Abstract
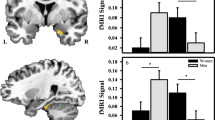
Prior studies show that individuals with alcohol use disorder exhibit exaggerated behavioral and brain reactivity to uncertain threats (U-threat). It is posited this brain-based factor emerges early in life and contributes to the onset and escalation of alcohol problems. However, no study to date has tested this theory using a longitudinal within-subjects design. Ninety-five young adults, ages 17–19, with minimal alcohol exposure and established risk factors for alcohol use disorder participated in this multi-session study with a 1-year tracking period. Startle eyeblink potentiation and brain activation were collected at separate baseline sessions during the well-validated No-Predictable-Unpredictable (NPU) threat-of-shock task designed to probe reactivity to U-threat and predictable threat (P-threat). Participants self-reported their drinking behavior over the past 90 days at baseline and one-year later. We fit a series of multilevel hurdle models to model the binary outcome of whether binge drinking occurred and the continuous outcome of number of binge drinking episodes. Zero-inflated binary submodels revealed that greater baseline startle reactivity, bilateral anterior insula (AIC) reactivity, and dorsal anterior cingulate cortex (dACC) reactivity to U-threat were associated with increased probability of binge drinking. There were no other associations between reactivity to U- and P-threat and probability of binge drinking and number of binging episodes. These results demonstrate that exaggerated reactivity to U-threat is a brain-based individual difference factor that connotes risk for problem drinking. These findings also add to a growing literature implicating AIC and dACC dysfunction in the pathophysiology of alcohol use disorder.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 13 print issues and online access
$259.00 per year
only $19.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Griswold MG, Fullman N, Hawley C, Arian N, Zimsen SR, Tymeson HD, et al. Alcohol use and burden for 195 countries and territories, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2018;392:1015–35.
Rehm J, Dawson D, Frick U, Gmel G, Roerecke M, Shield KD, et al. Burden of disease associated with alcohol use disorders in the United States. Alcohol Clin Exp Res. 2014;38:1068–77.
Substance Abuse and Mental Health Services Administration. Report to congress on the prevention and reduction of underage drinking. Washington, DC: Author; 2015.
Substance Abuse and Mental Health Services Administration. Results from the 2015 National Survey on Drug Use and Health: Detailed Tables. Rockville, MD: U.S. Department of Health and Human Services; 2016.
Substance Abuse and Mental Health Services Administration. Key substance use and mental health indicators in the United States: Results from the 2017 National Survey on Drug Use and Health (HHS Publication No. SMA 18-5068, NSDUH Series H-53). Rockville, MD: Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration; 2018. Retrieved from https://www.samhsa.gov/data
Barlow DH. Unraveling the mysteries of anxiety and its disorders from the perspective of emotion theory. Am Psychol. 2000;55:1247–63.
Davis M, Walker DL, Miles L, Grillon C. Phasic vs. sustained fear in rats and humans: role of the extended amygdala in fear vs anxiety. Neuropsychopharmacology. 2010;35:105–35.
Alvarez RP, Chen G, Bodurka J, Kaplan R, Grillon C. Phasic and sustained fear in humans elicits distinct patterns of brain activity. Neuroimage 2011;1:389–40.
Davis M. Neural systems involved in fear and anxiety measured with fear-potentiated startle. Am Psychol. 2006;61:741–5.
Carleton RN, Mulvogue MK, Thibodeau MA, McCabe RE, Antony MM, Asmundson GJ. Increasingly certain about uncertainty: Intolerance of uncertainty across anxiety and depression. J Anxiety Disord. 2012;26:468–79.
Schmitz A, Grillon C. Assessing fear and anxiety in humans using the threat of predictable and unpredictable aversive events (the NPU-threat test). Nat Protoc. 2012;7:527–32.
Grillon C, Baas J. A review of the modulation of the startle reflex by affective states and its application in psychiatry. Clin Neurophysiol. 2003;114:1557–79.
Grupe DW, Nitschke JB. Uncertainty and anticipation in anxiety: an integrated neurobiological and psychological perspective. Nat Rev Neurosci. 2013;14:488–501.
Morriss J, Gell M, van Reekum CM. The uncertain brain: a co-ordinate based meta-analysis of the neural signatures supporting uncertainty during different contexts. Neurosci Biobehav Rev. 2019;96:241–9.
