Abstract
Objective
To examine current level three Neonatal Intensive Care Unit (NICU) practices related to ROP screening and treatment.
Study design
A cross-sectional survey was sent to 29 level three NICU’s across Canada to survey current screening inclusion criteria, treatment options, supportive care and post-screening events for ROP.
Result
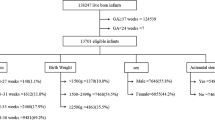
22/29 (76%) level three NICU’s responded. Ten different ROP screening inclusion criteria were found to be in use with significant variation in gestational age and birth weight criteria. Many other national variations also exist regarding the supportive and procedural protocols surrounding ROP screening as well as mode of treatment for ROP.
Conclusion
Despite national guidelines, significant variation in ROP screening inclusion criteria practices exist among neonatal units in Canada. Therefore, there is an urgent need for better evidence-based screening guidelines as well as a need to standardize supportive measures surrounding ROP screening and treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Jeffries AL. Retinopathy of prematurity recommendations for screening. Paediatr Child Health. 2010;15:667–74.
Wilkinson AR, Haines L, Head K, Fielder AR. UK retinopathy of prematurity guideline. Early Hum Dev. 2008;84:71–74.
Fierson WM, American Academy of Pediatrics, Section on Ophthalmology, American Academy of Ophthalmology, American Association for Pediatric Ophthalmology and Strabismus, American Association of Certified Orthoptists. Screening examination of premature infants for retinopathy of prematurity. Pediatrics. 2013;131:189–95.
The Canadian Neonatal Network. Abstractors manual, (v 1.3.4). http://www.canadianneonatalnetwork.org/Portal/LinkClick.aspx?fileticket=U4anCYsSN20%3D&tabid=69.
Ehringer G, Duffy B. Promoting best practice and safety through pre-printed Physician orders. In: Henriksen K, Battles JB, Keyes MA, et al., editors. Advances in patient safety: new directions and alternative approaches (Vol. 2: Culture and Redesign). Rockville, MD: Agency for Healthcare Research and Quality; 2008. https://www.ncbi.nlm.nih.gov/books/NBK43696/.
Amer M, Jafri WH, Nizami AM, Shomrani AI, Al-Dabaan AA, Rashid K. Retinopathy of prematurity: are we missing any infant with retinopathy of prematurity? Br J Ophthalmol. 2012;96:1052–5.
Bain LC, Dudley A, Gould JB, Lee HC. Factors associated with failure to screen newborns for retinopathy of prematurity. J Pediatr. 2012;161:819–23.
Black L, Hulsey T, Lee K, Parks DC, Ebeling MD. Incremental hospital costs associated with comorbidities of prematurity. Manag Care. 2015;24:54–60.
Abdul Aziz AA, Isaac M, Tehrani NN. Using telemedicine to screen for retinopathy of prematurity. CMAJ. 2014;186:1012–4.
Wang SK, Callaway NF, Wallenstein MB, Henderson MT, Leng T, Moshfeghi DM. SUNDROP: six years of screening for retinopathy of prematurity with telemedicine. Can J Ophthalmol. 2015;50:101–6.
Vinekar A, Gilbert C, Dogra M, Kurian M, Shainesh G, Shetty B, et al. The KIDROP model of combining strategies for providing retinopathy of prematurity screening in underserved areas in India using wide-field imaging, tele-medicine, non-physician graders and smart phone reporting. Indian J Ophthalmol. 2014;62:41–49.
Quinn GE, Ying GS, Daniel E, Hildebrand PL, Ells A, Baumritter A, et al. Validity of a telemedicine system for the evaluation of acute-phase retinopathy of prematurity. JAMA Ophthalmol. 2014;132:1178–84.
Mitchell AJ, Green A, Jeffs DA, Roberson PK. Physiologic effects of retinopathy of prematurity screening examinations. Adv Neonatal Care. 2011;11:291–7.
Sun X, Lemyre B, Barrowman N, O’Connor M. Pain management during eye examinations for retinopathy of prematurity in preterm infants: a systematic review. Acta Paediatr. 2010;99:329–34.
Neffendorf JE, Mota MP, Xue K, Hildebrand GD. Efficacy and safety of phenylephrine 2.5% with cyclopentolate 0.5% for retinopathy of prematurity screening in 1246 eye examinations. Eur J Ophthalmol. 2015;25:249–53.
Shah P, Yoon EW, Chan P, Members of the Annual Report Review Committee. The Canadian neonatal network annual report 2014. http://www.canadianneonatalnetwork.org/Portal/LinkClick.aspx?fileticket = eGgxmMubxjk%3d&tabid = 39. Accessed 2 Oct 2016.
Palmer EA, Hardy RJ, Dobson V, Phelps DL, Quinn GE, Summers CG, et al. 15-year outcomes following threshold retinopathy of prematurity: final results from the multicenter trial of cryotherapy for retinopathy of prematurity. Arch Ophthalmol. 2005;123:311–8.
Trigler L, Weaver RG Jr, O’Neil JW. Case series of angle-closure glaucoma after laser treatment for retinopathy of prematurity. J AAPOS. 2005;9:17–21.
Simons BD, Wilson MC, Hertle RW, Schaefer DB. Bilateral hyphemas and cataracts after diode laser retinal photoablation for retinopathy of prematurity. J Pediatr Ophthalmol Strabismus. 1998;35:185–7.
Lambert SR, Capone A Jr, Cingle KA, Drack AV. Cataract and phthisis bulbi after laser photoablation for threshold retinopathy of prematurity. Am J Ophthalmol. 2000;129:585–91.
Gordon RA, Donzis PA. Myopia associated with retinopathy of prematurity. Ophthalmol. 1986;93:1593–8.
Travassos A, Teixeira S, Ferreira P, Regadas I, Travassos AS, Esperancinha FE, et al. Intravitreal bevacizumab in aggressive posterior retinopathy of prematurity. Ophthal Surg Lasers Imaging. 2007;38:233–7.
Mintz-Hittner HA, Kennedy KA, Chuang AZ, BEAT-ROP Cooperative Group. Efficacy of intravitreal bevacizumab for stage 3+ retinopathy of prematurity. New Engl J Med. 2011;364:603–15.
Klufas MA, Chan RV. Intravitreal anti-VEGF therapy as a treatment for retinopathy of prematurity: what we know after 7 years. J Pediatr Ophthalmol Strabismus. 2015;52:77–84.
Morin J, Luu TM, Superstein R, Ospina LH, Befebvre F, Simard MN, et al. Neurodevelopmental outcomes following bevacizumab injections for retinopathy of prematurity. Pediatrics. 2016;137:e20153218.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Sabri, K., Woodward, M.A., Easterbrook, B. et al. Retinopathy of prematurity practices: a national survey of Canadian Neonatal Intensive Care Units. J Perinatol 38, 381–385 (2018). https://doi.org/10.1038/s41372-017-0030-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-017-0030-6
This article is cited by
-
Survey of preterm neuro-centric care practices in California neonatal intensive care units
Journal of Perinatology (2019)