, RSG-18-018-01- CPHPS, from the American Cancer Society.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
JRH owns controlling interest in Connecting Health Innovations LLC (CHI), a company planning to license the right to his invention of the dietary inflammatory index (DII®) from the University of South Carolina in order to develop computer and smart phone applications for patient counseling and dietary intervention in clinical settings. NS is an employee of CHI. The subject matter of this paper will not have any direct bearing on the activities of CHI, nor has CHI exerted any influence on this project. The other authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vidal, A.C., Oyekunle, T., Howard, L.E. et al. Dietary inflammatory index (DII) and risk of prostate cancer in a case–control study among Black and White US Veteran men. Prostate Cancer Prostatic Dis 22, 580–587 (2019). https://doi.org/10.1038/s41391-019-0143-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-019-0143-4
This article is cited by
-
Interaction between drinking and dietary inflammatory index affects prostate specific antigen: a cross-sectional study
BMC Geriatrics (2023)
-
Atopic allergic conditions and prostate cancer risk and survival in the Multiethnic Cohort study
British Journal of Cancer (2023)
-
Dietary inflammatory index and prostate cancer risk: MCC-Spain study
Prostate Cancer and Prostatic Diseases (2022)