Gorka SM, Lieberman L, Shankman SA, Phan KL. Association between neural reactivity and startle reactivity to uncertain threat in two independent samples. Psychophysiology. 2017;54:652–62.
Gorka SM, Shankman SA. Preliminary evidence that reactivity to uncertain threat is an endophenotype for alcohol use disorder. Drug Alcohol Depend. 2017;180:265–71.
Gorka SM, Kreutzer KA, Petrey KM, Radoman M, Phan KL. Behavioral and neural sensitivity to uncertain threat in individuals with alcohol use disorder: Associations with drinking behaviors and motives. Addict Biol. 2020;25:e12774.
Gorka SM, Nelson BD, Shankman SA. Startle response to unpredictable threat in comorbid panic disorder and alcohol dependence. Drug Alcohol Depend. 2013;132:216–22.
Gorka SM, Lieberman L, Phan KL, Shankman SA. Association between problematic alcohol use and reactivity to uncertain threat in two independent samples. Drug Alcohol Depend. 2016;164:89–96.
Moberg CA, Bradford DE, Kaye JT, Curtin JJ. Increased startle potentiation to unpredictable stressors in alcohol dependence: possible stress neuroadaptation in humans. J Abnorm Psychol. 2017;126:441.
Moberg CA, Curtin JJ. Alcohol selectively reduces anxiety but not fear: startle response during unpredictable versus predictable threat. J Abnorm Psychol. 2009;118:335–47.
Hefner KR, Moberg CA, Hachiya LY, Curtin JJ. Alcohol stress response dampening during imminent versus distal, uncertain threat. J Abnorm Psychol. 2013;122:756–69.
Gorka SM, Phan KL, Childs E. Acute calming effects of alcohol are associated with disruption of the salience network. Addict Biol. 2018;23:921–30.
Gorka SM, Hee D, Lieberman L, Mittal VA, Phan KL, Shankman SA. Reactivity to uncertain threat as a familial vulnerability factor for alcohol use disorder. Psychol Med. 2016;46:3349–58.
Brown SA, McGue M, Maggs J, Schulenberg J, Hingson R, Swartzwelder S, et al. Underage alcohol use: summary of developmental processes and mechanisms: ages 16–20. Alcohol Res Health. 2009;32:41.
Courtney KE, Polich J. Binge drinking in young adults: data, definitions, and determinants. Psychol Bull. 2009;135:142–56.
Ewing SWF, Sakhardande A, Blakemore SJ. The effect of alcohol consumption on the adolescent brain: a systematic review of MRI and fMRI studies of alcohol-using youth. NeuroImage Clin. 2014;5:420–37.
Yuen WS, Chan G, Bruno R, Clare P, Mattick R, Aiken A, et al. Adolescent alcohol use trajectories: risk factors and adult outcomes. Pediatrics. 2020;146:e20200440.
Wechsler H, Kuo M, Lee H, Dowdall GW. Environmental correlates of underage alcohol use and related problems of college students. Am J Prev Med. 2000;19:24–29.
American Psychiatric Association. Structured clinical interview for DSM‐5(SCID‐5). 2015. http://www.appi.org/products/structured-clinical-interview-for-dsm-5-scid-5/
Watson D, O’Hara MW, Naragon-Gainey K, Koffel E, Chmielewski M, Kotov R, et al. Development and validation of new anxiety and bipolar symptom scales for an expanded version of the IDAS (the IDAS-II). Assessment. 2012;19:399–420.
Gorka SM, Burkhouse KL, Klumpp H, Kennedy AE, Afshar K, Francis J, et al. Error-related brain activity as a treatment moderator and index of symptom change during cognitive-behavioral therapy or selective serotonin reuptake inhibitors. Neuropsychopharmacol. 2018;43:1355–63.
Sobell LC, Sobell MB. Timeline follow-back. In: Measuring alcohol consumption. Totowa, NJ: Humana Press; 1992. p. 41–72.
Sobell LC, Maisto SA, Sobell MB, Cooper AM. Reliability of alcohol abusers’ self-reports of drinking behavior. Behav Res Ther. 1979;17:157–60.
Grant KA, Tonigan JS, Miller WR. Comparison of three alcohol consumption measures: a concurrent validity study. J Stud Alcohol. 1995;56:168–72.
Blumenthal TD, Cuthbert BN, Filion DL, Hackley S, Lipp OV, Van, et al. Committee report: guidelines for human startle eyeblink electromyographic studies. Psychophysiol. 2005;42:1–15.
