Abstract
Objective
Intraventricular hemorrhage (IVH) is a common complication in extremely preterm infants. We aimed to demonstrate that umbilical cord milking (UCM) would reduce the incidence of IVH in this at risk population.
Study design
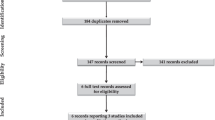
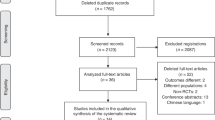
We compared the incidence of IVH in a prospective cohort of consecutively born preterm infants <32 weeks’ gestation receiving UCM (n = 33) with a historical cohort that underwent immediate cord clamping (ICC) (n = 36).
Results
No significant differences regarding perinatal characteristics were present between both groups except for chorioamnionitis and preterm rupture of membranes which were more frequent in the UCM group. There was a significant reduction in the incidence of IVH in the UCM group as compared to the ICC group (UCM vs. ICC = 12 vs. 33%, p = 0.037; OR = 0.276 (95% CI 0.079–0.967; p = 0.033; NNT = 4.7) and a reduction in the number of transfusions (UCM vs. ICC = 56 vs. 30%, p = 0.035; OR = 0.348 (0.129–0.938; p = 0.033; NNT = 3.8). UCM was safe for mothers (similar decrease in maternal hemoglobin) and offspring.
Conclusion
UCM significantly reduced the incidence of IVH in preterm infants < 32 weeks’ gestation without associated complications for mother or offspring.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
García-Muñoz Rodrigo F, Díez Recinos AL, García-Alix Pérez A, Figueras Aloy J, Vento Torres M. Changes in perinatal care and outcomes in newborns at the limit of viability in Spain: the EPI-SEN Study. Neonatology. 2015;107:120–9.
Rabe H, Diaz-Rossello JL, Duley L, Dowswell T. Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Syst Rev. 2012; 8. https://doi.org/10.1002/14651858.CD003248.pub3.
Committee on Obstetric Practice, American College of Obstetricians and Gynecologists. Committee Opinion no.543: timing of umbilical cord clamping after birth. Obstet Gynecol. 2012;120:1522–6.
Perlman JM, Wyllie J, Kattwinkel J, Wyckoff MH, Aziz K, Guinsburg R. et al. On behalf of the Neonatal Resuscitation Chapter CollaboratorsPart 7: neonatal resuscitation: 2015 International consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations. Circulation. 2015;132:S204–241.
Sommers R, Stonestret BS, Oh W, Laptook A, Yanowitz TD, Raker C, et al. Hemodynamic effects of delayed cord clamping in premature infants. Pediatrics. 2012;129:667–72.
Hosono S, Mugishima H, Fujita H, Hosono A, Minato M, Okada T, et al. Umbilical cord milking reduces the need for red cell transfusions and improves neonatal adaptation in infants born at less than 29 weeks’ gestation: a randomized controlled trial. Arch Dis Child Fetal Neonatal Ed. 2008;93:14–9.
March MI, Hacker MR, Parson AW, Modest AM, de Veciana M. The effects of umbilical cord milking in extremely preterm infants: a randomized controlled trial. J Perinatol. 2013;33:763–7.
Katheria AC, Leone TA, Woelkers D, Garey DM, Rich W, Finer NN. The effects of umbilical cord milking on hemodynamics and neonatal outcomes in premature neonates. J Pediatr. 2014;164:1045–50.
Katheria A, Blank D, Rich W, Finer N. Umbilical cord milking improves transition in premature infants at birth. PLoS One. 2014;7:e94085.
Alan S, Arsan S, Okulu E, Akin IM, Kilic A, Taskin S, et al. Effects of umbilical cord milking on the need for packed red blood cell transfusions and early neonatal hemodynamic adaptation in preterm infants born ≤1500 g: a prospective, randomized, controlled trial. J Pediatr Hematol Oncol. 2014;36:e493–8.
