Abstract
Objective
Identify risk factors for poor perineal outcome after operative vaginal delivery.
Study design
A retrospective cohort study was performed including operative vaginal deliveries during 2015 through 2016.
Results
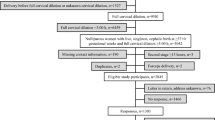
Of 529 operative vaginal deliveries, 79 (14.9%) had higher order perineal lacerations and 14 (2.7%) had a wound breakdown. The only significant risk factor for higher order lacerations was chorioamnionitis (aOR 2.2; 95% CI 1.09–4.44). Risk factors for perineal wound breakdown included episiotomy (5.2 vs. 1.2%; p < 0.01), type of operative delivery (5.5% after forceps vs. 1.4% after vacuum; p < 0.01) and postpartum narcotic use. Overall, 9.3% of those using narcotics subsequently had a perineal breakdown as compared to 0.7% (p < 0.01). Narcotic use postpartum remained strongly associated in multivariable logistic regression (aOR 21.29; 95% CI 5.43–83.47). Patients with forceps deliveries, episiotomy, and narcotic use had a 38% risk of breakdown.
Conclusion
Women at highest risk of perineal wound breakdown benefit from close follow-up.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Christianson LM, Bovbjerg VE, McDavitt EC, Hullfish KL. Risk factors for perineal injury during delivery. Am J Obstet Gynecol. 2003;189:255–60.
Kaltreider DE, Dixon DM. A study of 710 complete lacerations following central episiotomy. South Med J. 1968;36:816.
Ramin SM, Gilstrap LC III. Episiotomy and early repair of dehiscence. Clin Obstet Gynecol. 1994;37:816–23.
Goldaber KG, Wendel PJ, McIntire DD, Wendel GD Jr. Postpartum perineal morbidity after fourth degree perineal repair. Am J Obstet Gynecol. 1993;168:489–93.
Samarasakera DN, Bekhit MT, Wright Y, Lowndes RH, Stanley KP, Preston JP, et al. Long-term anal continence and quality of life following postpartum anal sphincter injury. Colorectal Dis. 2008;10:793–9.
Jallad K, Steele SE, Barber MD. Breakdown of perineal laceration repair after vaginal delivery: a case-control study. Female Pelvic Med Reconstr Surg. 2016;22:276–9.
Williams MK, Chames MC. Risk factors for the breakdown of perineal laceration repair after vaginal delivery. Am J Obstet Gynecol. 2006;195:755–9.
Pergialiotis V, Vlachos D, Protopapas A, Pappa K, Vlachos G. Risk factors for severe perineal lacerations during childbirth. Int J Gynaecol Obstet. 2014;125:6–14.
Lewicky-Gaupp C, Leader-Cramer A, Johnson LL, Kenton K, Gossett DR. Wound complications after obstetric anal sphincter injuries. Obstet Gynecol. 2015;125:1088–93.
Stock L, Basham E, Gossett DR, Lewicky-Gaupp C. Factors associated with wound complications in women with obstetric anal sphincter injuries (OASIS). Am J Obstet Gynecol. 2013;208:327. e1–6.
Lindholm ES, Altman D. Risk of obstetric anal sphincter lacerations among obese women. BJOG: Int J Obstet Gynecol. 2013;120:1110–5.
Garretto D, Lin BB, Syn HL, Judge N, Beckerman K, Atallah F, et al. Obesity may be protective against servere perineal lacerations. J Obes. 2016;2016:9376592.
Homsi R, Daikoku NH, Littlejohn J, Wheeless CR Jr. Episiotomy: risks of dehiscence and rectovaginal fistula. Obstet Gynecol Surv. 1994;49:803–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Wilkie, G.L., Saadeh, M., Robinson, J.N. et al. Risk factors for poor perineal outcome after operative vaginal delivery. J Perinatol 38, 1625–1630 (2018). https://doi.org/10.1038/s41372-018-0252-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0252-2