Radoman M, Lieberman L, Jimmy J, Gorka SM. Shared and unique neural circuitry underlying temporally unpredictable threat and reward processing. Soc Cogn Affect Neurosci. 2021;16:370–82.
Atkins DC, Baldwin SA, Zheng C, Gallop RJ, Neighbors C. A tutorial on count regression and zero-altered count models for longitudinal substance use data. Psychol Addict Behav. 2013;27:166.
Brooks ME, Kristensen K, Van Benthem KJ, Magnusson A, Berg CW, Nielsen A, et al. glmmTMB balances speed and flexibility among packages for zero-inflated generalized linear mixed modeling. R J. 2017;9:378–400.
Shihata S, McEvoy PM, Mullan BA, Carleton RN. Intolerance of uncertainty in emotional disorders: what uncertainties remain? J Anxiety Disord. 2016;41:115–24.
Bradford DE, Shapiro BL, Curtin JJ. How bad could it be? Alcohol dampens stress responses to threat of uncertain intensity. Psychol Sci. 2013;24:2541–9.
Oei TP, Baldwin AR. Expectancy theory: a two-process model of alcohol use and abuse. J Stud Alcohol. 1994;55:525–34.
Baker TB, Piper ME, McCarthy DE, Majeskie MR, Fiore MC. Addiction motivation reformulated: an affective processing model of negative reinforcement. Psychol Rev. 2004;111:33.
McCarthy DE, Curtin JJ, Piper ME, Baker TB. Negative reinforcement: possible clinical implications of an integrative model. In: Kassel JD, editor. Substance abuse and emotion. Washington, D.C.: American Psychological Association; 2010. p. 15–42.
Seeley WW, Menon V, Schatzberg AF, Keller J, Glover GH, Kenna H, et al. Dissociable intrinsic connectivity networks for salience processing and executive control. J Neurosci. 2007;27:2349–56.
Menon V, Uddin LQ. Saliency, switching, attention and control: a network model of insula function. Brain Struct Funct. 2010;214:655–67.
Craig AD. How do you feel—now? The anterior insula and human awareness. Nat Rev Neurosci. 2009;10:59–70.
Peters SK, Dunlop K, Downar J. Cortico-striatal-thalamic loop circuits of the salience network: a central pathway in psychiatric disease and treatment. Front Syst Neurosci. 2016;10:104.
Zhu X, Cortes CR, Mathur K, Tomasi D, Momenan R. Model‐free functional connectivity and impulsivity correlates of alcohol dependence: a resting‐state study. Addict Biol. 2017;22:206–17.
Naqvi NH, Gaznick N, Tranel D, Bechara A. The insula: a critical neural substrate for craving and drug seeking under conflict and risk. Ann NY Acad Sci. 2014;1316:53–70.
Ibrahim C, Rubin-Kahana DS, Pushparaj A, Musiol M, Blumberger DM, Daskalakis ZJ, et al. The insula: a brain stimulation target for the treatment of addiction. Front Pharmacol. 2019;10:720.
De Bellis MD, Nooner KB, Brumback T, Clark DB, Tapert SF, Brown SA. Posttraumatic stress symptoms predict transition to future adolescent and young adult moderate to heavy drinking in the NCANDA sample. Curr Addict Rep. 2020;7:99–107.
Funding
This work was supported by the National Institute of Alcohol Abuse and Alcoholism (NIAAA) of the National Institutes of Health (K23AA025111 awarded to SMG). The funding source had no role in the present manuscript.
Author information
Authors and Affiliations
Contributions
SMG was the principal investigator of the study. SC performed the statistical analyses and aided in the interpretation of the data. SMG wrote the first draft of the manuscript. MR, JJ, KAK, and CM contributed significantly to the discussion and revision of this work, including analysis, interpretation of results, proofreading, edits and approval for submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gorka, S.M., Radoman, M., Jimmy, J. et al. Behavioral and brain reactivity to uncertain stress prospectively predicts binge drinking in youth. Neuropsychopharmacol. 48, 1194–1200 (2023). https://doi.org/10.1038/s41386-023-01571-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-023-01571-x
This article is cited by
-
Increasing ecological validity in neuropsychopharmacology research on the relationship between alcohol use and uncertain stressors
Neuropsychopharmacology (2023)
-
Reply to Bradford: Comment on increasing ecological validity in neuropsychopharmacology research on the relationship between alcohol use and uncertain stressors
Neuropsychopharmacology (2023)