Song SY, Kim Y, Kang BH, Yoo HJ, Lee M. Safety of umbilical cord milking in very preterm neonates: a randomized controlled study. Obstet Gynecol Sci. 2017;60:527–34.
Al-Wassia H, Shah PS. Efficacy and safety of umbilical cord milking at birth: a systematic review and meta-analysis. JAMA Pediatr. 2015;169:18–25.
Dang D, Zhang C, Shi S, Mu X, Lv X, Wu H. Umbilical cord milking reduces need for red cell transfusions and improves neonatal adaptation in preterm infants: Meta-analysis. J Obstet Gynaecol Res. 2015;41:890–5.
Rabe H, Jewison A, Alvarez RF, Crook D, Stilton D, Bradley R, et al. Milking compared with delayed cord clamping to increase placental transfusion in preterm neonates: a randomized controlled trial. Obstet Gynecol. 2011;117:205–11.
Katheria AC, Truong G, Cousins L, Oshiro B, Finer NN. umbilical cord milking versus delayed cord clamping in preterm infants. Pediatrics. 2015;136:61–9.
Katheria A, Garey D, Truong G, Akshoomoff N, Steen J, Maldonado M, et al. A randomized clinical trial of umbilical cord milking vs delayed cord clamping in preterm infants: neurodevelopmental outcomes at 22-26 months of corrected age. J Pediatr. 2018;194:76–80.
Nagano N, Saito N, Sugiura T, Miyahara F, Namba F, Ota E. Benefits of umbilical cord milking versus delayed cord clamping on neonatal outcomes in preterm infants: a systematic review and meta-analysis. PLoS One. 2018;13:e0201528 https://doi.org/10.1371/journal.pone.0201528. 30
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1500 gm. J Pediatr. 1978;92:529–34.
Moro M, Vento M (eds). In: De guardia en Neonatologia. 3rd ed. Madrid: Panamericana; 2016. p. 650–9.
International Committee for the Classification of Retinopathy of Prematurity. The international classification of retinopathy of prematurity revisited. Arch Ophthalmol 2005;123:991–9.
Jobe AH, Bancalari E. Bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2001;163:1723.
Bell MJ, Ternberg J, Fengin RR. Neonatal necrotizing enterocolitis: therapeutic decisions based on clinical staging. Ann Surg. 1978;187:1–7.
Rezaie P, Dean A. Periventricular leukomalacia, inflammation and white matter lesions within the developing nervous system. Neuropathology. 2002;22:106–32.
Gibbs RS, Blanco JD, St Clair PJ, Castaneda YS. Quantitative bacteriology of amniotic fluid from women with clinical intraamniotic infection at term. J Infect Dis. 1982;145:1–8.
Anonymous. Practice Bulletin No.160: Premature rupture of membranes. Obstet Gynecol. 2016; 127:39-51.
Bolisetty S, Dhawan A, Abdel-Latif M, Bajuk B, Stack J, Lui K. Intraventricular hemorrhage and neurodevelopmental outcomes in extreme preterm infants. Pediatrics. 2014;133:55–62.
Osborn DA, Evans N, Kluckow M. Hemodynamic and antecedent risk factors of early and late periventricular/intraventricular haemorrhage in premature infants. Pediatrics. 2003;112:33–9.
Kluckow M, Evans N. Low superior vena cava flow and intraventricular haemorrhage in preterm infants. Arch Dis Child Fetal Neonatal Ed. 2000;82:188–94.
Takami T, Suganami Y, Sunohara D, Kondo A, Mizukaki N, Fujioka T, et al. Umbilical cord milking stabilizes cerebral oxygenation and perfusion in infants born before 29 weeks gestation. J Pediatr. 2012;161:742–7.
Rabe H, Sawyer A, Amess P, Ayers S. Neurodevelopmental outcomes at 2 and 3.5 years for very preterm babies enrolled in a randomized trial of milking the umbilical cord versus delayed cord clamping. Neonatology. 2016;109:113–9.
El-Naggar W, Simpson D, Hussain A, Armson A, Doods L, Warren A, et al. Cord milking versus immediate clamping in preterm infants: a randomised controlled trial. Arch Dis Child Fetal Neonatal 2018. https://doi.org/10.1136/archdischild-2018-314757.
Blank DA, Polglase GR, Kluckow M, Gill AW, Crossley KJ, Moxham A, et al. Haemodinamic effects of umbilical cord milking in premature sheep during neonatal transition. Arch Dis Child Fetal Neonatal 2017 https://doi.org/10.1136/archdischild-2017-314005.
Katheria A, Poeltler D, Durham J, Steen J, Rich W, Arnell K, et al. Neonatal resuscitation with an intact cord: a randomized clinical trial. J Pediatr. 2016;178:75–80.
Meyer MP, Nevill E, Wong MM. Provision of respiratory support compared to no respiratory support before cord clamping for preterm infants. Cochrane Database Syst Rev. 2018;3:CD012491 https://doi.org/10.1002/14651858.CD012491.pub2.
Gano D, Ho ML, Partridge JC, Glass HC, Xu D, Barkovich AJ, et al. Antenatal exposure to magnesium sulfate is associated with reduced cerebellar hemorrhage in preterm newborns. J Pediatr. 2016;178:68–74.
Patel S, Clark EAS, Rodriguez CE, Metz TD, Abbaszadeh M, Yoder BA. Effect of umbilical cord milking on morbidity and survival in extremely low gestational age neonates. Am J Obstet Gynecol. 2014;211:519.e1–7.
Kilicdag H, Gulcan H, Hanta D, Torer B, Gokmen Z, Ozdemir SI, et al. Is umbilical cord milking always an advantage? J Matern Fetal Neonatal Med. 2016;29:615–8.
Carroll J. Human cord blood for the hypoxic-ischemic neonate. Pediatr Res. 2012;71:459–63.
Li J, McDonald CA, Fahey MC, Jenkin G, Miller SL. Could cord blood cell therapy reduce preterm brain injury? Front Neurol. 2014;5:200.
Vatansever B, Demirel G, Ciler Eren E, Erel O, Neselioglu S, Karavar NH, et al. Is early cord clamping or cord milking best? J Mater Fetal Neonatal Med. 2018;31:877–80.
Acknowledgements
We would like to especially thank the families for their generosity in accepting participate in the study. We also would like to thank the obstetric team and the nursing staff in the delivery room for their essential contribution.
Funding
M Vento acknowledges a FIS PI17/0131 grant from the Instituto de Investigación Sanitaria Carlos III (Ministry of Science, Innovation and Universities; Kingdom of Spain)
Author information
Authors and Affiliations
Contributions
JDT conceived the study and contributed to its design, enrolled patients, retrieved and analyze the data, and wrote the draft of the manuscript. SR enrolled patients, retrieved and analyze the data, and wrote the draft of the manuscript. AP-I enrolled patients, retrieved and analyze the data, and wrote the draft of the manuscript, AD enrolled patients, retrieved and analyze the data, and wrote the draft of the manuscript, YM, enrolled patients, retrieved and analyze the data, and wrote the draft of the manuscript, MV contributed to the study design, supervised data analysis, and wrote the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Toledo, J.d., Rodilla, S., Pérez-Iranzo, A. et al. Umbilical cord milking reduces the risk of intraventricular hemorrhage in preterm infants born before 32 weeks of gestation. J Perinatol 39, 547–553 (2019). https://doi.org/10.1038/s41372-019-0329-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0329-6
This article is cited by
-
Neurodevelopmental outcomes of very preterm infants who received cord milking at birth: a randomized controlled trial
European Journal of Pediatrics (2022)
-
Less invasive surfactant administration reduces incidence of severe intraventricular haemorrage in preterms with respiratory distress syndrome: a cohort study
Journal of Perinatology (2020)
-
Grading the evidence to identify strategies to modify risk for necrotizing enterocolitis
Pediatric Research (2020)
-
Umbilical cord milking in preterm infants: time to act
Journal of Perinatology (2019)